Abstract
Objective
To test whether or not one out of two alloplastic materials used for ridge preservation (RP) is superior to the other in terms of volumetric and linear ridge changes over time.
Materials and methods
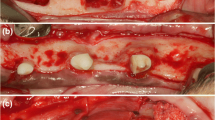
In 16 adult beagle dogs, the distal roots of P3 and P4 were extracted and 50% of the buccal bone plate removed. Ridge preservation was performed randomly using two different alloplastic bone grafting substitutes (poly lactic-co-glycolic acid (PLGA) coated biphasic calcium phosphate particles consisting of 60% hydroxyapatite (HA) and 40% beta-tricalcium phosphate (ß-TCP=test 1), (a biphasic calcium phosphate consisting 60% HA and 40% ß-TCP=test 2) and a resorbable collagen membrane or a control group (sham). Sacrifice was performed at three time-points (4, 8, 16 weeks later). Impressions were taken before extraction, after RP, and at sacrifice, allowing for assessment of volumetric changes. A multi-way ANOVA was computed, and partial Type-II F tests were performed.
Results
Both ridge preservation procedures minimized the volume loss compared to spontaneous healing. The median buccal volume changes between pre-extraction and sacrifice were − 1.76 mm (Q1 = − 2.56; Q3 = − 1.42) for test 1, − 1.62 mm (Q1 = − 2.06; Q3 = − 1.38) for test 2, and − 2.42 mm (Q1 = − 2.63; Q3 = − 2.03) for control. The mean ridge width measurements did not show statistically significant differences between test 1 (− 2.51 mm; Q1 = − 3.25; Q3 = − 1.70) and test 2 (− 2.04 mm; Q1 = − 3.82; Q3 = − 1.81) (p = 0.813), but between test and control (− 3.85 mm; Q1 = − 5.02; Q3 = − 3.27) (p = 0.003).
Conclusions
Both RP techniques were successful in maintaining the buccal contour from pre-extraction to sacrifice to a similar extent and more favorable compared to spontaneous healing.
Clinical relevance
Alloplastic materials can successfully be used for RP procedures.





Similar content being viewed by others
References
Araujo MG, Liljenberg B, Lindhe J (2010) Beta-Tricalcium phosphate in the early phase of socket healing: an experimental study in the dog. Clin Oral Implants Res 21(4):445–454. https://doi.org/10.1111/j.1600-0501.2009.01876.x
Araujo MG, Lindhe J (2005) Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol 32(2):212–218. https://doi.org/10.1111/j.1600-051X.2005.00642.x
Araujo MG, Lindhe J (2009) Ridge preservation with the use of Bio-Oss Collagen: a 6-month study in the dog. Clin Oral Implants Res 20(5):433–440. https://doi.org/10.1111/j.1600-0501.2009.01705.x
Artzi Z, Tal H, Dayan D (2000) Porous bovine bone mineral in healing of human extraction sockets. Part 1: histomorphometric evaluations at 9 months. J Periodontol 71(6):1015–1023. https://doi.org/10.1902/jop.2000.71.6.1015
Atwood DA (2001) Some clinical factors related to rate of resorption of residual ridges. J Prosthet Dent 86:119–125
Avila-Ortiz G, Elangovan S, Kramer KW, Blanchette D, Dawson DV (2014) Effect of alveolar ridge preservation after tooth extraction: a systematic review and meta-analysis. J Dent Res 93(10):950–958. https://doi.org/10.1177/0022034514541127
Barone A, Aldini NN, Fini M, Giardino R, Calvo Guirado JL, Covani U (2008) Xenograft versus extraction alone for ridge preservation after tooth removal: a clinical and histomorphometric study. J Periodontol 79(8):1370–1377. https://doi.org/10.1902/jop.2008.070628
Barone A, Orlando B, Cingano L, Marconcini S, Derchi G, Covani U (2012) A randomized clinical trial to evaluate and compare implants placed in augmented versus non-augmented extraction sockets: 3-year results. J Periodontol 83(7):836–846. https://doi.org/10.1902/jop.2011.110205
Barone A, Ricci M, Tonelli P, Santini S, Covani U (2013) Tissue changes of extraction sockets in humans: a comparison of spontaneous healing vs. ridge preservation with secondary soft tissue healing. Clin Oral Implants Res 24:1231–1237. https://doi.org/10.1111/j.1600-0501.2012.02535.x
Barone A, Toti P, Quaranta A, Alfonsi F, Cucchi A, Calvo-Guirado JL, Negri B, Di Felice R, Covani U (2015) Volumetric analysis of remodelling pattern after ridge preservation comparing use of two types of xenografts. A multicentre randomized clinical trial. Clin Oral Implants Res 27(11):e105–e115. https://doi.org/10.1111/clr.12572
Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L, Cardaropoli G (2012) Socket preservation using bovine bone mineral and collagen membrane: a randomized controlled clinical trial with histologic analysis. Int J Periodontics Restorative Dent 32(4):421–430
Cardaropoli G, Araujo M, Lindhe J (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol 30(9):809–818. https://doi.org/10.1034/j.1600-051X.2003.00366.x
Dahlin C, Obrecht M, Dard M, Donos N (2015) Bone tissue modelling and remodelling following guided bone regeneration in combination with biphasic calcium phosphate materials presenting different microporosity. Clin Oral Implants Res 26(7):814–822. https://doi.org/10.1111/clr.12361
Froum S, Orlowski W (2000) Ridge preservation utilizing an alloplast prior to implant placement—clinical and histological case reports. Pract Periodontics and Aesthet Dent 12:393–402 quiz 404
Froum SJ, Wallace SS, Cho SC, Elian N, Tarnow DP (2008) Histomorphometric comparison of a biphasic bone ceramic to anorganic bovine bone for sinus augmentation: 6- to 8-month postsurgical assessment of vital bone formation. A pilot study. Int J Periodontics Restorative Dent 28(3):273–281
Horowitz RA, Mazor Z, Miller RJ, Krauser J, Prasad HS, Rohrer MD (2009) Clinical evaluation alveolar ridge preservation with a beta-tricalcium phosphate socket graft. Compendium of Continuing Education in Dentistry 30:588–590 592, 594 passim; quiz 604, 606
Jensen SS, Bornstein MM, Dard M, Bosshardt DD, Buser D (2009) Comparative study of biphasic calcium phosphates with different HA/TCP ratios in mandibular bone defects. A long-term histomorphometric study in minipigs. J Biomed Mater Res Part B Appl Biomater 90(1):171–181. https://doi.org/10.1002/jbm.b.31271
Jung, R. (2017) Alveolar ridge preservation in the esthetic zone. Perio 2000 accepted
Jung RE, Philipp A, Annen BM, Signorelli L, Thoma DS, Hammerle CH, Attin T, Schmidlin P (2013) Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial. J Clin Periodontol 40(1):90–98. https://doi.org/10.1111/jcpe.12027
Kilkenny C, Browne W, Cuthill IC, Emerson M, Altman DG (2011) Animal research: reporting in vivo experiments—the ARRIVE guidelines. J Cereb Blood Flow Metab 31(4):991–993. https://doi.org/10.1038/jcbfm.2010.220
Kim JJ, Schwarz F, Song HY, Choi Y, Kang KR, Koo KT (2016) Ridge preservation of extraction sockets with chronic pathology using Bio-Oss(R) Collagen with or without collagen membrane: an experimental study in dogs. Clin Oral Implants Res 28(6):727–733. https://doi.org/10.1111/clr.12870
Lee DW, Pi SH, Lee SK, Kim EC (2009) Comparative histomorphometric analysis of extraction sockets healing implanted with bovine xenografts, irradiated cancellous allografts, and solvent-dehydrated allografts in humans. Int J Oral Maxillofac Implants 24(4):609–615
Lindhe J, Cecchinato D, Donati M, Tomasi C, Liljenberg B (2014) Ridge preservation with the use of deproteinized bovine bone mineral. Clin Oral Implants Res 25(7):786–790. https://doi.org/10.1111/clr.12170
Mardas N, Trullenque-Eriksson A, MacBeth N, Petrie A, Donos N (2015) Does ridge preservation following tooth extraction improve implant treatment outcomes: a systematic review: group 4: therapeutic concepts & methods. Clin Oral Implants Res 26(Suppl 11):180–201. https://doi.org/10.1111/clr.12639
Rothamel D, Schwarz F, Herten M, Engelhardt E, Donath K, Kuehn P, Becker J (2008) Dimensional ridge alterations following socket preservation using a nanocrystalline hydroxyapatite paste: a histomorphometrical study in dogs. Int J Oral Maxillofac Surg 37(8):741–747. https://doi.org/10.1016/j.ijom.2008.04.017
Scheyer ET, Heard R, Janakievski J, Mandelaris G, Nevins ML, Pickering SR, Richardson CR, Pope B, Toback G, Velasquez D, Nagursky H (2016) A randomized, controlled, multicentre clinical trial of post-extraction alveolar ridge preservation. J Clin Periodontol 43(12):1188–1199. https://doi.org/10.1111/jcpe.12623
Schneider D, Schmidlin PR, Philipp A, Annen BM, Ronay V, Hammerle CH, Attin T, Jung RE (2014) Labial soft tissue volume evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial. J Clin Periodontol 41(6):612–617. https://doi.org/10.1111/jcpe.12246
Schropp L, Wenzel A, Kostopoulos L, Karring T (2003) Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 23(4):313–323
Shi B, Zhou Y, Wang YN, Cheng XR (2007) Alveolar ridge preservation prior to implant placement with surgical-grade calcium sulfate and platelet-rich plasma: a pilot study in a canine model. Int J Oral Maxillofac Implants 22(4):656–665
Sisti A, Canullo L, Mottola MP, Covani U, Barone A, Botticelli D (2012) Clinical evaluation of a ridge augmentation procedure for the severely resorbed alveolar socket: multicenter randomized controlled trial, preliminary results. Clin Oral Implants Res 23(5):526–535. https://doi.org/10.1111/j.1600-0501.2011.02386.x
Spinato S, Galindo-Moreno P, Zaffe D, Bernardello F, Soardi CM (2014) Is socket healing conditioned by buccal plate thickness? A clinical and histologic study 4 months after mineralized human bone allografting. Clin Oral Implants Res 25(2):e120–e126. https://doi.org/10.1111/clr.12073
Tallgren A (1972) The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. Journal of Prosthetic Dentistry 27:120–132
Tan WL, Wong TL, Wong MC, Lang NP (2012) A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res 23 Suppl 5:1–21. https://doi.org/10.1111/j.1600-0501.2011.02375.x
Thoma DS, Jung RE, Schneider D, Cochran DL, Ender A, Jones AA, Gorlach C, Uebersax L, Graf-Hausner U, Hammerle CH (2010) Soft tissue volume augmentation by the use of collagen-based matrices: a volumetric analysis. J Clin Periodontol 37(7):659–666. https://doi.org/10.1111/j.1600-051X.2010.01581.x
Vignoletti F, Matesanz P, Rodrigo D, uero E, Martin C, Sanz M (2012) Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clin Oral Implants Res 23 Suppl 5:22–38. https://doi.org/10.1111/j.1600-0501.2011.02331.x
Acknowledgements
The authors would like to acknowledge Dr. M. Mayer, for his support in the statistical analysis of the data and the animal care team at NAMSA, Lyon, France, for assistance during surgery. The support and expertise of Dr. Lorenz Uebersax, Sunstar Suisse SA, Etoy, Switzerland, is highly appreciated. This study was funded by Sunstar Suisse SA, Etoy, Switzerland and the Clinic of Fixed and Removable Prosthodontics and Dental Material Science, Center of Dental Medicine, University of Zurich, Zurich, Switzerland.
Funding
The work was supported by Sunstar Suisse SA, Etoy, Switzerland and the Clinic of Fixed and Removable Prosthodontics and Dental Material Science, Center of Dental Medicine, University of Zurich, Zurich, Switzerland.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Naenni, N., Sapata, V., Bienz, S.P. et al. Effect of flapless ridge preservation with two different alloplastic materials in sockets with buccal dehiscence defects—volumetric and linear changes. Clin Oral Invest 22, 2187–2197 (2018). https://doi.org/10.1007/s00784-017-2309-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2309-6