Abstract
Objectives
To assess the biological, antimicrobial, and mechanical effects of the treatment of deep dentin with simvastatin (SV) before application of a glass-ionomer cement (GIC).
Materials and methods
Dentin discs were adapted to artificial pulp chambers and SV (2.5 or 1.0 mg/mL) was applied to the occlusal surface, either previously conditioned or not with EDTA (±EDTA). The extracts (culture medium + SV that diffused through dentin) was obtained and then applied to cultured odontoblast-like MDPC-23 cells. Cell viability, alkaline phosphatase (ALP) activity, and mineralization nodule (MN) deposition were evaluated. Untreated discs were used as control. The antibacterial activity of SV (2.5 or 1.0 mg/mL) against Streptococcus mutans and Lactobacillus acidophilus, as well as the bond strength of GIC to dentin in the presence of SV 2.5 mg/mL (±EDTA) were also assessed. The data were analyzed by ANOVA/Tukey tests (α = 5%).
Results
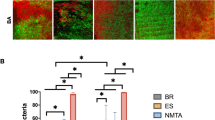
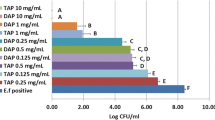
EDTA + SV 2.5 mg/mL significantly enhanced the ALP activity and MN deposition in comparison with the control, without changing in the cell viability (p < 0.05). The association EDTA + SV 2.5 mg/mL + GIC determined the highest ALP and MN values (p < 0.05). SV presented intense antimicrobial activity, and the EDTA dentin conditioning followed by SV application increased bond strength values compared with SV treatment alone (p < 0.05).
Conclusion
SV presents antimicrobial activity and diffuses across conditioned dentin to biostimulate odontoblast-like pulp cells.
Clinical significance
The use of SV as adjuvant agent for indirect pulp capping may biostimulate pulp cells thus preserving vitality and function of the pulp-dentin complex.







Similar content being viewed by others
References
Wataha JC (2012) Predicting clinical biological responses to dental materials. Dent Mater 28:23–40. https://doi.org/10.1016/j.dental.2011.08.595
de Souza Costa CA, Hebling J, Scheffel DL, Soares DG, Basso FG, Ribeiro AP (2014) Methods to evaluate and strategies to improve the biocompatibility of dental materials and operative techniques. Dent Mater 30:769–784. https://doi.org/10.1016/j.dental.2014.04.010
Hilton TJ (2002) Can modern restorative procedures and materials reliably seal cavities? In vitro investigations. Part 1. Am J Dent 15:198–210
Mitra SB, Lee CY, Bui HT, Tantbirojn D, Rusin RP (2009) Long-term adhesion and mechanism of bonding of a paste-liquid resin-modified glass-ionomer. Dent Mater 25:459–466. https://doi.org/10.1016/j.dental.2008.09.008
Xie D, Brantley WA, Culbertson BM, Wang G (2000) Mechanical properties and microstructures of glass-ionomner cements. Den Mater 16:129–138. https://doi.org/10.1016/S0109-5641(99)00093-7
Six N, Lasfargues JJ, Goldberg M (2000) In vivo study of the pulp reaction to Fuji IX, a glass ionomer cement. J Dent 28:413–422. https://doi.org/10.1016/S0300-5712(00)00015-4
Costa CA, Giro EM, do Nascimento AB, Teixeira HM, Hebling J (2003) Short-term evaluation of the pulp-dentin complex response to a resin-modified glass-ionomer cement and a bonding agent applied in deep cavities. Dent Mater 19:739–746. https://doi.org/10.1016/S0109-5641(03)00021-6
de Souza Costa CA, Teixeira HM, Lopes do Nascimento AB, Hebling J (2007) Biocompatibility of resin-based dental materials applied as liners in deep cavities prepared in human teeth. J Biomed Mater Res B Appl Biomater 81:175–184. https://doi.org/10.1002/jbm.b.30651
Costa CA, Ribeiro AP, Giro EM, Randall RC, Hebling J (2011) Pulp response after application of two resin modified glass ionomer cements (RMGICs) in deep cavities of prepared human teeth. Dent Mater 27:e158–e170. https://doi.org/10.1016/j.dental.2011.04.002
Okamoto Y, Sonoyama W, Ono M, Akiyama K, Fujisawa T, Oshima M, Tsuchimoto Y, Matsuka Y, Yasuda T, Shi S, Kuboki T (2009) Simvastatin induces the odontogenic differentiation of human dental pulp stem cells in vitro and in vivo. J Endod 35:367–372. https://doi.org/10.1016/j.joen.2008.11.024
Min KS, Lee YM, Hong SO, Kim EC (2010) Simvastatin promotes odontoblastic differentiation and expression of angiogenic factors via heme oxygenase-1 in primary cultured human dental pulp cells. J Endod 36:447–452. https://doi.org/10.1016/j.joen.2009.11.021
Tanigo T, Takaoka R, Tabata Y (2010) Sustained release of water-insoluble simvastatin from biodegradable hydrogel augments bone regeneration. J Control Release 143:201–206. https://doi.org/10.1016/j.jconrel.2009.12.027
Wadagaki R, Mizuno D, Yamawaki-Ogata A, Satake M, Kaneko H, Hagiwara S, Yamamoto N, Narita Y, Hibi H, Ueda M (2011) Osteogenic induction of bone marrow-derived stromal cells on simvastatin-releasing, biodegradable, nano- to microscale fiber scaffolds. Ann Biomed Eng 39:1872–1881. https://doi.org/10.1007/s10439-011-0327-0
Karanxha L, Park SJ, Son WJ, Nör JE, Min KS (2013) Combined effects of simvastatin and enamel matrix derivative on odontoblastic differentiation of human dental pulp cells. J Endod 39:76–82. https://doi.org/10.1016/j.joen.2012.10.013
Miyazawa A, Matsuno T, Asano K, Tabata Y, Satoh T (2015) Controlled release of simvastatin from biodegradable hydrogels promotes odontoblastic differentiation. Dent Mater J 34:466–474. https://doi.org/10.4012/dmj.2014-272
Lee SY, Min KS, Choi GW, Park JH, Park SH, Lee SI, Kim EC (2012) Effects of simvastain and enamel matrix derivative on Portland cement with bismuth oxide-induced growth andodontoblastic differentiation in human dental pulp cells. J Endod 38:405–410. https://doi.org/10.1016/j.joen.2011.12.025
Soares DG, Zhang Z, Mohamed F, Eyster TW, de Souza Costa CA, Ma PX (2018) Simvastatin and nanofibrous poly(l-lactic acid) scaffolds to promote the odontogenic potential of dental pulp cells in an inflammatory environment. Acta Biomater 1:190–203. https://doi.org/10.1016/j.actbio.2017.12.037
Leite MLAS, Soares DG, Basso FG, Hebling J, de Souza Costa CA (2017) Biostimulatory effects of simvastatin on MDPC-23 odontoblast-like cells. Braz Oral Res 18:e104. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0104
Varalakshmi PR, Kavitha M, Govindan R, Narasimhan S (2013) Effect of statins with α-tricalcium phosphate on proliferation, differentiation, and mineralization of human dental pulp cells. J Endod 39:806–812. https://doi.org/10.1016/j.joen.2012.12.036
Jia W, Zhao Y, Yang J, Wang W, Wang X, Ling L, Ge L (2016) Simvastatin promotes dental pulp stem cell–induced coronal pulp regeneration in pulpotomized teeth. J Endod 42:1049–1054. https://doi.org/10.1016/j.joen.2016.03.007
Ferracane JL, Cooper PR, Smith AJ (2010) Can interaction of materials with the dentin-pulp complex contribute to dentin regenetarion? Odontology 98:2–14. https://doi.org/10.1007/s10266-009-0116-5
Leite MLAS, Costa CAS, Duarte RM, Andrade AKM, Soares DG (2018) Bond strength and cytotoxicity of a universal adhesive according to the hybridization strategies to dentin. Braz Dent J 29:68–75. https://doi.org/10.1590/0103-6440201801698
Hanks CT, Sun ZL, Fang DN, Edwards CA, Wataha JC, Ritchie HH, Butler WT (1998) Cloned 3T6 cell line from CD-1 mouse fetal molar dental papillae. Connect Tissue Res 37:233–249. https://doi.org/10.3109/03008209809002442
Soares DG, Gonçalves Basso F, Hebling J, de Souza Costa CA (2015) Effect of hydrogen-peroxide-mediated oxidative stress on human dental pulp cells. J Dent 43:750–756. https://doi.org/10.1016/j.jdent.2014.12.006
Bianchi L, Ribeiro AP, de Oliveira Carrilho MR, Pashley DH, de Souza Costa CA, Hebling J (2013) Transdentinal cytotoxicity of experimental adhesive systems of different hydrophilicity applied to ethanol-saturated dentin. Dent Mater 29:980–990. https://doi.org/10.1016/j.dental.2013.07.006
Scheffel DL, Sacono NT, Ribeiro AP, Soares DG, Basso FG, Pashley D, Costa CA, Hebling J (2015) Immediate human pulp response to ethanol-wet bonding technique. J Dent 43:537–545. https://doi.org/10.1016/j.jdent.2015.02.014
Jacques P, Hebling J (2005) Effect of dentin conditioners on the microtensile bond strength of a conventional and a self-etching primer adhesive system. Dent Mater 21:103–109. https://doi.org/10.1016/j.dental.2003.12.004
Kasraei S, Azarsina M, Khamverdi Z (2013) Effect of ethylene diamine tetra acetic acid and sodium hypochlorite solution conditioning on microtensile bond strength of one-step self-etch adhesives. J Conserv Dent 16:243–246. https://doi.org/10.4103/0972-0707.111324
Ishihata H, Kanehira M, Finger WJ, Takahashi H, Tomita M, Sasaki K (2017) Effect of two desensitizing agents on dentin permeability in vitro. J Appl Oral Sci 25:34–41. https://doi.org/10.1590/1678-77572016-0228
Saewong S, Thammasitboon K, Wattanaroonwong N (2013) Simvastatin induces apoptosis and disruption of the actin cytoskeleton in human dental pulp cells and periodontal ligament fibroblasts. Arch Oral Biol 58:964–974. https://doi.org/10.1016/j.archoralbio.2013.03.002
Baek KH, Lee WY, Oh KW, Tae HJ, Lee JM, Lee EJ, Han JH, Kang MI, Cha BY, Lee KW, Son HY, Kang SK (2005) The effect of simvastatin on the proliferation and differentiation of human bone marrow stromal cells. J Korean Med Sci 20:438–444. https://doi.org/10.3346/jkms.2005.20.3.438
Kupcsik L, Meurya T, Flury M, Stoddart M, Alini M (2009) Statin-induced calcification in human mesenchymal stem cells is cell death related. J Cell Mol Med 13:4465–4473. https://doi.org/10.1111/j.1582-4934.2008.00545.x
Sidhu SK, Nicholson JW (2016) A review of glass-ionomer cements for clinical dentistry. J Funct Biomater 7:1–15. https://doi.org/10.3390/jfb7030016
de Souza Costa CA, Hebling J, Garcia-Godoy F, Hanks CT (2003) In vitro cytotoxicity of five glass-ionomer cements. Biomaterials 24:3853–3858. https://doi.org/10.1016/S0142-9612(03)00253-9
Ben-Amar A, Liberman R, Apatowsky U, Pilo R (1999) pH changes of glass-ionomer lining materials at various time intervals. J Oral Rehabil 26:847–852. https://doi.org/10.1046/j.1365-2842.1999.00480.x
Camilleri J, Montesin FE, Juszczyk AS, Papaioannou S, Curtis RV, Donald FM (2008) The constitution, physical properties and biocompatibility of modified accelerated cement. Dent Mater 24:341–350. https://doi.org/10.1016/j.dental.2007.06.004
Stanislawski L, Daniau X, Lauti A, Goldberg M (1999) Factors responsible for pulp cell cytotoxicity induced by resin-modified glass ionomer cements. J Biomed Mater Res 48:277–288. https://doi.org/10.1002/(SICI)1097-4636(1999)48:3<277::AID-JBM11>3.0.CO;2-T
do Nascimento AB, Fontana UF, Teixeira HM, Costa CA (2000) Biocompatibility of a resin-modified glass ionomer cement applied as pulp capping in human teeth. Am J Dent 13:28–34
Souza PP, Aranha AM, Hebling J, Giro EM, Costa CA (2006) In vitro cytotoxicity and in vivo biocompatibility of contemporary resin-modified glass-ionomer cements. Dent Mater 22:838–844. https://doi.org/10.1016/j.dental.2005.10.002
Soares DG, Basso FG, Scheffel DL, Giro EM, de Souza Costa CA, Hebling J (2016) Biocompatibility of a restorative resin-modified glass ionomer cement applied in very deep cavities prepared in human teeth. Gen Dent 64:33–40
Gerzina TM, Hume WR (1994) Effect of dentin on release of TEGMA from resin composite in vitro. J Oral Rehabil 21:463–468. https://doi.org/10.1016/j.dental.2005.10.002
Hume WR (1994) Influence of dentine on the pulpward release of eugenol or acids from restorative materials. J Oral Rehabil 21:469–473. https://doi.org/10.1111/j.1365-2842.1994.tb01161.x
Asl Aminabadi N, Maljaei E, Erfanparast L, Ala Aghbali A, Hamishehkar H, Najafpour E (2013) Simvastatin versus calcium hydroxide direct pulp capping of human primary molars: a randomized clinical trial. J Dent Res Dent Clin Dent Prospects 7:8–14. https://doi.org/10.5681/joddd.2013.002
Stein D, Lee Y, Schmid MJ, Killpack B, Genrich MA, Narayana N, Marx DB, Cullen DM, Reinhardt RA (2005) Local simvastatin effects on mandibular bone growth and inflammation. J Periodontol 76:1861–1870. https://doi.org/10.1902/jop.2005.76.11.1861
Bergman P, Linde C, Pütsep K, Pohanka A, Normark S, Henriques-Normark B, Andersson J, Björkhem-Bergman L (2011) Studies on the antibacterial effects of statins—in vitro and in vivo. PLoS One 6:e24394. https://doi.org/10.1371/journal.pone.0024394
Haeri MR, White K, Qharebeglou M, Ansar MM (2015) Cholesterol suppresses antimicrobial effect of statins. Iran J Basic Med Sci 18:1253–1256. https://doi.org/10.22038/IJBMS.2015.6282
Macreadie IG, Johnson G, Schlosser T, Macreadie PI (2006) Growth inhibition of Candida species and Aspergillus fumigatus by statins. FEMS Microbiol Lett 262:9–13. https://doi.org/10.1111/j.1574-6968.2006.00370.x
Youm SH, Jung KH, Son SA, Kwon YH, Park JK (2015) Effect of dentin pretreatment and curing mode on the microtensile bond strength of self-adhesive resincements. J Adv Prosthodont 7:317–322. https://doi.org/10.4047/jap.2015.7.4.317
El-Askary FS, Nassif MS (2011) The effect of the pre-conditioning step on the shear bond strength of nano-filled resin-modified glass-ionomer to dentin. Eur J Dent 5:150–156
Munirathinam D, Mohanaj D, Beganam M (2012) Efficacy of various cleansing techniques on dentin wettability and its influence on shear bond strength of a resin luting agent. J Adv Prosthodont 4:139–145. https://doi.org/10.4047/jap.2012.4.3.139
Czarnecka B, Deregowska-Nosowicz P, Limanowska-Shaw H, Nicholson JW (2007) Shear bond strengths of glass-ionomer cements to sound and to prepared carious dentine. J Mater Sci Mater Med 18:845–849. https://doi.org/10.1007/s10856-006-0085-y
Funding
The work was supported by financial support from the São Paulo Research Foundation/FAPESP (grant # 2015/15635-7) and the National Council for Scientific and Technological Development/CNPq (grant #s 303599/2014-6 and 443153/2014-0).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
This study was approval by the Research Ethics Committee of Araraquara School of Dentistry, São Paulo, Brazil (Proc. No.: 51908415.3.0000.5416). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Leite, M.L., Soares, D.G., de Oliveira Duque, C.C. et al. Positive influence of simvastatin used as adjuvant agent for cavity lining. Clin Oral Invest 23, 3457–3469 (2019). https://doi.org/10.1007/s00784-018-2757-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2757-7