Abstract
Background
The predictive value of short-term arm pain relief after ‘indirect’ cervical epidural steroid injection (ESI) for the 1-month treatment response has been previously demonstrated. It remained to be answered whether the long-term response could be estimated by the early post-interventional pain course as well.
Methods
Prospective observational study, following a cohort of n = 45 patients for a period of 24 months after ‘indirect’ ESI for radiculopathy secondary to a single-level cervical disk herniation (CDH). Arm and neck pain on the visual analog scale (VAS), health-related quality of life with the Short Form-12 (SF-12), and functional outcome with the Neck Pain and Disability (NPAD) Scale were assessed. Any additional invasive treatment after a single injection (second injection or surgery) defined treatment outcome as ‘non-response’.
Results
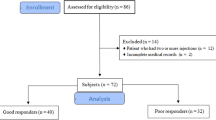
At 24 months, n = 30 (66.7%) patients were responders and n = 15 (33.3%) were non-responders. Non-responders exited the follow-up at 1 month (n = 10), at 3 months (n = 4), and at 6 months (n = 1). No patients were injected again or operated on between the 6- and 24-month follow-up. Patients with favorable treatment response at 24 months had significantly lower VAS arm pain (p < 0.05) than non-responders at days 6, 8–11, and at the 3-month follow-up. The previously defined cut-off of > 50% short term pain reduction was not a reliable predictor of the 24-month responder status. SF-12 and NPAD scores were better among treatment responders in the long term.
Conclusions
Patients who require a second injection or surgery after ‘indirect’ cervical ESI for a symptomatic CDH do so within the first 6 months. Short-term pain relief cannot reliably predict the long-term outcome.



Similar content being viewed by others
References
Brandle K, Stienen MN, Neff A, Hildebrandt G, Joswig H (2016) Ten-day response to CT-guided spinal infiltration therapy in more than a thousand patients. J Neurol Surg A Cent Eur Neurosurg 77:181–194
Bush K, Chaudhuri R, Hillier S, Penny J (1997) The pathomorphologic changes that accompany the resolution of cervical radiculopathy. A prospective study with repeat magnetic resonance imaging. Spine (Phila Pa 1976) 22:183–186 discussion 187
Copay AG, Glassman SD, Subach BR, Berven S, Schuler TC, Carreon LY (2008) Minimum clinically important difference in lumbar spine surgery patients: a choice of methods using the Oswestry disability index, medical outcomes study questionnaire short form 36, and pain scales. Spine J 8:968–974
Corniola MV, Stienen MN, Joswig H, Smoll NR, Schaller K, Hildebrandt G, Gautschi OP (2016) Correlation of pain, functional impairment, and health-related quality of life with radiological grading scales of lumbar degenerative disc disease. Acta Neurochir 158:499–505
Cyteval C, Thomas E, Decoux E, Sarrabere MP, Cottin A, Blotman F, Taourel P (2004) Cervical radiculopathy: open study on percutaneous periradicular foraminal steroid infiltration performed under CT control in 30 patients. AJNR Am J Neuroradiol 25:441–445
Desai A, Saha S, Sharma N, Huckerby L, Houghton R (2014) The short- and medium-term effectiveness of CT-guided selective cervical nerve root injection for pain and disability. Skelet Radiol 43:973–978
Desai K, Spikings E, Zhang T (2015) Short-term chilled storage of zebrafish (Danio rerio) embryos in cryoprotectant as an alternative to cryopreservation. Zebrafish 12:111–120
Fish DE, Kobayashi HW, Chang TL, Pham Q (2009) MRI prediction of therapeutic response to epidural steroid injection in patients with cervical radiculopathy. Am J Phys Med Rehabil 88:239–246
Gautschi OP, Stienen MN, Corniola MV, Joswig H, Schaller K, Hildebrandt G, Smoll NR (2017) Assessment of the minimum clinically important difference in the timed up and go test after surgery for lumbar degenerative disc disease. Neurosurgery 80:380–385
Gautschi OP, Stienen MN, Joswig H, Smoll NR, Schaller K, Corniola MV (2017) The usefulness of radiological grading scales to predict pain intensity, functional impairment, and health-related quality of life after surgery for lumbar degenerative disc disease. Acta Neurochir 159:271–279
Ghahreman A, Bogduk N (2011) Predictors of a favorable response to transforaminal injection of steroids in patients with lumbar radicular pain due to disc herniation. Pain Med 12:871–879
International Standard Classification of Occupations (ISCO). http://www.ilo.org/public/english/bureau/stat/isco/ Accessed February 3, 2018
Joswig H, Neff A, Ruppert C, Hildebrandt G, Stienen MN (2016) The value of short-term pain relief in predicting the one-month outcome of lumbar Transforaminal epidural steroid injections. World Neurosurg 96:323–333
Joswig H, Neff A, Ruppert C, Hildebrandt G, Stienen MN (2017) The value of short-term pain relief in predicting the 1-month outcome of 'indirect' cervical epidural steroid injections. Acta Neurochir 159:291–300
Joswig H, Neff A, Ruppert C, Hildebrandt G, Stienen MN (2017) The value of short-term pain relief in predicting the long-term outcome of lumbar Transforaminal epidural steroid injections. World Neurosurg 107:764–771
Klessinger S, Freund W, Karpel-Massler G, Halatsch ME (2014) Response to transforaminal injection of steroids and correlation to mri findings in patients with cervical radicular pain or radiculopathy due to disc herniation or spondylosis. Pain Med 15:929–937
Kolstad F, Leivseth G, Nygaard OP (2005) Transforaminal steroid injections in the treatment of cervical radiculopathy. A prospective outcome study. Acta Neurochir (Wien) 147:1065–1070 discussion 1070
Kwon JW, Lee JW, Kim SH, Choi JY, Yeom JS, Kim HJ, Kwack KS, Moon SG, Jun WS, Kang HS (2007) Cervical interlaminar epidural steroid injection for neck pain and cervical radiculopathy: effect and prognostic factors. Skelet Radiol 36:431–436
Lee JW, Park KW, Chung SK, Yeom JS, Kim KJ, Kim HJ, Kang HS (2009) Cervical transforaminal epidural steroid injection for the management of cervical radiculopathy: a comparative study of particulate versus non-particulate steroids. Skelet Radiol 38:1077–1082
Lee SH, Kim KT, Kim DH, Lee BJ, Son ES, Kwack YH (2012) Clinical outcomes of cervical radiculopathy following epidural steroid injection: a prospective study with follow-up for more than 2 years. Spine (Phila Pa 1976) 37:1041–1047
Scherer M, Blozik E, Himmel W, Laptinskaya D, Kochen MM, Herrmann-Lingen C (2008) Psychometric properties of a German version of the neck pain and disability scale. Eur Spine J 17:922–929
Strobel K, Pfirrmann CW, Schmid M, Hodler J, Boos N, Zanetti M (2004) Cervical nerve root blocks: indications and role of MR imaging. Radiology 233:87–92
Sutter R, Pfirrmann CW, Zanetti M, Hodler J, Peterson CK (2011) CT-guided cervical nerve root injections: comparing the immediate post-injection anesthetic-related effects of the transforaminal injection with a new indirect technique. Skelet Radiol 40:1603–1608
Vallee JN, Feydy A, Carlier RY, Mutschler C, Mompoint D, Vallee CA (2001) Chronic cervical radiculopathy: lateral-approach periradicular corticosteroid injection. Radiology 218:886–892
Wald JT, Maus TP, Geske JR, Diehn FE, Kaufmann TJ, Murthy NS, Thielen KR, Watson S (2013) Immediate pain response does not predict long-term outcome of CT-guided cervical transforaminal epidural steroid injections. AJNR Am J Neuroradiol 34:1665–1668
Acknowledgements
The authors thank their study nurse, Cornelia Lüthi, for her outstanding diligence in pursuing follow-up. The authors thank Jessica Reid and Meagan MacArthur for proof-reading the manuscript.
Funding
No funding was received for this study. Expenditures (questionnaires, study nurse) were financed by the Department of Neurosurgery at Cantonal Hospital St. Gallen.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Compliance with ethical standards
Written informed consent was obtained from all included patients. The study was conducted in accordance with the ethical standards of the Cantonal Ethical Review Board St. Gallen, Switzerland (EKSG 13/061) with the Helsinki Declaration (1964, amended most recently in 2008) of the World Medical Association and registered under clinicaltrials.gov (Identifier: NCT01945554).
Conflict of interest
Dr. Holger Joswig receives speaker honoraria from UCB Canada and travel grants from Medtronic. All other authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
The study was conducted in accordance with the ethical standards of the Cantonal Ethical Review Board St. Gallen, Switzerland (EKSG 13/061) and with the Helsinki Declaration (1964, amended most recently in 2008) of the World Medical Association.
Informed consent
Written informed consent was obtained from all included patients.
Rights and permissions
About this article
Cite this article
Joswig, H., Neff, A., Ruppert, C. et al. The value of short-term pain relief in predicting the long-term outcome of ‘indirect’ cervical epidural steroid injections. Acta Neurochir 160, 935–943 (2018). https://doi.org/10.1007/s00701-018-3511-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-018-3511-2