Abstract
Background
The dominant invasive breast cancer histologic subtype, ductal carcinoma, shows intrinsic subtype diversity. However, lobular breast cancers are predominantly Luminal A. Both histologic subtypes show distinct relationships with patient and tumor characteristics, but it is unclear if these associations remain after accounting for intrinsic subtype.
Methods
Generalized linear models were used to estimate relative frequency differences (RFDs) and 95% confidence intervals (95% CIs) for the associations between age, race, tumor characteristics, immunohistochemistry (IHC) and RNA-based intrinsic subtype, TP53 status, and histologic subtype in the Carolina Breast Cancer Study (CBCS, n = 3,182) and The Cancer Genome Atlas (TCGA, n = 808).
Results
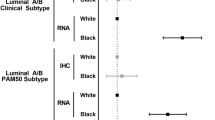
Relative to ductal tumors, lobular tumors were significantly more likely to be Luminal A [CBCS RNA RFD: 44.9%, 95% CI (39.6, 50.1); TCGA: RFD: 50.5%, 95% CI (43.9, 57.1)], were less frequent among young (≤ 50 years) and black women, were larger in size, low grade, less frequently had TP53 pathway defects, and were diagnosed at later stages. These associations persisted among Luminal A tumors (n = 242).
Conclusions
While histology is strongly associated with molecular characteristics, histologic associations with age, race, size, grade, and stage persisted after restricting to Luminal A subtype. Histology may continue to be clinically relevant among Luminal A breast cancers.

Similar content being viewed by others
References
Arps DP, Healy P, Zhao L et al (2013) Invasive ductal carcinoma with lobular features: a comparison study to invasive ductal and invasive lobular carcinomas of the breast. Breast Cancer Res Treat 138:719–726. https://doi.org/10.1007/s10549-013-2493-2
Makki J (2015) Diversity of breast carcinoma: histological subtypes and clinical relevance. Clin Med Insights Pathol 8:23–31. https://doi.org/10.4137/CPath.S31563.TYPE
Rosen PP (2009) Rosen’s breast pathology, 3rd edn. Lippincott Williams & Wilkins, Phildelphia
Arpino G, Bardou VJ, Clark GM, Elledge RM (2004) Infiltrating lobular carcinoma of the breast: tumor characteristics and clinical outcome. Breast Cancer Res 6:R149–R156. https://doi.org/10.1186/bcr767
Cristofanilli M, Gonzalez-Angulo A, Sneige N et al (2005) Invasive lobular carcinoma classic type: response to primary chemotherapy and survival outcomes. J Clin Oncol 23:41–48. https://doi.org/10.1200/JCO.2005.03.111
Li CI, Uribe DJ, Daling JR (2005) Clinical characteristics of different histologic types of breast cancer. Br J Cancer 93:1046–1052. https://doi.org/10.1038/sj.bjc.6602787
Li CI (2010) Risk of mortality by histologic type of breast cancer in the United States. Horm Cancer 1:156–165. https://doi.org/10.1007/s12672-010-0016-8
Pestalozzi BC, Zahrieh D, Mallon E et al (2008) Distinct clinical and prognostic features of infiltrating lobular carcinoma of the breast: combined results of 15 International Breast Cancer Study Group clinical trials. J Clin Oncol 26:3006–3014. https://doi.org/10.1200/JCO.2007.14.9336
Phipps AI, Li CI, Kerlikowske K et al (2010) Risk factors for ductal, lobular, and mixed ductal-lobular breast cancer in a screening population. Cancer Epidemiol Biomarkers Prev 19:1643–1654. https://doi.org/10.1158/1055-9965.EPI-10-0188
Rakha EA, Gill MS, El-Sayed ME et al (2009) The biological and clinical characteristics of breast carcinoma with mixed ductal and lobular morphology. Breast Cancer Res Treat 114:243–250. https://doi.org/10.1007/s10549-008-0007-4
Zengel B, Yararbas U, Duran A et al (2015) Comparison of the clinicopathological features of invasive ductal, invasive lobular, and mixed (invasive ductal + invasive lobular) carcinoma of the breast. Breast Cancer 22:374–381. https://doi.org/10.1007/s12282-013-0489-8
Metzger Filho O, Giobbie-Hurder A, Mallon E et al (2015) Relative effectiveness of letrozole compared with tamoxifen for patients with lobular carcinoma in the BIG 1–98 Trial. J Clin Oncol 33:2772–2779. https://doi.org/10.1200/JCO.2015.60.8133
Badowska-Kozakiewicz AM, Patera J, Sobol M, Przybylski J (2015) The role of oestrogen and progesterone receptors in breast cancer—immunohistochemical evaluation of oestrogen and progesterone receptor expression in invasive breast cancer in women. Współczesna Onkol 3:220–225. https://doi.org/10.5114/wo.2015.51826
Azim HA, Malek RA, Azim HA (2014) Pathological features and prognosis of lobular carcinoma in Egyptian breast cancer patients. Womens Health (Lond Engl) 10:511–518. https://doi.org/10.2217/whe.14.48
Biglia N, Maggiorotto F, Liberale V et al (2013) Clinical-pathologic features, long term-outcome and surgical treatment in a large series of patients with invasive lobular carcinoma (ILC) and invasive ductal carcinoma (IDC). Eur J Surg Oncol 39:455–460. https://doi.org/10.1016/j.ejso.2013.02.007
Braunstein LZ, Brock JE, Chen Y-H et al (2015) Invasive lobular carcinoma of the breast: local recurrence after breast-conserving therapy by subtype approximation and surgical margin. Breast Cancer Res Treat 149:555–564. https://doi.org/10.1007/s10549-015-3273-y
Cha YJ, Jung WH, Cho NH, Koo JS (2015) Expression of sarcosine metabolism-related proteins in invasive lobular carcinoma: comparison to invasive ductal carcinoma. Yonsei Med J 56:598–607. https://doi.org/10.3349/ymj.2015.56.3.598
Delpech Y, Coutant C, Hsu L et al (2013) Clinical benefit from neoadjuvant chemotherapy in oestrogen receptor-positive invasive ductal and lobular carcinomas. Br J Cancer 108:285–291. https://doi.org/10.1038/bjc.2012.557
García-Fernández A, Lain JM, Chabrera C et al (2015) Comparative long-term study of a large series of patients with invasive ductal carcinoma and invasive lobular carcinoma. Loco-regional recurrence, metastasis, and survival. Breast J 21:533–537. https://doi.org/10.1111/tbj.12455
Kwast ABG, Groothuis-Oudshoorn KCGM, Grandjean I et al (2012) Histological type is not an independent prognostic factor for the risk pattern of breast cancer recurrences. Breast Cancer Res Treat 135:271–280. https://doi.org/10.1007/s10549-012-2160-z
Rakha E, El-Sayed ME, Menon S et al (2008) Histologic grading is an independent prognostic factor in invasive lobular carcinoma of the breast. Breast Cancer Res Treat 111:121–127. https://doi.org/10.1007/s10549-007-9768-4
Jung S-Y, Jeong J, Shin S-H et al (2010) The invasive lobular carcinoma as a prototype luminal A breast cancer: a retrospective cohort study. BMC Cancer 10:664. https://doi.org/10.1186/1471-2407-10-664
Bharat A, Gao F, Margenthaler JA (2009) Tumor characteristics and patient outcomes are similar between invasive lobular and mixed invasive ductal/lobular breast cancers but differ from pure invasive ductal breast cancers. Am J Surg 198:516–519. https://doi.org/10.1016/j.amjsurg.2009.06.005
Suryadevara A, Paruchuri LP, Banisaeed N et al (2010) The clinical behavior of mixed ductal/lobular carcinoma of the breast: a clinicopathologic analysis. World J Surg Oncol 8:51. https://doi.org/10.1186/1477-7819-8-51
Conners AL, Jones KN, Hruska CB et al (2015) Direct-conversion molecular breast imaging of invasive breast cancer: imaging features, extent of invasive disease, and comparison between invasive ductal and lobular histology. Am J Roentgenol 205:W374–W381. https://doi.org/10.2214/AJR.14.13502
Tavassoli F, Schnitt SJ, Hoefler H et al (2003) Intraductal proliferative lesions. In: Tavassoli F, Devilee P (eds) World Health Organization classification of tumours. Pathology and genetics of tumours of the breast and female genital organs. IARC Press, Lyon, pp 63–74
Vlug E, Ercan C, van der Wall E et al (2014) Lobular breast cancer: pathology, biology, and options for clinical intervention. Arch Immunol Ther Exp (Warsz) 62:7–21. https://doi.org/10.1007/s00005-013-0251-0
Weiss A, Chang DC (2016) A comparison of breast-specific gamma imaging of invasive lobular carcinomas and ductal carcinomas. JAMA Surg 150(8):815–816. https://doi.org/10.1001/jamasurg.2015.0962
Langlands F, White J, Kearins O et al (2015) Contralateral breast cancer: incidence according to ductal or lobular phenotype of the primary. Clin Radiol 71:159–163. https://doi.org/10.1016/j.crad.2015.10.030
Kanumuri P, Hayse B, Killelea BK et al (2015) Characteristics of Multifocal and multicentric breast cancers. Ann Surg Oncol 22:2475–2482. https://doi.org/10.1245/s10434-015-4430-6
Arps DP, Jorns JM, Zhao L et al (2014) Re-excision rates of invasive ductal carcinoma with lobular features compared with invasive ductal carcinomas and invasive lobular carcinomas of the breast. Ann Surg Oncol 21:4152–4158. https://doi.org/10.1245/s10434-014-3871-7
Cao A-Y, Huang L, Wu J et al (2012) Tumor characteristics and the clinical outcome of invasive lobular carcinoma compared to infiltrating ductal carcinoma in a Chinese population. World J Surg Oncol 10:152. https://doi.org/10.1186/1477-7819-10-152
Ciriello G, Gatza ML, Beck AH et al (2015) Comprehensive molecular portraits of invasive lobular breast cancer. Cell 163:506–519. https://doi.org/10.1016/j.cell.2015.09.033
Newman B, Moorman PG, Millikan R et al (1995) The Carolina Breast Cancer Study: integrating population-based epidemiology and molecular biology. Breast Cancer Res Treat 35:51–60
Moorman PG, Millikan RC, Newman B (2001) Oral contraceptives and breast cancer among African-American women and White women. J Natl Med Assoc 93:329–334
The Cancer Genome Atlas Network (2012) Comprehensive molecular portraits of human breast tumors. Nature 490:61–70. https://doi.org/10.1038/nature11412.Comprehensive
Carey LA, Perou CM, Livasy CA et al (2006) Race, breast cancer subtypes, and survival in the Carolina Breast Cancer Study. JAMA 295:2492–2502. https://doi.org/10.1001/jama.295.21.2492
O’Brien KM, Cole SR, Tse C-K et al (2010) Intrinsic breast tumor subtypes, race, and long-term survival in the Carolina Breast Cancer Study. Clin Cancer Res 16:6100–6110. https://doi.org/10.1158/1078-0432.CCR-10-1533
Allott EH, Cohen SM, Geradts J et al (2016) Performance of three-biomarker immunohistochemistry for intrinsic breast cancer subtyping in the AMBER consortium. Cancer Epidemiol Biomarkers Prev 25:470–478. https://doi.org/10.1158/1055-9965.EPI-15-0874
Parker JS, Mullins M, Cheang MCU et al (2009) Supervised risk predictor of breast cancer based on intrinsic subtypes. J Clin Oncol 27:1160–1167. https://doi.org/10.1200/JCO.2008.18.1370
Troester MA, Herschkowitz JI, Oh DS et al (2006) Gene expression patterns associated with p53 status in breast cancer. BMC Cancer 6:276. https://doi.org/10.1186/1471-2407-6-276
Williams LA, Butler EN, Sun X et al (2018) TP53 protein levels, RNA-based pathway assessment, and race among invasive breast cancer cases. NPJ Breast Cancer June 25:4:13. https://doi.org/10.1038/s41523-018-0067-5
Taylor NJ, Nikolaishvili-Feinberg N, Midkiff BR et al (2015) Rational manual and automated scoring thresholds for the immunohistochemical detection of TP53 missense mutations in human breast carcinomas. Appl Immunohistochem Mol Morphol 24:1–7
Spiegelman D, Hertzmark E (2005) Easy SAS calculations for risk or prevalence ratios and differences. Am J Epidemiol 162:199–200. https://doi.org/10.1093/aje/kwi188
Furberg H, Millikan R, Dressler L et al (2001) Tumor characteristics in African American and white women. Breast Cancer Res Treat 68(1):33–43
Iorfida M, Maiorano E, Orvieto E et al (2012) Invasive lobular breast cancer: subtypes and outcome. Breast Cancer Res Treat 133:713–723. https://doi.org/10.1007/s10549-012-2002-z
Caldarella A, Buzzoni C, Crocetti E et al (2013) Invasive breast cancer: a significant correlation between histological types and molecular subgroups. J Cancer Res Clin Oncol 139:617–623. https://doi.org/10.1007/s00432-012-1365-1
Lim ST, Yu JH, Park HK et al (2014) A comparison of the clinical outcomes of patients with invasive lobular carcinoma and invasive ductal carcinoma of the breast according to molecular subtype in a Korean population. World J Surg Oncol 12:56. https://doi.org/10.1186/1477-7819-12-56
Engstrøm MJ, Opdahl S, Vatten LJ et al (2015) Invasive lobular breast cancer: the prognostic impact of histopathological grade, E-cadherin and molecular subtypes. Histopathology 66:409–419. https://doi.org/10.1111/his.12572
Lips EH, Mukhtar R, Yau C et al (2012) Lobular histology and response to neoadjuvant chemotherapy in invasive breast cancer. Breast Cancer Res Treat 136:35–43. https://doi.org/10.1007/s10549-012-2233-z
Sisti JS, Collins LC, Beck AH et al (2016) Reproductive risk factors in relation to molecular subtypes of breast cancer: results from the nurses’ health studies. Int J Cancer 138:2346–2356. https://doi.org/10.1002/ijc.29968
Cha YJ, Kim YH, Cho NH, Koo JS (2014) Expression of autophagy related proteins in invasive lobular carcinoma: comparison to invasive ductal carcinoma. Int J Clin Exp Pathol 7:3389–3398
Acknowledgments
We would like to thank that participants who generously participated in these studies. This work was supported by the Komen Graduate Training and Disparities Research Training Grant (LAW); Komen Career Catalyst Grant (CCR16376756) (KAH); National Institutes of Health: P50 CA058223 and U01 CA179715 (AFO and MAT); R01 HG009125, P01 CA142538, and P30 ES010126 (MIL), and U54 CA156733 (MAT), R01 CA19575401 (CMP).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Williams, L.A., Hoadley, K.A., Nichols, H.B. et al. Differences in race, molecular and tumor characteristics among women diagnosed with invasive ductal and lobular breast carcinomas. Cancer Causes Control 30, 31–39 (2019). https://doi.org/10.1007/s10552-018-1121-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-018-1121-1