Abstract
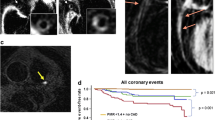
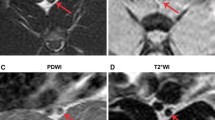
Our aim is to introduce an atherosclerotic rabbit model for inducing atherosclerosis lesions in rabbits, and to validate the model in vivo with 3T high resolution magnetic resonance imaging of the thrombosis followed a pharmacologically triggered plaque disruption. Twenty male New Zealand White rabbits were randomly allocated into an experimental group (n = 16) and a control group (n = 4). The aortic wall injuries were induced by an intravascular balloon in the experimental group rabbits after feeding them with a high cholesterol diet for 2 weeks. The pharmacological triggering with Russell’s viper venom and histamine was performed after totally 16 weeks of intermittent cholesterol feeding. All of the animals underwent both the pre-trigger and post-trigger MR examinations including TOF, T1WI, T2WI and post contrast T1WI. Euthanasia was performed in all rabbits; gross anatomy and histological specimen of aorta were obtained. MR images were analyzed and compared with histological results. Compared with the control group rabbits, the aorta of the experimental group rabbits in the pre-triggered MR images showed an increased vessel wall thickening, luminal narrowing, and vessel wall enhancement. Fourteen rabbits survived the triggering, and 8 of them developed thrombosis (58.1%). No thrombus was found in the control group. The accuracy of the multi-sequences MR including TOF, T1WI, T2WI and post contrast T1WI was 87.1% (27/31) for detecting thrombus. MR data significantly correlated with the histopathology data for both thrombus length (r = 0.94, P < 0.01) and thrombus location (r = 0.85, P < 0.01), respectively. The study demonstrated that MR reliably determined the plaque disruption and thrombus formation in the atherosclerotic rabbit model.




Similar content being viewed by others
References
Ross R (1999) Atherosclerosis: an inflammatory disease. N Engl J Med 340:115–126
Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, De Simone G et al (2010) Heart disease and stroke statistics—2009 update: a report from the American Heart Association. Circulation 121(7):e46–e215
Lutgens E, van Suylen RJ, Faber BC, Gijbels MJ, Eurlings PM, Bijnens AP et al (2003) Atherosclerotic plaque rupture: local or systemic process? Arterioscler Thromb Vasc Biol 23:2123–2130
Phinikaridou A, Hallock KJ, Qiao Y, Hamilton JA (2009) A robust rabbit model of human atherosclerosis and atherothrombosis. J Lipid Res 50(5):787–797
Russell JC, Proctor SD (2006) Small animal models of cardiovascular disease: tools for the study of the roles of metabolic syndrome, dyslipidemia, and atherosclerosis. Cardiovasc Pathol 15(6):318–330
Schaar JA, de Korte CL, Mastik F, Baldewsing R, Regar E, de Feyter P et al (2003) Intravascular palpography for high-risk vulnerable plaque assessment. Herz 28(6):488–495
Maurice RL, Fromageau J, Cardinal MH, Doyley M, de Muinck E, Robb J et al (2008) Characterization of atherosclerotic plaques and mural thrombi with intravascular ultrasound elastography: a potential method evaluated in an aortic rabbit model and a human coronary artery. IEEE Trans Inf Technol Biomed 12(3):290–298
Aziz K, Berger K, Claycombe K et al (2008) Noninvasive detection and localization of vulnerable plaque and arterial thrombosis with computed tomography angiography/positron emission tomography. Circulation 117:2061–2070
Meng L, Lv B, Zhang S, Yv B (2008) In vivo optical coherence tomography of experimental thrombosis in a rabbit carotid model. Heart 94(6):777–780
Chen WQ, Zhang L, Liu YF, Chen L, Ji XP, Zhang M et al (2007) Prediction of atherosclerotic plaque ruptures with high-frequency ultrasound imaging and serum inflammatory markers. Am J Physiol Heart Circ Physiol 293(5):H2836–H2844
Fuster V, Fayad ZA, Moreno PR, Poon M, Corti R, Badimon JJ (2005) Atherothrombosis and high-risk plaque part II: approaches by noninvasive computed tomographic/magnetic resonance imaging. J Am Coll Cardiol 46:1209–1218
Chu B, Ferguson MS, Chen H, Hippe DS, Kerwin WS, Canton G et al (2009) Magnetic resonance imaging features of the disruption-prone and the disrupted carotid plaque. JACC Cardiovasc Imag 2(7):883–896
Constantinides P, Chakravarti RN (1961) Rabbit arterial thrombosis production by systemic procedures. Arch Pathol 72(8):197–208
McConnell MV, Aikawa M, Maier SE, Ganz P, Libby P, Lee RT (1999) MRI of rabbit atherosclerosis in response to dietary cholesterol lowering. Arterioscler Thromb Vasc Biol 19:1956–1959
Abela GS, Picon PD, Friedl SE, Gebara OC, Miyamoto A, Federman M, Tofler GH, Muller JE (1995) Triggering of plaque disruption and arterial thrombosis in an atherosclerotic rabbit model. Circulation 91:776–784
Rekhter MD, Hicks GW, Brammer DW et al (1998) Animal model that mimics atherosclerotic plaque rupture. Circ Res 83(7):705–713
Johnstone MT, Botnar RM, Perez AS, Stewart R, Quist WC, Hamilton JA et al (2001) In vivo magnetic resonance imaging of experimental thrombosis in a rabbit model. Arterioscler Thromb Vasc Biol 21:1556–1560
Viereck J, Ruberg FL, Qiao Y, Perez AS, Detwiller K, Johnstone M, Hamilton JA (2005) MRI of atherothrombosis associated with plaque rupture. Arterioscler Thromb Vasc Biol 25(1):240–245
Corti R, Osende JI, Fayad ZA, Fallon JT, Fuster V, Mizsei G et al (2002) In vivo non-invasive detection and age definition of arterial thrombus by MRI. J Am Coll Cardiol 39:1366–1373
Botnar RM, Perez AS, Witte S, Wiethoff AJ, Laredo J, Hamilton J et al (2004) In vivo molecular imaging of acute and subacute thrombosis using a fibrin-binding magnetic resonance imaging contrast agent. Circulation 109(16):2023–2029
Sirol M, Fuster V, Badimon JJ et al (2005) Chronic thrombus detection with in vivo magnetic resonance imaging and a fibrin-targeted contrast agent. Circulation 112:1594–1600
Wasserman BA, Smith WI, Trout HH III, Cannon RO III, Balaban RS, Arai AE (2002) Carotid artery atherosclerosis: in vivo morphologic characterization with gadolinium-enhanced double-oblique MR imaging—initial results. Radiology 223:566–573
Kerwin WS, Hooker A, Spilker M, Vicini P, Ferguson M, Hatsukami T, Yuan C (2003) Quantitative magnetic resonance imaging analysis of neovasculature volume in carotid atherosclerotic plaque. Circulation 107:851–856
Barkhausen J, Ebert W, Heyer C et al (2003) Detection of Atherosclerotic plaque with gadofluorine-enhanced magnetic resonance imaging. Circulation 108:605–609
Naghavi M, Libby P, Falk E et al (2003) From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies—part I. Circulation 108:1664–1672
Naghavi M, Libby P, Falk E et al (2003) From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies—part II. Circulation 108:1772–1778
Phinikaridou A, Ruberg FL, Hallock KJ, Qiao Y, Hua N, Viereck J et al (2010) In vivo detection of vulnerable atherosclerotic plaque by MRI in a rabbit model. Circ Cardiovasc Imag 3(3):323–332
Calcagno C, Cornily JC, Hyafil F et al (2008) Detection of neovessels in atherosclerotic plaques of rabbits using dynamic contrast enhanced MRI and 18F-FDG PET. Atherioscler Thromb Vasc Biol 28:1311–1317
Schmitz SA, Winterhalter S, Schiffler S, Gust R, Wagner S, Kresse M et al (2001) USPIO-enhanced direct MR imaging of thrombus: preclinical evaluation in rabbits. Radiology 221(1):237–243
Acknowledgments
Grants: National Natural Science Grant of China (30870733,30972810).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ma, X., Zhao, Q., Zhao, L. et al. In vivo MR imaging of plaque disruption and thrombus formation in an atherosclerotic rabbit model. Int J Cardiovasc Imaging 28, 577–586 (2012). https://doi.org/10.1007/s10554-011-9854-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-011-9854-x