Abstract
Background
The purpose of this study was to conduct a meta-analysis examining the efficacy of cyclophosphamide, cyclosporin, and tacrolimus in treating steroid resistant nephrotic syndrome.
Methods
Medline, Cochrane, EMBASE, and Google Scholar were searched until May 02, 2017 using the keywords: immunosuppressive therapy, steroid-resistant nephrotic syndrome, cyclophosphamide, cyclosporine A, and tacrolimus. Inclusion criteria were randomized controlled trials (RCTs) including patients with SRNS treated with an immunosuppressive therapy or placebo.
Results
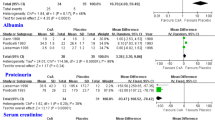
Seven RCTs were included, and the number of patients ranged from 30 to 131. Conventional pair-wise meta-analysis indicated a higher odds of complete or partial remission with tacrolimus as compared to cyclophosphamide [odds ratio (OR) 4.908, 95% confidence interval (CI) 2.278–10.576, P < 0.001], and cyclophosphamide (OR 0.143, 95% CI 0.028–0.721, P = 0.019) and placebo (OR 0.043, 95% CI 0.012–0.157, P < 0.001) were associated with a lower likelihood of complete or partial remission than cyclosporine. Bayesian analysis indicated that tacrolimus and cyclosporine were the best and the second-best agents for inducing a complete or partial remission (rank probability = 0.53 for tacrolimus and 0.46 for cyclosporine).
Conclusion
As compared to cyclophosphamide and cyclosporin, tacrolimus is more effective at inducing remission in patients with SRNS.



Similar content being viewed by others
References
El Bakkali L, Rodrigues Pereira R, Kuik DJ, Ket JC, van Wijk JA. Nephrotic syndrome in the Netherlands: a population-based cohort study and a review of the literature. Pediatr Nephrol. 2011;26:1241–6.
McKinney PA, Feltbower RG, Brocklebank JT, Fitzpatrick MM. Time trends and ethnic patterns of childhood nephrotic syndrome in Yorkshire, UK. Pediatr Nephrol. 2001;16:1040–4.
Kidney Disease: Improving Global Outcomes (KDIGO) Glomerulonephritis Work Group. KDIGO clinical practice guideline for glomerulonephritis. Kidney Int Suppl. 2012;2:139–274.
Aizawa-Yashiro T, Tsuruga K, Watanabe S, Oki E, Ito E, Tanaka H. Novel multidrug therapy for children with cyclosporine-resistant or -intolerant nephrotic syndrome. Pediatr Nephrol. 2011;6:1255–61.
Lombel RM, Hodson EM, Gipson DS. Improving Global Outcomes. Treatment of steroid-resistant nephrotic syndrome in children: new guidelines from KDIGO. Pediatr Nephrol. 2013;28:409–14.
Chapter 4: Steroid-resistant nephrotic syndrome in children. Kidney Int Suppl (2011). 2012; 2:172–6.
Lieberman KV, Tejani A. A randomized double-blind placebo-controlled trial of cyclosporine in steroid-resistant idiopathic focal segmental glomerulosclerosis in children. J Am Soc Nephrol. 1996;7:56–63.
Plank C, Kalb V, Hinkes B, Hildebrandt F, Gefeller O, Rascher W. Cyclosporin A is superior to cyclophosphamide in children with steroid-resistant nephrotic syndrome—a randomized controlled multicentre trial by the Arbeitsgemeinschaft für Pädiatrische Nephrologie. Pediatr Nephrol. 2008;23(9):1483–93.
Cattran DC, Appel GB, Hebert LA, Hunsicker LG, Pohl MA, Hoy WE, Maxwell DR, Kunis CL. A randomized trial of cyclosporine in patients with steroid-resistant focal segmental glomerulosclerosis. North America Nephrotic Syndrome Study Group. Kidney Int. 1999;56:2220–6.
Choudhry S, Bagga A, Hari P, Sharma S, Kalaivani M, Dinda A. Efficacy and safety of tacrolimus versus cyclosporine in children with steroid-resistant nephrotic syndrome: a randomized controlled trial. Am J Kidney Dis. 2009;53:760–9.
Tarshish P, Tobin JN, Bernstein J, Edelmann CM Jr. Cyclophosphamide does not benefit patients with focal segmental glomerulosclerosis. A report of the International Study of Kidney Disease in Children. Pediatr Nephrol. 1996;10:590–3.
Gulati A, Sinha A, Gupta A, Kanitkar M, Sreenivas V, Sharma J, Mantan M, Agarwal I, Dinda AK, Hari P, Bagga A. Treatment with tacrolimus and prednisolone is preferable to intravenous cyclophosphamide as the initial therapy for children with steroid-resistant nephrotic syndrome. Kidney Int. 2012;82:1130–5.
Shah SR, Altaf A, Arshad MH, Mari A, Noorani S, Saeed E, Mevawalla AA, Haq ZU, Faquih ME. Use of cyclosporine therapy in steroid resistant nephrotic syndrome (SRNS): a review. Glob J Health Sci. 2015;8(4):49961. doi:10.5539/gjhs.v8n4p136.
Coban M, Eke RN, Kizilates F, Ucar S, Dede F. Effect of steroid and cyclosporine in membranous nephropathy that is resistant to steroid and/or cytotoxic treatment. Int J Clin Exp Med. 2014;7:255–61.
Kim J, Patnaik N, Chorny N, Frank R, Infante L, Sethna C. Second-line immunosuppressive treatment of childhood nephrotic syndrome: a single-center experience. Nephron Extra. 2014;4:8–17.
Hodson EM, Willis NS, Craig JC. Interventions for idiopathic steroid-resistant nephrotic syndrome in children. Cochrane Database Syst Rev. 2010;(11):CD003594. doi:10.1002/14651858.CD003594.pub4
Colquitt JL, Kirby J, Green C, Cooper K, Trompeter RS. The clinical effectiveness and cost-effectiveness of treatments for children with idiopathic steroid-resistant nephrotic syndrome: a systematic review. Health Technol Assess. 2007;11:1–93 (iii–iv, ix–xi).
Beins NT, Dell KM. Long-term outcomes in children with steroid-resistant nephrotic syndrome treated with calcineurin inhibitors. Front Pediatr. 2015;3:104. doi:10.3389/fped.2015.00104.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151:W65–94.
Higgins JPT, Green S, eds. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration; 2011. http://www.cochrane-handbook.org. Updated Mar 2011.
Brooks SP, Gelman A. General methods for monitoring convergence of iterative simulations. J Comput Graph Stat. 1998;7:434–55.
Lu G, Ades AE. Assessing evidence inconsistency in mixed treatment comparisons. J Am Stat Assoc. 2006;101:447–59.
Dias S, Welton NJ, Caldwell DM, Ades AE. Checking consistency in mixed treatment comparison meta-analysis. Stat Med. 2010;29:932–44.
van Valkenhoef G, Tervonen T, Zwinkels T, Brock BD, Hillege H. ADDIS: a decision support system for evidence-based medicine. Decis Support Syst. 2013;55:459–75.
Davin JC. The glomerular permeability factors in idiopathic nephrotic syndrome. Pediatr Nephrol. 2016;31:207–15.
Zagury A, Oliveira AL, Montalvão JA, Novaes RH, Sá VM, Moraes CA, Tavares Mde S. Steroid-resistant idiopathic nephrotic syndrome in children: long-term follow-up and risk factors for end-stage renal disease. J Bras Nefrol. 2013;35:191–9 [Article in English, Portuguese].
Hino S, Takemura T, Okada M, Murakami K, Yagi K, Fukushima K, Yoshioka K. Follow-up study of children with nephrotic syndrome treated with a long-term moderate dose of cyclosporine. Am J Kidney Dis. 1998;31:932–3.
Hamasaki Y, Yoshikawa N, Hattori S, Sasaki S, Iijima K, Nakanishi K, Matsuyama T, Ishikura K, Yata N, Kaneko T, Honda M. Cyclosporine and steroid therapy in children with steroid-resistant nephrotic syndrome. Pediatr Nephrol. 2009;24:2177–85.
Dötsch J, Dittrich K, Plank C, Rascher W. Is tacrolimus for childhood steroid-dependent nephrotic syndrome better than cyclosporin A? Nephrol Dial Transplant. 2006;21:173–6.
Sinha MD, MacLeod R, Rigby E, Clark AG. Treatment of severe steroid-dependent nephrotic syndrome (SDNS) in children with tacrolimus. Nephrol Dial Transplant. 2006;21:1848–54.
Echeverri CV, Valencia GA, Higuita LM, Gayubo AK, Ochoa CL, Rosas LF, Muñoz LC, Sierra J, Zuleta JJ, Ruiz JJ. Immunosupressive therapy in children with steroid-resistant nephrotic syndrome: single center experience. J Bras Nefrol. 2013;35(3):200–5 [Article in English, Portuguese].
Wu B, Mao J, Shen H, Fu H, Wang J, Liu A, Gu W, Shu Q, Du L. Triple immunosuppressive therapy in steroid-resistant nephrotic syndrome children with tacrolimus resistance or tacrolimus sensitivity but frequently relapsing. Nephrology (Carlton). 2015;20(1):18–24.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors have declared that no conflict of interest exists.
Funding source
Zhejiang Provincial Natural Science Fund LY17H050008, Zhejiang Provincial Medical Science and Technology Plan Projects 2017KY227.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Jiang, X., Shen, W., Xu, X. et al. Immunosuppressive therapy for steroid-resistant nephrotic syndrome: a Bayesian network meta-analysis of randomized controlled studies. Clin Exp Nephrol 22, 562–569 (2018). https://doi.org/10.1007/s10157-017-1484-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-017-1484-8