Summary
Background
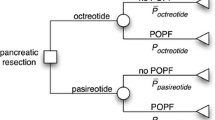
Previous cost evaluation studies reported either no increase or cost-saving using pasireotide in patients undergoing pancreaticoduodenectomy. We examined the likelihood and magnitude of cost-saving when using pasireotide at our institution to determine the generalizability of prior reports.
Methods
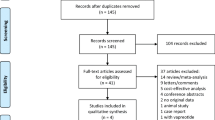
Cost data were obtained for a cohort of 440 patients undergoing pancreaticoduodenectomy at a single institution during 2009–2016. A statistical model was used to simulate the cost of patient care had they received pasireotide. Sensitivity analyses were performed to assess the impact of pasireotide price and pancreatic fistula rate on cost.
Results
With a fistula rate of 10.2% and a current price for pasireotide of $1257, the likelihood of cost-saving is 60%. When cost-saving does occur, the mean cost-saving per patient is $1442, 2.5–97.5% quantile difference (QD): $69–3756. At the same pasireotide price but with a fistula rate of 30%, the likelihood of cost-saving increases to 91% with a mean cost-saving of $4030, 2.5–97.5% QD: $402–8511. At the same fistula rate but with a pasireotide price of $1000, the likelihood of cost-saving increases to 65% with a cost-saving of $1566, 2.5–97.5% QD: $75–3979.
Conclusion
At its current price, and with the fistula rate at our institution, pasireotide is more likely to pay for itself than not, but there is a significant probability that it will not be cost-saving. Negotiating a better price (i.e., to the lowest found in the literature) will reduce the likelihood of pasireotide not being cost-saving by 5%.


Similar content being viewed by others
References
McEvoy SH, Lavelle LP, Hoare SM, O’Neill AC, Awan FN, Malone DE, et al. Pancreaticoduodenectomy: expected post-operative anatomy and complications. Br J Radiol. 2014;87(1041):20140050.
Denbo JW, Orr WS, Zarzaur BL, Behrman SW. Toward defining grade C pancreatic fistula following pancreaticoduodenectomy: incidence, risk factors, management and outcome. HPB (Oxford). 2012;14(9):589–93.
Gurusamy KS, Koti R, Fusai G, Davidson BR. Somatostatin analogues for pancreatic surgery. Cochrane Database Syst Rev. 2013; https://doi.org/10.1002/14651858.cd008370.pub2.
Boike GM, Sightler SE, Averette HE. Treatment of small intestinal fistulas with octreotide, a somatostatin analog. J Surg Oncol. 1992;49(1):63–5.
Lowy AM, Lee JE, Pisters PW, Davidson BS, Fenoglio CJ, Stanford P, et al. Prospective, randomized trial of octreotide to prevent pancreatic fistula after pancreaticoduodenectomy for malignant disease. Ann Surg. 1997;226(5):632–41.
Yeo CJ, Cameron JL, Lillemoe KD, Sauter PK, Coleman J, Sohn TA, et al. Does prophylactic octreotide decrease the rates of pancreatic fistula and other complications after pancreaticoduodenectomy? Results of a prospective randomized placebo-controlled trial. Ann Surg. 2000;232(3):419–29.
Sarr MG, Pancreatic Surgery G. The potent somatostatin analogue vapreotide does not decrease pancreas-specific complications after elective pancreatectomy: a prospective, multicenter, double-blinded, randomized, placebo-controlled trial. J Am Coll Surg. 2003;196(4):556–64. discussion 64–5; author reply 65.
Li-Ling J, Irving M. Somatostatin and octreotide in the prevention of postoperative pancreatic complications and the treatment of enterocutaneous pancreatic fistulas: a systematic review of randomized controlled trials. Br J Surg. 2001;88(2):190–9.
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, et al. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005;138(1):8–13.
Fernandez-Cruz L, Jimenez Chavarria E, Taura P, Closa D, Boado MA, Ferrer J. Prospective randomized trial of the effect of octreotide on pancreatic juice output after pancreaticoduodenectomy in relation to histological diagnosis, duct size and leakage. HPB (Oxford). 2013;15(5):392–9.
Kollmar O, Moussavian MR, Richter S, de Roi P, Maurer CA, Schilling MK. Prophylactic octreotide and delayed gastric emptying after pancreaticoduodenectomy: results of a prospective randomized double-blinded placebo-controlled trial. Eur J Surg Oncol. 2008;34(8):868–75.
Hesse UJ, De Decker C, Houtmeyers P, Demetter P, Ceelen W, Pattyn P, et al. Prospectively randomized trial using perioperative low dose octreotide to prevent organ related and general complications following pancreatic surgery and pancreatico-jejunostomy. Acta Chir Belg. 2005;105(4):383–7.
Allen PJ. Pasireotide for postoperative pancreatic fistula. N Engl J Med. 2014;371(9):875–6.
Bruns C, Lewis I, Briner U, Meno-Tetang G, Weckbecker G. SOM230: a novel somatostatin peptidomimetic with broad somatotropin release inhibiting factor (SRIF) receptor binding and a unique antisecretory profile. Eur J Endocrinol. 2002;146(5):707–16.
Dominguez-Rosado I, Fields RC, Woolsey CA, Williams G, Horwedel TA, Rose JB, et al. Prospective evaluation of pasireotide in patients undergoing pancreaticoduodenectomy: the Washington University experience. J Am Coll Surg. 2018;226(2):147–154 e1.
Daskalaki D, Butturini G, Molinari E, Crippa S, Pederzoli P, Bassi C. A grading system can predict clinical and economic outcomes of pancreatic fistula after pancreaticoduodenectomy: results in 755 consecutive patients. Langenbecks Arch Surg. 2011;396(1):91–8.
Cecka F, Jon B, Subrt Z, Ferko A. Clinical and economic consequences of pancreatic fistula after elective pancreatic resection. HBPD INT. 2013;12(5):533–9.
Enestvedt CK, Diggs BS, Cassera MA, Hammill C, Hansen PD, Wolf RF. Complications nearly double the cost of care after pancreaticoduodenectomy. Am J Surg. 2012;204(3):332–8.
Pratt WB, Maithel SK, Vanounou T, Huang ZS, Callery MP, Vollmer CM Jr.. Clinical and economic validation of the International Study Group of Pancreatic Fistula (ISGPF) classification scheme. Ann Surg. 2007;245(3):443–51.
Abbott DE, Sutton JM, Jernigan PL, Chang A, Frye P, Shah SA, et al. Prophylactic pasireotide administration following pancreatic resection reduces cost while improving outcomes. J Surg Oncol. 2016;113(7):784–8.
Ma LW, Dominguez-Rosado I, Gennarelli RL, Bach PB, Gonen M, D’Angelica MI, et al. The cost of postoperative pancreatic fistula versus the cost of pasireotide: results from a prospective randomized trial. Ann Surg. 2017;265(1):11–6.
Denbo JW, Slack RS, Bruno M, Cloyd JM, Prakash L, Fleming JB, et al. Selective perioperative administration of pasireotide is more cost-effective than routine administration for pancreatic fistula prophylaxis. J Gastrointest Surg. 2017;21(4):636–46.
Goyert N, Eeson G, Kagedan DJ, Behman R, Lemke M, Hallet J, et al. Pasireotide for the prevention of pancreatic fistula following pancreaticoduodenectomy: a cost-effectiveness analysis. Ann Surg. 2017;265(1):2–10.
Kajiwara T, Sakamoto Y, Morofuji N, Nara S, Esaki M, Shimada K, et al. An analysis of risk factors for pancreatic fistula after pancreaticoduodenectomy: clinical impact of bile juice infection on day 1. Langenbecks Arch Surg. 2010;395(6):707–12.
Topal B, Fieuws S, Aerts R, Weerts J, Feryn T, Roeyen G, et al. Pancreaticojejunostomy versus pancreaticogastrostomy reconstruction after pancreaticoduodenectomy for pancreatic or periampullary tumours: a multicentre randomised trial. Lancet Oncol. 2013;14(7):655–62.
Lee SE, Jang JY, Lim CS, Kang MJ, Kim SH, Kim MA, et al. Measurement of pancreatic fat by magnetic resonance imaging: predicting the occurrence of pancreatic fistula after pancreatoduodenectomy. Ann Surg. 2010;251(5):932–6.
Addeo P, Delpero JR, Paye F, Oussoultzoglou E, Fuchshuber PR, Sauvanet A, et al. Pancreatic fistula after a pancreaticoduodenectomy for ductal adenocarcinoma and its association with morbidity: a multicentre study of the French Surgical Association. HPB (Oxford). 2014;16(1):46–55.
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M, et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery. 2017;161(3):584–91.
Tani M, Kawai M, Hirono S, Hatori T, Imaizumi T, Nakao A, et al. Use of omentum or falciform ligament does not decrease complications after pancreaticoduodenectomy: nationwide survey of the Japanese Society of Pancreatic Surgery. Surgery. 2012;151(2):183–91.
Schmidt CM, Turrini O, Parikh P, House MG, Zyromski NJ, Nakeeb A, et al. Effect of hospital volume, surgeon experience, and surgeon volume on patient outcomes after pancreaticoduodenectomy: a single-institution experience. Arch Surg. 2010;145(7):634–40.
Sugimoto M, Takahashi S, Gotohda N, Kato Y, Kinoshita T, Shibasaki H, et al. Schematic pancreatic configuration: a risk assessment for postoperative pancreatic fistula after pancreaticoduodenectomy. J Gastrointest Surg. 2013;17(10):1744–51.
Gafni A, Walter S, Birch S. Uncertainty and the decision maker: assessing and managing the risk of undesirable outcomes. Health Econ. 2013;22(11):1287–94.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
F. Yuan, A. Gafni, C.-S. Gu, and P.E. Serrano declare that they have no competing interests.
Ethical standards
As part of our institutional Research Ethics Board submission, a waiver of consent was approved for this retrospective chart review.
Additional information
Presentations
This work was presented in part at: SSAT, Chicago, Illinois, May 9, 2017 and Pancreas Club, Chicago, Illinois, May 5, 2017.
Caption Electronic Supplementary Material
10353_2018_563_MOESM2_ESM.docx
Table S2: Market price of 14 doses of pasireotide and the price after converting into Canadian currency from 14 different countries/regions according to hospital pricing
Rights and permissions
About this article
Cite this article
Yuan, F., Gafni, A., Gu, CS. et al. Does giving pasireotide to patients undergoing pancreaticoduodenectomy always pay for itself?. Eur Surg 52, 132–140 (2020). https://doi.org/10.1007/s10353-018-0563-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10353-018-0563-8