Abstract
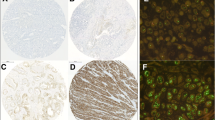
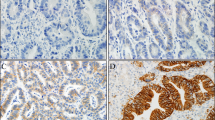
Mucinous adenocarcinoma, gastric type (GAS) is difficult to diagnose and shows poor prognosis. Trastuzumab, an anti-human epidermal growth factor type 2 (HER2) monoclonal antibody, is effective in HER2-positive stomach cancer. The objectives of this study were to identify the clinicopathological characteristics of GAS and to evaluate HER2 expression in GAS. We retrospectively reviewed 322 cervical cancer cases diagnosed at the Kyoto University Hospital from 2010 to 2016. The incidence, clinical factors including age, stage, and lymph node status, tumor markers, immunoreactive expression of MUC6, HIK1083, and HER2, and HER2 amplification were evaluated. Of the 322 cases of cervical cancer, 13 cases of the adenocarcinoma cases were diagnosed as GAS. Watery discharge, lower abdominal pain, CA19-9 elevation, and lymph node metastasis were frequently observed in GAS (p = 0.0226, p = 0.0400, p = 0.0346, and p = 0.0274, respectively). Immunohistochemistry showed positive MUC6 status in all 13 cases and positive HIK1083 status in 8 cases. The HER2 expression status was equivocal in six cases by immunohistochemistry and HER2 amplification was identified in one case. GAS exhibits frequent lymph node metastasis and clinical symptoms such as watery discharge and lower abdominal pain, high levels of CA19-9. In addition, some parts of GAS exhibit HER2 amplification.


Similar content being viewed by others
References
Mikami Y, McCluggage WG (2013) Endocervical glandular lesions exhibiting gastric differentiation: an emerging spectrum of benign, premalignant, and malignant lesions. Adv Anat Pathol 20:227–237
Baalbergen A (2004) Prognostic factors in adenocarcinoma of the uterine cervix. Gynecol Oncol 92:262–267
Iwasaka T, Fukuda K, Hara K, Yokoyama M, Nakao Y, Uchiyama M, Sugimori H (1998) Neoadjuvant chemotherapy with mitomycin C, etoposide, and cisplatin for adenocarcinoma of the cervix. Gynecol Oncol 70:236–240
Kawakami F, Mikami Y, Kojima A, Ito M, Nishimura R, Manabe T (2010) Diagnostic reproducibility in gastric-type mucinous adenocarcinoma of the uterine cervix: validation of novel diagnostic criteria. Histopathology 56:551–553
Bang YJ, Van Cutsem E, Feyereislova A, Chung HC, Shen L, Sawaki A, Lordick F, Ohtsu A, Omuro Y, Satoh T, Aprile G, Kulikov E, Hill J, Lehle M, Ruschoff J, Kang YK, To GATI (2010) Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet 376:687–697
Carleton C, Hoang L, Sah S, Kiyokawa T, Karamurzin YS, Talia KL, Park KJ, McCluggage WG (2016) A detailed immunohistochemical analysis of a large series of cervical and vaginal gastric-type adenocarcinomas. Am J Surg Pathol 40:636–644
Kojima A, Mikami Y, Sudo T, Yamaguchi S, Kusanagi Y, Ito M, Nishimura R (2007) Gastric morphology and immunophenotype predict poor outcome in mucinous adenocarcinoma of the uterine cervix. Am J Surg Pathol 31:664–672
Pecorelli S, Zigliani L, Odicino F (2009) Revised FIGO staging for carcinoma of the cervix. Int J Gynaecol Obstet 105:107–108
Mikami Y, Minamiguchi S, Teramoto N, Nagura M, Haga H, Konishi I (2013) Carbonic anhydrase type IX expression in lobular endocervical glandular hyperplasia and gastric-type adenocarcinoma of the uterine cervix. Pathol Res Pract 209:173–178
Yu J, Zheng W (2016) An alternative method for screening gastric cancer based on serum levels of CEA, CA19-9, and CA72-4. J Gastrointest Cancer 49(1):57–62. https://doi.org/10.1007/s12029-016-9912-7
Kusanagi Y, Kojima A, Mikami Y, Kiyokawa T, Sudo T, Yamaguchi S, Nishimura R (2010) Absence of high-risk human papillomavirus (HPV) detection in endocervical adenocarcinoma with gastric morphology and phenotype. Am J Pathol 177:2169–2175
Kido A, Mikami Y, Koyama T, Kataoka M, Shitano F, Konishi I, Togashi K (2014) Magnetic resonance appearance of gastric-type adenocarcinoma of the uterine cervix in comparison with that of usual-type endocervical adenocarcinoma: a pitfall of newly described unusual subtype of endocervical adenocarcinoma. Int J Gynecol Cancer 24:1474–1479
Takatsu A, Shiozawa T, Miyamoto T, Kurosawa K, Kashima H, Yamada T, Kaku T, Mikami Y, Kiyokawa T, Tsuda H, Ishii K, Togashi K, Koyama T, Fujinaga Y, Kadoya M, Hashi A, Susumu N, Konishi I (2011) Preoperative differential diagnosis of minimal deviation adenocarcinoma and lobular endocervical glandular hyperplasia of the uterine cervix: a multicenter study of clinicopathology and magnetic resonance imaging findings. Int J Gynecol Cancer 21:1287–1296
Stolnicu S, Barsan I, Hoang L, Patel P, Chiriboga L, Terinte C, Pesci A, Aviel-Ronen S, Kiyokawa T, Alvarado-Cabrero I, Pike MC, Oliva E, Park KJ, Soslow RA (2018) Diagnostic algorithmic proposal based on comprehensive immunohistochemical evaluation of 297 invasive endocervical adenocarcinomas. Am J Surg Pathol. https://doi.org/10.1097/PAS.0000000000001090
Park KJ, Kiyokawa T, Soslow RA, Lamb CA, Oliva E, Zivanovic O, Juretzka MM, Pirog EC (2011) Unusual endocervical adenocarcinomas: an immunohistochemical analysis with molecular detection of human papillomavirus. Am J Surg Pathol 35:633–646
Nucci MR, Clement PB, Young RH (1999) Lobular endocervical glandular hyperplasia, not otherwise specified: a clinicopathologic analysis of thirteen cases of a distinctive pseudoneoplastic lesion and comparison with fourteen cases of adenoma malignum. Am J Surg Pathol 23:886–891
Mikami Y, Kiyokawa T, Hata S, Fujiwara K, Moriya T, Sasano H, Manabe T, Akahira J, Ito K, Tase T, Yaegashi N, Sato I, Tateno H, Naganuma H (2004) Gastrointestinal immunophenotype in adenocarcinomas of the uterine cervix and related glandular lesions: a possible link between lobular endocervical glandular hyperplasia/pyloric gland metaplasia and ‘adenoma malignum’. Mod Pathol 17:962–972
Nara M, Hashi A, Murata S, Kondo T, Yuminamochi T, Nakazawa K, Katoh R, Hoshi K (2007) Lobular endocervical glandular hyperplasia as a presumed precursor of cervical adenocarcinoma independent of human papillomavirus infection. Gynecol Oncol 106:289–298
Tsuji T, Togami S, Nomoto M, Higashi M, Fukukura Y, Kamio M, Yonezawa S, Douchi T (2011) Uterine cervical carcinomas associated with lobular endocervical glandular hyperplasia. Histopathology 59:55–62
Nishio S, Tsuda H, Fujiyoshi N, Ota S, Ushijima K, Sasajima Y, Kasamatsu T, Kamura T, Matsubara O (2009) Clinicopathological significance of cervical adenocarcinoma associated with lobular endocervical glandular hyperplasia. Pathol Res Pract 205:331–337
Karamurzin YS, Kiyokawa T, Parkash V, Jotwani AR, Patel P, Pike MC, Soslow RA, Park KJ (2015) Gastric-type endocervical adenocarcinoma: an aggressive tumor with unusual metastatic patterns and poor prognosis. Am J Surg Pathol 39:1449–1457
Park YS, Hwang HS, Park HJ, Ryu MH, Chang HM, Yook JH, Kim BS, Jang SJ, Kang YK (2012) Comprehensive analysis of HER2 expression and gene amplification in gastric cancers using immunohistochemistry and in situ hybridization: which scoring system should we use? Hum Pathol 43:413–422
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL (1987) Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 235:177–182
Kurokawa Y, Matsuura N, Kimura Y, Adachi S, Fujita J, Imamura H, Kobayashi K, Yokoyama Y, Shaker MN, Takiguchi S, Mori M, Doki Y (2015) Multicenter large-scale study of prognostic impact of HER2 expression in patients with resectable gastric cancer. Gastric Cancer 18:691–697
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Nakamura, A., Yamaguchi, K., Minamiguchi, S. et al. Mucinous adenocarcinoma, gastric type of the uterine cervix: clinical features and HER2 amplification. Med Mol Morphol 52, 52–59 (2019). https://doi.org/10.1007/s00795-018-0202-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00795-018-0202-2