Abstract
Objectives
Sprays containing fine and ultrafine particles are commonly used for optical scanning. The aim of this study was to measure the particle exposure of patient and dentist during application of scanning spray and to evaluate measures for its reduction.
Materials and methods
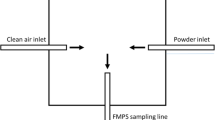
A lower molar in a dental simulator was powdered with scanning spray. Patient’s particle exposure was measured by a condensation particle counter in the nasal region of the simulator without (P) and with rubber dam (PC). Dentist’s exposure (D) was measured behind a surgical mask. Particle concentrations were determined 5-fold without suction (NS), using conventional dental suction (CDS), or high volume evacuation (HVE).
Results
Mean background air particle concentrations for the patient were 3.3 × 103 and 1.3 × 103 pt/cm3 for the dentist. Particle concentrations increased after spraying; mean cumulated additional particle exposures for the patient were the following: P-NS 7.2 × 106, P-CDS 4.6 × 106, P-HVE 2.4 × 104; using rubber dam: PC-NS 3.6 × 106, PC-CDS 3.3 × 105, PC-HVE 2.2 × 105. The particle exposures of the dentist were the following: D-NS 9.7 × 105, D-CDS 1.8 × 105, D-HVE 1.6 × 104.
Conclusions
The use of HVE is recommended to reduce exposure of patients and dental staff to fine and ultrafine particles when using scanning sprays.
Clinical relevance
Effective protection is available for staff and patient by means of high volume evacuation. In patients suffering from obstructive lung diseases, the use of scanning sprays should be avoided altogether.




Similar content being viewed by others
References
Harrel SK, Molinari J (2004) Aerosols and splatter in dentistry: a brief review of the literature and infection control implications. J Am Dent Assoc 135:429–437
Kimmerle H, Wiedmann-Al-Ahmad M, Pelz K, Wittmer A, Hellwig E, Al-Ahmad A (2012) Airborne microbes in different dental environments in comparison to a public area. Arch Oral Biol 57:689–696
Yamada H, Ishihama K, Yasuda K, Hasumi-Nakayama Y, Shimoji S, Furusawa K (2011) Aerial dispersal of blood-contaminated aerosols during dental procedures. Quintessence Int 42:399–405
Sotiriou M, Ferguson SF, Davey M, Wolfson JM, Demokritou P, Lawrence J, Sax SN, Koutrakis P (2008) Measurement of particle concentrations in a dental office. Environ Monit Assess 137:351–361
Bogdan A, Buckett MI, Japuntich DA (2014) Nano-sized aerosol classification, collection and analysis—method development using dental composite materials. J Occup Environ Hyg 11. doi: 10.1080/15459624.2013.875183
Hoffmeyer F, van Kampen V, Bruening T, Merget R (2007) Pneumokoniosen. Pneumologie 61:774–797
Ender A, Mehl A, Wolf D, Bindl A (2011) CEREC Basic Information 4.0. A clinical guide. Sirona Dental Systems GmbH in cooperation with the University of Zurich.
Leggat PA, Kedjarune U, Smith DR (2007) Occupational health problems in modern dentistry: a review. Ind Health 45:611–621
Roller M (2009) Carcinogenicity of inhaled nanoparticles. Inhal Toxicol 21:144–157
Nurkiewicz TR, Porter DW, Hubbs AF, Stone S, Moseley AM, Cumpston JL, Goodwill AG, Frisbee SJ, Perrotta PL, Brock RW, Frisbee JC, Boegehold MA, Frazer DG, Chen BT (2011) Castranova V; HEI Health Review Committee (2011) Pulmonary particulate matter and systemic microvascular dysfunction. Res Rep Health Eff Inst 164:3–48
Hussain S, Vanoirbeek JA, Luyts K, De Vooght V, Verbeken E, Thomassen LC, Martens JA, Dinsdale D, Boland S, Marano F, Nemery B, Hoet PH (2011) Lung exposure to nanoparticles modulates an asthmatic response in a mouse model. Eur Respir J 37:299–309
Osman IF, Jacob BK, Anderson D (2011) Effect of nanoparticles on human cells from healthy individuals and patients with respiratory diseases. J Biomed Nanotechnol 7:26–27
McKinney W, Jackson M, Sager TM, Reynolds JS, Chen BT, Afshari A, Krajnak K, Waugh S, Johnson C, Mercer RR, Frazer DG, Thomas TA, Castranova V (2012) Pulmonary and cardiovascular responses of rats to inhalation of a commercial antimicrobial spray containing titanium dioxide nanoparticles. Inhal Toxicol 24:447–457
Scarino A, Noël A, Renzi PM, Cloutier Y, Vincent R, Truchon G, Tardif R, Charbonneau M (2012) Impact of emerging pollutants on pulmonary inflammation in asthmatic rats: ethanol vapors and agglomerated TiO(2) nanoparticles. Inhal Toxicol 24:528–538
Sun Q, Tan D, Zhou Q, Liu X, Cheng Z, Liu G, Zhu M, Sang X, Gui S, Cheng J, Hu R, Tang M, Hong F (2012) Oxidative damage of lung and its protective mechanism in mice caused by long-term exposure to titanium dioxide nanoparticles. J Biomed Mater Res A. doi:10.1002/jbm.a.34190
Naya M, Kobayashi N, Ema M, Kasamoto S, Fukumuro M, Takami S, Nakajima M, Hayashi M, Nakanishi J (2012) In vivo genotoxicity study of titanium dioxide nanoparticles using comet assay following intratracheal instillation in rats. Regul Toxicol Pharmacol 62:1–6
Scherbart AM, Langer J, Bushmelev A, van Berlo D, Haberzettl P, van Schooten FJ, Schmidt AM, Rose CR, Schins RP, Albrecht C (2011) Contrasting macrophage activation by fine and ultrafine titanium dioxide particles is associated with different uptake mechanisms. Part Fibre Toxicol 8:31
Akbar-Khanzadeh F, Milz S, Ames A, Susi PP, Bisesi M, Khuder SA, Akbar-Khanzadeh M (2007) Crystalline silica dust and respirable particulate matter during indoor concrete grinding—wet grinding and ventilated grinding compared with uncontrolled conventional grinding. J Occup Environ Hyg 10:770–779
Thomas MV, Jarboe G, Frazer RQ (2008) Infection control in the dental office. Dent Clin N Am 52:609–628
Jacks ME (2002) A laboratory comparison of evacuation devices on aerosol reduction. J Dent Hyg 76:202–206
Pingarrón Martín L, Morán Soto MJ, Sánchez Burgos R, Burgueño García M (2010) Bronchial impaction of an implant screwdriver after accidental aspiration: report of a case and revision of the literature. Oral Maxillofac Surg 14:43–47
Mörmann WH (2006) The evolution of the CEREC system. J Am Dent Assoc 137:7S–13S
Logozzo S, Franceschini G, Kilpelä A, Caponi M, Governi L, Blois L (2011) A comparative analysis of intraoral 3D digital scanners for restorative dentistry. Internet J Med Technol 5. doi:10.5580/1b90
Timmerman MF, Menso L, Steinfort J, van Winkelhoff AJ, van der Weijden GA (2004) Atmospheric contamination during ultrasonic scaling. J Clin Periodontol 31:458–462
Yuzbasioglu E, Kurt H, Turunc R, Bilir H (2014) Comparison of digital and conventional impression techniques: evaluation of patients’ perception, treatment comfort, effectiveness and clinical outcomes. BMC Oral Health 10. doi: 10.1186/1472-6831-14-10.
Tang M, Zhang T, Xue Y, Wang S, Huang M, Yang Y, Lu M, Lei H, Kong L, Yuepu P (2010) Dose dependent in vivo metabolic characteristics of titanium dioxide nanoparticles. J Nanosci Nanotechnol 12:8575–8583
Andersson PO, Lejon C, Ekstrand-Hammarström B, Akfur C, Ahlinder L, Bucht A, Osterlund L (2011) Polymorph- and size-dependent uptake and toxicity of TiO2 nanoparticles in living lung epithelial cells. Small 7:514–523
Wan R, Mo Y, Feng L, Chien S, Tollerud DJ, Zhang Q (2012) DNA Damage caused by metal nanoparticles: involvement of oxidative stress and activation of ATM. Chem Res Toxicol 25:1402–1411
Zhang XQ, Yin LH, Tang M, Pu YP (2011) ZnO, TiO(2), SiO(2,) and Al(2)O(3) nanoparticles-induced toxic effects on human fetal lung fibroblasts. Biomed Environ Sci 6:661–669
Belade E, Armand L, Martinon L, Kheuang L, Fleury-Feith J, Baeza-Squiban A, Lanone S, Billon-Galland MA, Pairon JC, Boczkowski J (2012) A comparative transmission electron microscopy study of titanium dioxide and carbon black nanoparticles uptake in human lung epithelial and fibroblast cell lines. Toxicol in Vitro 26:57–66
Leung CC, Yu IT, Chen W (2012) Silicosis. Lancet 379:2008–2018
Marchiori E, Lourenço S, Gasparetto TD, Zanetti G, Mano CM, Nobre LF (2010) Pulmonary talcosis: imaging findings. Lung 188:165–171
Iavicoli I, Leso V, Fontana L, Bergamaschi A (2011) Toxicological effects of titanium dioxide nanoparticles: a review of in vitro mammalian studies. Eur Rev Med Pharmacol Sci 15:481–508
Acknowledgments
Institutional funding was used for this study. We thank Mr. Rudolf Jung and Mr. Norbert Pütz for technical assistance and Ms. Dr. Melanie Chapat and Ms. Anja Niemeyer-Rupf for critical reading of the manuscript.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rupf, S., Berger, H., Buchter, A. et al. Exposure of patient and dental staff to fine and ultrafine particles from scanning spray. Clin Oral Invest 19, 823–830 (2015). https://doi.org/10.1007/s00784-014-1300-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-014-1300-8