Abstract
Objectives
To develop algorithms mapping the Kidney Disease Quality of Life 36-Item Short Form Survey (KDQOL-36) onto the 3-level EQ-5D questionnaire (EQ-5D-3L) and the 5-level EQ-5D questionnaire (EQ-5D-5L) for patients with end-stage renal disease requiring dialysis.
Methods
We used data from a cross-sectional study in Europe (France, n = 299; Germany, n = 413; Italy, n = 278; Spain, n = 225) to map onto EQ-5D-3L and data from a cross-sectional study in Singapore (n = 163) to map onto EQ-5D-5L. Direct mapping using linear regression, mixture beta regression and adjusted limited dependent variable mixture models (ALDVMMs) and response mapping using seemingly unrelated ordered probit models were performed. The KDQOL-36 subscale scores, i.e., physical component summary (PCS), mental component summary (MCS), three disease-specific subscales or their average, i.e., kidney disease component summary (KDCS), and age and sex were included as the explanatory variables. Predictive performance was assessed by mean absolute error (MAE) and root mean square error (RMSE) using 10-fold cross-validation.
Results
Mixture models outperformed linear regression and response mapping. When mapping to EQ-5D-3L, the ALDVMM model was the best-performing one for France, Germany and Spain while beta regression was best for Italy. When mapping to EQ-5D-5L, the ALDVMM model also demonstrated the best predictive performance. Generally, models using KDQOL-36 subscale scores showed better fit than using the KDCS.
Conclusions
This study adds to the growing literature suggesting the better performance of the mixture models in modelling EQ-5D and produces algorithms to map the KDQOL-36 onto EQ-5D-3L (for France, Germany, Italy, and Spain) and EQ-5D-5L (for Singapore).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The number of patients with end-stage renal disease (ESRD) is projected to increase substantially, driven by the ageing population and the rising number of people with diabetes, hypertension, and obesity [1, 2]. Due to the limited organ donors, the majority of ESRD patients have to receive maintenance dialysis and, therefore, the care for these patients has focused on improving their health-related quality of life (HRQoL) [3]. Currently, there are numerous HRQoL measures being used in patients with dialysis. In particular, the disease-specific instrument, Kidney Disease Quality of Life 36-Item Short Form Survey (KDQOL-36), is the most frequently used one in these patients and its validity and reliability has been demonstrated previously [4,5,6]. The KDQOL-36 has also been recommended by the United States Centers for Medicare and Medicaid to periodically collect HRQoL data for dialysis patients [7] so that the results could be used to inform and support clinicians in their decision-making and furthermore contribute to the development of clinical interventions to provide better care for dialysis patients.
KDQOL-36 consists of the Short Form 12-Item (SF-12) instrument to capture the general physical and mental well-being of the patient plus 24 items on kidney disease- and dialysis-related symptoms, effects, and burden [8]. Nevertheless, KDQOL-36 instrument is not preference-based and, therefore, does not allow the calculation of health utilities for quality-adjusted life years (QALYs) estimates. The QALYs could provide a generic health outcome comparable across disease areas and are recommended by decision makers such as the National Institute of Health and Care Excellence (NICE) [9] in their assessment of the cost-effectiveness of health care interventions. The EQ-5D is the preferred preference-based instrument to provide health utility estimates to enable QALYs calculations in the context of NICE appraisals [9]. But EQ-5D has not been a routine measure for dialysis patients and EQ-5D data of these patients is limited in literature [10]. Given the widespread use of KDQOL-36 among dialysis patients and the recommendation of using KDQOL-36 in the clinical setting, it is expected that HRQoL data measured using KDQOL-36 is accumulating. In such circumstance, the availability of a valid mapping algorithm from KDQOL-36 onto EQ-5D would make it possible to use the KDQOL-36 data in estimating health utilities for cost-effectiveness analysis (CEA). According to the Health Economics Research Centre Database of Mapping Studies [11], there is no mapping algorithm yet to map from KDQOL-36 to EQ-5D. One alternative approach is to use the currently available mapping algorithms from SF-12 onto EQ-5D [12,13,14,15], but these algorithms do not show the complete picture of KDQOL-36 (only includes 12 items of KDQOL-36) and may not produce the reliable estimates. This concern has been supported by one recently published study which reported that the EQ-5D scores mapped from SF-12 would underestimate the QALYs gained in cost-utility analysis compared to the observed EQ-5D [16], and thus there is a necessity for developing new methods to enable better health utility estimates from KDQOL-36 data for future economic evaluations in dialysis patients when EQ-5D data are not available.
Therefore, this study aimed to produce mapping algorithms from KDQOL-36 to generic EQ-5D as well as to provide a user-friendly tool for implementation.
Methods
Outcome measures
KDQOL-36
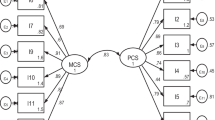
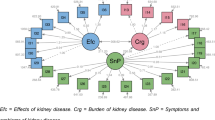
The KDQOL-36 is a 36-item self-reported questionnaire that combines the generic SF-12 instrument with disease-specific component for assessing the HRQoL of chronic kidney disease patients, adapted from the original 134-item KDQOL and the 76-item KDQOL Short Form (KDQOL-SF), with a 4-week recall period [8]. The SF-12 is the shorter version of the Short Form 36-Item (SF-36), one of the most popular generic worldwide instruments for evaluating HRQoL. It includes 12 items about general health, activity limits, ability to accomplish desired tasks, depression and anxiety, energy level, and social activities; there are 2–6 response levels for items [13]. The disease-specific component has 24 items comprising three subscales, burden of kidney disease (4 items), symptoms/problems of kidney disease (12 items), and effects of kidney disease (8 items), with 5 response levels for each item to measure how much the disease interferes with daily life and how bothered the respondent feels by symptoms/problems and the restrictions due to dialysis. The 12 items of SF-12 could be used to derive two summary measures, physical component summary (PCS) and mental component summary (MCS), ranging from 0 to 100 [17]. Responses to the three disease-specific subscales are transformed linearly to scores ranging from 0 to 100 and can be summated into the kidney disease component summary (KDCS) score [18]. As there is no overall KDQOL-36 score that incorporates all of its subscale scores, the following scores were calculated separately: PCS, MCS, burden of kidney disease (Burden), symptoms/problems of kidney disease (Symptoms), and effects of kidney disease (Effect), using the Excel file provided by the RAND Corporation [19]; and then KDCS was calculated by averaging the three disease-specific subscale scores. For all scores, higher values indicating better self-reported quality of life.
EQ-5D
The EQ-5D instrument has 5 items (mobility, self-care, usual activities, pain/discomfort, and anxiety/depression) [20] measuring the health on the day of survey with 3 or 5 descriptive levels for each item. In the 3-level version of EQ-5D (EQ-5D-3L), respondents choose one of three levels, ranging from ‘no problems’, ‘some/moderate problems’ to ‘unable/extreme problems’ while in the 5-level version (EQ-5D-5L), respondents choose their responses from five levels including no problems, slight problems, moderate problems, severe problems, and extreme problems. For both versions of EQ-5D, responses to the five items define a health state for which an index score can be generated to indicate its value to the general public. The index score is anchored by 0 (death) and 1 (full health), with higher scores corresponding to higher utility.
Data
Data from two cross-sectional studies were used to develop mapping algorithms from KDQOL-36 onto EQ-5D-3L and EQ-5D-5L, respectively.
EQ-5D-3L
The dataset from the Adelphi CKD Disease-Specific Programme [21], a cross-sectional survey, was used to develop mapping algorithms from KDQOL-36 to EQ-5D-3L, including dialysis patients across five countries: France (n = 299), Germany (n = 413), Italy (n = 278), Spain (n = 225) and the UK (n = 34) [22]. The data included complete information on patients’ HRQoL measured using KDQOL-36 and EQ-5D-3L and patients’ demographic characteristics (e.g., age and sex). The country-specific EQ-5D-3L value sets [23,24,25,26,27] were used to calculate the EQ-5D-3L scores and then these scores were used for developing mapping algorithms for France, Germany, Italy and Spain, respectively, but not for the UK because of the small sample size (n = 34) [32].
EQ-5D-5L
Another dataset from a cross-sectional study in Singapore (n = 163) including patients undergoing dialysis for at least 3 months with complete data on KDQOL-36 and EQ-5D-5L was used to develop mapping algorithms onto EQ-5D-5L [28]. Patients’ socio-demographic characteristics were also available. The EQ-5D-5L value set for Singapore (unpublished data) was used to calculate the EQ-5D-5L scores. As there was no other dataset available with information on both KDQOL-36 and EQ-5D-5L, the mapping algorithms from KDQOL-36 to EQ-5D-5L were developed for Singapore only.
Statistical analysis
Correlation
The estimation of a mapping algorithm relies on there being conceptual overlap between the source and the target measures [29], so the KDQOL-36 and EQ-5D are expected to be correlated. Spearman rank correlations were used to test the correlations between the KDQOL-36 subscale scores and EQ-5D index scores or item responses. The strength of correlation was defined as low, moderate, high, and very high with coefficient value of 0.30–0.49, 0.50–0.69, 0.70–0.89, and 0.90-1, respectively [30]. The correlations between the KDQOL-36 subscale scores were also tested and two highly correlated scores were not included in the same regression model. The correlations between the EQ-5D items were also explored.
Model development
A range of statistical models have been used in the literature for the development of mapping algorithms [11], in attempts to account for the unique distribution of EQ-5D: it is commonly skewed, multimodal, and often has one peak at 1 (indicating full health), bounded top and bottom (indicating best and worse health states) and a gap between 1 and the next feasible value. Generally, there are two broad approaches to mapping, direct mapping, which models the EQ-5D index values themselves using regression models, and indirect mapping, also referred to as response mapping, which models responses to each item of EQ-5D and then calculates the predicted utilities as a separate second step.
Direct mapping
Ordinary least squares (OLS) regression is the most commonly used model in direct mapping by assuming the relationship between the dependent variable (EQ-5D index values) and the independent variables can be expressed as a linear function [31]. OLS models are able to predict mean values with reasonable accuracy, but are poor at predicting those in poor health and full health [32], and the predicted values may fall outside of the plausible range.
To allow for the bounded nature of EQ-5D, mixture beta regression model could be used, as suggested by Basu and Manca [33]. This is a two-part model consisting of a multinomial logit model and a beta mixture model. It allows the estimation of dependent variables that are discrete at the bottom limit (i.e., the worst health state), at the truncation point (i.e., the second-best health state), and at the upper limit (i.e., full health), and continuous between the bottom limit and the upper limit. This method has been used in some mapping studies [34, 35] and has been shown to be more robust than OLS [36, 37].
Another mixture model which was specially developed to deal with the distributional features of EQ-5D is known as the adjusted limited dependent variable mixture model (ALDVMM) [38]. It has been shown to perform better than models used traditionally in this area [34]. It uses a mixture of adjusted normal distributions to account for the multimodality of EQ-5D by assuming that EQ-5D can be modelled as a mixture of C-components, which represent the clusters of individuals with similar utility scores. It also accounts for the peak of observations at full health and the option of a gap in the distribution below that peak, referred as truncation point as with mixture beta regression. The ALDVMM has been used with success in previous mapping studies [39,40,41].
Response mapping
In response mapping for EQ-5D, the five regression models, each for one item, together estimate the discrete distribution for all the health status in EQ-5D. The expected EQ-5D score is the average of all possible health states utilities weighted by the individual predicted probabilities. It should be noted that response mapping models require observations (preferably a sizeable number) at all levels of each item [34] and this can be a problem for EQ-5D-5L if the dataset is small and some of the item levels may not be selected by respondents. Regression models used in response mapping include multinomial logit [15], ordered logistic [42], and ordered probit [41], but these models do not account for the correlations between EQ-5D items, which may lead to biased predictions. To take the correlations into account, a recently published study applied response mapping using seemingly unrelated ordered probit models for developing mapping algorithms, although its performance was not as good as mixture models [39].
Mapping algorithms were derived in this study using all the four of the aforementioned regression methods: OLS, mixture beta regression (BETAMIX), ALDVMM, and seemingly unrelated ordered probit models (SUROPM). ALDVMM with up to three components were tested in line with methods used by the developers of the approach [38]. All analyses were undertaken in Stata using the command “regress” for OLS, “betamix” [43] for mixture beta regression, “aldvmm” for ALDVMM and “cmp” for SUROPM. The index values for the bottom limit, truncation point and upper limit were obtained from the value set specific to the country and EQ-5D version (EQ-5D-3L/EQ-5D-5L). As the country-specific EQ-5D value sets were used to calculate the EQ-5D index values, the mapping algorithms were developed for each country separately, i.e., EQ-5D-3L for France, Germany, Spain and Italy, and EQ-5D-5L for Singapore. For response mapping to EQ-5D-3L, we pooled the data of patients from the four countries together to develop the algorithms to the item responses first and then used the country-specific value sets to estimate the EQ-5D-3L index values. In supplementary analysis, we applied one value set, i.e., the UK EQ-5D-3L value set [27], to the pooled data of patients from five countries and then performed the same analyses.
As described previously, the KDQOL-36 is made up of a set of subscales scores: PCS, MCS, symptoms, effects, burden and KDCS. We mapped from the KDQOL-36 to EQ-5D using two sets of explanatory variables. First, PCS, MCS and the disease-specific summary score (i.e., KDCS) were included. Second, PCS, MCS and the disease-specific subscales scores (i.e., Symptoms, Effects and Burden) were used. We also included squared terms and all possible two-way interaction terms of KDQOL-36 subscale scores in regression models to address potential nonlinear associations. Age and sex of the patient were included in the regression models, but no other demographic or clinical covariates, to facilitate the use of the mapping algorithms to a wide range of dataset.
Model performance
To assess the model performance, we used the 10-fold cross-validation procedure [44]. The full sample was randomly split into 10 equally sized groups. Each combination of nine groups formed a training dataset that was used to estimate the parameters of the regression model, while the remaining group was considered as a test dataset to generate the predicted EQ-5D values based on the model developed using the training dataset. Predicted scores and observed scores were compared and mean absolute error (MAE) and root mean square error (RMSE) were calculated. This procedure was repeated until all the 10 possible training datasets were tested.
Models were ranked based on MAE and RMSE and the two rankings were summated to generate an average ranking. The model with the lowest value in average ranking would be the best-performing one [45, 46]. In the event of there being no clear difference between models, we gave priority to the model with lowest RMSE value.
All models were estimated in Stata version 15.1 (Stata Corp, College Station, TX).
Results
Descriptive information
Patient characteristics and summary statistics for the outcome measures are presented in Table 1. The mean age ranged from 60.5 to 66.6 years and there were more males (range 52.2%–62.5%) in all samples. The mean EQ-5D-3L score reported by patients from France, Germany, Italy and Spain was 0.622, 0.796, 0.864 and 0.746, respectively, with more than 30% patients reporting full health in Italy (37.77%) and Spain (35.11%) and about 20% in France (20.74%) and Germany (21.31%). The mean EQ-5D-5L score reported by patients from Singapore was 0.621, lower than the EQ-5D-3L scores, and 25.8% patients reported full health. Figures 1 and 2 show the distribution of EQ-5D-3L and EQ-5D-5L scores. For both EQ-5D-3L and EQ-5D-5L, the distribution is highly skewed, has a spike of observations at full health and displays the gap between full health and the next feasible state. It should be noted that the EQ-5D-3L scores had different distributions across countries (Fig. 1), which may result from the country-specific value sets and patient samples differing in health status.
The KDQOL-36 subscale scores were similar in all five samples, but patients from Italy had higher scores in PCS, KDCS, and three disease-specific subscale scores, indicating better physical health, fewer symptoms, fewer effects on daily life and less self-perceived burden to family, consistent with the highest EQ-5D scores and more patients with full health reported by them (Table 1).
Correlation
The Spearman rank correlation coefficients between the KDQOL-36 subscale scores and the EQ-5D index scores and items is presented in Table S1. Generally, the correlations between KDQOL-36 subscale scores and EQ-5D-3L index scores or item responses were moderate to high, although some low correlations were observed. The correlations between KDQOL-36 subscales and EQ-5D-5L index scores or item responses were low to moderate. These suggest that the two instruments overlap to some extent, which could support the attempt of mapping from one to the other.
Table S2 presents the correlations between KDQOL-36 subscale scores (excluding correlations between KDCS and the three disease-specific subscale scores, as KDCS is the average of the three scores). There was no high correlation between any two scores, so they could be included in one regression model.
The correlations between EQ-5D items were low to moderate (Table S3), supporting our approach of using seemingly unrelated regression models in response mapping, which could account for the correlations between items.
Model
EQ-5D-3L
The results of the model performance mapping KDQOL-36 to EQ-5D-3L are presented in Table 2 (for France) and Table S4-S6 (for Germany, Italy and Spain).
For France, of all the 30 models tested, RMSEs ranged from 0.2328 to 0.2825 and MAEs were between 0.1730 and 0.2102. The results of some ALDVMMs were not included if there were problems with convergence. According to MAE and RMSE, the best-performing model was ALDVMM with 2-component, which included PCS, MCS, Symptoms, Effects, Burden, and their squared terms and interaction terms, as well as age and sex as explanatory variables. For Germany, a total of 30 models were tested, among which the ADVLMM with 2-component including PCS, MCS, disease-specific subscales, age and sex as explanatory variables showed the lowest overall ranking based on MAE and RMSE. For Italy, 25 models were tested as some of the ALDVMM had problems with convergence. In contrast with the results for France and Germany, the best-performing model was the BETAMIX model including PCS, MCS, Symptoms, Effects, Burden, their squared terms, and age and sex as explanatory variables. For Spain, 28 models were tested and the best-performing one was the ALDVMM with one component including PCS, MCS, KDCS, age and sex as explanatory variables. Results of the model using the UK EQ-5D-3L value set are available in Table S7 and the best-performing model was the same one as that for France.
Figure 3 plots mean predicted versus mean observed EQ-5D-3L values of the best-performing model for the four countries. The figures show that these mapping algorithms seem to predict well for patients at the high end of EQ-5D-3L, but may not predict very well for patients scoring at the low end of the EQ-5D-3L.
EQ-5D-5L
The results of the model performance mapping KDQOL-36 to EQ-5D-5L are presented in Table 3. In total, 34 models were tested and the best-performing one was ALDVMM with 1-component including PCS, MCS, Symptoms, Effects, Burden, age and sex as explanatory variables. Figure 4 plots mean predicted versus mean observed EQ-5D-5L values of this best-performing model, showing that this algorithm could fit the observed data closely, but may over-predict the values when the EQ-5D observed scores were lower than 0.
The best-performing algorithms estimated in this study can be easily implemented via Excel, which is provided in the Supplementary Materials.
Discussion
This study aimed to develop mapping algorithms to predict EQ-5D-3L and EQ-5D-5L utility scores from the widely used KDQOL-36 instrument in the absence of directly collected EQ-5D data. By exploring different regression techniques, the algorithms using mixture models showed better predictive ability than the commonly used linear regression and response mapping models. Given the lack of previous mapping studies in this disease area and the increasing use of KDQOL-36 in the clinical setting, the mapping algorithms would provide reliable estimates for the calculation of the EQ-5D-3L and EQ-5D-5L scores as a function of KDQOL-36 and the user-friendly tool would enable researchers to implement the algorithms for EQ-5D utility values generation in applied CEA studies.
We found that the mixture models offer better model fit than linear regression and response mapping, consistent with the growing literature showing the superiority of mixture models in modelling EQ-5D [39,40,41]. But the target instrument in these studies was EQ-5D-3L, and our results also demonstrated the better performance of ALDVMM model in modelling EQ-5D-5L. Therefore, these findings would support the suggestion that the mixture models should be included when mapping EQ-5D from clinical measures [47], although the mapping guidelines do not recommend a specific mapping technique [48, 49].
It should be noted that the best-performing model is different in terms of regression techniques and explanatory variables for different countries and different EQ-5D versions. First, ALDVMM was the best-performing model in modelling EQ-5D-3L scores in France, Germany and Spain, but beta regression showed best fit for Italy. This may be explained by the characteristics of patients from Italy. As shown in Table 1, they reported the highest KDCS scores while the scores of patients from France, Germany and Spain were similar, and thus it is likely that they had better health than other patients did, so the mapping algorithms based on samples differing in health status were not expected to be the same. In addition, there was a strong ceiling effect of the EQ-5D-3L data for Italy (Fig. 1), which may limit the advantage of ALDVMM in addressing the multimodality of data. This may suggest the importance of considering the distribution when selecting the most appropriate model for modelling EQ-5D data, and thus future research is suggested to investigate it further. Second, the models including the KDQOL-36 disease-specific subscales scores as explanatory variables had a model fit superior to those including KDCS, but this was not the case for Spain. This may be because the three disease-specific subscale scores were highly skewed for Spain and the KDCS, which condenses them into one score, could better reflect the differences between patients, although it would discard important information. As the subscales of KDQOL-36 could be easily calculated using the Excel file provided by the instrument developer [19], the use of the KDCS is still practical to researchers populating cost-effectiveness models. Furthermore, the mapping algorithms are different when mapping to EQ-5D-3L and to EQ-5D-5L in terms of the explanatory variables included. Undoubtedly, the country-specific value set used to generate index values would contribute to the differences, but these would also be driven by the differences between the two versions of EQ-5D. The differences in the utility estimates using EQ-5D-3L and EQ-5D-5L have been reported in literature [50] and, therefore, they should not be used interchangeably. As the EQ-5D-5L is increasingly being used in practice and more EQ-5D-5L value sets are published, the results of this study suggesting the better model fit of the mixture model would help future researchers to select the appropriate model when modelling EQ-5D-5L.
This study has limitations. First, the mapping algorithms did not perform well at the low end of the EQ-5D, as illustrated in Figs. 3 and 4. This was an expected consequence of the shape of the EQ-5D distribution and the poor performance at the tails of EQ-5D distribution is a limitation common to many mapping studies [32]. Although the mixture models have been used, the impact of the distribution of EQ-5D data could not be fully addressed by the models. Second, the sample size used to derive mapping algorithms to EQ-5D-5L was small (n = 163). The sample size used to develop mapping algorithms should be taken into consideration when carrying out mapping [32]. This would affect the response mapping more as the models require observations at all the five levels of the EQ-5D items and a very small number of patients choosing the ‘extreme problems’ level would bias the estimation of the parameters and further limit the model performance. A larger sample would be preferable to increase the statistical power and thus lead to improved precision in estimating parameters. Third, the validity of the mapping algorithms was assessed using 10-fold cross-validation procedure. It would be preferred to assess the generalisability of the algorithms in another independent dataset; however, this was not available when conducting this study.
When such algorithms mapping the KDQOL-36 onto EQ-5D were not available, researchers who would like to generate EQ-5D values for CEAs using KDQOL-36 data have to rely on the SF-12-based functions, however, the use of these mapping functions have been found to greatly affect the QALYs estimates [16]. This study provides methods of using KDQOL-36 data to generate EQ-5D-3L and EQ-5D-5L scores. Given the requirement that the KDQOL-36 should be used in US clinical setting to assess patients’ HRQoL annually [4], it is expected that the KDQOL-36 would be more widely used in other countries to periodically collect data from patients. The algorithms developed here would provide an alternative to estimate EQ-5D from a large sample and potentially contribute to modelling the HRQoL change in CEAs assessing interventions or treatments for dialysis patients in the long-term time horizon. But it should be noted that although the mapping algorithms could provide reliable EQ-5D health utility estimates from KDQOL-36, mapping to obtain EQ-5D health utility values is still a ‘second-best’ solution [45].
Conclusion
To the best of our knowledge, this is the first study to develop mapping algorithms from the widely used KDQOL-36 to EQ-5D-3L and EQ-5D-5L utility scores. Mapping algorithms using mixture models were found to be better than the linear regression and response mapping. A user-friendly freely accessible tool was provided to assist the implementation of these algorithms. Although it is preferred to use utilities directly derived from the EQ-5D, the algorithms can be used to generate reliable utility estimates in future economic evaluations of health care interventions for ESRD patients undergoing dialysis.
References
Jha, V., Garcia-Garcia, G., Iseki, K., Li, Z., Naicker, S., Plattner, B., Saran, R., Wang, A.Y., Yang, C.W.: Chronic kidney disease: global dimension and perspectives. Lancet 382(9888), 260–272 (2013). https://doi.org/10.1016/S0140-6736(13)60687-X
White, S.L., Chadban, S.J., Jan, S., Chapman, J.R., Cass, A.: How can we achieve global equity in provision of renal replacement therapy? Bull. World Health Organ. 86(3), 229–237 (2008)
Finkelstein, F.O., Arsenault, K.L., Taveras, A., Awuah, K., Finkelstein, S.H.: Assessing and improving the health-related quality of life of patients with ESRD. Nat Rev Nephrol 8(12), 718–724 (2012). https://doi.org/10.1038/nrneph.2012.238
Peipert, J.D., Bentler, P.M., Klicko, K., Hays, R.D.: Psychometric properties of the kidney disease quality of life 36-item short-form survey (KDQOL-36) in the United States. Am. J. Kidney Dis. 71(4), 461–468 (2018). https://doi.org/10.1053/j.ajkd.2017.07.020
Chen, J.Y., Choi, E.P., Wan, E.Y., Chan, A.K., Tsang, J.P., Chan, K.H., Lo, W.K., Lui, S.L., Chu, W.L., Lam, C.L.: Validation of the disease-specific components of the kidney disease quality of life-36 (KDQOL-36) in Chinese patients undergoing maintenance dialysis. PLoS One 11(5), e0155188 (2016). https://doi.org/10.1371/journal.pone.0155188
Yang, F., Wang, V.W., Joshi, V.D., Lau, T.W., Luo, N.: Validation of the english version of the kidney disease quality of life questionnaire (KDQOL-36) in haemodialysis patients in Singapore. Patient 6(2), 135–141 (2013). https://doi.org/10.1007/s40271-013-0015-2
Register, F.: Medicare and medicaid programs; conditions for coverage for end-stage renal disease facilities; final rule. https://www.cms.gov/Regulations-and-Guidance/Legislation/CFCsAndCoPs/Downloads/ESRDfinalrule0415.pdf (2008). Accessed 3 Oct 2018
Hays, R.D., Kallich, J.D., Mapes, D.L., Coons, S.J., Carter, W.B.: Development of the kidney disease quality of life (KDQOL) instrument. Qual. Life Res. 3(5), 329–338 (1994)
Rabin, R., de Charro, F.: EQ-5D: a measure of health status from the EuroQol Group. Ann. Med. 33(5), 337–343 (2001)
Wyld, M., Morton, R.L., Hayen, A., Howard, K., Webster, A.C.: A systematic review and meta-analysis of utility-based quality of life in chronic kidney disease treatments. PLoS Med. 9(9), e1001307 (2012). https://doi.org/10.1371/journal.pmed.1001307
Dakin, H., Abel, L., Burns, R., Yang, Y.: Review and critical appraisal of studies mapping from quality of life or clinical measures to EQ-5D: an online database and application of the MAPS statement. Health Qual Life Outcomes 16(1), 31 (2018). https://doi.org/10.1186/s12955-018-0857-3
Franks, P., Lubetkin, E.I., Gold, M.R., Tancredi, D.J.: Mapping the SF-12 to preference-based instruments: convergent validity in a low-income, minority population. Med. Care 41(11), 1277–1283 (2003). https://doi.org/10.1097/01.MLR.0000093480.58308.D8
Franks, P., Lubetkin, E.I., Gold, M.R., Tancredi, D.J., Jia, H.: Mapping the SF-12 to the EuroQol EQ-5D index in a national US sample. Med. Decis. Mak. 24(3), 247–254 (2004)
Lawrence, W.F., Fleishman, J.A.: Predicting EuroQoL EQ-5D preference scores from the SF-12 Health Survey in a nationally representative sample. Med. Decis. Mak. 24(2), 160–169 (2004). https://doi.org/10.1177/0272989X04264015
Gray, A.M., Rivero-Arias, O., Clarke, P.M.: Estimating the association between SF-12 responses and EQ-5D utility values by response mapping. Med. Decis. Mak. 26(1), 18–29 (2006). https://doi.org/10.1177/0272989X05284108
Yang, F., Devlin, N., Luo, N.: Impact of mapped EQ-5D utilities on cost-effectiveness analysis: in the case of dialysis treatments. Eur. J. Health Econ. (2018). https://doi.org/10.1007/s10198-018-0987-x
Ware Jr., J., Kosinski, M., Keller, S.D.: A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med. Care 34(3), 220–233 (1996)
Saban, K.L., Bryant, F.B., Reda, D.J., Stroupe, K.T., Hynes, D.M.: Measurement invariance of the kidney disease and quality of life instrument (KDQOL-SF) across veterans and non-veterans. Health Qual Life Outcomes 8, 120 (2010). https://doi.org/10.1186/1477-7525-8-120
https://www.rand.org/health-care/surveys_tools/kdqol.html. Accessed 20 June 2019
Rabin, R., de Charro, F.: EQ-5D: a measure of health status from the EuroQol group. Ann. Med. 33(5), 337–343 (2001). https://doi.org/10.3109/07853890109002087
Anderson, P., Benford, M., Harris, N., Karavali, M., Piercy, J.: Real-world physician and patient behaviour across countries: disease-specific programmes—a means to understand. Curr. Med. Res. Opin. 24(11), 3063–3072 (2008). https://doi.org/10.1185/03007990802457040
Eriksson, D., Goldsmith, D., Teitsson, S., Jackson, J., van Nooten, F.: Cross-sectional survey in CKD patients across Europe describing the association between quality of life and anaemia. BMC Nephrol 17(1), 97 (2016). https://doi.org/10.1186/s12882-016-0312-9
Chevalier, J., de Pouvourville, G.: Valuing EQ-5D using time trade-off in France. Eur J Health Econ 14(1), 57–66 (2013). https://doi.org/10.1007/s10198-011-0351-x
Claes, C., Greiner, W., Uber, A., Graf von der Schulenburg, J.: An interview-based comparison of the TTO and VAS values given to EuroQol states of health by the general German population. In: Proceedings of the 15th Plenary Meeting of the EuroQol Group. Hannover, Germany: Centre for Health Economics and Health Systems Research, University of Hannover, pp. 13–38 (1999)
Scalone, L., Cortesi, P.A., Ciampichini, R., Belisari, A., D’Angiolella, L.S., Cesana, G., Mantovani, L.G.: Italian population-based values of EQ-5D health states. Value Health 16(5), 814–822 (2013). https://doi.org/10.1016/j.jval.2013.04.008
Badia, X., Roset, M., Herdman, M., Kind, P.: A comparison of United Kingdom and Spanish general population time trade-off values for EQ-5D health states. Med. Decis. Mak. 21(1), 7–16 (2001). https://doi.org/10.1177/0272989X0102100102
Dolan, P.: Modeling valuations for EuroQol health states. Med. Care 35(11), 1095–1108 (1997)
Yang, F., Lau, T., Lee, E., Vathsala, A., Chia, K.S., Luo, N.: Comparison of the preference-based EQ-5D-5L and SF-6D in patients with end-stage renal disease (ESRD). Eur.J. Health Econ. 16(9), 1019–1026 (2015). https://doi.org/10.1007/s10198-014-0664-7
Round, J., Hawton, A.: Statistical alchemy: conceptual validity and mapping to generate health state utility values. Pharm. Open 1(4), 233–239 (2017). https://doi.org/10.1007/s41669-017-0027-2
Hinkle, D.E., Wiersma, W., Jurs, S.G.: Applied statistics for the behavioral sciences, vol. 663. Houghton Mifflin, Boston (2003)
Brazier, J.E., Yang, Y., Tsuchiya, A., Rowen, D.L.: A review of studies mapping (or cross walking) non-preference based measures of health to generic preference-based measures. Eur J Health Econ 11(2), 215–225 (2010). https://doi.org/10.1007/s10198-009-0168-z
Longworth, L., Yang, Y., Young, T., Mulhern, B., Hernandez Alava, M., Mukuria, C., Rowen, D., Tosh, J., Tsuchiya, A., Evans, P., Devianee Keetharuth, A., Brazier, J.: Use of generic and condition-specific measures of health-related quality of life in NICE decision-making: a systematic review, statistical modelling and survey. Health Technol. Assess. 18(9), 1–224 (2014). https://doi.org/10.3310/hta18090
Basu, A., Manca, A.: Regression estimators for generic health-related quality of life and quality-adjusted life years. Med. Decis. Mak. 32(1), 56–69 (2012). https://doi.org/10.1177/0272989X11416988
Gray, L.A., Hernandez Alava, M., Wailoo, A.J.: Development of methods for the mapping of utilities using mixture models: mapping the AQLQ-S to the EQ-5D-5L and the HUI3 in patients with asthma. Value Health 21(6), 748–757 (2018). https://doi.org/10.1016/j.jval.2017.09.017
Kent, S., Gray, A., Schlackow, I., Jenkinson, C., McIntosh, E.: Mapping from the Parkinson’s disease questionnaire PDQ-39 to the generic EuroQol EQ-5D-3L: the value of mixture models. Med. Decis. Mak. 35(7), 902–911 (2015). https://doi.org/10.1177/0272989X15584921
Khan, I., Morris, S., Pashayan, N., Matata, B., Bashir, Z., Maguirre, J.: Comparing the mapping between EQ-5D-5L, EQ-5D-3L and the EORTC-QLQ-C30 in non-small cell lung cancer patients. Health Qual Life Outcomes 14, 60 (2016). https://doi.org/10.1186/s12955-016-0455-1
Khan, K.A., Madan, J., Petrou, S., Lamb, S.E.: Mapping between the Roland Morris Questionnaire and generic preference-based measures. Value Health 17(6), 686–695 (2014). https://doi.org/10.1016/j.jval.2014.07.001
Hernandez Alava, M., Wailoo, A.J., Ara, R.: Tails from the peak district: adjusted limited dependent variable mixture models of EQ-5D questionnaire health state utility values. Value Health 15(3), 550–561 (2012). https://doi.org/10.1016/j.jval.2011.12.014
Gray, L.A., Wailoo, A.J., Hernandez Alava, M.: Mapping the FACT-B instrument to EQ-5D-3L in patients with breast cancer using adjusted limited dependent variable mixture models versus response mapping. Value Health 21(12), 1399–1405 (2018). https://doi.org/10.1016/j.jval.2018.06.006
Wailoo, A., Hernandez, M., Philips, C., Brophy, S., Siebert, S.: Modeling health state utility values in ankylosing spondylitis: comparisons of direct and indirect methods. Value Health 18(4), 425–431 (2015). https://doi.org/10.1016/j.jval.2015.02.016
Hernandez Alava, M., Wailoo, A., Wolfe, F., Michaud, K.: A comparison of direct and indirect methods for the estimation of health utilities from clinical outcomes. Med. Decis. Mak. 34(7), 919–930 (2014). https://doi.org/10.1177/0272989X13500720
van Hout, B., Janssen, M.F., Feng, Y.S., Kohlmann, T., Busschbach, J., Golicki, D., Lloyd, A., Scalone, L., Kind, P., Pickard, A.S.: Interim scoring for the EQ-5D-5L: mapping the EQ-5D-5L to EQ-5D-3L value sets. Value Health 15(5), 708–715 (2012). https://doi.org/10.1016/j.jval.2012.02.008
Gray, L.A., Alava, M.H.: A command for fitting mixture regression models for bounded dependent variables using the beta distribution. Sata J. 18(1), 51–75 (2018)
Wong, C.K., Lam, C.L., Rowen, D., McGhee, S.M., Ma, K.P., Law, W.L., Poon, J.T., Chan, P., Kwong, D.L., Tsang, J.: Mapping the functional assessment of cancer Therapy-general or -Colorectal to SF-6D in Chinese patients with colorectal neoplasm. Value Health 15(3), 495–503 (2012). https://doi.org/10.1016/j.jval.2011.12.009
Longworth, L., Rowen, D.: Mapping to obtain EQ-5D utility values for use in NICE health technology assessments. Value Health 16(1), 202–210 (2013). https://doi.org/10.1016/j.jval.2012.10.010
Ara, R., Rowen, D., Mukuria, C.: The use of mapping to estimate health state utility values. Pharmacoeconomics 35(Suppl 1), 57–66 (2017). https://doi.org/10.1007/s40273-017-0548-7
Coca Perraillon, M., Shih, Y.C., Thisted, R.A.: Predicting the EQ-5D-3L preference index from the SF-12 health survey in a national US Sample: a finite mixture approach. Med. Decis. Mak. 35(7), 888–901 (2015). https://doi.org/10.1177/0272989X15577362
Petrou, S., Rivero-Arias, O., Dakin, H., Longworth, L., Oppe, M., Froud, R., Gray, A.: preferred reporting items for studies mapping onto preference-based outcome measures: the MAPS statement. Pharmacoeconomics 33(10), 985–991 (2015). https://doi.org/10.1007/s40273-015-0319-2
Wailoo, A.J., Hernandez-Alava, M., Manca, A., Mejia, A., Ray, J., Crawford, B., Botteman, M., Busschbach, J.: Mapping to estimate health-state utility from non-preference-based outcome measures: an ISPOR good practices for outcomes research task force report. Value Health 20(1), 18–27 (2017). https://doi.org/10.1016/j.jval.2016.11.006
Law, E.H., Pickard, A.S., Xie, F., Walton, S.M., Lee, T.A., Schwartz, A.: Parallel valuation: a direct comparison of EQ-5D-3L and EQ-5D-5L societal value Sets. Med. Decis. Mak. 38(8), 968–982 (2018). https://doi.org/10.1177/0272989X18802797
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Yang, F., Wong, C.K.H., Luo, N. et al. Mapping the kidney disease quality of life 36-item short form survey (KDQOL-36) to the EQ-5D-3L and the EQ-5D-5L in patients undergoing dialysis. Eur J Health Econ 20, 1195–1206 (2019). https://doi.org/10.1007/s10198-019-01088-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-019-01088-5