Abstract
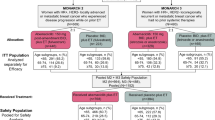
We sought to determine if an association exists between age and capecitabine efficacy among patients with metastatic breast cancer (MBC). Pooled analysis of five phase II or III registration trials of capecitabine 2,500–2,510 mg/m2/day for 2 weeks and 1 week off, or combination therapy was performed. Four trials enrolled patients previously exposed to other chemotherapy, generally a taxane. Of 570 patients, 193 (34%) were 18–49 years old, 246 (43%) were 50–64, and 131 (23%) were ≥65. Median average daily dose was 2,067 mg/m2 in the 18- to 49-year-old group and 2,105 mg/m2 in the 50–64 and ≥65 year groups. Overall survival (OS) in all groups was similar by log-rank test for the individual trials (P = 0.71–0.95) and Cox regression of the pooled trials. Univariate analysis demonstrated no difference in clinical benefit or objective response between groups. Treatment failure analysis showed 283 (50%) patients experienced progressive disease, while 114 (20%) withdrew for safety. Serious adverse events (AEs) occurred in 71 (36.8%), 85 (34.6%), and 59 (45.0%) patients in the 18–49, 50–64, and ≥65 years groups, respectively. There was no statistically significant association between age and OS, clinical benefit, or objective response in patients with MBC treated with capecitabine. Frequency of AEs and serious AEs was not related to age at treatment, although women ≥65 years were more likely to withdraw from treatment because of an AE than younger women.


Similar content being viewed by others
References
U.S. Centers for Disease Control and Prevention: Breast cancer rates by age. http://www.cdc.gov/cancer/breast/statistics/age.htm
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics, 2009. CA Cancer J Clin 598:225–249
Anderson WF, Jatoi I, Sherman ME (2009) Qualitative age interactions in breast cancer studies: mind the gap. J Clin Oncol 27:5308–5311
Christman K, Muss HB, Case LD, Stanley V (1992) Chemotherapy of metastatic breast cancer in the elderly. The Piedmont Oncology Association experience [see comment]. JAMA 268:57–62
Pentheroudakis G, Fountzilas G, Kalofonos HP, Hellenic Cooperative Oncology Group et al (2008) Palliative chemotherapy in elderly patients with common metastatic malignancies: a Hellenic Cooperative Oncology Group registry analysis of management, outcome and clinical benefit predictors. Crit Rev Oncol Hematol 66:237–247
Muss HB, Berry DA, Cirrincione C et al (2007) Toxicity of older and younger patients treated with adjuvant chemotherapy for node-positive breast cancer: the Cancer and Leukemia Group B experience. J Clin Oncol 25:3699–3704
Sledge GW, Robert N, Sparano JA et al (1995) Eastern Cooperative Oncology Group studies of paclitaxel and doxorubicin in advanced breast cancer. Semin Oncol 22(3 Suppl 6):105–108
Xeloda® (capecitabine) [prescribing information]: Genentech, Inc. South San Francisco, CA; 2009
Sledge GW, Neuberg D, Bernardo P, Ingle JN, Martino S, Rowinsky EK, Wood WC (2003) Phase III trial of doxorubicin, paclitaxel, and the combination of doxorubicin and paclitaxel as front-line chemotherapy for metastatic breast cancer: an intergroup trial (E1193). J Clin Oncol 21:588–592
Stockler M, Sourjina T, Grimison P et al (2007) A randomized trial of capecitabine (C) given intermittently (IC) rather than continuously (CC) compared to classical CMF as first-line chemotherapy for advanced breast cancer (ABC). J Clin Oncol 25:39s (18S; abstr 1031)
O’Shaughnessy J, Miles D, Vukelja S et al (2002) Superior survival with capecitabine plus docetaxel combination therapy in anthracycline-pretreated patients with advanced breast cancer: phase III trial results. J Clin Oncol 20:2812–2823
Blum JL, Jones SE, Buzdar AU et al (1999) Multicenter phase II study of capecitabine in paclitaxel-refractory metastatic breast cancer. J Clin Oncol 17:485–493
Blum JL, Dieras V, Lo Russo PM, Horton J, Rutman O, Buzdar A, Osterwalder B (2001) Multicenter, phase II study of capecitabine in taxane-pretreated metastatic breast carcinoma patients. Cancer 92:1759–1768
Talbot DC, Moiseyenko V, Van Belle S et al (2002) Randomised, phase II trial comparing oral capecitabine (Xeloda) with paclitaxel in patients with metastatic/advanced breast cancer pretreated with anthracyclines. Br J Cancer 86:1367–1372
O’Shaughnessy JA, Blum J, Moiseyenko V et al (2001) Randomized, open-label, phase II trial of oral capecitabine (Xeloda) vs. a reference arm of intravenous CMF (cyclophosphamide, methotrexate and 5-fluorouracil) as first-line therapy for advanced/metastatic breast cancer. Ann Oncol 12:1247–1254
Balducci L (2001) The geriatric cancer patient: equal benefit from equal treatment. Cancer Control 8(Suppl 2):1–25
Ibrahim NK, Frye DK, Buzdar AU, Walters RS, Hortobagyi GN (1996) Doxorubicin-based chemotherapy in elderly patients with metastatic breast cancer: tolerance and outcome. Arch Intern Med 156:882–888
Muss HB, Berry DA, Cirrincione CT et al (2009) Adjuvant chemotherapy in older women with early-stage breast cancer. N Engl J Med 360:2055–2065
Rimawi MF, Shetty PB, Weiss HL, Schiff R, Osborne CK, Chamness GC, Elledge RM (2010) Epidermal growth factor receptor expression in breast cancer association with biologic phenotype and clinical outcomes. Cancer 116:1234–1242
Heitz F, Harter P, Lueck HJ, Fissler-Eckhoff A, Lorenz-Salehi F, Scheil-Bertram S, Traut A, du Bois A (2009) Triple-negative and HER2-overexpressing breast cancers exhibit an elevated risk and an earlier occurrence of cerebral metastases. Eur J Cancer 45:2792–2798
Chang J, Clark GM, Allred DC, Mohsin S, Chamness G, Elledge RM (2003) Survival of patients with metastatic breast carcinoma: importance of prognostic markers of the primary tumor. Cancer 97:545–553
Acknowledgments
The five studies, individually and pooled, were sponsored by Roche, manufacturer of Xeloda® (capecitabine). Editorial support was provided by Insight Medical Communications, NY, funded by Roche.
Conflict of interest
Dr. Joanne Blum serves as a consultant or advisor to Roche, manufacturer of capecitabine [Xeloda®]. Dr. Joseph Kohles was an employee of Roche Laboratories, Inc. at the time this study and manuscript were developed. Dr. Edward McKenna is an employee of Roche Laboratories, Inc. Dr. Nana Scotto is an employee of F. Hoffmann-La Roche. Dr. Sylvia Hu is an employee of Genentech-Roche and has stock ownership in F. Hoffman-La Roche. Roche sponsored the research summarized in this manuscript through funding to RTI Health Solutions, which employs Dawn Odom and Dr. James Kaye. Dr. Stefan Glück serves as a consultant or advisor for and has received honoraria and research support from Roche.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Blum, J.L., Kohles, J., McKenna, E. et al. Association of age and overall survival in capecitabine-treated patients with metastatic breast cancer in clinical trials. Breast Cancer Res Treat 125, 431–439 (2011). https://doi.org/10.1007/s10549-010-1222-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-010-1222-3