Abstract
Purpose
High mammographic breast density is a strong, well-established breast cancer risk factor. Whether stem cells may explain high breast cancer risk in dense breasts is unknown. We investigated the association between breast density and breast cancer risk by the status of stem cell markers CD44, CD24, and ALDH1A1 in the tumor.
Methods
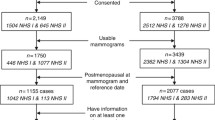
We included 223 women with primary invasive or in situ breast cancer and 399 age-matched controls from Mayo Clinic Mammography Study. Percent breast density (PD), absolute dense area (DA), and non-dense area (NDA) were assessed using computer-assisted thresholding technique. Immunohistochemical analysis of the markers was performed on tumor tissue microarrays according to a standard protocol. We used polytomous logistic regression to quantify the associations of breast density measures with breast cancer risk across marker-defined tumor subtypes.
Results
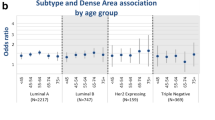
Of the 223 cancers in the study, 182 were positive for CD44, 83 for CD24 and 52 for ALDH1A1. Associations of PD were not significantly different across t marker-defined subtypes (51% + vs. 11–25%: OR 2.83, 95% CI 1.49–5.37 for CD44+ vs. OR 1.87, 95% CI 0.47–7.51 for CD44−, p-heterogeneity = 0.66; OR 2.80, 95% CI 1.27–6.18 for CD24+ vs. OR 2.44, 95% CI 1.14–5.22 for CD24−, p-heterogeneity = 0.61; OR 3.04, 95% CI 1.14–8.10 for ALDH1A1+ vs. OR 2.57. 95% CI 1.30–5.08 for ALDH1A1−, p-heterogeneity = 0.94). Positive associations of DA and inverse associations of NDA with breast cancer risk were similar across marker-defined subtypes.
Conclusions
We found no evidence of differential associations of breast density with breast cancer risk by the status of stem cell markers. Further studies in larger study populations are warranted to confirm these associations.
Similar content being viewed by others
References
McCormack VA, dos Santos Silva I (2006) Breast density and parenchymal patterns as markers of breast cancer risk: a meta-analysis. Cancer Epidemiol Biomark Prev 15:1159–1169
Vachon CM, Kuni CC, Anderson K, Anderson VE, Sellers TA (2000) Association of mammographically defined percent breast density with epidemiologic risk factors for breast cancer (United States). Cancer Causes Control 11:653–662
Vachon CM, Sellers TA, Vierkant RA, Wu FF, Brandt KR (2002) Case–control study of increased mammographic breast density response to hormone replacement therapy. Cancer Epidemiol Biomark Prev 11:1382–1388
Titus-Ernstoff L, Tosteson AN, Kasales C, Weiss J, Goodrich M, Hatch EE, Carney PA (2006) Breast cancer risk factors in relation to breast density (United States). Cancer Causes Control 17:1281–1290
Tamimi RM, Hankinson SE, Colditz GA, Byrne C (2005) Endogenous sex hormone levels and mammographic density among postmenopausal women. Cancer Epidemiol Biomark Prev 14:2641–2647
Yaghjyan L, Colditz GA, Rosner B, Bertrand KA, Tamimi RM (2016) Reproductive factors related to childbearing and mammographic breast density. Breast Cancer Res Treat 158:351–359
Cobaleda C, Cruz JJ, Gonzalez-Sarmiento R, Sanchez-Garcia I, Perez-Losada J (2008) The emerging picture of human breast cancer as a stem cell-based disease. Stem Cell Rev 4:67–79
Smalley M, Ashworth A (2003) Stem cells and breast cancer: a field in transit. Nat Rev Cancer 3:832–844
Stingl J, Eirew P, Ricketson I, Shackleton M, Vaillant F, Choi D, Li HI, Eaves CJ (2006) Purification and unique properties of mammary epithelial stem cells. Nature 439:993–997
Trichopoulos D, Adami HO, Ekbom A, Hsieh CC, Lagiou P (2008) Early life events and conditions and breast cancer risk: from epidemiology to etiology. Int J Cancer 122:481–485
Savarese TM, Low HP, Baik I, Strohsnitter WC, Hsieh CC (2006) Normal breast stem cells, malignant breast stem cells, and the perinatal origin of breast cancer. Stem Cell Rev 2:103–110
Giatromanolaki A, Sivridis E, Fiska A, Koukourakis M (2011) The CD44+/CD24− phenotype relates to ‘triple-negative’ state and unfavorable prognosis in breast cancer patients. Med Oncolgy 28(3):745–752
Abraham BK, Fritz P, Van der Kuip H, Buck M, Szabo Z, Athelogou M, and Brauch H (2005) Evaluation of CD44+/CD24−/low cells in breast cancer and relevance for distant metastasis. AACR Meeting Abstracts, p 481
Neumeister V, Agarwal S, Bordeaux J, Camp RL, Rimm DL (2010) In situ identification of putative cancer stem cells by multiplexing ALDH1, CD44, and cytokeratin identifies breast cancer patients with poor prognosis. Am J Pathol 176:2131–2138
Eden JA (2010) Human breast cancer stem cells and sex hormones–a narrative review. Menopause 17:801–810
Ginestier C, Hur MH, Charafe-Jauffret E, Monville F, Dutcher J, Brown M, Jacquemier J, Viens P, Kleer CG, Liu S, Schott A, Hayes D, Birnbaum D, Wicha MS, Dontu G (2007) ALDH1 is a marker of normal and malignant human mammary stem cells and a predictor of poor clinical outcome. Cell Stem Cell 1:555–567
Liu Y, Lv DL, Duan JJ, Xu SL, Zhang JF, Yang XJ, Zhang X, Cui YH, Bian XW, Yu SC (2014) ALDH1A1 expression correlates with clinicopathologic features and poor prognosis of breast cancer patients: a systematic review and meta-analysis. BMC Cancer 14:444
Yaghjyan L, Stoll E, Ghosh K, Scott CG, Jensen MR, Brandt KR, Visscher D, Vachon CM (2017) Tissue-based associations of mammographic breast density with breast stem cell markers. Breast Cancer Res 19:100
Vachon CM, Brandt KR, Ghosh K, Scott CG, Maloney SD, Carston MJ, Pankratz VS, Sellers TA (2007) Mammographic breast density as a general marker of breast cancer risk. Cancer Epidemiol Biomark Prev 16:43–49
Bertrand KA, Tamimi RM, Scott CG, Jensen MR, Pankratz VS, Visscher D, Norman A, Couch F, Shepherd J, Fan B, Chen Y-Y, Ma L, Beck AH, Cummings SR, Kerlikowske K, Vachon CM (2013) Mammographic density and risk of breast cancer by age and tumor characteristics. Breast Cancer Res 15:R104
Ursin G, Ma H, Wu AH, Bernstein L, Salane M, Parisky YR, Astrahan M, Siozon CC, Pike MC (2003) Mammographic density and breast cancer in three ethnic groups. Cancer Epidemiol Biomark Prev 12:332–338
Byng JW, Boyd NF, Fishell E, Jong RA, Yaffe MJ (1994) The quantitative analysis of mammographic densities. Phys Med Biol 39:1629–1638
Boyd NF, Byng JW, Jong RA, Fishell EK, Little LE, Miller AB, Lockwood GA, Tritchler DL, Yaffe MJ (1995) Quantitative classification of mammographic densities and breast cancer risk: results from the Canadian National Breast Screening Study. J Natl Cancer Inst 87:670–675
Phipps AI, Buist DS, Malone KE, Barlow WE, Porter PL, Kerlikowske K, O’Meara ES, Li CI (2012) Breast density, body mass index, and risk of tumor marker-defined subtypes of breast cancer. Ann Epidemiol 22:340–348
Ziv E, Tice J, Smith-Bindman R, Shepherd J, Cummings S, Kerlikowske K (2004) Mammographic density and estrogen receptor status of breast cancer. Cancer Epidemiol Biomark Prev 13:2090–2095
Cerhan JR, Sellers TA, Janney CA, Pankratz VS, Brandt KR, Vachon CM (2005) Prenatal and perinatal correlates of adult mammographic breast density. Cancer Epidemiol Biomark Prev 14:1502–1508
Ginestier C, Wicha MS (2007) Mammary stem cell number as a determinate of breast cancer risk. Breast Cancer Res 9:109
Xue F, Michels KB (2007) Intrauterine factors and risk of breast cancer: a systematic review and meta-analysis of current evidence. Lancet Oncol 8:1088–1100
Rice MS, Tamimi RM, Connolly JL, Collins LC, Shen D, Pollak MN, Rosner B, Hankinson SE, Tworoger SS (2012) Insulin-like growth factor-1, insulin-like growth factor binding protein-3 and lobule type in the nurses’ health study II. Breast Cancer Res 14:1–7
Christopoulos PF, Msaouel P, Koutsilieris M (2015) The role of the insulin-like growth factor-1 system in breast cancer. Mol Cancer 14:43
Rinaldi S, Peeters PHM, Berrino F, Dossus L, Biessy C, Olsen A, Tjonneland A, Overvad K, Clavel-Chapelon F, Boutron-Ruault MC, Téhard B, Nagel G, Linseisen J, Boeing H, Lahmann PH, Trichopoulou A, Trichopoulos D, Koliva M, Palli D, Panico S, Tumino R, Sacerdote C, van Gils CH, van Noord P, Grobbee DE, Bueno-de-Mesquita HB, Gonzalez CA, Agudo A, Chirlaque MD, Barricarte A, Larrañaga N, Quiros JR, Bingham S, Khaw KT, Key T, Allen NE, Lukanova A, Slimani N, Saracci R, Riboli E, Kaaks R (2006) IGF-I, IGFBP-3 and breast cancer risk in women: the European prospective investigation into cancer and nutrition (EPIC). Endocr Relat Cancer 13:593–605
Baer HJ, Colditz GA, Willett WC, Dorgan JF (2007) Adiposity and sex hormones in girls. Cancer Epidemiol Biomark Prev 16:1880–1888
Bertrand KA, Baer HJ, Orav EJ, Klifa C, Shepherd JA, Van Horn L, Snetselaar L, Stevens VJ, Hylton NM, Dorgan JF (2015) Body fatness during childhood and adolescence and breast density in young women: a prospective analysis. Breast Cancer Res 17:1–10
Poole EM, Tworoger SS, Hankinson SE, Schernhammer ES, Pollak MN, Baer HJ (2011) Body size in early life and adult levels of insulin-like growth factor 1 and insulin-like growth factor binding protein 3. Am J Epidemiol 174:642–651
Warner ET, Eliassen AH, Chen WY, Holmes MD, Willett WC, Tamimi RM (2013) Abstract 130: childhood and adolescent body size and risk of fatal breast cancer. Cancer Res 73:130
Baer HJ, Colditz GA, Rosner B, Michels KB, Rich-Edwards JW, Hunter DJ, Willett WC (2005) Body fatness during childhood and adolescence and incidence of breast cancer in premenopausal women: a prospective cohort study. Breast Cancer Res 7:1–12
Palmer JR, Adams-Campbell LL, Boggs DA, Wise LA, Rosenberg L (2007) A prospective study of body size and breast cancer in black women. Cancer Epidemiol Biomark Prev 16:1795–1802
Frazier AL, Rosenberg SM (2013) Pre-adolescent and adolescent risk factors for benign breast disease. J Adolesc Health 52:S36–S40
Warner ET, Hu R, Collins LC, Beck AH, Schnitt S, Rosner B, Eliassen AH, Michels KB, Willett WC, Tamimi RM (2016) Height and body size in childhood, adolescence, and young adulthood and breast cancer risk according to molecular Subtype in the nurses’ health studies. Cancer Prev Res 9:732–738
Woolcott CG, Koga K, Conroy SM, Byrne C, Nagata C, Ursin G, Vachon CM, Yaffe MJ, Pagano I, Maskarinec G (2012) Mammographic density, parity and age at first birth, and risk of breast cancer: an analysis of four case–control studies. Breast Cancer Res Treat 132:1163–1171
Yaghjyan L, Mahoney MC, Succop P, Wones R, Buckholz J, Pinney SM (2012) Relationship between breast cancer risk factors and mammographic breast density in the Fernald Community Cohort. Br J Cancer 106(5):996–1003
Anwar T, Kleer CG (2013) Tissue-based identification of stem cells and epithelial-to-mesenchymal transition in breast cancer. Hum Pathol 44:1457–1464
Collins LC, Marotti J, Baer HJ, Deitz AC, Colditz GA, Tamimi RM (2008) Comparison of estrogen receptor assay results from pathology reports with results from central laboratory testing: implications for population-based studies of breast cancer. J Natl Cancer Inst 100:218–221
Ma H, Wang Y, Sullivan-Halley J, Weiss L, Burkman RT, Simon MS, Malone KE, Strom BL, Ursin G, Marchbanks PA, McDonald JA, Spirtas R, Press MF, Bernstein L (2009) Breast cancer receptor status: do results from a centralized pathology laboratory agree with SEER registry reports? Cancer Epidemiol Biomark Prev 18:2214–2220
Ahern TP, Beck AH, Rosner BA, Glass B, Frieling G, Collins LC, Tamimi RM (2017) Continuous measurement of breast tumour hormone receptor expression: a comparison of two computational pathology platforms. J Clin Pathol 70(5):428–434
Acknowledgments
This study was funded by the University of Florida Cancer Center through the Florida Consortium of National Cancer Institute Centers Program at the University of Florida (Bridge Funding to L.Y.); and Mayo Clinic Breast SPORE (NCI P50 CA116201) and National Cancer Institute (R01 CA128931; R01 CA140286). The authors would like to thank Ms. Elaine Dooley for performing immunohistochemical analyses for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
This study was compliant with the U.S. Health Insurance Portability and Accountability Act and was approved by the Mayo Clinic Institutional Review Board (IRB) which issued a waiver of informed consent as well as the University of Florida IRBs. The Mayo Clinic patients provided a general authorization for use of medical record information for research purposes.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yaghjyan, L., Esnakula, A.K., Scott, C.G. et al. Associations of mammographic breast density with breast stem cell marker-defined breast cancer subtypes. Cancer Causes Control 30, 1103–1111 (2019). https://doi.org/10.1007/s10552-019-01207-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-019-01207-w