Abstract
Background
The optimal management of asymptomatic, petroclival meningiomas remains incompletely defined. The purpose of this study was to evaluate the safety and efficacy of upfront stereotactic radiosurgery (SRS) for patients with asymptomatic, petroclival region meningiomas.
Methods
This retrospective, international, multicenter study involved patients treated with SRS for an asymptomatic, petroclival region meningioma. Study endpoints included local tumor control rate, procedural complications, and the emergence of new neurological deficits.
Results
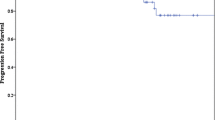
There were 72 patients (22 males, mean age 59.53 years (SD ± 11.9)) with an asymptomatic meningioma located in the petroclival region who were treated with upfront SRS. Mean margin dose and maximum dose were 13.26 (SD ± 2.72) Gy and 26.14 (SD ± 6.75) Gy respectively. Median radiological and clinical follow-up periods post-SRS were 52.5 (IQR 61.75) and 47.5 months (IQR 69.75) respectively. At last follow-up, tumor control was achieved in all patients. SRS-related complications occurred in 6 (8.33%) patients, with 3 of them (4.17%) exhibiting new neurological deficits.
Conclusions
Upfront SRS for asymptomatic, petroclival region meningiomas affords excellent local tumor control and does so with a relatively low risk of SRS-related complications. SRS can be considered at diagnosis of an asymptomatic petroclival region meningioma. If active surveillance is initially chosen, SRS should be recommended when growth is noted during radiological follow-up.

Similar content being viewed by others
References
Almefty R, Dunn IF, Pravdenkova S, Abolfotoh M, Al-Mefty O (2014) True petroclival meningiomas: results of surgical management. J Neurosurg 120(1):40–51
Barnett GH, Linskey ME, Adler JR, Cozzens JW, Friedman WA, Heilbrun MP, Lunsford LD, Schulder M, Sloan AE (2007) Stereotactic radiosurgery—an organized neurosurgery-sanctioned definition. J Neurosurg 106(1):1–5
Bunevicius A, Tamasauskas S, Deltuva V, Tamasauskas A, Radziunas A, Bunevicius R (2014) Predictors of health-related quality of life in neurosurgical brain tumor patients: focus on patient-centered perspective. Acta Neurochir 156(2):367–374
Bunevicius A, Pikis S, Schlesinger D, Sheehan J (2021) Editorial: radiosurgical induced malignancy associated with stereotactic radiosurgery. Acta Neurochir 163(4):969–970
Flannery TJ, Kano H, Lunsford LD, Sirin S, Tormenti M, Niranjan A, Flickinger JC, Kondziolka D (2010) Long-term control of petroclival meningiomas through radiosurgery. J Neurosurg 112(5):957–964
Giammattei L, di Russo P, Starnoni D, Passeri T, Bruneau M, Meling TR, Berhouma M, Cossu G, Cornelius JF, Paraskevopoulos D, Zazpe I, Jouanneau E, Cavallo LM, Benes V, Seifert V, Tatagiba M, Schroeder HWS, Goto T, Ohata K, Al-Mefty O, Fukushima T, Messerer M, Daniel RT, Froelich S (2021) Petroclival meningiomas: update of current treatment and consensus by the EANS skull base section. Acta Neurochir 163(6):1639–1663
Huang RY, Bi WL, Weller M, Kaley T, Blakeley J, Dunn I, Galanis E, Preusser M, McDermott M, Rogers L, Raizer J, Schiff D, Soffietti R, Tonn JC, Vogelbaum M, Weber D, Reardon DA, Wen PY (2019) Proposed response assessment and endpoints for meningioma clinical trials: report from the Response Assessment in Neuro-Oncology Working Group. Neuro Oncol 21(1):26–36
Hunter JB, Yawn RJ, Wang R, O’Connell BP, Carlson ML, Mistry A, Haynes DS, Thompson RC, Weaver KD, Wanna GB (2017) The natural history of petroclival meningiomas: a volumetric study. Otol Neurotol 38(1):123–128
Jung H-W, Yoo H, Paek SH, Choi KS (2000) Long-term outcome and growth rate of subtotally resected petroclival meningiomas: experience with 38 cases. Neurosurgery 46(3):567–575
Kim JW, Jung H-W, Kim YH, Park C-K, Chung H-T, Paek SH, Kim DG, Lee SH (2019) Petroclival meningiomas: long-term outcomes of multimodal treatments and management strategies based on 30 years of experience at a single institution. J Neurosurg 132(6):1675–1682
Pikis S, Bunevicius A, Sheehan J (2021) Outcomes from treatment of asymptomatic skull base meningioma with stereotactic radiosurgery. Acta Neurochir 163(1):83–88
Pollock BE, Stafford SL, Utter A, Giannini C, Schreiner SA (2003) Stereotactic radiosurgery provides equivalent tumor control to Simpson Grade 1 resection for patients with small- to medium-size meningiomas. Int J Radiat Oncol Biol Phys 55(4):1000–1005
Rowe J, Grainger A, Walton L, Silcocks P, Radatz M, Kemeny A (2007) Risk of malignancy after gamma knife stereotactic radiosurgery. Neurosurgery 60(1):60–66
Sheehan J, Pikis S, Islim A, Chen CJ, Bunevicius A, Peker S, Samanci Y, Nabeel AM, Reda WA, Tawadros SR, El-Shehaby AMN, Abdelkarim K, Emad RM, Delabar V, Mathieu D, Lee CC, Yang HC, Liscak R, Hanuska J, Alvarez RM, Patel D, Kondziolka D, Moreno NM, Tripathi M, Speckter H, Albert C, Bowden GN, Benveniste RJ, Lunsford LD, Jenkinson MD (2021) An international multicenter matched cohort analysis of incidental meningioma progression during active surveillance or after stereotactic radiosurgery: the IMPASSE study. Neuro Oncol. https://doi.org/10.1093/neuonc/noab132
Starke R, Kano H, Ding D, Nakaji P, Barnett GH, Mathieu D, Chiang V, Yu JB, Hess J, McBride HL, Honea N, Lee JY, Rahmathulla G, Evanoff WA, Alonso-Basanta M, Lunsford LD, Sheehan JP (2014) Stereotactic radiosurgery of petroclival meningiomas: a multicenter study. J Neurooncol 119(1):169–176
Sughrue ME, Rutkowski MJ, Aranda D, Barani IJ, McDermott MW, Parsa AT (2010) Treatment decision making based on the published natural history and growth rate of small meningiomas: a review and meta-analysis. J Neurosurg 113(5):1036–1042
Van Havenbergh T, Carvalho G, Tatagiba M, Plets C, Samii M (2003) Natural history of petroclival meningiomas. Neurosurgery 52(1):55–64
Wayhs SY, Lepski GA, Frighetto L, Isolan GR (2017) Petroclival meningiomas: remaining controversies in light of minimally invasive approaches. Clin Neurol Neurosurg 152:68–75
Wolf A, Naylor K, Tam M, Habibi A, Novotny J, Liščák R, Martinez-Moreno N, Martinez-Alvarez R, Sisterson N, Golfinos JG, Silverman J, Kano H, Sheehan J, Lunsford LD, Kondziolka D (2019) Risk of radiation-associated intracranial malignancy after stereotactic radiosurgery: a retrospective, multicentre, cohort study. Lancet Oncol 20(1):159–164
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Conflict of interest
L. Dade Lunsford is a shareholder in Elekta AB, the manufacturer of some radiosurgical devices. All other authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Comments
This paper is by a group of experts of SRS and is a timely and important contribution to the pre-existing literature. For many years the dogma was to propose proactive neurosurgical management of meningiomas only in symptomatic patients with growth demonstration. In skull base meningiomas and specially those of the petroclival region (PCM) this attitude was completely justified by the significant risk of morbimortality and the high risk of uncomplete resection carried by microsurgical removal in this difficult anatomical area, even in the best hands (1). The achievement of radiosurgery came along (SRS) this strategy was, by default, applied to SRS. However in small middle size PCM SRS has demonstrated a very low rate of morbidity with no mortality and a high rate of tumor control (2) comparable to the one provided by complete tumor resection including the surrounding dura and bone (3). However, the best safety efficacy is obtained with the smaller tumors in SRS. Thus, numerous neurosurgeons have started to propose upfront radiosurgery in asymptomatic MPC, even in absence of growth demonstration, in order to give to the patient the higher probability of long term tumor control with the lowest risk.
The manuscript is putting under the magnifying glass a subset of patients of an earlier publication on upfront radiosurgery for meningiomas, with a patient selection completely different from the one of the papers (4,5).
This paper shows that upfront SRS in asymptomatic is a safe and efficient option in small and middle size Petroclival Meningiomas and is strongly advocating for upfront SRS in PCM without proof of growth.
Jean-Paul Regis
Marseille, France
This article is part of the Topical Collection on Tumor—Meningioma
Rights and permissions
About this article
Cite this article
Mantziaris, G., Pikis, S., Bunevicius, A. et al. Stereotactic radiosurgery for asymptomatic petroclival region meningiomas: a focused analysis from the IMPASSE study. Acta Neurochir 164, 273–279 (2022). https://doi.org/10.1007/s00701-021-05056-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-021-05056-y