Abstract
Background
Reintegration into school is a decisive time for children who have been absent from school due to health problems, such as survivors of brain tumours and other types of acquired brain injury or cancer in childhood. Parents, school staff and healthcare providers are important stakeholders during this phase of transition.
Objective
To study the perspectives of parents, school personnel and healthcare providers on communication and collaboration following the child’s return to school, to gain insight into their experiences, and to develop recommendations for each stakeholder.
Method
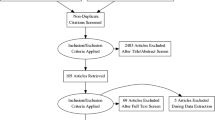
We reviewed the literature on school reintegration in accordance with the configurative approach for research synthesis. Search and selection processes ended in 22 articles published between January 2000 and September 2015, consisting of quantitative, qualitative or mixed methods research. Data analysis resulted in themes with emphasis on communication and collaboration.
Results
Knowledge about the child’s condition, education and support are the main topics of consultation between parents, school personnel and healthcare providers. Based on their experiences, practices of communication and collaboration are variable and mostly inadequate. They report clear and complementary needs and expectations on how to effectively work together. Especially the need for a school liaison as connection between family, education and healthcare is commonly discussed.
Conclusion
The often suboptimal communication and collaboration between parents, school personnel and healthcare providers needs more coordination and consistency, starting from the child’s return to school. In addition, all stakeholders should be aware of related factors that facilitate or hinder the child’s reintegration process.

Similar content being viewed by others
References
Andersson, K., Bellon, M., & Walker, R. (2016). Parents’ experiences of their child’s return to school following acquired brain injury (ABI): A systematic review of qualitative studies. Brain Injury, 30, 829–838.
Annett, R. D., & Erickson, S. J. (2009). Feasibility of a school reintegration programme for children with acute lymphoblastic leukaemia. European Journal of Cancer Care, 18, 421–428.
Asprey, A., & Nash, T. (2006). The importance of awareness and communication for the inclusion of young people with life-limiting and life-threatening conditions in mainstream schools and colleges. British Journal of Special Education, 33, 10–18.
Aukema, E. J., Last, B. F., Schouten-van Meeteren, A. Y. N., & Grootenhuis, M. A. (2011). Explorative study on the aftercare of pediatric brain tumor survivors: A parents’ perspective. Supportive Care in Cancer, 19, 1637–1646.
Ball, H., & Howe, J. (2013). How can educational psychologists support the reintegration of children with an acquired brain injury upon their return to school? Educational Psychology in Practice, 29, 69–78.
Barnett-Page, E., & Thomas, J. (2009). Methods for the synthesis of qualitative research: A critical review. BMC Medical Research Methodology, 9, 59.
Bedell, G. M., Cohn, E. S., & Dumas, H. M. (2005). Exploring parents’ use of strategies to promote social participation of school-age children with acquired brain injuries. American Journal of Occupational Therapy, 59, 273–284.
Boonen, H., & Petry, K. (2012). How do children with a chronic or long-term illness perceive their school re-entry after a period of homebound instruction? Child: Care, Health and Development, 38, 490–496.
Bradley-Klug, K. L., Sundman, A. N., Nadeau, J., Cunningham, J., & Ogg, J. (2010). Communication and collaboration with schools: Pediatricians’ perspectives. Journal of Applied School Psychology, 26, 263–281.
Brown, M. B., Bolen, L. M., Brinkman, T. M., Carreira, K., & Cole, S. (2011). A collaborative strategy with medical providers to improve training for teachers of children with cancer. Journal of Educational & Psychological Consultation, 21, 149–165.
Bruce, B. S., Chapman, A., MacDonald, A., & Newcombe, J. (2008). School experiences of families of children with brain tumors. Journal of Pediatric Oncology Nursing, 25, 331–339.
Bruce, B. S., Newcombe, J., & Chapman, A. (2012). School liaison program for children with brain tumors. Journal of Pediatric Oncology Nursing, 29, 45–54.
Butler, R. W., & Haser, J. K. (2006). Neurocognitive effects of treatment for childhood cancer. Mental Retardation and Developmental Disabilities Research Reviews, 12, 184–191.
Canto, A. I., Chesire, D. J., Buckley, V. A., Andrews, T. W., & Roehrig, A. D. (2014). Barriers to meeting the needs of students with traumatic brain injury. Educational Psychology in Practice, 30, 88–103.
Capurso, M., & Dennis, J. L. (2017). Key educational factors in the education of students with a medical condition. Support for Learning, 32, 158–179.
Cheung, L. L., Wakefield, C. E., Ellis, S. J., Mandalis, A., Frow, E., & Cohn, R. J. (2014). Neuropsychology reports for childhood brain tumor survivors: Implementation of recommendations at home and school. Pediatric Blood & Cancer, 61, 1080–1087.
Chevignard, M., Toure, H., Brugel, D. G., Poirier, J., & Laurent-Vannier, A. (2010). A comprehensive model of care for rehabilitation of children with acquired brain injuries. Child: Care. Health and Development, 36, 31–43.
Clay, D. L., Cortina, S., Harper, D. C., Cocco, K. M., & Drotar, D. (2004). Schoolteachers’ experiences with childhood chronic illness. Children’s Health Care, 33, 227–239.
Critical Appraisal Skills Programme (CASP). (2006). 10 questions to help you make sense of qualitative research. England: Public Health Resource Unit. Retrieved February 26, 2016, from http://www.casp-uk.net/checklists.
Deatrick, J. A., Mullaney, E. K., & Mooney-Doyle, K. (2009). Exploring family management of childhood brain tumor survivors. Journal of Pediatric Oncology Nursing, 26, 303–311.
Deidrick, K. K., & Farmer, J. E. (2005). School reentry following traumatic brain injury. Preventing School Failure, 49, 23–33.
Dixon-Woods, M., Agarwal, S., Jones, D., Young, B., & Sutton, A. (2005). Synthesizing qualitative and quantitative evidence: A review of possible methods. Journal of Health Services Research & Policy, 10, 45–53.
Donnan, B. M., Webster, T., Wakefield, C. E., Dalla-Pozza, L., Alvaro, F., Lavoipierre, J., et al. (2015). What about school? Educational challenges for children and adolescents with cancer. The Australian Educational and Developmental Psychologist, 32, 23–40.
Eaton Russell, C., Bouffet, E., Beaton, J., & Lollis, S. (2016). Balancing grief and survival: Experiences of children with brain tumors and their parents. Journal of Psychosocial Oncology, 34, 376–399.
Eilertsen, M. B., Rannestad, T., Indredavik, M. S., & Vik, T. (2011). Psychosocial health in children and adolescents surviving cancer. Scandinavian Journal of Caring Sciences, 25, 725–734.
Eilertsen, M. B., Reinfjell, T., & Vik, T. (2004). Value of professional collaboration in the care of children with cancer and their families. European Journal of Cancer Care, 13, 349–355.
Engeström, Y. (2008). From teams to knots: Activity-theoretical studies of collaboration and learning at work. Cambridge: Cambridge University Press.
Ernst, W. J., Gallo, A. B., Sellers, A. L., Mulrine, J., MacNamara, L., Abrahamson, A., et al. (2016). Knowledge of traumatic brain injury among educators. Exceptionality, 24, 123–136.
Gagnon, I., Swaine, B., Champagne, F., & Lefebvre, H. (2008). Perspectives of adolescents and their parents regarding service needs following a mild traumatic brain injury. Brain Injury, 22, 161–173.
Gfroerer, S. D., Wade, S. L., & Wu, M. (2008). Parent perceptions of school-based support for students with traumatic brain injuries. Brain Injury, 22, 649–656.
Gioia, G. A. (2016). Medical-school partnership in guiding return to school following mild traumatic brain injury in youth. Journal of Child Neurology, 31, 93–108.
Glang, A., Todis, B., Thomas, C. W., Hood, D., Bedell, G., & Cockrell, J. (2008). Return to school following childhood TBI: Who gets service? NeuroRehabilitation, 23, 477–486.
Gorin, S. S., & McAuliffe, P. (2009). Implications of childhood cancer survivors in the classroom and the school. Health Education, 109, 25–48.
Gough, D., Thomas, J., & Oliver, S. (2012). Clarifying differences between review designs and methods. Systematic Reviews, 1, 28.
Gutkin, T. B. (2012). Ecological psychology: Replacing the medical model paradigm for school-based psychological and psychoeducational services. Journal of Educational & Psychological Consultation, 22, 1–20.
Harris, M. S. (2009). School reintegration for children and adolescents with cancer: The role of school psychologists. Psychology in the Schools, 46, 579–592.
Hartman, L. R., Duncanson, M., Farahat, S. M., & Lindsay, S. (2015). Clinician and educator experiences of facilitating students’ transition to school following acquired brain injury: A qualitative systematic review. Brain Injury, 29, 1387–1399.
Hawley, C. A., Ward, A. B., Magnay, A. R., & Mychalkiw, W. (2004). Return to school after brain injury. Archives of Disease in Childhood, 89, 136–142.
Hinton, D., & Kirk, S. (2015). Teachers’ perspectives of supporting pupils with long-term health conditions in mainstream schools: A narrative review of the literature. Health and Social Care in the Community, 23, 107–120.
Hopkins, L., Green, J., Henry, J., Edwards, B., & Wong, S. (2014). Staying engaged: The role of teachers and schools in keeping young people with health conditions engaged in education. The Australian Educational Researcher, 41, 25–41.
Kaffenberger, C. J. (2006). School reentry for students with a chronic illness: A role for professional school counselors. Professional School Counseling, 9, 223–230.
Kirk, S., Fallon, D., Fraser, C., Robinson, G., & Vassallo, G. (2015). Supporting parents following childhood traumatic brain injury: A qualitative study to examine information and emotional support needs across key care transitions. Child: Care, Health and Development, 41, 303–313.
Knauer, H., Baker, D. L., Hebbeler, K., & Davis-Alldritt, L. (2015). The mismatch between children’s health needs and school resources. Journal of School Nursing, 31, 326–333.
Lähteenmäki, P. M., Huostila, J., Hinkka, S., & Salmi, T. T. (2002). Childhood cancer patients at school. European Journal of Cancer, 38, 1227–1240.
Linden, M. A., Braiden, H., & Miller, S. (2013). Educational professionals’ understanding of childhood traumatic brain injury. Brain Injury, 27, 92–102.
Long, K. A., & Marsland, A. L. (2011). Family adjustment to childhood cancer: A systematic review. Clinical Child and Family Psychology Review, 14, 57–88.
Lown, E. A., Phillips, F., Schwartz, L. A., Rosenberg, A. R., & Jones, B. (2015). Psychosocial follow-up in survivorship as a standard of care in pediatric oncology. Pediatric Blood & Cancer, 62, S514–S584.
Lum, A., Wakefield, C. E., Donnan, B., Burns, M. A., Fardell, J. E., & Marshall, G. M. (2017). Understanding the school experiences of children and adolescents with serious chronic illness: A systematic meta-review. Child: Care, Health and Development, 43, 645–663.
Massey, S., Fisher, K., Croker, A., & Smith, T. (2015). Collaboration across the health care and education interface: What is it like for teachers of children with traumatic brain injury. Australian Journal of Primary Health, 21, 74–78.
McLoone, J. K., Wakefield, C. E., Butow, P., Fleming, C., & Cohn, R. J. (2011). Returning to school after adolescent cancer: A qualitative examination of Australian survivors’ and their families’ perspectives. Journal of Adolescent and Young Adult Oncology, 1, 87–94.
McLoone, J. K., Wakefield, C. E., & Cohn, R. J. (2013). Childhood cancer survivors’ school (re)entry: Australian parents’ perceptions. European Journal of Cancer Care, 22, 484–492.
Mealings, M., Douglas, J., & Olver, J. (2012). Considering the student perspective in returning to school after TBI: A literature review. Brain Injury, 26, 1165–1176.
Mitchell, W., Clarke, S., & Sloper, P. (2006). Care and support needs of children and young people with cancer and their parents. Psycho-Oncology, 15, 805–816.
Mohr, J. D., & Bullock, L. M. (2005). Traumatic brain injury: Perspectives from educational professionals. Preventing School Failure: Alternative Education for Children and Youth, 49, 53–57.
Moore, B. D. (2005). Neurocognitive outcomes in survivors of childhood cancer. Journal of Pediatric Psychology, 30, 51–63.
Moore, J. B., Kaffenberger, C., Goldberg, P., Mi Oh, K., & Hudspeth, R. (2009). School reentry for children with cancer: Perceptions of nurses, school personnel, and parents. Journal of Pediatric Oncology Nursing, 2009(26), 86–99.
Mukherjee, S., Lightfoot, J., & Sloper, P. (2002). Communicating about pupils in mainstream school with special health needs: The NHS perspective. Child: Care, Health and Development, 28, 21–27.
Nabors, L. A., Little, S. G., Akin-Little, A., & Iobst, E. A. (2008). Teacher knowledge of and confidence in meeting the needs of children with chronic medical conditions: Pediatric psychology’s contribution to education. Psychology in the Schools, 45, 217–226.
National Collaborating Centre for Methods and Tools. (2015). Appraising qualitative, quantitative, and mixed methods studies included in mixed studies reviews: The MMAT. Hamilton, ON: McMaster University. (Updated September 01, 2017) Retrieved from http://www.nccmt.ca/knowledge-repositories/search/232.
Patterson, J. M., Holm, K. E., & Gurney, J. G. (2004). The impact of childhood cancer on the family: A qualitative analysis of strains, resources, and coping behaviors. Psycho-Oncology, 13, 390–407.
Pini, S., Gardner, P., & Hugh-Jones, S. (2013). The impact of a cancer diagnosis on the education engagement of teenagers—Patient and staff perspective. European Journal of Oncology Nursing, 17, 317–323.
Poggi, G., Liscio, M., Adduci, A., Galbiatti, S., Massimino, M., Sommovigo, M., et al. (2005). Psychological and adjustment problems due to acquired brain lesions in childhood: A comparison between post-traumatic patients and brain tumour survivors. Brain Injury, 19, 777–785.
Popernack, M. L., Gray, N., & Reuter-Rice, K. (2015). Moderate-to-severe traumatic brain injury in children: Complications and rehabilitation strategies. Journal of Pediatric Health Care, 29, e1–e7.
Poursanidou, K., Garner, P., & Watson, A. (2008). Hospital-school liaison: Perspectives of health and education professionals supporting children with renal transplants. Journal of Child Health Care, 12, 253–267.
Prevatt, F. F., Heffer, R. W., & Lowe, P. A. (2000). A review of school reintegration programs for children with cancer. Journal of School Psychology, 38, 447–467.
QSR International Pty Ltd. (2008). NVivo qualitative data analysis software (Version 8) [Computer software]. Cambridge, MA: QSR International Pty Ltd.
Roscigno, C. I., Fleig, D. K., & Knafl, K. A. (2015). Parent management of the school reintegration needs of children and youth following moderate or severe traumatic brain injury. Disability and Rehabilitation, 37, 523–533.
Sandelowski, M., Voils, C. I., Leeman, J., & Crandell, J. L. (2012). Mapping the mixed methods-mixed research synthesis terrain. Journal of Mixed Methods Research, 6, 317–331.
Savage, R. C., DePompei, R., Tyler, J., & Lash, M. (2005). Paediatric traumatic brain injury: A review of pertinent issues. Pediatric Rehabilitation, 8, 92–103.
Schachar, R. J., Park, L. S., & Dennis, M. (2015). Mental health implications of traumatic brain injury (TBI) in children and youth. Journal of the Canadian Academy of Child and Adolescent Psychiatry, 24, 100–108.
Selwood, K., Hemsworth, S., & Rigg, J. (2013). Children with cancer: Quality of information for returning to school. Nursing Children and Young People, 25, 14–18.
Sharp, N. L., Bye, R. A., Llewellyn, G. M., & Cusick, A. (2006). Fitting back in: Adolescents returning to school after severe acquired brain injury. Disability and Rehabilitation, 28, 767–778.
Shaw, R. S., Glaser, S. E., & Ouimet, T. (2011). Developing the medical liaison role in school settings. Journal of Educational and Psychological Consultation, 21, 106–117.
Shields, J. D., Heron, T. E., Rubenstein, C. L., & Katz, E. R. (1995). The eco-triadic model of educational consultation for students with cancer. Education and Treatment of Children, 18, 184–200.
Slomine, B. S., Mccarthy, M. L., Ding, R., Mackenzie, E. J., Jaffe, K. M., Aitken, M. E., et al. (2006). Health care utilization and needs after pediatric traumatic brain injury. Pediatrics, 117, e663–e674.
Smith, M. A., Seibel, N. L., Altekruse, S. F., Ries, L. A., Melbert, D. L., O’Leary, M., et al. (2010). Outcomes for children and adolescents with cancer: Challenges for the twenty-first century. Journal of Clinical Oncology, 28, 2625–2634.
Sullivan, N. A., Fulmer, D. L., & Zigmond, N. (2001). School: The normalizing factor for children with childhood leukemia: Perspectives of young survivors and their parents. Preventing School Failure: Alternative Education for Children and Youth, 46, 4–13.
Thomas, J., & Harden, A. (2008). Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Medical Research Methodology, 8, 45.
Van’t Hooft, I., Norberg, A. L., Björklund, A., Lönnerblad, M., & Strömberg, B. (2016). Multiprofessional follow-up programmes are needed to address psychosocial, neurocognitive and educational issues in children with brain tumours. Acta Paediatrica, 105, 676–683.
Vance, Y. H., & Eiser, C. (2002). The school experience of the child with cancer. Child: Care, Health and Development, 28, 5–19.
Vance, Y. H., Eiser, C., & Horne, B. (2004). Parents’ views of the impact of childhood brain tumours and treatment on young people’s social and family functioning. Clinical Child Psychology and Psychiatry, 9, 271–288.
Wade, S. L., Gerry Taylor, H., Yeates, K. O., Drotar, D., Stancin, T., Minich, N. M., et al. (2006). Long-term parental and family adaptation following pediatric brain injury. Journal of Pediatric Psychology, 31, 1072–1083.
Wakefield, C. E., McLoone, J. K., Butow, P., Lenthen, K., & Cohn, R. J. (2011). Parental adjustment to the completion of their child’s cancer treatment. Pediatric Blood & Cancer, 56, 524–531.
West, A. M., Denzer, A. Q., Wildman, B. G., & Anhalt, K. (2013). Teacher perception of burden and willingness to accommodate children with chronic health conditions. Advances in School Mental Health Promotion, 6, 35–50.
Woodgate, R. L. (2006). Life is never the same: Childhood cancer narratives. European Journal of Cancer Care, 15, 8–18.
Yeates, K. O., Bigler, E. D., Dennis, M., Gerhardt, C. A., Rubin, K. H., Stancin, T., et al. (2007). Social outcomes in childhood brain disorder: A heuristic integration of social neuroscience and developmental psychology. Psychological Bulletin, 133, 535–556.
Ylvisaker, D. M., Adelson, W. P., Braga, M. L., Burnett, M. S., Glang, M. A., Feeney, M. T., et al. (2005). Rehabilitation and ongoing support after pediatric TBI: Twenty years of progress. Journal of Head Trauma Rehabilitation, 20, 95–109.
Ysseldyke, J., Lekwa, A. J., Klingbeil, B. A., & Cormier, D. C. (2012). Assessment of ecological factors as an integral part of academic and mental health consultation. Journal of Educational and Psychological Consultation, 22, 21–43.
Zeltzer, L. K., Recklitis, C., Buchbinder, D., Zebrack, B., Casillas, J., Tsao, J. C., et al. (2009). Psychological status in childhood cancer survivors: A report from the Childhood Cancer Survivor Study. Journal of Clinical Oncology, 27, 2396–2404.
Acknowledgements
The main researcher received a bursary from the Jeanne and Alice Van de Voorde Fund from the King Baouduin Foundation, Belgium and the Wetenschappelijk Fonds Willy Gepts of the UZ Brussel. The bursars had no involvement in the study design, data collection and analysis, writing process or decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Vanclooster, S., Benoot, C., Bilsen, J. et al. Stakeholders’ Perspectives on Communication and Collaboration Following School Reintegration of a Seriously Ill Child: A Literature Review. Child Youth Care Forum 47, 583–612 (2018). https://doi.org/10.1007/s10566-018-9443-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10566-018-9443-4