Abstract
Background
The aim of this study was to evaluate the safety, effectiveness, and health-related QOL impact of early rehabilitation in patients with nephrotic syndrome.
Methods
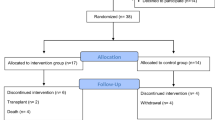
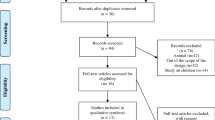
Subjects consisted of 23 patients with nephrotic syndrome who had previously received steroid treatment. Patients worked performed quadriceps resistance training and aerobic training 5 days per week for 5 weeks. Urinary protein, albumin (Alb), creatinine (Cre), and blood urea nitrogen (BUN) were monitored once every week over a 5-week period based on medical records. The 36-item short form health survey (SF-36) score was used to evaluate health-related QOL.
Results
There was no significant difference in quadriceps force and no significant effect of age as shown by ANCOVA. Anaerobic threshold (AT) and peak oxygen consumption (peak VO2) both increased significantly. AT was affected by the degree of change in body weight according to ANCOVA. Cre and BUN were not significantly altered. Urinary protein showed a significant decrease and Alb was significantly increased. Only physical function (PF) in the SF-36 showed a significant improvement following the intervention.
Conclusion
Our data indicate that early rehabilitation involving quadriceps resistance training and aerobic training for nephrotic syndrome is safe and effective.



Similar content being viewed by others
References
Imai E, Horio M, Iseki K, et al. Prevalence of chronic kidney disease (CKD) in the Japanese general population predicted by the MDRD equation modified by a Japanese coefficient. Clin Exp Nephrol. 2007;11:156–63.
Molsted A, Prescott L, Heaf J, et al. Assessment and clinical aspects of health-related quality of life in dialysis patients and patients with chronic kidney disease. Nephron Clin Pract. 2007;106:24–33.
Odden MC, Whooley MA, Shlipak MG. Association of chronic kidney disease and anemia with physical capacity: The heat and soul study. J Am Soc Nephrol. 2004;15:2908–15.
NKF-K/DOQI. K/DOQI clinical practice guideline for cardiovascular disease in dialysis patients. Am J Kidney Dis. 2005;45:1–128.
Castaneda C, Gordon PL, Parker RC, et al. Resistance training to reduce the malnutrition-inflammation complex syndrome of chronic kidney disease. Am J Kidney Dis. 2004;43:607–16.
Pupim LB, Flakoll PJ, Levenhagen DK, et al. Exercise augments the acute anabolic effects of intradialytic parenteral nutrition in chronic hemodialysis patients. Am J Physiol. 2004;286:E589–97.
Leaf DA, MacRae HS, Grant E, et al. Isometric exercise increase the size of forearm veins in patients with chronic renal failure. Am J Med Sci. 2003;325:115–9.
Delingiannis A, Kouidi E, Tourkantonis A. Effects of physical training on heart rate variability in patients on hemodialysis. Am J Cardiol. 1999;84:197–202.
Nishi S, Ubara Y, Utsunomiya Y, et al. Evidence-based clinical practice guidelines for nephrotic syndrome 2014. Clin Exp Nephrol. 2016;20:342–70.
Taniguchi M, Sawano S, Kugo M, et al. Physical activity promotes gait improvement in patients with total knee arthroplasty. J Arthroplast. 2016;31:984–8.
Caspo R, Alegre LM. Effects of resistance training with moderate vs heavy load on muscle mass and strength in the elderly: a meta-analysis. Scand J Med Sci Sports. 2016;26:995–1006.
Hayashi H, Iwai K, Tobita R, et al. The relationship between skeletal muscle and ventilator response to exercise in myocardial infarction. IJC Metab Endocr. 2016;12:14–8.
Fukuhara S, Suzukamo Y. Munual of SF-36 v2 Japanese version. Kyoto: Institute for Health Outcomes & Process Evaluation Research; 2004. pp. 55–138.
Iwai K, Hatanaka Y. A pilot study to relationship between urinary protein excretion and muscle strengthening in patients with acute onset renal disease. Phys Ther Res. 2018;21:59–64.
Troyanov S, Wall CA, Miller JA, et al. Idiopathic membranous nephropathy: definition and relevance of a partial remission. Kidney Int. 2004;66:1199–205.
Kawakami S, Yasuno T, Matsuda T, et al. Association between exercise intensity and renal blood flow evaluated using ultrasound echo. Clin Exp Nephrol. 2018;22:1061–8.
Miura H, Fukui H, Hayano K, et al. A case of minimal change nephrotic syndrome associated with acute renal failure after excessive exercise. Nippon Jinzo Gakkai Shi. 1993;35:387–91.
Mahmoodi BK, ten Kate MK, Waanders F, et al. High absolute risks and predictors of venous and arterial thromboembolic events in patients with nephrotic syndrome: results from a large retrospective cohort study. Circulation. 2008;117:224–30.
Smith DE, Hyneck ML, Berardi RR, et al. Urinary protein binding, kinetics, and dynamics of furosemide in nephrotic patients. J Pharm Sci. 1985;74:603–7.
Sugiyama H, Yokoyama H, Sato H, et al. Japan Renal Biopsy Registry: the first nationwide, web-based, and prospective registry system of renal biopsies in Japan. Clin Exp Nephrol. 2011;15:493–503.
Ji L: Disability prevention of renal failure: effects of exercise and enalapril in nephrotic rats. In: Proceedings of the 2nd world congress of the international society of physical and rehabilitation Medicine. 2003. p. 525–528.
Acknowledgements
The authors acknowledge Professor Toru Yamakado in Suzuka University of Medical Science and thank the people who participated in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest to declare in connection with this paper. The study protocol conformed to the ethical guidelines of the 1975 Declaration of Helsinki as reflected in a priori approval by the clinical research ethical committee of Hospital of Shiga University of Medical Science (approval number: 27-187), and informed consent was obtained from all patients enrolled.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Iwai, K., Hatanaka, Y., kawaguchi, T. et al. Evaluation of the safety, effectiveness, and health-related QOL impact of early rehabilitation in patients with nephrotic syndrome. Clin Exp Nephrol 23, 606–612 (2019). https://doi.org/10.1007/s10157-018-1681-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-018-1681-0