Abstract
Objective
To evaluate the thermocycling effect of 3D-printed resins on flexural strength, surface roughness, microbiological adhesion, and porosity.
Materials and methods
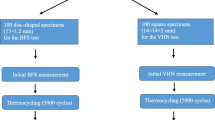
150 bars (8 × 2 × 2 mm) and 100 blocks (8 × 8 × 2 mm) were made and divided into 5 groups, according to two factors: “material” (AR: acrylic resin, CR: composite resin, BIS: bis-acryl resin, CAD: CAD/CAM resin, and PRINT: 3D-printed resin) and “aging” (non-aged and aged – TC). Half of them were subjected to thermocycling (10,000 cycles). The bars were subjected to mini-flexural strength (σ) test (1 mm/min). All the blocks were subjected to roughness analysis (Ra/Rq/Rz). The non-aged blocks were subjected to porosity analysis (micro-CT; n = 5) and fungal adherence (n = 10). Data were statistically analyzed (one-way ANOVA, two-way ANOVA; Tukey’s test, α = 0.05).
Results
For σ, “material” and “aging” factors were statistically significant (p < 0.0001). The BIS (118.23 ± 16.26A) presented a higher σ and the PRINT group (49.87 ± 7.55E) had the lowest mean σ. All groups showed a decrease in σ after TC, except for PRINT. The CRTC showed the lowest Weibull modulus. The AR showed higher roughness than BIS. Porosity revealed that the AR (1.369%) and BIS (6.339%) presented the highest porosity, and the CAD (0.002%) had the lowest porosity. Cell adhesion was significantly different between the CR (6.81) and CAD (6.37).
Conclusion
Thermocycling reduced the flexural strength of most provisional materials, except for 3D-printed resin. However, it did not influence the surface roughness. The CR showed higher microbiological adherence than CAD group. The BIS group reached the highest porosity while the CAD group had the lowest values.
Clinical relevance
3D-printed resins are promising materials for clinical applications because they have good mechanical properties and low fungal adhesion.





Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article (and its supplementary information files).
References
Gratton DG, Aquilino SA (2004) Interim restorations. Dent Clin North Am 48:487–497. https://doi.org/10.1016/j.cden.2003.12.007
Abad-Coronel C, Carrera E, Mena Córdova N, Fajardo JI, Aliaga P (2021) Comparative analysis of fracture resistance between CAD/CAM materials for interim fixed prosthesis. Materials (Basel) 14:7791. https://doi.org/10.3390/ma14247791
Saisadan D, Manimaran P, Meenapriya PK (2016) In vitro comparative evaluation of mechanical properties of temporary restorative materials used in fixed partial denture. J Pharm Bioallied Sci 8:S105–S109. https://doi.org/10.4103/0975-7406.191936
Miura S, Fujisawa M, Komine F, Maseki T, Ogawa T, Takebe J, Nara Y (2019) Importance of interim restorations in the molar region. J Oral Sci 61:195–199. https://doi.org/10.2334/josnusd.19-0102
Peng CC, Chung KH, Ramos VJr, (2020) Assessment of the adaptation of interim crowns using different measurement techniques. J Prosthodont 29:87–93. https://doi.org/10.1111/jopr.13122
Muta S, Ikeda M, Nikaido T, Sayed M, Sadr A, Suzuki T, Tagami J (2020) Chairside fabrication of provisional crowns on FDM 3D-printed PVA model. J Prosthodont Res 64:401–407. https://doi.org/10.1016/j.jpor.2019.11.004
Al Jabbari YS, Al-Rasheed A, Smith JW, Iacopino AM (2013) An indirect technique for assuring simplicity and marginal integrity of provisional restorations during full mouth rehabilitation. Saudi Dent J 25:39–42. https://doi.org/10.1016/j.sdentj.2012.10.003
Vally Z, Sykes LM, Aspeling ME, Van de Merwe J, Ballyram R (2013) In vitro comparison of the compressive strengths of seven different provisional crown materials. SADJ 68:64–67
Dureja I, Yadav B, Malhotra P, Dabas N, Bhargava A, Pahwa R (2018) A comparative evaluation of vertical marginal fit of provisional crowns fabricated by computer-aided design/computer-aided manufacturing technique and direct (intraoral technique) and flexural strength of the materials: an in vitro study. J Indian Prosthodont Soc 18:314–320. https://doi.org/10.4103/jips.jips_306_17
Fernandes NA, Vally ZI, Sykes LM (2015) The longevity of restorations - a literature review. SADJ 70:410–413
Naveen KS, Singh JP, Viswanbaran M, Dhiman RK (2012) Evaluation of flexural strength of resin interim restorations impregnated with various types of silane treated and untreated glass fibres. Med J Armed Forces India 71:S293–S298. https://doi.org/10.1016/j.mjafi.2012.06.015
Yilmaz A, Baydas SS (2007) Fracture resistance of various temporary crown materials. J Contemp Dent Pract 8:044–051
Alt V, Hannig M, Wöstmann B, Balkenhol M (2011) Fracture strength of temporary fixed partial dentures: CAD/CAM versus directly fabricated restorations. Dent Mater 27:339–347. https://doi.org/10.1016/j.dental.2010.11.012
Celej-Piszcz C, Szalewsk L, Kleinrok P, Borowic J (2017) Mechanical properties of materials used for temporary fixed dentures – in vitro study. Curr Issues Pharm Med Sci 30:61–64. https://doi.org/10.1515/cipms-2017-0012
Haselton DR, Diaz-Arnold AM, Dawson DV (2004) Effect of storage solution on surface roughness of provisional crown and fixed partial denture materials. J Prosthodont 13:227–232. https://doi.org/10.1111/j.1532-849X.2004.04039.x
Li Z, Sun J, Lan J, Qi Q (2016) Effect of a denture base acrylic resin containing silver nanoparticles on Candida albicans adhesion and biofilm formation. Gerodontology 33:209–216. https://doi.org/10.1111/ger.12142
Derchi G, Vano M, Barone A, Covani U, Diaspro A, Salerno M (2017) Bacterial adhesion on direct and indirect dental restorative composite resins: an in vitro study on a natural biofilm. J Prosthet Dent 117:669–676. https://doi.org/10.1016/j.prosdent.2016.08.022
Beldüz N, Kamburoğlu A, Yilmaz Y, Tosun I, Beldüz M, Kara C (2017) Evaluation of candida albicans biofilm formation on various dental restorative material surfaces. Niger J Clin Pract 20:355–360. https://doi.org/10.4103/1119-3077.198388
Perry RD, Magnuson B (2012) Provisional materials: key components of interim fixed restorations. Compend Contin Educ Dent 33:59–62
Tahayeri AD, Morgan M, Fugolin AP, Bompolaki D, Athirasala A, Pfeifer CS, Ferracane JL, Bertassoni LE (2018) 3D printed versus conventionally cured provisional crown and bridge dental materials. Dent Mater 34:192–200. https://doi.org/10.1016/j.dental.2017.10.003
Sari T, Usumez A, Strasser T, Şahinbas A, Rosentritt M (2020) Temporary materials: comparison of in vivo and in vitro performance. Clin Oral Investig 24:4061–4068. https://doi.org/10.1007/s00784-020-03278-5
Aldahian N, Khan R, Mustafa M, Vohra F, Alrahlah A (2021) Influence of conventional, CAD-CAM, and 3D printing fabrication techniques on the marginal integrity and surface roughness and wear of interim crowns. Appl Sci 11:8964. https://doi.org/10.3390/app11198964
Lambert H, Durand JC, Jacquot B, Fages M (2017) Dental biomaterials for chairside CAD/CAM: state of the art. Korean Acad Prosthodont 9:486–495. https://doi.org/10.4047/jap.2017.9.6.486
Myagmar G, Lee JH, Ahn JS, Yeo IL, Yoon HI, Han JS (2021) Wear of 3D printed and CAD/CAM milled interim resin materials after chewing simulation. J Adv Prosthodont 13:144–151. https://doi.org/10.4047/jap.2021.13.3.144
Tian Y, Chen C, Xu X, Wang J, Hou X, Li K, Lu X, Shi H, Lee E, Jiang HB (2021) A review of 3D printing in dentistry: technologies, affecting factors, and applications. Scanning 2021:9950131. https://doi.org/10.1155/2021/9950131
Kim YH, Jung BY, Han SS, Woo CW (2020) Accuracy evaluation of 3D printed interim prosthesis fabrication using a CBCT scanning based digital model. PLoS One 15:e0240508. https://doi.org/10.1371/journal.pone.0240508
Park JY, Jeong ID, Lee JJ, Bae SY, Kim JH, Kim WC (2016) In vitro assessment of the marginal and internal fits of interim implant restorations fabricated with different methods. J Prosthet Dent 116:536–542. https://doi.org/10.1016/j.prosdent.2016.03.012
Kim DY, Jeon JH, Kim JH, Kim HY, Kim WC (2017) Reproducibility of different arrangement of resin copings by dental microstereolithography: evaluating the marginal discrepancy of resin copings. J Prosthet Dent 117:260–265. https://doi.org/10.1016/j.prosdent.2016.07.007
Rayyan MM, Aboushelib M, Sayed NM, Ibrahim A, Jimbo R (2015) Comparison of interim restorations fabricated by CAD/CAM with those fabricated manually. J Prosthet Dent 114:414–419. https://doi.org/10.1016/j.prosdent.2015.03.007
Yao J, Li J, Wang Y, Huang H (2014) Comparison of the flexural strength and marginal accuracy of traditional and CAD/CAM interim materials before and after thermal cycling. J Prosthet Dent 112:649–657. https://doi.org/10.1016/j.prosdent.2014.01.012
Digholkar S, Madhav VN, Palaskar J (2016) Evaluation of the flexural strength and microhardness of provisional crown and bridge materials fabricated by different methods. J Indian Prosthodont Soc 16:328–334. https://doi.org/10.4103/0972-4052.191288
Park SM, Park JM, Kim SK, Heo SJ, Koak JY (2020) Flexural strength of 3D-printing resin materials for provisional fixed dental prostheses. Materials (Basel) 13:3970. https://doi.org/10.3390/ma13183970
Gonçalves TS, Spohr AM, de Souza RM, de Menezes LM (2008) Surface roughness of auto polymerized acrylic resin according to different manipulation and polishing methods: an in situ evaluation. Angle Orthod 78:931–934. https://doi.org/10.2319/080307-363.1
Soares IA, Leite PKBDS, Farias OR, Lemos GA, Batista AUD, Montenegro RV (2019) Polishing methods’ influence on color stability and roughness of 2 provisional prosthodontic materials. J Prosthodont 28:564–571. https://doi.org/10.1111/jopr.13062
Mondelli RF, Garrido LM, Soares AF, Rodriguez-Medina AD, Mondelli J, Lucena FS, Furuse AY (2022) Effect of simulated brushing on surface roughness and wear of bis-acryl-based materials submitted to different polishing protocols. J Clin Exp Dent 14:e168–e176. https://doi.org/10.4317/jced.58920
Kawano F, Ohguri T, Ichikawa T, Matsumoto N (2001) Influence of thermal cycles in water on flexural strength of laboratory-processed composite resin. J Oral Rehabil 28:703–707. https://doi.org/10.1046/j.1365-2842.2001.00724.x
Atria PJ, Lagos I, Sampaio CS (2020) In vitro evaluation of surface roughness, color stability, and color masking of provisional restoration materials for veneers and crowns. Int J Comput Dent 23:343–350
Oliveira JC, Aiello G, Mendes B, Urban VM, Campanha NH, Jorge JH (2010) Effect of storage in water and thermocycling on hardness and roughness of resin materials for temporary restorations. Mater Res 13:355–359. https://doi.org/10.1590/S1516-14392010000300013
Mehrpour H, Farjood E, Giti R, Ghasrdashti AB, Heidari H (2016) Evaluation of the flexural strength of interim restorative materials in fixed prosthodontics. J Dent (Shiraz) 17:201–206
Kadiyala KK, Badisa MK, Anne G, Anche SC, Chiramana S, Muvva SB, Zakkula S, Jyothula RRD (2016) Evaluation of flexural strength of thermocycled interim resin materials used in prosthetic rehabilitation- an in-vitro study. J Clin Diagn Res 10:ZC91-ZC95. https://doi.org/10.7860/JCDR/2016/20020.8566
Barnes CM, Covey D, Watanabe H, Simetich B, Schulte JR, Chen H (2014) An in vitro comparison of the effects of various air polishing powders on enamel and selected esthetic restorative materials. J Clin Dent 25:76–87
Vila-Nova TEL, de Carvalho IHG, Moura DMD, Batista AUD, Zhang Y, Paskocimas CA, Bottino MA, Souza ROA (2020) Effect of finishing/polishing techniques and low temperature degradation on the surface topography, phase transformation and flexural strength of ultra-translucent ZrO2 ceramic. Dent Mater 36:e126–e139. https://doi.org/10.1016/j.dental.2020.01.004
de Carvalho IHG, da Silva NR, Vila-Nova TEL, de Almeida LFD, Veríssimo AH, de Melo RM, Zhang Y, Souza ROA (2022) Effect of finishing/polishing techniques and aging on topography, C. albicans adherence, and flexural strength of ultra-translucent zirconia: an in situ study. Clin Oral Investig 26:889–900. https://doi.org/10.1007/s00784-021-04068-3
Cavalcanti YW, Morse DJ, da Silva WJ, Del-Bel-Cury AA, Wei X, Wilson M, Milward P, Lewis M, Bradshaw D, Williams DW (2015) Virulence and pathogenicity of Candida albicans is enhanced in biofilms containing oral bacteria. Biofouling 31:27–38. https://doi.org/10.1080/08927014.2014.996143
Gale MS, Darvell BW (1999) Thermal cycling procedures for laboratory testing of dental restorations. J Dent 27:89–99. https://doi.org/10.1016/s0300-5712(98)00037-2
Barker TM, Earwaker WJ, Lisle DA (1994) Accuracy of stereolithographic models of human anatomy. Australas Radiol 38:106–111. https://doi.org/10.1111/j.1440-1673.1994.tb00146.x
Hazeveld A, Slater JJH, Ren Y (2014) Accuracy and reproducibility of dental replica models reconstructed by different rapid prototyping techniques. Am J Orthod Dentofacial Orthop 145:108–115. https://doi.org/10.1016/j.ajodo.2013.05.011
Haselton DR, Diaz-Arnold AM, Vargas MA (2002) Flexural strength of provisional crown and fixed partial denture resins. J Prosthet Dent 87:225–228. https://doi.org/10.1067/mpr.2002.121406
Nejatidanesh F, Momeni G, Savabi O (2009) Flexural strength of interim resin materials for fixed prosthodontics. J Prosthodont 18:507–511. https://doi.org/10.1111/j.1532-849X.2009.00473.x
Almeida CS, Amaral M, Gonçalves FCP, de ArrudaPaes-Junior TJ (2016) Effect of an experimental silica-nylon reinforcement on the fracture load and flexural strength of bisacrylic interim partial fixed dental prostheses. J Prosthet Dent 115:301–305. https://doi.org/10.1016/j.prosdent.2015.08.009
Endo T, Finger WJ, Kanehira M, Utterodt A, Komatsu M (2010) Surface texture and roughness of polished nanofill and nanohybrid resin composites. Dent Mater J 29:213–223. https://doi.org/10.4012/dmj.2009-019
Gantz L, Fauxpoint G, Arntz Y, Pelletier H, Etienne O (2021) In vitro comparison of the surface roughness of polymethyl methacrylate and bis-acrylic resins for interim restorations before and after polishing. J Prosthet Dent 125:833.e1-833.e10. https://doi.org/10.1016/j.prosdent.2021.02.009
Köroğlu A, Sahin O, Dede DÖ, Yilmaz B (2016) Effect of different surface treatment methods on the surface roughness and color stability of interim prosthodontic materials. J Prosthet Dent 115:447–455. https://doi.org/10.1016/j.prosdent.2015.10.005
Revilla-León M, Morillo JA, Att W, Özcan M (2021) Chemical composition, Knoop hardness, surface roughness, and adhesion aspects of additively manufactured dental interim materials. J Prosthodont 30:698–705. https://doi.org/10.1111/jopr.13302
Giti R, Dabiri S, Motamedifar M, Derafshi R (2021) Surface roughness, plaque accumulation, and cytotoxicity of provisional restorative materials fabricated by different methods. PLoS One 16:e0249551. https://doi.org/10.1371/journal.pone.0249551
Cox BD, Wilcox RK, Levesley MC, Hall RM (2006) Assessment of a three-dimensional measurement technique for the porosity evaluation of PMMA bone cement. J Mater Sci Mater Med 17:553–557. https://doi.org/10.1007/s10856-006-8939-x
Quirynen M, Marechal M, Busscher HJ, Weerkamp AH, Darius PL, van Steenberghe D (1990) The influence of surface free energy and surface roughness on early plaque formation. An in vivo study in man. J Clin Periodontol 17:138–144. https://doi.org/10.1111/j.1600-051x.1990.tb01077.x
Kumar GV, Devi R, Anto N (2016) Evaluation and comparison of the surface roughness and porosity of different provisional restorative materials: an in vitro study. J Dent 8:39–45. https://doi.org/10.5005/jp-journals-10063-0010
Hiramatsu DA, Moretti-Neto RT, Feraz BFR, Porto VC, Rubo JH (2011) Roughness and porosity of provisional crowns. RPG 18:108–112
Jerolimov V, Brooks SC, Huggett R, Bates JF (1989) Rapid curing of acrylic denture-base materials. Dent Mater 5:18–22. https://doi.org/10.1016/0109-5641(89)90086-9
Singh S, Palaskar JN, Mittal S (2013) Comparative evaluation of surface porosities in conventional heat polymerized acrylic resin cured by water bath and microwave energy with microwavable acrylic resin cured by microwave energy. Contemp Clin Dent 4:147–151. https://doi.org/10.4103/0976-237X.114844
Karaokutan I, Sayin G, Kara O (2015) In vitro study of fracture strength of provisional crown materials. J Adv Prosthodont 7:27–31. https://doi.org/10.4047/jap.2015.7.1.27
Schwedhelm ER (2006) Direct technique for the fabrication of acrylic provisional restorations. J Contemp Dent Pract 7:157–173
Maalhagh-Fard A, Wagner WC, Pink FE, Neme AM (2003) Evaluation of surface finish and polish of eight provisional restorative materials using acrylic bur and abrasive disk with and without pumice. Oper Dent 28:734–739
Tupinambá ÍVM, Giampá PCC, Rocha IAR, Lima EMCX (2018) Effect of different polishing methods on surface roughness of provisional prosthetic materials. J Indian Prosthodont Soc 18:96–101. https://doi.org/10.4103/jips.jips_258_17
Taşın S, Ismatullaev A, Usumez A (2021) Comparison of surface roughness and color stainability of 3-dimensionally printed interim prosthodontic material with conventionally fabricated and CAD-CAM milled materials. J Prosthet Dent S0022–3913:00075–00085. https://doi.org/10.1016/j.prosdent.2021.01.027
Ozel GS, Guneser MB, Inan O, Eldeniz AU (2017) Evaluation of C. Albicans and S. Mutans adherence on different provisional crown materials. J Adv Prosthodont 9:335–340. https://doi.org/10.4047/jap.2017.9.5.335
Bürgers R, Gerlach T, Hahnel S, Schwarz F, Handel G, Gosau M (2010) In vivo and in vitro biofilm formation on two different titanium implant surfaces. Clin Oral Implants Res 21:156–164. https://doi.org/10.1111/j.1600-0501.2009.01815.x
Quirynen M, De Soete M, Van Steenberghe D (2002) Infectious risks for oral implants: a review of the literature. Clin Oral Implants Res 13:1–19. https://doi.org/10.1034/j.1600-0501.2002.130101.x
Kiomarsi N, Saburian P, Chiniforush N, Karazifard MJ, Hashemikamangar SS (2017) Effect of thermocycling and surface treatment on repair bond strength of composite. J Clin Exp Dent 9:e945–e951. https://doi.org/10.4317/jced.53721
Pinto JRR, Mesquita MF, Henriques GEP, Nóbilo MAA (2004) Evaluation of varying amounts of thermal cycling on bond strength and permanent deformation of two resilient denture liners. J Prosthet Dent 92:288–293. https://doi.org/10.1016/j.prosdent.2004.06.005
Bollen CML, Lambrechts P, Quirynen M (1997) Comparison of surface roughness of oral hard materials to the threshold surface roughness for bacterial plaque retention: a review of the literature. Dent Mater 13:258–269. https://doi.org/10.1016/s0109-5641(97)80038-3
Acknowledgements
The authors thank the Science and Technology Institute of the State University of São Paulo (UNESP), São José dos Campos/SP, Brazil, for their support in thermocycling test.
Funding
This study was financed in part by the Coordination for the Improvement of Higher Education Personnel (CAPES) – Finance Code 001.
Author information
Authors and Affiliations
Contributions
Anne Kaline Claudino Ribeiro, Rodrigo Falcão Carvalho Porto de Freitas, and Isabelle Helena Gurgel de Carvalho: methodology, formal analysis, investigation, resources, data curation, writing—original draft; Larissa Mendonça de Miranda and Nathália Ramos da Silva and Leopoldina de Fátima Dantas de Almeida: formal analysis, data curation; Adriana da Fonte Porto Carreiro: writing—review and editing, formal analysis; supervision, data curation; Yu Zhang: writing—review and editing, visualization, supervision; Rodrigo Othávio de Assunção e Souza: conceptualization, writing—review and editing, supervision, project administration and funding acquisition.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ribeiro, A.K.C., de Freitas, R.F.C.P., de Carvalho, I.H.G. et al. Flexural strength, surface roughness, micro-CT analysis, and microbiological adhesion of a 3D-printed temporary crown material. Clin Oral Invest 27, 2207–2220 (2023). https://doi.org/10.1007/s00784-023-04941-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-04941-3