Abstract
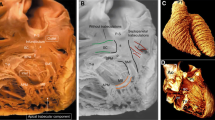
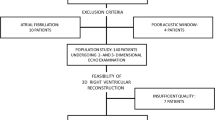
Obtaining focused right ventricular (RV) apical view remains challenging using conventional two-dimensional (2D) echocardiography. This study main objective was to determine whether measurements from RV focused views derived from three-dimensional (3D) echocardiography (3D-RV-focused) are closely related to measurements from magnetic resonance (CMR). A first cohort of 47 patients underwent 3D echocardiography and CMR imaging within 2 h of each other. A second cohort of 25 patients had repeat 3D echocardiography to determine the test–retest characteristics; and evaluate the bias associated with unfocused RV views. Tomographic views were extracted from the 3D dataset: RV focused views were obtained using the maximal RV diameter in the transverse plane, and unfocused views from a smaller transverse diameter enabling visualization of the tricuspid valve opening. Measures derived using the 3D-RV-focused view were strongly associated with CMR measurements. Among functional metrics, the strongest association was between RV fractional area change (RVFAC) and ejection fraction (RVEF) (r = 0.92) while tricuspid annular plane systolic excursion moderately correlated with RVEF (r = 0.47), all p < 0.001. Among RV size measures, the strongest association was found between RV end-systolic area (RVESA) and volume (r = 0.87, p < 0.001). RV unfocused views led on average to 10% underestimation of RVESA. The 3D-RV-focused method had acceptable test–retest characteristics with a coefficient of variation of 10% for RVESA and 11% for RVFAC. Deriving standardized RV focused views using 3D echocardiography strongly relates to CMR-derived measures and may improve reproducibility in RV 2D measurements.






Similar content being viewed by others
References
Amsallem M, Kuznetsova T, Hanneman K, Denault A, Haddad F (2016) Right heart imaging in patients with heart failure: a tale of two ventricles. Curr Opin Cardiol 31:469 –482
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 28:1–39
Hendel RC, Patel MR, Kramer CM, Poon M, Hendel RC, Carr JC et al (2006) ACCF/ACR/SCCT/SCMR/ASNC/NASCI/SCAI/SIR appropriateness criteria for cardiac computed tomography and cardiac magnetic resonance imaging: a report of the American College of Cardiology Foundation Quality Strategic Directions Committee Appropriateness Criteria Working Group, American College of Radiology, Society of Cardiovascular Computed Tomography, Society for Cardiovascular Magnetic Resonance, American Society of Nuclear Cardiology, North American Society for Cardiac Imaging, Society for Cardiovascular Angiography and Interventions, and Society of Interventional Radiology. J Am Coll Cardiol 2006; 48:1475–1497
Lang RM, Badano LP, Tsang W, Adams DH, Agricola E, Buck T et al (2012) EAE/ASE recommendations for image acquisition and display using three-dimensional echocardiography. J Am Soc Echocardiogr 25:3–46
Rudski LG, Lai WW, Afilalo J, Hua L, Handschumacher MD, Chandrasekaran K et al (2010) Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. J Am Soc Echocardiogr 23:685–713
Yang T, Liang Y, Zhang Y, Gu Q, Chen G, Ni X-H et al (2013) Echocardiographic parameters in patients with pulmonary arterial hypertension: correlations with right ventricular ejection fraction derived from cardiac magnetic resonance and hemodynamics. PLoS ONE 8:e71276
Wang Z, Yang Z, Wan Z, Yu T, Jia L, Du X et al (2014) Association between echocardiography derived right ventricular function parameters with cardiac magnetic resonance derived right ventricular ejection fraction and 6-minute walk distance in pulmonary hypertension patients. Zhonghua Xin Xue Guan Bing Za Zhi 42:748–752
Shiran H, Zamanian RT, McConnell MV, Liang DH, Dash R, Heidary S et al (2014) Relationship between echocardiographic and magnetic resonance derived measures of right ventricular size and function in patients with pulmonary hypertension. J Am Soc Echocardiogr 27:405–412
Li Y, Wang Y, Zhai Z, Guo X, Wu Y, Yang Y et al (2015) Relationship between echocardiographic and cardiac magnetic resonance imaging-derived measures of right ventricular function in patients with chronic thromboembolic pulmonary hypertension. Thromb Res 135:602–606
Focardi M, Cameli M, Carbone SF, Massoni A, De Vito R, Lisi M et al (2015) Traditional and innovative echocardiographic parameters for the analysis of right ventricular performance in comparison with cardiac magnetic resonance. Eur Heart J Cardiovasc Imaging 16:47–52
Tuzovic M, Adigopula S, Amsallem M, Kobayashi Y, Kadoch M, Boulate D et al (2015) Regional right ventricular dysfunction in acute pulmonary embolism: relationship with clot burden and biomarker profile. Int J Cardiovasc Imaging 32:389–398
Acknowledgements
The authors would like to thank Paul Kim and Semhar Sibhatu (Stanford University for their help in data collection, and Allan Paloma (from Stanford Cardiovascular Echocardiography Laboratory) for his technological expertise and knowledge.
Funding
This study was funded by the Stanford Cardiovascular Institute and the Vera Moulton Wall Center of Pulmonary Hypertension at Stanford.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MA received a Young Investigator Seed Grant from the Vera Moulton Wall Center. FH received funds from Pai Chan Lee Research fund. The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were approved by Stanford University Institutional Review Board in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study. This article does not contain any studies with animals performed by any of the authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Amsallem, M., Lu, H., Tang, X. et al. Optimizing right ventricular focused four-chamber views using three-dimensional imaging, a comparative magnetic resonance based study. Int J Cardiovasc Imaging 34, 1409–1417 (2018). https://doi.org/10.1007/s10554-018-1356-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-018-1356-7