Abstract
Background
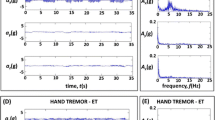
The current gold standard for evaluating normal and impaired motor performances includes the use of the information provided by the patient and the Unified Parkinson’s Disease Rating Scale (UPDRS). However, clinical rating scales are typically subjective and their time-limited duration may fail to capture daily fluctuations in motor symptoms resulting from Parkinson’s disease. Recently, a new tool has been proposed for objective and continuous assessment of movement disorders based on the evaluation of frequential data content from multi-axial sensors and the identification of specific movement patterns typically associated with disorders. This reduces the probability of confusing physiological or pathological movements occurring at the same frequency with a different movement pattern. However, the data provided by the tool have not yet been compared with the information provided by the typically used clinical rating scales.
Objectives
The aim of this work is to investigate the possible relationship between UPRDS scores and the information provided by the tool for continuous and long-term monitoring.
Materials and methods
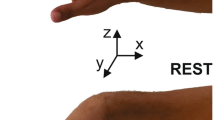
In this study, 20 patients with hand tremor were recruited. The UPDRS scoring was performed by a neurologist. Then, continuous monitoring was performed; data were acquired by means of the proposed wrist-worn-device “PD-Watch” for 24 h and then processed in order to get information and indexes on motor symptoms. Finally, these indexes were correlated to the UPDRS scores.
Results
Results show that the concise indexes provided by the tool correlate well with some items in UPDRS Part III, and this correlation has allowed to provide a more direct and immediate meaning to the values of the concise indexes detected by the tool.
Conclusions
While results need to be extended with further studies, this can be considered useful information in the context of clinical trials and routine clinical practice for assessing motor symptoms and movement disorders.



Similar content being viewed by others
References
Pringsheim T, Jette N, Frolkis A, Steeves TD (2014) The prevalence of Parkinson’s disease: a systematic review and meta-analysis. Mov Disord 29:1583–1590
Guttman M, Kish SJ, Furukawa Y (2003) Current concepts in the diagnosis and management of Parkinson’s disease. Canadian Med Ass J 168:293–301
Janckovic J (2008) Parkinson’s disease: clinical features and diagnosis. J Neurol Neurosurg Psychiatry 79:368–376
Fox SH, Katzenschlager R, Lim SY, Barton B, de Bie RMA, Seppi K, Coelho M, Sampaio C (2018) International Parkinson and movement disorder society evidence-based medicine review: update on treatments for the motor symptoms of Parkinson’s disease. Mov Disord 3:1248–1266
Dunnewold RJ, Jacobi CE, van Hilten JJ (1997) Quantitative assessment of bradykinesia in patients with Parkinson’s disease. J Neurosci Methods 74:107–112
de Lau LML, Breteler MMB (2006) Epidemiology of Parkinson’s disease. Lancet Neurol 5:525–535
Movement Disorder Society Task Force on Rating Scales for Parkinson’s Disease (2003) The Unified Parkinson’s disease rating scale (UPDRS): status and recommendations. Mov Disord 18:738–750
Goetz CG, Tilley BC, Shaftman SR, Stebbins GT, Fahn S, Martinez-Martin P, Poewe W, Sampaio C, Stern MB, Dodel R, Dubois B, Holloway R, Jankovic J, Kulisevsky J, Lang AE, Lees A, Leurgans S, LeWitt PA, Nyenhuis D, Olanow CW, Rascol O, Schrag A, Teresi JA, van Hilten JJ, LaPelle N (2008) Movement Disorder Society-Sponsored Revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS): Scale Presentation and Clinimetric Testing Results. Mov Disord 23:2129–2170
Barroso Júnior MC, Esteves GP, Nunes TP, Silva LM, Faria ACD, Melo PL (2011) A telemedicine instrument for remote evaluation of tremor: design and initial applications in fatigue and patients with Parkinson’s disease. Biomed Eng Online 10:1–14
Brown RG, MacCarthy B, Jahanshahi M, Marsden CD (1989) Accuracy of self-reported disability in patients with Parkinsonism. Arch Neurol 46:955–959
Waerling RD, Kjaer TW (2020) A systematic review of impairment focussed technology in neurology. Disability and Rehabilitation: Assistive Technology:1–14. https://doi.org/10.1080/17483107.2020.1776776
Ferreira-Sánchez MDR, Moreno-Verdú M, Cano-de-la-Cuerda R (2020) Quantitative measurement of rigidity in Parkinson’s disease: a systematic review. Sensors 20:880
Cai G, Huang Y, Luo S, Lin Z, Dai H, Ye Q (2017) Continuous quantitative monitoring of physical activity in Parkinson’s disease patients by using wearable devices: a case-control study. Neurol Sci 38:1657–1663
Espay AJ, Bonato P, Nahab FB, Maetzler W, Dean JM, Klucken J, Eskofier BM, Merola A, Horak F, Lang AE, Reilmann R, Giuffrida J, Nieuwboer A, Horne M, Little MA, Litvan I, Simuni T, Dorsey ER, Burack MA, Kubota K, Kamondi A, Godinho C, Daneault J, Mitsi G, Krinke L, Hausdorff JM, Bloem BR, Papapetropoulos S (2016) Technology in Parkinson disease: challenges and opportunities. Mov Disord 31:1272–1282
Godinho C, Domingos J, Cunha G, Santos AT (2016) A systematic review of the characteristics and validity of monitoring technologies to assess Parkinson’s disease. J NeuroEng Rehab 13:1–10
Bhatia KP, Bain P, Bajaj N, Elble RJ, Hallett M, Louis ED, Raethjen J, Stamelou M, Testa CM, Deuschl G (2018) Consensus Statement on the classification of tremors. From the Task Force on Tremor of the International Parkinson and Movement Disorder Society organize a program to provide the Movement Disorder. Mov Disord 33:75–87
Mathie MJ, Coster AC, Lovell NH, Celler BG (2004) Accelerometry providing an integrated practical method for long-term ambulatory monitoring of human movement. Physiol Meas 25:R1–R20
Battista L, Romaniello A (2018) A novel device for continuous monitoring of tremor and other motor symptoms. Neurol Sci 39:1333–1343
Battista L, Casali M, Coletti C, Grassini P, Radicati FG, Stocchi F (2020) A preliminary investigation on the accuracy of the wearable systems for continuous monitoring of movement disorders. Proceedings of the 6th Conference of Italian Academy on movement disorders. P6. Available at https://www.accademialimpedismov.it/web/image/51617/AbstractCongressoVirtualeAccademiaLIMPE_DISMOV_2020.pdf
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research involving human participants and/or animals
Yes, human participants. The study protocol was approved by the Ethics Committee of Basilicata, Italy.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
Eng. Luigi Battista holds intellectual property rights for a wearable system for Parkinson’s disease. Dr. Antonietta Romaniello has nothing to disclose.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Battista, L., Romaniello, A. A wearable tool for continuous monitoring of movement disorders: clinical assessment and comparison with tremor scores. Neurol Sci 42, 4241–4248 (2021). https://doi.org/10.1007/s10072-021-05120-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05120-6