Abstract
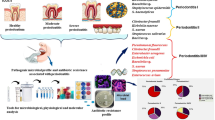
This study aimed to identify the aerobic and anaerobic causal microorganisms of odontogenic infections and their antibiotic sensitivity. Purulent exudates were taken from patients with odontogenic infections by transdermal puncture, and aerobic and anaerobic microorganisms were identified using biochemical tests. Susceptibility to antibiotics was tested using the Kirby-Bauer method; the inhibition halos were measured according to NCCLS, and based on the results, the microorganisms were classified as susceptible, intermediate or resistant to each antibiotic. Frequencies of species and percentages of resistance were calculated. The microorganisms associated with odontogenic infections were principally anaerobic (65.3% anaerobic vs. 35.7% aerobic), and the susceptibility to antibiotics was higher in anaerobic than in aerobic microorganisms. The majority of isolated microorganisms (82%) showed susceptibility to amoxicillin/clavulanic acid. The causal agents of odontogenic infections were anaerobic microorganisms, which exhibited high resistance to antibiotics.




Similar content being viewed by others
References
Taub D, Yampolsky A, Diecidue R, Gold L. Controversies in the management of oral and maxillofacial infections. Oral Maxillofac Surg Clin North Am. 2017;4:465–73.
McDonald C, Hennedige A, Henry A, et al. Management of cervicofacial infections: a survey of current practice in maxillofacial units in the UK. Br J Oral Maxillofac Surg. 2017;9:940–5.
The Japanese Association for Infectious Disease/Japanese Society of Chemotherapy, The JAID/JSC Committee for Developing Treatment Guide and Guidelines for Clinical Management of Infectious Disease, Odontogenic Infection Working Group. The 2016 JAID/JSC guidelines for clinical management of infectious disease-Odontogenic infections. J Infect Chemother. 2018;24:320–4.
Bahl R, Sandhu S, Singh K, Sahai N, Gupta M. Odontogenic infections: microbiology and management. Contemp Clin Dent. 2014;3:307–11.
Heim N, Faron A, Wiedemeyer V, Reich R, Martini M. Microbiology and antibiotic sensitivity of head and neck space infections of odontogenic origin. Differences in inpatient and outpatient management. J Craniomaxillofac Surg. 2017;45:1731–5.
Tung-Yiu W, Jehn-Shyun H, Ching-Hung C, Hung-An C. Cervical necrotizing fasciitis of odontogenic origin: a report of 11 cases. J Oral Maxillofac Surg. 2000;12:1347–52. discussion 1353.
Gore MR. Odontogenic necrotizing fasciitis: a systematic review of the literature. BMC Ear Nose Throat Disord. 2018;18:14.
Arora N, Juneja R, Meher R. Complication of an odontogenic infection to an orbital abscess: the role of a medical fraudster (“Quack”). Iran J Otorhinolaryngol. 2018;30:181–4.
Farmahan S, Tuopar D, Ameerally PJ, Kotecha R, Sisodia B. Microbiological examination and antibiotic sensitivity of infections in the head and neck. Has anything changed? Br J Oral Maxillofac Surg. 2014;52:632–5.
Chunduri NS, Madasu K, Goteki VR, Karpe T, Reddy H. Evaluation of bacterial spectrum of orofacial infections and their antibiotic susceptibility. Ann Maxillofac Surg. 2012;2:46–50.
Walia IS, Borle RM, Mehendiratta D, Yadav AO. Microbiology and antibiotic sensitivity of head and neck space infections of odontogenic origin. J Maxillofac Oral Surg. 2014;1:16–21.
Tüzüner Öncül AM, Uzunoğlu E, Karahan ZC, Aksoy AM, Kişnişci R, Karaahmetoğlu Ö. Detecting gram-positive anaerobic cocci directly from the clinical samples by multiplex polymerase chain reaction in odontogenic infections. J Oral Maxillofac Surg. 2015;73:259–66.
Singh M, Kambalimath DH, Gupta KC. Management of odontogenic space infection with microbiology study. J Maxillofac Oral Surg. 2014;13:133–9.
Performed standards for antimicrobial disk susceptibility tests. National Committee for Clinical Laboratory Standards. Approved standard M2-A8. 8th ed. Pa: NCCLS, Wayne; 2003.
Babu VR, Ikkurthi S, Perisetty DK, Babu KAS, Rasool M, Shaik S. A prospective comparison of computed tomography and magnetic resonance imaging as a diagnostic tool for maxillofacial space infections. J Int Soc Prev Community Dent. 2018;8:343–8.
Nadig K, Taylor NG. Management of odontogenic infection at a district general hospital. Br Dent J. 2018;224:962–6.
Bakathir AA, Moos KF, Ayoub AF, Bagg J. Factors contributing to the spread of odontogenic infections: a prospective pilot study. Sultan Qaboos Univ Med J. 2009;9:296–304.
Chang JS, Yoo KH, Yoon SH, et al. Odontogenic infection involving the secondary fascial space in diabetic and non-diabetic patients: a clinical comparative study. J Korean Assoc Oral Maxillofac Surg. 2013;39:175–81.
Lin RH, Huang CC, Tsou YA, et al. Correlation between imaging characteristics and microbiology in patients with deep neck infections: a retrospective review of one hundred sixty-one cases. Surg Infect (Larchmt). 2014;15:794–9.
Shakya N, Sharma D, Newaskar V, Agrawal D, Shrivastava S, Yadav R. Epidemiology, microbiology and antibiotic sensitivity of odontogenic space infections in Central India. J Maxillofac Oral Surg. 2018;3:324–31.
Fu B, McGowan K, Sun H, Batstone M. Increasing use of intensive care unit for odontogenic infection over one decade: Incidence and predictors. J Oral Maxillofac Surg. 2018. https://doi.org/10.1016/j.joms.2018.05.021.
Bhagania M, Youseff W, Mehra P, Figueroa R. Treatment of odontogenic infections: an analysis of two antibiotic regimens. J Oral Biol Craniofac Res. 2018;8:78–81.
Mathew GC, Ranganathan LK, Gandhi S, et al. Odontogenic maxillofacial space infections at a tertiary care center in North India: a five-year retrospective study. Int J Infect Dis. 2012;16:e296–302.
Shah A, Ramola V, Nautiyal V. Aerobic microbiology and culture sensitivity of head and neck space infection of odontogenic origin. Natl J Maxillofac Surg. 2016;7:56–61.
Hyun SY, Oh HK, Ryu JY, Kim JJ, Cho JY, Kim HM. Closed suction drainage for deep neck infections. J Craniomaxillofac Surg. 2014;42:751–6.
Fating NS, Saikrishna D, Vijay Kumar GS, Shetty SK, Raghavendra Rao M. Detection of bacterial flora in orofacial space infections and their antibiotic sensitivity profile. J Maxillofac Oral Surg. 2014;13:525–32.
Gómez-Arámbula H, Hidalgo-Hurtado A, Rodríguez-Flores R, González-Amaro AM, Garrocho-Rangel A, Pozos-Guillén A. Moxifloxacin versus clindamycin/ceftriaxone in the management of odontogenic maxillofacial infectious processes: a preliminary, intrahospital, controlled clinical trial. J Clin Exp Dent. 2015;7:e634–9.
Farmahan S, Tuopar D, Ameerally PJ. A study to investigate changes in the microbiology and antibiotic sensitivity of head and neck space infections. Surgeon. 2015;13:316–20.
Davis K, Gill D, Mouton CP, Southerland J, Halpern L. An unusual odontogenic infection due to clostridium subterminale in an immunocompetent patient: a case report and review of the literature. IDCases. 2018;12:34–40.
Tancawan AL, Pato MN, Abidin KZ, et al. Amoxicillin/clavulanic acid for the treatment of odontogenic infections: a randomised study comparing efficacy and tolerability versus Clindamycin. Int J Dent. 2015;2015:472470.
Dar-Odeh NS, Abu-Hammad OA, Al-Omiri MK, Khraisat AS, Shehabi AA. Antibiotic prescribing practices by dentists: a review. Ther Clin Risk Manag. 2010;6:301–6.
Sweeney LC, Dave J, Chambers PA, Heritage J. Antibiotic resistance in general dental practice—a cause for concern? J Antimicrob Chemother. 2004;53:567–76.
Svensäter G, Bergenholtz G. Biofilm in endodontic infections. Endodontic Topics. 2004;9:27–36.
Acknowledgements
This study was partially supported by PFCE-UASLP 2018 grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
López-González, E., Vitales-Noyola, M., González-Amaro, A.M. et al. Aerobic and anaerobic microorganisms and antibiotic sensitivity of odontogenic maxillofacial infections. Odontology 107, 409–417 (2019). https://doi.org/10.1007/s10266-019-00414-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-019-00414-w