Abstract
Purpose
The contribution of menstrual and reproductive factors to risk of ductal carcinoma (DCIS) of the breast is poorly understood.
Methods
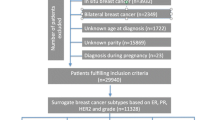
The association between menstrual and reproductive factors and subsequent DCIS risk was examined in Women’s Health Initiative (WHI) clinical trial participants, in which mammography was protocol mandated. The cohort consisted of 64,060 women, among whom 664 cases of DCIS were ascertained over a median follow-up of 12.0 years. Cox proportional hazards models were used to estimate hazard ratios (HR) and 95% confidence intervals (95% CI).
Results
After adjustment for covariates, only older age at menopause (HR ≥ 55 vs. 45–54 : 1.39, 95% CI 1.08–1.79) was significantly associated with risk; however, greater parity (HR ≥ 5 live births vs. 0: 0.70, 95% CI 0.47–1.03), among parous women, and age at first live birth (HR ≥ 30 years relative to <20 years: 1.32, 95% CI 0.92–1.90) were of borderline significance. Age at menarche and months of breast-feeding were not associated with risk. Associations did not differ between high- and low-/moderate-grade DCIS, or by level of body mass index or family history of breast cancer; however, there was a suggestion that the associations of age at menopause, parity, and age at first live birth were limited to women who had ever used hormone therapy.
Conclusions
Findings from this large cohort of postmenopausal women suggest that age at menopause, and possibly, age at first live birth, and parity are associated with risk of DCIS, whereas age at menarche and duration of breast-feeding are not.
Similar content being viewed by others
References
Harris JR, Lippman ME, Veronesi U, Willett WC (1992) Breast cancer (1). N Engl J Med 327:319–328
Kelsey JL, Gammon MD, John EM (1993) Reproductive factors and breast cancer. Epidemiol Rev 15:36–47
Key TJ, Verkasalo PK, Bank E (2001) Epidemiology of breast cancer. Lancet Oncol 2:133–140
Colditz GA, Baer HJ, Tamimi RM Breast cancer. In: Schottenfeld D, Fraumeni JF Jr. (eds) Cancer epidemiology and prevention (3rd edition), New York: Oxford University Press, 2006, pp 995–1012
Pike MC, Spicer DV, Dahmoush L, Press MF (1993) Estrogens, progestogens, normal breast cell proliferation, and breast cancer risk. Epidemiol Rev 15:17–35
Hankinson SE, Colditz GA, Willett WC (2004) Towards an integrated model for breast cancer etiology: the lifelong interplay of genes, lifestyle, and hormones. Breast Cancer Res 6:213–218. doi:10.1186/bcr921
Weiss HA, Brinton LA, Brogan D, Coates RJ, Gammon MD, Malone KE, Schoenberg JB (1996) Epidemiology of in situ and invasive breast cancer in women aged under 45. Br J Cancer 73:1298–1305
Longnecker MP, Bernstein L, Paganini-Hill A, Enger SM, Ross RK (1996) Risk factors for in situ breast cancer. Cancer Epidemiol Biomarkers Prev 5:961–965
Kerlikowske K, Barclay J, Grady D, Sickles EA, Ernster V (1997) Comparison of risk factors for ductal carcinoma in situ and invasive breast cancer. J Natl Cancer Inst 89:76–82
Lambe M, Hsieh C–C, Tsaih S-W, Ekbom A, Trichopoulos D, Adami H-O (1998) Parity, age at first birth and the risk of carcinoma in situ of the breast. Int J Cancer 77:330–332
Trentham-Dietz A, Newcomb PA, Storer BE, Remington PL (2000) Risk factors for carcinoma in situ of the breast. Cancer Epidemiol Biomarkers Prev 9:697–703
Claus EB, Stowe M, Carter D (2001) Breast carcinoma in situ: risk factors and screening patterns. J Natl Cancer Inst 93:1811–1817
Wohlfahrt J, Rank F, Kroman N, Melbye M (2004) A comparison of reproductive risk factors for CIS lesions and invasive breast cnacer. Int J Cancer 108:750–753
Granström C, Sundquist J, Hemminki K (2008) Population attributable risks for breast cancer in Swedish women by morphological type. Breast Cancer Res Treat 111:559–568
Phillips LS, Millikan RC, Schroeder JC, Barnholtz-Sloan JS, Levine BJ (2009) Reproductive and hormonal risk factors for ductal carcinoma in situ of the breast. Cancer Epidemiol Biomarkers Prev 18:1507–1514
Ma J, Henderson KD, Sullivan-Halley J, Duan L, Marshall SF, Ursin G, Horn-Ross P, Largent J, Deapen DM, Lacey JV, Bernstein L (2010) Breast Cancer Res 12:R35 http//:breast-cancer-research.com/content/12/3/R35
Allegra CJ, Aberle DR, Ganschow P et al (2010) National institutes of health state-of-the-science conference statement: diagnosis and management of ductal carcinoma in situ september 22–24, 2009. J Natl Cancer Inst 102(3):161–169
Virnig BA, Tuttle TM, Shamlilyan T, Kane RL (2010) Ductal carcinoma in situ of the breast: a systemic review of incidence, treatment, and outcomes. J Natl Cancer Inst 102(3):170–178
Shackney SE, Silverman JF (2003) Molecular evolutionary patterns of breast cancer. Adv Anat Pathol 10:278–290
Erbas B, Provenzano E, Armes J, Gertig D (2006) The natural history of ductal carcinoma in situ of the breast: a review. Breast Cancer Res Treat 97:135–144
Anderson WF, Chu KC, Devesa SS (2004) Distinct incidence patterns among in situ and invasive breast carcinomas, with possible etiologic implications. Breast Cancer Res Treat 88:149–159
The women’s health initiative study group (1998) Design of the women’s health initiative clinical trial and observational study. Control Clin Trials 19:61–109
Anderson GL, Manson J, Wallace R et al (2003) Implementation of the women’s health initiative study design. Ann Epidemiol 13:S5–S17
Langer RD, White E, Lewis CE, Kotchen JM, Hendrix SL, Trevisan M (2003) The women’s health initiative observational study: baseline characteristics of participants and reliability of baseline measures. Ann Epidemiol 13:S107–S121
Curb JD, McTiernan A, Heckbert SR et al (2003) Outcomes ascertainment and adjudication methods in the Women’s Health Initiative. Ann Epidemiol (9 Suppl): S122-S128
Chlebowski RT, Hendrix SL, Langer RD et al (2003) Influence of estrogen plus progestin on breast cancer and mammography in healthy postmenopausal women: the women’s health initiative randomized trial. JAMA 289:3243–3253
Prentice RL, Caan B, Chlebowski RT et al (2006) Low-fat dietary pattern and risk of invasive breast cancer: the women’s health initiative randomized controlled dietary modification trial. JAMA 295:629–642
Kerlikowske K (2010) Epidemiology of ductal carcinoma in situ. J Natl Cancer Inst Monogr 41:139–141
Kuerer HM, Albarracin CT, Yang WT et al (2008) Ductal carcinoma in situ: state of the science and roadmap to advance the field. J Clin Oncol 27:279–288
Sontag L, Axelrod DE (2005) Evaluation of pathways for progression of heterogeneous breast tumors. J Theor Biol 232:179–189
Dupont WD, Parl FF, Hartmann WH et al (1993) Breast cancer risk associated with proliferative breast disease and atypical hyperplasia. Cancer 71:1258–1265
Carter CL, Corle DK, Micozzi MS, Schatzkin A, Taylor PR (1988) A prospective study of the development of breast cancer in 16, 692 women with benign breast disease. Am J Epidemiol 128:467–477
Lakhani SR, Chaggar R, Davies S et al (1999) Genetic alterations in ‘normal’ luminal and myoepithelial cells of the breast. J Pathol 189:496–503
Kinne DW, Petrek JA, Osborne MP, Fracchia AA, DePaol AA, Rosen PP (1989) Breast carcinoma in situ. Arch Surg 124:33–36
Morrow M, Schnitt SJ, Harris JR (2000) Ductal carcinoma in situ and microinvasive carcinoma. In: Harris JR, Lippman ME, Morrow M, Osborne CK (eds) Diseases of the breast. Lippincott Williams & Wilkins, Philadelphia, pp 383–401
Morrow M (1992) Precancerous breast lesions: implications for breast cancer prevention trials. Int J Oncol 23:1071–1078
Anderson GL, Limacher M, Assaf AR et al (2004) Effects of equine estrogen in postmenopausal women with hypterectomy: the women’s health initiative randomized controlled trial. JAMA 291:1701–1712
Acknowledgments
Short list Of WHI investigators. Program Office: (National Heart, Lung, and Blood Institute, Bethesda, Maryland) Jacques Rossouw, Shari Ludlam, Joan McGowan, Leslie Ford, and Nancy Geller.
Clinical Coordinating Center: (Fred Hutchinson Cancer Research Center, Seattle, WA) Ross Prentice, Garnet Anderson, Andrea LaCroix, Charles Kooperberg; (Medical Research Labs, Highland Heights, KY) Evan Stein; (University of California at San Francisco, San Francisco, CA) Steven Cummings.
Clinical Centers: (Albert Einstein College of Medicine, Bronx, NY) Sylvia Wassertheil-Smoller; (Baylor College of Medicine, Houston, TX) Haleh Sangi-Haghpeykar; (Brigham and Women’s Hospital, Harvard Medical School, Boston, MA) JoAnn E. Manson; (Brown University, Providence, RI) Charles B. Eaton; (Emory University, Atlanta, GA) Lawrence S. Phillips; (Fred Hutchinson Cancer Research Center, Seattle, WA) Shirley Beresford; (George Washington University Medical Center, Washington, DC) Lisa Martin; (Los Angeles Biomedical Research Institute at Harbor- UCLA Medical Center, Torrance, CA) Rowan Chlebowski; (Kaiser Permanente Center for Health Research, Portland, OR) Erin LeBlanc; (Kaiser Permanente Division of Research, Oakland, CA) Bette Caan; (Medical College of Wisconsin, Milwaukee, WI) Jane Morley Kotchen; (MedStar Research Institute/Howard University, Washington, DC) Barbara V. Howard; (Northwestern University, Chicago/Evanston, IL) Linda Van Horn; (Rush Medical Center, Chicago, IL) Henry Black; (Stanford Prevention Research Center, Stanford, CA) Marcia L. Stefanick; (State University of New York at Stony Brook, Stony Brook, NY) Dorothy Lane; (The Ohio State University, Columbus, OH) Rebecca Jackson; (University of Alabama at Birmingham, Birmingham, AL) Cora E. Lewis; (University of Arizona, Tucson/Phoenix, AZ) Cynthia A. Thomson; (University at Buffalo, Buffalo, NY) Jean Wactawski-Wende; (University of California at Davis, Sacramento, CA) John Robbins; (University of California at Irvine, CA) F. Allan Hubbell; (University of California at Los Angeles, Los Angeles, CA) Lauren Nathan; (University of California at San Diego, LaJolla/Chula Vista, CA) Robert D. Langer; (University of Cincinnati, Cincinnati, OH) Margery Gass; (University of Florida, Gainesville/Jacksonville, FL) Marian Limacher; (University of Hawaii, Honolulu, HI) J. David Curb; (University of Iowa, Iowa City/Davenport, IA) Robert Wallace; (University of Massachusetts/Fallon Clinic, Worcester, MA) Judith Ockene; (University of Medicine and Dentistry of New Jersey, Newark, NJ) Norman Lasser; (University of Miami, Miami, FL) Mary Jo O’Sullivan; (University of Minnesota, Minneapolis, MN) Karen Margolis; (University of Nevada, Reno, NV) Robert Brunner; (University of North Carolina, Chapel Hill, NC) Gerardo Heiss; (University of Pittsburgh, Pittsburgh, PA) Lewis Kuller; (University of Tennessee Health Science Center, Memphis, TN) Karen C. Johnson; (University of Texas Health Science Center, San Antonio, TX) Robert Brzyski; (University of Wisconsin, Madison, WI) Gloria E. Sarto; (Wake Forest University School of Medicine, Winston-Salem, NC) Mara Vitolins; (Wayne State University School of Medicine/Hutzel Hospital, Detroit, MI) Michael S. Simon.
Women’s Health Initiative Memory Study: (Wake Forest University School of Medicine, Winston-Salem, NC) Sally Shumaker.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kabat, G.C., Kim, M.Y., Woods, N.F. et al. Reproductive and menstrual factors and risk of ductal carcinoma in situ of the breast in a cohort of postmenopausal women. Cancer Causes Control 22, 1415–1424 (2011). https://doi.org/10.1007/s10552-011-9814-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-011-9814-8