Abstract
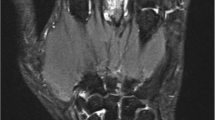
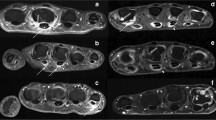
Contrast-enhanced magnetic resonance imaging with maximum intensity projection (MRI-MIP) is an easy, useful imaging method to evaluate synovitis in rheumatoid hands. However, the prognosis of synovitis-positive joints on MRI-MIP has not been clarified. The aim of this study was to evaluate the relationship between synovitis visualized by MRI-MIP and joint destruction on X-rays in rheumatoid hands. The wrists, metacarpophalangeal (MP) joints, and proximal interphalangeal (PIP) joints of both hands (500 joints in total) were evaluated in 25 rheumatoid arthritis (RA) patients. Synovitis was scored from grade 0 to 2 on the MRI-MIP images. The Sharp/van der Heijde score and Larsen grade were used for radiographic evaluation. The relationships between the MIP score and the progression of radiographic scores and between the MIP score and bone marrow edema on MRI were analyzed using the trend test. As the MIP score increased, the Sharp/van der Heijde score and Larsen grade progressed severely. The rate of bone marrow edema-positive joints also increased with higher MIP scores. MRI-MIP imaging of RA hands is a clinically useful method that allows semi-quantitative evaluation of synovitis with ease and can be used to predict joint destruction.


Similar content being viewed by others
References
Smolen JS, Landewé R, Breedveld FC et al (2014) EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2013 update. Ann Rheum Dis 73:492–509. doi:10.1136/annrheumdis-2013-204573
Kawashiri S, Suzuki T, Okada A et al (2013) Musculoskeletal ultrasonography assists the diagnostic performance of the 2010 classification criteria for rheumatoid arthritis. Mod Rheumatol 23:36–43. doi:10.1007/s10165-012-0628-7
Colebatch AN, Edwards CJ, Østergaard M et al (2013) EULAR recommendations for the use of imaging of the joints in the clinical management of rheumatoid arthritis. Ann Rheum Dis 72:804–814. doi:10.1136/annrheumdis-2012-203158
Nakagomi D, Ikeda K, Okubo A et al (2013) Ultrasound can improve the accuracy of the 2010 American College of Rheumatology/European League against rheumatism classification criteria for rheumatoid arthritis to predict the requirement for methotrexate treatment. Arthritis Rheum 65:890–898. doi:10.1002/art.37848
Østergaard M, Ejbjerg B, Szkudlarek M (2005) Imaging in early rheumatoid arthritis: roles of magnetic resonance imaging, ultrasonography, conventional radiography and computed tomography. Best Pract Res Clin Rheumatol 19:91–116. doi:10.1016/j.berh.2004.08.006
Ostergaard M, Ejbjerg B (2004) Magnetic resonance imaging of the synovium in rheumatoid arthritis. Semin Musculoskelet Radiol 8:287–299. doi:10.1055/s-2004-861576
Ostergaard M, Hansen M, Stoltenberg M et al (1999) Magnetic resonance imaging-determined synovial membrane volume as a marker of disease activity and a predictor of progressive joint destruction in the wrists of patients with rheumatoid arthritis. Arthritis Rheum 42:918–929. doi:10.1002/1529-0131(199905)42:5<918::AID-ANR10>3.0.CO;2-2
McQueen F, Lassere M, Edmonds J et al (2003) OMERACT Rheumatoid Arthritis Magnetic Resonance Imaging Studies. Summary of OMERACT 6 MR Imaging Module. J Rheumatol 30:1387–1392
Fishman EK, Ney DR, Heath DG et al (2006) Volume rendering versus maximum intensity projection in CT angiography: what works best, when, and why. Radiographics 26:905–922. doi:10.1148/rg.263055186
Li X, Liu X, Du X, Ye Z (2014) Diagnostic performance of three-dimensional MR maximum intensity projection for the assessment of synovitis of the hand and wrist in rheumatoid arthritis: a pilot study. Eur J Radiol 83:797–800. doi:10.1016/j.ejrad.2014.02.004
Mori G, Tokunaga D, Takahashi KA et al (2008) Maximum intensity projection as a tool to diagnose early rheumatoid arthritis. Mod Rheumatol 18:247–251. doi:10.1007/s10165-008-0043-2
Taniguchi D, Tokunaga D, Oda R et al (2014) Maximum intensity projection with magnetic resonance imaging for evaluating synovitis of the hand in rheumatoid arthritis: comparison with clinical and ultrasound findings. Clin Rheumatol 33:911–917. doi:10.1007/s10067-014-2526-1
Van der Heijde DM (1996) Plain X-rays in rheumatoid arthritis: overview of scoring methods, their reliability and applicability. Baillieres Clin Rheumatol 10:435–453
Van der Heijde D (1999) How to read radiographs according to the Sharp/van der Heijde method. J Rheumatol 26:743–745
Larsen A, Dale K, Eek M (1977) Radiographic evaluation of rheumatoid arthritis and related conditions by standard reference films. Acta Radiol Diagn (Stockh) 18:481–491
Suter LG, Fraenkel L, Braithwaite RS (2011) Role of magnetic resonance imaging in the diagnosis and prognosis of rheumatoid arthritis. Arthritis Care Res 63:675–688. doi:10.1002/acr.20409
Naredo E, Collado P, Cruz A et al (2007) Longitudinal power Doppler ultrasonographic assessment of joint inflammatory activity in early rheumatoid arthritis: predictive value in disease activity and radiologic progression. Arthritis Rheum 57:116–124. doi:10.1002/art.22461
Kirino Y, Hama M, Takase-Minegishi K et al. (2015) Predicting joint destruction in rheumatoid arthritis with power Doppler, anti-citrullinated peptide antibody, and joint swelling. Mod Rheumatol 1–7. doi: 10.3109/14397595.2015.1026025
Bøyesen P, Haavardsholm EA, Ostergaard M et al (2011) MRI in early rheumatoid arthritis: synovitis and bone marrow oedema are independent predictors of subsequent radiographic progression. Ann Rheum Dis 70:428–433. doi:10.1136/ard.2009.123950
Kita J, Tamai M, Arima K et al (2013) Significant improvement in MRI-proven bone edema is associated with protection from structural damage in very early RA patients managed using the tight control approach. Mod Rheumatol 23:254–259. doi:10.1007/s10165-012-0646-5
Kawashiri S, Suzuki T, Nakashima Y et al (2014) Synovial inflammation assessed by ultrasonography correlates with MRI-proven osteitis in patients with rheumatoid arthritis. Rheumatology (Oxford) 53:1452–1456. doi:10.1093/rheumatology/keu034
Brown AK, Conaghan PG, Karim Z et al (2008) An explanation for the apparent dissociation between clinical remission and continued structural deterioration in rheumatoid arthritis. Arthritis Rheum 58:2958–2967. doi:10.1002/art.23945
Toyama S, Tokunaga D, Fujiwara H et al (2014) Rheumatoid arthritis of the hand: a five-year longitudinal analysis of clinical and radiographic findings. Mod Rheumatol 24:69–77. doi:10.3109/14397595.2013.854054
Takeuchi T, Yamanaka H, Inoue E et al (2008) Retrospective clinical study on the notable efficacy and related factors of infliximab therapy in a rheumatoid arthritis management group in Japan: one-year outcome of joint destruction (RECONFIRM-2J). Mod Rheumatol 18:447–454. doi:10.1007/s10165-008-0077-5
Ikeda K, Nakagomi D, Sanayama Y et al (2013) Correlation of radiographic progression with the cumulative activity of synovitis estimated by power Doppler ultrasound in rheumatoid arthritis: difference between patients treated with methotrexate and those treated with biological agents. J Rheumatol 40:1967–1976. doi:10.3899/jrheum.130556
Kaneko A, Matsushita I, Kanbe K et al (2013) Development and validation of a new radiographic scoring system to evaluate bone and cartilage destruction and healing of large joints with rheumatoid arthritis: ARASHI (Assessment of rheumatoid arthritis by scoring of large joint destruction and healing in radiographic imaging) study. Mod Rheumatol 23:1053–1062. doi:10.1007/s10165-012-0823-6
Acknowledgments
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was conducted according to the principles of the Declaration of Helsinki and approved by the ethics committee of Kyoto Prefectural University of Medicine, and informed consent was obtained from all patients.
Disclosures
None.
Rights and permissions
About this article
Cite this article
Akai, T., Taniguchi, D., Oda, R. et al. Prediction of radiographic progression in synovitis-positive joints on maximum intensity projection of magnetic resonance imaging in rheumatoid arthritis. Clin Rheumatol 35, 873–878 (2016). https://doi.org/10.1007/s10067-016-3208-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-016-3208-y