Abstract
Objective
To examine if survival has changed over the last 20 years in patients with base of tongue and tonsil cancers in the United States.
Methods
Using SEER data, we employed Kaplan–Meier method to draw survival curves and calculate survival rates, and estimated adjusted hazard ratios (HR).
Results
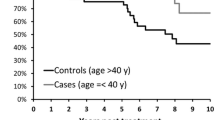
From the 1980s to the 2000s, the 5-year overall survival rates statistically significantly improved by 100% from 25 to 51% among patients with one primary base of tongue cancer and 28–60% among those with one primary tonsil cancer (p values for trend <0.001). In addition, the 5-year cancer-specific survival improved by 222.4 and 276%, respectively, among two types of patients. Survival improvement was more pronounced among male patients than among female patients regardless of young or old age, while the improvement was generally consistent among patients with different tumor stages and treatment methods. In contrast, however, those patients with subsequent multiple cancers showed no improvement in overall survival over time.
Conclusions
The survival of patients with base of tongue and tonsil cancer has significantly improved over the last decades in the United States. Whether the improvement is associated with HPV infection, screening, or early detection is worthy to study in future.





Similar content being viewed by others
References
Ryerson AB, Peters ES, Coughlin SS et al (2008) Burden of potentially human papillomavirus-associated cancers of the oropharynx and oral cavity in the US, 1998–2003. Cancer 113:2901–2909
Schantz SP, Yu GP (2002) Head and neck cancer incidence trends in young Americans, 1973–1997, with a special analysis for tongue cancer. Arch Otolaryngol Head Neck Surg 128:268–274
Shiboski CH, Schmidt BL, Jordan RC (2005) Tongue and tonsil carcinoma: increasing trends in the US population ages 20–44 years. Cancer 103:1843–1849
Frisch M, Hjalgrim H, Jaeger AB, Biggar RJ (2000) Changing patterns of tonsillar squamous cell carcinoma in the United States. Cancer Causes Control 11:489–495
Kingsley K, O’Malley S, Ditmyer M, Chino M (2008) Analysis of oral cancer epidemiology in the US reveals state-specific trends: implications for oral cancer prevention. BMC Public Health 8:87
Mellin H, Friesland S, Lewensohn R, Dalianis T, Munck-Wikland E (2000) Human papillomavirus (HPV) DNA in tonsillar cancer: clinical correlates, risk of relapse, and survival. Int J Cancer 89:300–304
Kreimer AR, Clifford GM, Boyle P, Franceschi S (2005) Human papillomavirus types in head and neck squamous cell carcinomas worldwide: a systematic review. Cancer Epidemiol Biomark Prev 14:467–475
Attner P, Du J, Nasman A et al (2010) The role of human papillomavirus in the increased incidence of base of tongue cancer. Int J Cancer 126:2879–2884
Dunne EF, Unger ER, Sternberg M et al (2007) Prevalence of HPV infection among females in the United States. JAMA 297:813–819
Dahlgren L, Dahlstrand HM, Lindquist D et al (2004) Human papillomavirus is more common in base of tongue than in mobile tongue cancer and is a favorable prognostic factor in base of tongue cancer patients. Int J Cancer 112:1015–1019
af Geijersstam V, Wang Z, Lewensohn-Fuchs I et al (1998) Trends in seroprevalence of human papillomavirus type 16 among pregnant women in Stockholm, Sweden, during 1969–1989. Int J Cancer 76:341–344
Zhen W, Karnell LH, Hoffman HT et al (2004) The National Cancer Data Base report on squamous cell carcinoma of the base of tongue. Head Neck 26:660–674
Brunin F, Mosseri V, Jaulerry C et al (1999) Cancer of the base of the tongue: past and future. Head Neck 21:751–759
Ritchie JM, Smith EM, Summersgill KF et al (2003) Human papillomavirus infection as a prognostic factor in carcinomas of the oral cavity and oropharynx. Int J Cancer 104:336–344
Schwartz SR, Yueh B, McDougall JK, Daling JR, Schwartz SM (2001) Human papillomavirus infection and survival in oral squamous cell cancer: a population-based study. Otolaryngol Head Neck Surg 125:1–9
Ang KK, Harris J, Wheeler R et al (2010) Human papillomavirus and survival of patients with oropharyngeal cancer. N Engl J Med 363:24–35
Fakhry C, Westra WH, Li S et al (2008) Improved survival of patients with human papillomavirus-positive head and neck squamous cell carcinoma in a prospective clinical trial. J Natl Cancer Inst 100:261–269
Lam L, Logan RM, Luke C (2006) Epidemiological analysis of tongue cancer in South Australia for the 24-year period, 1977–2001. Aust Dent J 51:16–22
Chaturvedi AK, Engels EA, Anderson WF, Gillison ML (2008) Incidence trends for human papillomavirus-related and -unrelated oral squamous cell carcinomas in the United States. J Clin Oncol 26:612–619
Surveillance, Epidemiology, and End Results (SEER) Program (www.seer.cancer.gov) SEER*Stat Database: incidence—SEER 17 Regs limited-use + Hurricane Katrina Impacted Louisiana Cases, Nov 2008 Sub (1973–2006 varying), National Cancer Institute, DCCPS, Surveillance Research Program, Cancer Statistics Branch, released April 2009, based on the November 2008 submission
Spiegelman D, Hertzmark E (2005) Easy SAS calculations for risk or prevalence ratios and differences. Am J Epidemiol 162:199–200
Shiboski CH, Shiboski SC, Silverman S Jr (2000) Trends in oral cancer rates in the United States, 1973–1996. Community Dent Oral Epidemiol 28:249–256
Cosetti M, Yu GP, Schantz SP (2008) Five-year survival rates and time trends of laryngeal cancer in the US population. Arch Otolaryngol Head Neck Surg 134:370–379
Carvalho AL, Nishimoto IN, Califano JA, Kowalski LP (2005) Trends in incidence and prognosis for head and neck cancer in the United States: a site-specific analysis of the SEER database. Int J Cancer 114:806–816
Altekruse SF, Kosary CL, Krapcho M, Neyman N, Aminou R, Waldron W et al (eds) (2010) SEER cancer statistics review, 1975–2007, National Cancer Institute. Bethesda, MD, http://seer.cancer.gov/csr/1975_2007/, based on November 2009 SEER data submission, posted to the SEER web site, 2010
US Department of Health and Human Services (1994) Preventing tobacco use among young people: a report of the surgeon general. US Dept of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking on Health, Atlanta
Centers for Disease Control and Prevention (CDC) (2002) Cigarette smoking among adults—United States, 2000. MMWR Morb Mortal Wkly Rep 51:642–645
Kujan O, Glenny AM, Duxbury J, Thakker N, Sloan P (2005) Evaluation of screening strategies for improving oral cancer mortality: a Cochrane systematic review. J Dent Educ 69:255–265
Cruz GD, Ostroff JS, Kumar JV, and Gajendra S (2005) Preventing and detecting oral cancer. Oral health care providers’ readiness to provide health behavior counseling and oral cancer examinations. J Am Dent Assoc 136:594–601. (quiz 681–682)
Netuveli G, Sheiham A, Watt RG (2006) Does the ‘inverse screening law’ apply to oral cancer screening and regular dental check-ups? J Med Screen 13:47–50
Pinto LH, Canary PC, Araujo CM, Bacelar SC, Souhami L (1991) Prospective randomized trial comparing hyperfractionated versus conventional radiotherapy in stages III and IV oropharyngeal carcinoma. Int J Radiat Oncol Biol Phys 21:557–562
Horiot JC, Le Fur R, N’Guyen T et al (1992) Hyperfractionation versus conventional fractionation in oropharyngeal carcinoma: final analysis of a randomized trial of the EORTC cooperative group of radiotherapy. Radiother Oncol 25:231–241
Harrison LB, Lee HJ, Pfister DG et al (1998) Long term results of primary radiotherapy with/without neck dissection for squamous cell cancer of the base of tongue. Head Neck 20:668–673
Mendenhall WM, Stringer SP, Amdur RJ et al (2000) Is radiation therapy a preferred alternative to surgery for squamous cell carcinoma of the base of tongue? J Clin Oncol 18:35–42
Bourhis J, Le Maitre A, Baujat B, Audry H, Pignon JP (2007) Individual patients’ data meta-analyses in head and neck cancer. Curr Opin Oncol 19:188–194
Pignon JP, Bourhis J, Domenge C, Designe L (2000) Chemotherapy added to locoregional treatment for head and neck squamous-cell carcinoma: three meta-analyses of updated individual data. MACH-NC Collaborative Group. Meta-analysis of chemotherapy on head and neck cancer. Lancet 355:949–955
Pignon JP, le Maitre A, Bourhis J (2007) Meta-Analyses of Chemotherapy in Head and Neck Cancer (MACH-NC): an update. Int J Radiat Oncol Biol Phys 69:S112–S114
Budach W, Hehr T, Budach V, Belka C, Dietz K (2006) A meta-analysis of hyperfractionated and accelerated radiotherapy and combined chemotherapy and radiotherapy regimens in unresected locally advanced squamous cell carcinoma of the head and neck. BMC Cancer 6:28
Acknowledgments
Drs. Yu and Schantz had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Drs. Yu and Schantz developed study concept and design, interpreted analytic results, and drafted the manuscript. Drs. Zhang and Hashibe criticized and revised the manuscript for important intellectual content.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yu, GP., Mehta, V., Branovan, D. et al. Improved survival among patients with base of tongue and tonsil cancer in the United States. Cancer Causes Control 23, 153–164 (2012). https://doi.org/10.1007/s10552-011-9864-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-011-9864-y