Abstract
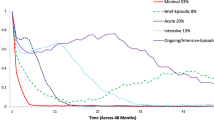
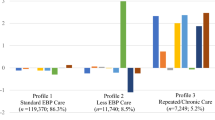
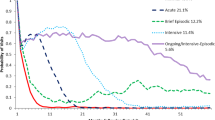
Little is known about high-cost service users in the context of youth outpatient mental health, despite the fact that they account for a large proportion of overall mental healthcare expenditures. A nuanced understanding of these users is critical to develop and implement tailored services, as well as to inform relevant policies. This study aims to characterize high-cost service users by examining demographic factors, diagnoses, and service type use. Administrative service use data were extracted from a large County Department of Behavioral Health Services database. Latent profile analyses suggest a four-profile solution primarily distinguished by youth age and diagnostic complexity. Study findings have implications for defining high-cost service users and key targets for efforts aiming to improve outcomes for these youth.

Similar content being viewed by others
References
Alexandre, P. K. (2009). Mental health care for youth: Predictors of use are not always the same as predictors of volume. Social Science Journal,45(4), 1–13. https://doi.org/10.1016/j.soscij.2008.09.004.Mental.
Alexandre, P. K., Dowling, K., Stephens, R. M., Laris, A. S., & Rely, K. (2008). Predictors of outpatient mental health service use by American youth. Psychological Services,5(3), 251–261. https://doi.org/10.1037/1541-1559.5.3.251.
Barlow, D. H., Farchione, T. J., Bullis, J. R., Gallagher, M. W., Murray-Latin, H., Sauer-Zavala, S., et al. (2017). The unified protocol for transdiagnostic treatment of emotional disorders compared with diagnosis-specific protocols for anxiety disorders. JAMA Psychiatry,74(9), 875. https://doi.org/10.1001/jamapsychiatry.2017.2164.
Berwick, D. M., Nolan, T. W., & Whittington, J. (2019). The triple aim: Care, health, and cost. Helath Affairs,27, 759–769. https://doi.org/10.1377/hlthaff.
Bickman, L. (2008). A measurement feedback system (MFS) is necessary to improve mental health outcomes. Journal of the American Academy of Child and Adolescent Psychiatry,47(10), 1114–1119. https://doi.org/10.1097/CHI.0b013e3181825af8.
Chandler, R. K., Peters, R. H., Field, G., & Juliano-Bult, D. (2004). Challenges in implementing evidence-based treatment practices for co-occurring disorders in the criminal justice system. Behavioral Sciences & the Law,22(4), 431–448. https://doi.org/10.1002/bsl.598.
Cohen, S., & Yu, W. (2012). The concentration and persistence in the level of health expenditures over time: Estimates for the US population, 2008–2009, Agency for Healthcare Research and Quality Statistical Brief #354.
De Oliveira, C., Cheng, J., Vigod, S., Rehm, J., & Kurdyak, P. (2016). Patients With high mental health costs incur over 30 percent more costs than other high-cost patients. Health Affairs,35(1), 36–43. https://doi.org/10.1377/hlthaff.2015.0278.
Dopp, A. R., Hanson, R. F., Saunders, B. E., Dismuke, C. E., & Moreland, A. D. (2017). Community-based implementation of trauma-focused interventions for youth: Economic impact of the learning collaborative model. Psychological Services,14(1), 57–65. https://doi.org/10.1037/ser0000131.
Dopp, A. R., Mundey, P., Silovsky, J. F., Hunter, M., & Slemaker, A. (2019). Economic value of community-based services for problematic sexual behaviors in youth: A mixed-method cost-effectiveness analysis. Child Abuse & Neglect, Advanced Online Publication. https://doi.org/10.1016/j.chiabu.2019.104043.
Foti, R. J., Bray, B. C., Thompson, N. J., & Allgood, S. F. (2012). Know thy self, know thy leader: Contributions of a pattern-oriented approach to examining leader perceptions. The Leadership Quarterly,23, 702–717. https://doi.org/10.1016/j.leaqua.2012.03.007.
Graham, K., Cheng, J., Bernards, S., Wells, S., Rehm, J., & Kurdyak, P. (2017). How much do mental health and substance use/addiction affect use of general medical services? Extent of use, reason for use, and associated costs. Canadian Journal of Psychiatry,62(1), 48–56. https://doi.org/10.1177/0706743716664884.
Grimes, K. E., Schulz, M. F., Cohen, S. A., Mullin, B. O., Lehar, S. E., & Tien, S. (2011). Pursuing cost-effectiveness in mental health service delivery for youth with complex needs. Journal of Mental Health Policy and Economics,86, 73–86.
Hastings, S. N., Whitson, H. E., Sloane, R., Landerman, L. R., Horney, C., & Johnson, K. S. (2012). Using the past to predict the future: Latent class analysis of patterns of health service use among older emergency department patients. Journal of the American Geriatrics Society,62(4), 711–715. https://doi.org/10.1111/jgs.12746.
Jaycox, L. H., Stein, B. D., Paddock, S., Miles, J. N. V., Chandra, A., Meredith, L. S., et al. (2009). Impact of teen depression on academic, social, and physical functioning. Pediatrics,124(4), e596–e605. https://doi.org/10.1542/peds.2008-3348.
Jerrell, J. M. (1998). Utilization management analysis for children’s mental health services. Journal of Behavioral Health Services and Research,25(1), 35–42. https://doi.org/10.1007/BF02287498.
Kelley, S. D., & Bickman, L. (2009). Beyond outcomes monitoring: Measurement feedback systems in child and adolescent clinical practice. Current Opinion in Psychiatry. https://doi.org/10.1097/YCO.0b013e32832c9162.
Kessler, R. C., Berglund, P., Demler, O., Jin, R., Merikangas, K. R., & Walters, E. E. (2005). Lifetime prevalence and age-of-onset distributions of. Archives of General Psychiatry,62, 593–602. https://doi.org/10.1001/archpsyc.62.6.593.
Lee, Y. C., Chatterton, M. Lou, Magnus, A., Mohebbi, M., Le, L. K. D., & Mihalopoulos, C. (2017). Cost of high prevalence mental disorders: Findings from the 2007 Australian National Survey of Mental Health and Wellbeing. Australian and New Zealand Journal of Psychiatry,51(12), 1198–1211. https://doi.org/10.1177/0004867417710730.
Lee, N. S., Whitman, N., Vakharia, N., Taksler, G. B., & Rothberg, M. B. (2016). High-cost patients: Hot-spotters don’t explain the half of it. Journal of General Internal Medicine,32(1), 28–34. https://doi.org/10.1007/s11606-016-3790-3.
Mirel, L., & Carper, K. (2011). Trends in Health Care Expenditures for Children under Age 18: 2001, 2006, and 2011. Agency for Healthcae Research and Quality Statistical Brief # 428. Retrieved from http://www.meps.ahrq.gov/mepsweb/about_meps/Price_Index.shtml.
Mitchell, E. M. (2016). Statistical Brief #521: Concentration of Health Expenditures and Selected Characteristics of High Spenders, U.S. Civilian Noninstitutionalized Population, 2016. Retrieved from https://meps.ahrq.gov/data_files/publications/mr23/mr23.pdf.
Morin, A. J. S., Morizot, J., Bastien Boudrias, J.-S., & Madore, I. (2011). A multifoci person-centered perspective on workplace affective commitment: A latent profile/factor mixture analysis. Organizational Research Methods,14(1), 58–90. https://doi.org/10.1177/1094428109356476.
Nakamura, B. J., Chorpita, B. F., Hirsch, M., Daleiden, E., Slavin, L., Amundson, M. J., et al. (2011). Large-scale implementation of evidence-based treatments for children 10 years later: Hawaii’s evidence-based services initiative in children’s mental health. Clinical Psychology: Science and Practice,18(1), 24–35. https://doi.org/10.1111/j.1468-2850.2010.01231.x.
Powers, B. W., & Chaguturu, S. K. (2016). ACOs and high-cost patients. New England Journal of Medicine,374(3), 203–205. https://doi.org/10.1056/NEJMp1511131.
Prince, M., Patel, V., Saxena, S., Maj, M., Maselko, J., Phillips, M. R., et al. (2007). No health without mental health. Lancet. https://doi.org/10.1016/s0140.
RAND. (2001). Mental health care for youth, 52(2).
Robst, J. (2012). Comparing methods for identifying future high-cost mental health cases in medicaid. Value in Health,15(1), 198–203. https://doi.org/10.1016/j.jval.2011.08.007.
Roehrig, C. (2016). Mental disorders top the list of the most costly conditions in the United States: $201 Billion. Health Affairs,35(6), 1130–1135. https://doi.org/10.1377/hlthaff.2015.1659.
Soni, A. (2015). The five most costly children’s conditions among children, ages 0-17, 2012. Agency for Healthcae Research and Quality Statistical Brief,472, 3–5. https://doi.org/10.1111/j.1476-5381.1973.tb08378.x.
StataCorp. (2017). Stata statistical software: Release 15. College Station, TX: StataCorp LLC.
Subcommitte on Attention-Deficit, Hyperactivity Disorder. (2011). ADHD: Clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics. https://doi.org/10.1542/peds.2011-2654.
U.S. Departmemt of Health and Human Services. (2001). Mental health: culture, race, and ethnicity: a supplement to mental health: a report of the surgeon general (pp. 1–204). Rockville, MD: US Public Health Service: Substance Abuse and Mental Health Services Administration.
Van der Oord, S., Prins, P. J. M., Oosterlaan, J., & Emmelkamp, P. M. G. (2008). Efficacy of methylphenidate, psychosocial treatments and their combination in school-aged children with ADHD: A meta-analysis. Clinical Psychology Review,28(5), 783–800. https://doi.org/10.1016/j.cpr.2007.10.007.
Wammes, J. J. G., van der Wees, P. J., Tanke, M. A. C., Westert, G. P., & Jeurissen, P. P. T. (2018). Systematic review of high-cost patients’ characteristics and healthcare utilisation. British Medical Journal Open,8(9), e023113. https://doi.org/10.1136/bmjopen-2018-023113.
Watkins, E. R. (2015). Psychological treatment of depressive rumination. Current Opinion in Psychology,4, 32–36. https://doi.org/10.1016/j.copsyc.2015.01.020.
Whiteford, H. A., Degenhardt, L., Rehm, J., Baxter, A. J., Ferrari, A. J., Erskine, H. E., et al. (2013). Articles Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. Lancet. https://doi.org/10.1016/S0140-6736(13)61611-6.
Whitney, D. G., & Peterson, M. D. (2019). Changing organizational constructs into functional tools: An assessment of the 5 A’s in primary care practices. JAMA Pediatrics,173(4), 389–391. https://doi.org/10.1370/afm.357.
Whitson, H. E., Johnson, K. S., Sloane, R., Cigolle, C., Pieper, C. F., Landerman, L., et al. (2016). Identifying patterns of multimorbidity in Older Americans: Application of latent class analysis HHS public access. Journal of the American Geriatrics Society,64(8), 1668–1673. https://doi.org/10.1111/jgs.14201.
Zulman, D. M., Chee, C. P., Wagner, T. H., Yoon, J., Cohen, D. M., Holmes, T. H., et al. (2015). Multimorbidity and healthcare utilisation among high-cost patients in the US Veterans Affairs Health Care System. British Medical Journal Open,5(4), 1–9. https://doi.org/10.1136/bmjopen-2015-007771.
Funding
This study was supported by funding from the San Diego County Behavioural Health Services, Health and Human Services Agency as well as NIMH Grant K23 MH115100 and NIMH Grant K23 MH110602.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest
Ethical Approval
Ethics approval for this study was obtained from the UC San Diego Human Research Protection Program (HRPP). These data were collected as part of evaluation activities and analyses were conducted using an anonymized dataset.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dickson, K.S., Stadnick, N.A., Lind, T. et al. Defining and Predicting High Cost Utilization in Children’s Outpatient Mental Health Services. Adm Policy Ment Health 47, 655–664 (2020). https://doi.org/10.1007/s10488-019-00988-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10488-019-00988-1