Abstract
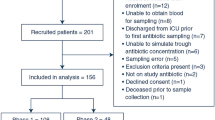
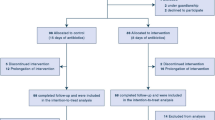
Diagnostic uncertainty is common in the emergency room and multidrug-resistant bacteria emerge in the community setting, implying to establish the most efficient empirical antibiotic therapy (eEAT). Our aim was to identify such eEAT, considering that in case of DU with severe clinical presentation, most prescribers would propose an empiric combination (EC). The medical dashboard of our ward records prospectively 28 characteristics of each hospitalization including hospitalization motive, final diagnosis, and all antibiotics prescribed. All patients with community-acquired bacteremia (CAB) were included. DU was defined by a discrepancy between suspected diagnosis in the emergency room and final diagnosis. eEAT was defined by in vitro activity of at least one prescribed compound. Finally, independently from the dashboard, we retrospectively compared 2 CTs: amoxicillin/clavulanic acid (AMC)+gentamicin (G) and cefotaxime (3GC)+G. One thousand thirty-four patients with a final diagnosis of CAB were identified from July 2005 to June 2018, including 357 DU (35%) at baseline. eEAT (n = 553) was associated with a trend towards a lower death rate compared to inefficient therapies: 5.4 vs 10.0% (p = 0.053), and effective antibiotic reassessment was the most protective factor against an unfavorable outcome: 0.34 (0.16–0.71). Bacteria involved in case of UD were resistant to AMC+G and to 3GC+G in 8.1% and 12.8% of patients, respectively. Diagnostic uncertainty was a frequent event requiring antibiotic reassessment. As the latter was not systematically realized, the best eEAT is required and AMC+aminoglycoside should be considered.

Similar content being viewed by others
Abbreviations
- AMC:
-
amoxicilline-clavulanic acid
- 3GC:
-
cefotaxime
- EC:
-
empiric combination
- CAB:
-
community acquired bacteremia
- DRG:
-
diagnosis-related group
- DU:
-
diagnostic uncertainty
- eEAT:
-
efficient empirical antibiotic therapy
- G 3GC:
-
gentamicin cefotaxime
- MDR:
-
multidrug-resistant
References
Aillet C, Jammes D, Fribourg A, Léotard S, Pellat O, Etienne P, et al (2018) Bacteraemia in emergency departments: effective antibiotic reassessment is associated with a better outcome. Eur J Clin Microbiol Infect Dis 37:325–31. https://doi.org/10.1007/s10096-017-3136-z
Roger P-M, Demonchy E, Risso K, Courjon J, Leroux S, Leroux E, et al (2017) Medical table: A major tool for antimicrobial stewardship policy. Med Mal Infect 47:311–8. https://doi.org/10.1016/j.medmal.2017.03.005
Denis E, Martis N, Guillouet-de-Salvador F (2016) Bacteraemic urinary tract infections may mimic respiratory infections: a nested case-control study. Eur J Clin Microbiol Infect Dis 1601–1605
Gavazzi G, Krause K-H (2002) Ageing and infection. Lancet Infect Dis 2:659–666
Filice AG, Drekonja DM, Thurn H JR, GM M, T J JR (2015) Diagnostic errors that lead to inappropriate antimicrobial use. Infect Control Hosp Epidemiol 949–956
Roca I, Akova M, Baquero F, Carlet J, Cavaleri M, Coenen S, et al (2015) The global threat of antimicrobial resistance: science for intervention. New Microbes New Infect 6:22–9. https://doi.org/10.1016/j.nmni.2015.02.007
Sartelli M, Malangoni MA, May AK, Viale P, Kao LS, Catena F, et al (2014) World Society of Emergency Surgery (WSES) guidelines for management of skin and soft tissue infections. World J Emerg Surg 9:57. https://doi.org/10.1186/1749-7922-9-57
Barlam TF, Cosgrove SE, Abbo LM, MacDougall C, Schuetz AN, Septimus EJ, et al (2016) Implementing an Antibiotic Stewardship Program: Guidelines by the Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America. Clin Infect Dis 62:e51-77. https://doi.org/10.1093/cid/ciw118
Zahar J-R, Lesprit P, Ruckly S, Eden A, Hikombo H, Bernard L, et al (2017) Predominance of healthcareassociated cases among episodes of community-onset bacteraemia due to extended-spectrum ß-lactamase-producing Enterobacteriaceae. Int J Antimicrob Agents 49:67–73. https://doi.org/10.1016/j.ijantimicag.2016.09.032
Rogers BA, Sidjabat HE, Paterson DL (2011) Escherichia coli O25b-ST131: a pandemic, multiresistant, community-associated strain. J Antimicrob Chemother 66:1–14. https://doi.org/10.1093/jac/dkq415
Vazquez-Grande G, Kumar A (2015) Optimizing antimicrobial therapy of sepsis and septic shock: focus on antibiotic combination therapy. Semin Respir Crit Care Med 36:154–66. https://doi.org/10.1055/s-0034-1398742
Vallés J, Rello J, Ochagavía A, Garnacho J, Alcalá MA (2003) Community-acquired bloodstream infection in critically ill adult patients: impact of shock and inappropriate antibiotic therapy on survival. Chest 123:1615–24
Marchaim D, Zaidenstein R, Lazarovitch T, Karpuch Y, Ziv T, Weinsberger M (2008) Epidemiology of bacteremia episodes in a single center: increase in gram-negative isolates, antibiotics resistance and patient age. Eur J Mircobiol Infect Dis 27(11):1045–51. https://doi.org/10.1007/s10096-008-0545-z
Spivak ES, Cosgrove SE, Srinivasan A (2016) Measuring Appropriate Antimicrobial Use: Attempts at Opening the Black Box. Clin Infect Dis 63:1639–44. https://doi.org/10.1093/cid/ciw658
Braykov N, Morgan DJ, Schweizer. ML et al (2014) Assessment of empirical therapy in six hospitals: an observational cohort study. Lancet Infect Dis 1220–7
Shallcross LJ, Freemantle N, Nisar S, Ray D (2016) A cross-sectional study of blood cultures and antibiotic use in patients admitted from the Emergency Department: missed opportunities for antimicrobial stewardship BMC Infect Dis 16:166. https://doi.org/10.1186/s12879-016-1515-1
Winokur PL, Canton R. Casellas JM, Legakis N. (2001) Variations in the prevalence of strains expressing an extended-spectrum beta-lactamase phenotype and characterization of isolates from Europe, the Americas, and the Western Pacific region. Clin Infect Dis 32(Suppl 2):s94–103
Russo A, Falcone M, Gutiérrez-Gutiérrez B, Calbo E, Almirante B, Viale PL, et al (2018) Predictors of outcome in patients with severe sepsis or septic shock due to extended-spectrum ß-lactamase-producing Enterobacteriaceae. Int J Antimicrob Agents 52:577–85. https://doi.org/10.1016/j.ijantimicag.2018.06.018
Lefort A, Panhard X, Clermont O, Woerther P-L, Branger C, Mentré F, et al (2011) Host factors and portal of entry outweigh bacterial determinants to predict the severity of Escherichia coli bacteremia. J Clin Microbiol 49:777–783. https://doi.org/10.1128/JCM.01902-10
Courjon J, Demonchy E, Degand N, Risso K, Ruimy R, Roger P-M (2017) Patients with community-acquired bacteremia of unknown origin: clinical characteristics and usefulness of microbiological results for therapeutic issues: a single-center cohort study. Ann Clin Microbiol Antimicrob 16:40. https://doi.org/10.1186/s12941-017-0214-0
Availability of data
The dataset used during the current study is available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Contributions
Study concept and design, PMR; acquisition of subjects, JC, ED, DC, CM, ND; analysis and interpretation of data, JC, PMR; preparation of manuscript, JC, ND, PMR.
Corresponding author
Ethics declarations
Conflict of interest
All of the authors declare that they have no conflicts of interest.
Ethical approval and consent to participate
The antibiotic audit was sponsored by the French National Health Agency. The patients or their relatives provided written consent for computerization of their personal data for hospitalization purposes and clinical research.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Courjon, J., Chirio, D., Demonchy, E. et al. Amoxicillin/clavulanic acid+aminoglycoside as empirical antibiotic treatment in severe community-acquired infections with diagnostic uncertainty. Eur J Clin Microbiol Infect Dis 38, 895–901 (2019). https://doi.org/10.1007/s10096-019-03496-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-019-03496-0