Abstract
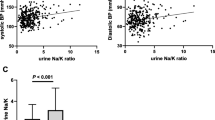
Hypertension is highly prevalent in patients with rheumatoid arthritis (RA). In other populations, high sodium (Na+) and low potassium (K+) intake are associated with an increased risk of hypertension, and in animal models, a high salt intake exacerbated arthritis. Patients with RA have many comorbidities associated with salt sensitivity, but their salt intake and its relationship to blood pressure and inflammation is unknown. Using the Kawasaki formula, Na+ and K+ urinary excretion (reflecting intake) was estimated in 166 patients with RA and 92 controls, frequency matched for age, sex, and race. Inflammatory markers and disease activity were measured in RA patients. We tested the associations between blood pressure and Na+ and K+ excretion. Estimated 24-h Na+ excretion was similarly high in both RA (median [IQR] 5.1 g, [3.9–6.6 g]) and controls (4.9 g, [4.0–6.5 g]), p = 0.9, despite higher rates of hypertension in RA (54 vs. 39%, p = 0.03). The Na+:K+ excretion ratio was significantly higher in RA (2.0 [1.6–2.4]) vs. 1.7 [1.5–2.1]), p = 0.02] compared to controls. In RA, a lower K+ excretion was inversely correlated with diastolic blood pressure (adjusted β = − 1.79, p = 0.04). There was no significant association between Na+ or K+ excretion and inflammatory markers. Despite a similar Na+ excretion, patients with RA had higher rates of hypertension than controls, a finding compatible with increased salt sensitivity. Patients with RA had a lower Na+:K+ excretion ratio than controls, and lower K+ excretion was associated with higher diastolic blood pressure in RA.
Similar content being viewed by others
References
Panoulas VF, Metsios GS, Pace AV, John H, Treharne GJ, Banks MJ, Kitas GD (2008) Hypertension in rheumatoid arthritis. Rheumatology 47(9):1286–1298. https://doi.org/10.1093/rheumatology/ken159
Assous N, Touze E, Meune C, Kahan A, Allanore Y (2007) Cardiovascular disease in rheumatoid arthritis: single-center hospital-based cohort study in France. Joint Bone Spine 74(1):66–72. https://doi.org/10.1016/j.jbspin.2006.10.001
Schuett KA, Lehrke M, Marx N, Burgmaier M (2015) High-risk cardiovascular patients: clinical features, comorbidities, and interconnecting mechanisms. Front Immunol 6:591. https://doi.org/10.3389/fimmu.2015.00591
Wallberg-Jonsson S, Ohman ML, Dahlqvist SR (1997) Cardiovascular morbidity and mortality in patients with seropositive rheumatoid arthritis in Northern Sweden. J Rheumatol 24(3):445–451
Manavathongchai S, Bian A, Rho YH, Oeser A, Solus JF, Gebretsadik T, Shintani A, Stein CM (2013) Inflammation and hypertension in rheumatoid arthritis. J Rheumatol 40(11):1806–1811. https://doi.org/10.3899/jrheum.130394
Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER 3rd, Simons-Morton DG, Karanja N, Lin PH, Group DA-SCR (2001) Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med 344(1):3–10. https://doi.org/10.1056/NEJM200101043440101
Cook NR, Obarzanek E, Cutler JA, Buring JE, Rexrode KM, Kumanyika SK, Appel LJ, Whelton PK, Trials of Hypertension Prevention Collaborative Research G (2009) Joint effects of sodium and potassium intake on subsequent cardiovascular disease: the Trials of Hypertension Prevention follow-up study. Arch Intern Med 169(1):32–40. https://doi.org/10.1001/archinternmed.2008.523
Yang Q, Liu T, Kuklina EV, Flanders WD, Hong Y, Gillespie C, Chang MH, Gwinn M, Dowling N, Khoury MJ, FB H (2011) Sodium and potassium intake and mortality among US adults: prospective data from the Third National Health and Nutrition Examination Survey. Arch Intern Med 171(13):1183–1191. https://doi.org/10.1001/archinternmed.2011.257
Chang HY, YW H, Yue CS, Wen YW, Yeh WT, Hsu LS, Tsai SY, Pan WH (2006) Effect of potassium-enriched salt on cardiovascular mortality and medical expenses of elderly men. Am J Clin Nutr 83(6):1289–1296
KB DS (2016) Public Health 3.0: applying the 2015-2020 dietary guidelines for Americans. Public Health Rep 131(4):518–521
Mozaffarian D, Fahimi S, Singh GM, Micha R, Khatibzadeh S, Engell RE, Lim S, Danaei G, Ezzati M, Powles J, Global Burden of Diseases N, Chronic Diseases Expert G (2014) Global sodium consumption and death from cardiovascular causes. N Engl J Med 371 (7):624–634. https://doi.org/10.1056/NEJMoa1304127
Cook NR, Cutler JA, Obarzanek E, Buring JE, Rexrode KM, Kumanyika SK, Appel LJ, Whelton PK (2007) Long term effects of dietary sodium reduction on cardiovascular disease outcomes: observational follow-up of the trials of hypertension prevention (TOHP). BMJ 334(7599):885–888. https://doi.org/10.1136/bmj.39147.604896.55
Mente A, O'Donnell MJ, Rangarajan S, McQueen MJ, Poirier P, Wielgosz A, Morrison H, Li W, Wang X, Di C, Mony P, Devanath A, Rosengren A, Oguz A, Zatonska K, Yusufali AH, Lopez-Jaramillo P, Avezum A, Ismail N, Lanas F, Puoane T, Diaz R, Kelishadi R, Iqbal R, Yusuf R, Chifamba J, Khatib R, Teo K, Yusuf S, Investigators P (2014) Association of urinary sodium and potassium excretion with blood pressure. N Engl J Med 371(7):601–611. https://doi.org/10.1056/NEJMoa1311989
Chung CP, Oeser A, Solus JF, Avalos I, Gebretsadik T, Shintani A, Raggi P, Sokka T, Pincus T, Stein CM (2008) Prevalence of the metabolic syndrome is increased in rheumatoid arthritis and is associated with coronary atherosclerosis. Atherosclerosis 196(2):756–763. https://doi.org/10.1016/j.atherosclerosis.2007.01.004
Avalos I, Chung CP, Oeser A, Gebretsadik T, Shintani A, Kurnik D, Raggi P, Sokka T, Pincus T, Stein CM (2007) Increased augmentation index in rheumatoid arthritis and its relationship to coronary artery atherosclerosis. J Rheumatol 34(12):2388–2394
Chung CP, Oeser A, Solus JF, Gebretsadik T, Shintani A, Avalos I, Sokka T, Raggi P, Pincus T, Stein CM (2008) Inflammation-associated insulin resistance: differential effects in rheumatoid arthritis and systemic lupus erythematosus define potential mechanisms. Arthritis Rheum 58(7):2105–2112. https://doi.org/10.1002/art.23600
Ormseth MJ, Lipson A, Alexopoulos N, Hartlage GR, Oeser AM, Bian A, Gebretsadik T, Shintani A, Raggi P, Stein CM (2013) Association of epicardial adipose tissue with cardiometabolic risk and metabolic syndrome in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken) 65(9):1410–1415. https://doi.org/10.1002/acr.22027
Khan F, Galarraga B, Belch JJ (2010) The role of endothelial function and its assessment in rheumatoid arthritis. Nat Rev Rheumatol 6(5):253–261. https://doi.org/10.1038/nrrheum.2010.44
Becetti K, Oeser A, Ormseth MJ, Solus JF, Raggi P, Stein CM, Chung CP (2015) Urinary albumin excretion is increased in patients with rheumatoid arthritis and associated with arterial stiffness. J Rheumatol 42(4):593–598. https://doi.org/10.3899/jrheum.141295
Kleinewietfeld M, Manzel A, Titze J, Kvakan H, Yosef N, Linker RA, Muller DN, Hafler DA (2013) Sodium chloride drives autoimmune disease by the induction of pathogenic TH17 cells. Nature 496(7446):518–522. https://doi.org/10.1038/nature11868
Wu C, Yosef N, Thalhamer T, Zhu C, Xiao S, Kishi Y, Regev A, Kuchroo VK (2013) Induction of pathogenic TH17 cells by inducible salt-sensing kinase SGK1. Nature 496(7446):513–517. https://doi.org/10.1038/nature11984
Sehnert B, Pohle S, Schroder A, Titze J, Voll RE (2014) A low salt diet ameliorates clinical manifestations in collagen-induced arthritis. Arthritis & Rheumatology 66:S145–S145
Chung CP, Oeser A, Raggi P, Gebretsadik T, Shintani AK, Sokka T, Pincus T, Avalos I, Stein CM (2005) Increased coronary-artery atherosclerosis in rheumatoid arthritis: relationship to disease duration and cardiovascular risk factors. Arthritis Rheum 52(10):3045–3053. https://doi.org/10.1002/art.21288
Chung CP, Oeser A, Raggi P, Sokka T, Pincus T, Solus JF, Linton MF, Fazio S, Stein CM (2010) Lipoprotein subclasses determined by nuclear magnetic resonance spectroscopy and coronary atherosclerosis in patients with rheumatoid arthritis. J Rheumatol 37(8):1633–1638. https://doi.org/10.3899/jrheum.090639
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS, Healey LA, Kaplan SR, Liang MH, Luthra HS et al (1988) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31(3):315–324. https://doi.org/10.1002/art.1780310302
Reilly MP, Wolfe ML, Rhodes T, Girman C, Mehta N, Rader DJ (2004) Measures of insulin resistance add incremental value to the clinical diagnosis of metabolic syndrome in association with coronary atherosclerosis. Circulation 110(7):803–809. https://doi.org/10.1161/01.CIR.0000138740.84883.9C
Kawasaki T, Itoh K, Uezono K, Sasaki H (1993) A simple method for estimating 24 h urinary sodium and potassium excretion from second morning voiding urine specimen in adults. Clin Exp Pharmacol Physiol 20(1):7–14. https://doi.org/10.1111/j.1440-1681.1993.tb01496.x
Kawamura M, Kusano Y, Takahashi T, Owada M, Sugawara T (2006) Effectiveness of a spot urine method in evaluating daily salt intake in hypertensive patients taking oral antihypertensive drugs. Hypertens Res 29(6):397–402. https://doi.org/10.1291/hypres.29.397
Chung CP, Oeser A, Avalos I, Gebretsadik T, Shintani A, Raggi P, Sokka T, Pincus T, Stein CM (2006) Utility of the Framingham risk score to predict the presence of coronary atherosclerosis in patients with rheumatoid arthritis. Arthritis Res Ther 8(6):R186. https://doi.org/10.1186/ar2098
Jackson SL, King SM, Zhao L, Cogswell ME (2016) Prevalence of excess sodium intake in the United States—NHANES, 2009-2012. MMWR Morb Mortal Wkly Rep 64(52):1393–1397. https://doi.org/10.15585/mmwr.mm6452a1
Whelton PK, Appel LJ, Sacco RL, Anderson CA, Antman EM, Campbell N, Dunbar SB, Frohlich ED, Hall JE, Jessup M, Labarthe DR, MacGregor GA, Sacks FM, Stamler J, Vafiadis DK, Van Horn LV (2012) Sodium, blood pressure, and cardiovascular disease: further evidence supporting the American Heart Association sodium reduction recommendations. Circulation 126(24):2880–2889. https://doi.org/10.1161/CIR.0b013e318279acbf
Bibbins-Domingo K (2014) The institute of medicine report sodium intake in populations: assessment of evidence: summary of primary findings and implications for clinicians. JAMA Intern Med 174(1):136–137. https://doi.org/10.1001/jamainternmed.2013.11818
Panoulas VF, Douglas KM, Milionis HJ, Stavropoulos-Kalinglou A, Nightingale P, Kita MD, Tselios AL, Metsios GS, Elisaf MS, Kitas GD (2007) Prevalence and associations of hypertension and its control in patients with rheumatoid arthritis. Rheumatology (Oxford) 46(9):1477–1482. https://doi.org/10.1093/rheumatology/kem169
Weinberger MH, Miller JZ, Luft FC, Grim CE, Fineberg NS (1986) Definitions and characteristics of sodium sensitivity and blood-pressure resistance. Hypertension 8(6):127–134
Chen J, Gu D, Huang J, Rao DC, Jaquish CE, Hixson JE, Chen CS, Chen J, Lu F, Hu D, Rice T, Kelly TN, Hamm LL, Whelton PK, He J, GenSalt Collaborative Research G (2009) Metabolic syndrome and salt sensitivity of blood pressure in non-diabetic people in China: a dietary intervention study. Lancet 373(9666):829–835. https://doi.org/10.1016/S0140-6736(09)60144-6
Bragulat E, de la Sierra A, Antonio MT, Coca A (2001) Endothelial dysfunction in salt-sensitive essential hypertension. Hypertension 37(2 Pt 2):444–448. https://doi.org/10.1161/01.HYP.37.2.444
O'Donnell M, Mente A, Rangarajan S, McQueen MJ, Wang X, Liu L, Yan H, Lee SF, Mony P, Devanath A, Rosengren A, Lopez-Jaramillo P, Diaz R, Avezum A, Lanas F, Yusoff K, Iqbal R, Ilow R, Mohammadifard N, Gulec S, Yusufali AH, Kruger L, Yusuf R, Chifamba J, Kabali C, Dagenais G, Lear SA, Teo K, Yusuf S, Investigators P (2014) Urinary sodium and potassium excretion, mortality, and cardiovascular events. N Engl J Med 371(7):612–623. https://doi.org/10.1056/NEJMoa1311889
Lewington S, Clarke R, Qizilbash N, Peto R, Collins R, Prospective Studies C (2002) Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 360(9349):1903–1913
Hansen TW, Jeppesen J, Rasmussen S, Ibsen H, Torp-Pedersen C (2005) Ambulatory blood pressure and mortality: a population-based study. Hypertension 45(4):499–504. https://doi.org/10.1161/01.HYP.0000160402.39597.3b
van der Meer JW, Netea MG (2013) A salty taste to autoimmunity. N Engl J Med 368(26):2520–2521. https://doi.org/10.1056/NEJMcibr1303292
Sundstrom B, Johansson I, Rantapaa-Dahlqvist S (2015) Interaction between dietary sodium and smoking increases the risk for rheumatoid arthritis: results from a nested case-control study. Rheumatology (Oxford) 54(3):487–493. https://doi.org/10.1093/rheumatology/keu330
Salgado E, Bes-Rastrollo M, de Irala J, Carmona L, Gomez-Reino JJ (2015) High sodium intake is associated with self-reported rheumatoid arthritis: a cross sectional and case control analysis within the SUN cohort. Medicine (Baltimore) 94(37):e924. https://doi.org/10.1097/MD.0000000000000924
Financial support
Supported by grants from: Alpha Omicron Pi (Stein), Arthritis Foundation Clinical to Research Transition Award (Stein), P60-AR-056116 (Stein), K23AR064768 (Chung), Rheumatology Research Foundation K-supplement (Chung), T32 GM07569 (Stein), and CTSA awards No. UL1TR000445 and UL1RR024975 from the National Center for Advancing Translational Sciences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Its contents are solely the responsibility of the authors and do not necessarily represent official views of the National Institutes of Health. Informed consent was given by all patients and controls prior to data and sample collection. The study protocol was approved by the Vanderbilt University Medical Center’s institutional review board.
Disclosures
None.
Rights and permissions
About this article
Cite this article
Carranza-Leon, D., Octaria, R., Ormseth, M.J. et al. Association between urinary sodium and potassium excretion and blood pressure and inflammation in patients with rheumatoid arthritis. Clin Rheumatol 37, 895–900 (2018). https://doi.org/10.1007/s10067-017-3935-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-017-3935-8