Abstract
Background
Ventricular pneumocephalus is a rare but potentially life-threatening complication of cranial surgery in the sitting position.
Objective
The objective of the study is to assess the incidence and risk factors of postoperative ventricular pneumocephalus.
Methods
We performed a retrospective chart review of 307 consecutive patients (147 men, 160 women) treated at our institution by intracranial surgery in the sitting position from January 2010 to October 2014. Ventricular air entrapment with lack of arousal or neurologic deterioration requiring external ventriculostomy (EVD) was defined as ventricular tension pneumocephalus (VTP). Demographic variables were recorded along with radiological and clinical data. The occurrence of pneumocephalus was correlated with patient-related and surgical variables.
Results
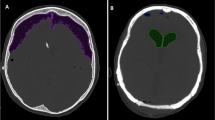
VTP was observed in 12 cases (3.9%). These patients had higher intraventricular air volumes (48.5 cm3 (CI 95% [29.06–67.86])) compared to asymptomatic patients (7.4 cm3 (CI 95% [5.43–9.48])). Opening of the fourth ventricle was the most potent predictor of VTP (OR = 34.7, CI 95% [4.4–273.5], p = 0.001). In patients undergoing no additional treatment for pneumocephalus, ventricular air volume declined to an average of 41.7% of the initial postoperative volume on postoperative day 3.
Conclusions
Entrapment of intracranial and particularly ventricular air requiring emergent EVD occurred in 3.9% cases of intracranial surgery in the sitting position. Especially the opening of the fourth ventricle was associated with the development of VTP, which should warrant particularly diligent postoperative observation of these patients. In cases without neurological symptoms, the rate of spontaneous air resorption is sufficiently high to warrant expectant management.




Similar content being viewed by others
References
Aydoseli A, Akcakaya MO, Aras Y, Boyali O, Unal OF (2013) Emergency management of an acute tension pneumocephalus following ventriculoperitoneal shunt surgery for normal pressure hydrocephalus. Turk Neurosurg 23(4):564–567
Banu MA, Szentirmai O, Mascarenhas L, Salek AA, Anand VK, Schwartz TH (2014) Pneumocephalus patterns following endonasal endoscopic skull base surgery as predictors of postoperative CSF leaks. J Neurosurg 121(4):961–975
Beseoglu K, Lodes S, Stummer W, Steiger HJ, Hänggi D (2011) The transorbital keyhole approach: early and long-term outcome analysis of approach-related morbidity and cosmetic results. Technical note. J Neurosurg 114(3):852–856. https://doi.org/10.3171/2010.9.JNS1095
Blount A, Riley K, Cure J, Woodworth BA (2012) Cerebrospinal fluid volume replacement following large endoscopic anterior cranial base resection. Int Forum Allergy Rhinol 2(3):217–221
Chandler JP, Pelzer HJ, Bendok BB, Hunt Batjer H, Salehi SA (2005) Advances in surgical management of malignancies of the cranial base: the extended transbasal approach. J Neuro-Oncol 73(2):145–152
Coffey CE, Lucke JF, Saxton JA, Ratcliff G, Unitas LJ, Billig B, Bryan RN (1998) Sex differences in brain aging: a quantitative magnetic resonance imaging study. Arch Neurol 55(2):169–179
Daszkiewicz P, Dziedzic D (2017) Tension pneumocephalus following suboccipital sitting craniotomy in the pediatric population. Neurol Neurochir Pol 51(4):286–289
Dexter F, Reasoner DK (1996) Theoretical assessment of normobaric oxygen therapy to treat pneumocephalus. Anesthesiology 84(2):442–447
Di Lorenzo N, Caruso R, Floris R, Guerrisi V, Bozzao L, Fortuna A (1986) Pneumocephalus and tension pneumocephalus after posterior fossa surgery in the sitting position: a prospective study. Acta Neurochir 83(3–4):112–115
Domaingue CM (2005) Anaesthesia for neurosurgery in the sitting position: a practical approach. Anaesth Intensive Care 33(3):323–331
Dudoit T, Labeyrie PE, Deryckere S, Emery E, Gaberel T (2016) Is systematic post-operative CT scan indicated after chronic subdural hematoma surgery? A case-control study. Acta Neurochir 158(7):1241–1246. https://doi.org/10.1007/s00701-016-2820-6
Fathi A-R, Eshtehardi P, Meier B (2009) Patent foramen ovale and neurosurgery in sitting position: a systematic review. Br J Anaesth 102(5):588–596
Gore PA, Maan H, Chang S, Pitt AM, Spetzler RF, Nakaji P (2008) Normobaric oxygen therapy strategies in the treatment of postcraniotomy pneumocephalus. J Neurosurg 108(5):926–929
Greenberg MS (2016) Handbook of Neurosurgery. Thieme
Gur RC, Mozley PD, Resnick SM, Gottlieb GL, Kohn M, Zimmerman R, Herman G, Atlas S, Grossman R, Berretta D (1991) Gender differences in age effect on brain atrophy measured by magnetic resonance imaging. Proc Natl Acad Sci U S A 88(7):2845–2849
Haran RP, Chandy MJ (1997) Symptomatic pneumocephalus after transsphenoidal surgery. Surg Neurol 48(6):575–578
Harris AE, Hadjipanayis CG, Lunsford LD, Lunsford AK, Kassam AB (2008) Microsurgical removal of intraventricular lesions using endoscopic visualization and stereotactic guidance. Neurosurgery 62(Suppl 2):622–629
Hernández-Palazón J, Martínez-Lage JF, de la Rosa-Carrillo VN, Tortosa JA, López F, Poza M (2003) Anesthetic technique and development of pneumocephalus after posterior fossa surgery in the sitting position. Neurocir Astur Spain 14(3):216–221
Himes BT, Mallory GW, Abcejo AS et al (2017) Contemporary analysis of the intraoperative and perioperative complications of neurosurgical procedures performed in the sitting position. J Neurosurg 127(1):182–188
Hong B, Biertz F, Raab P et al (2015) Normobaric hyperoxia for treatment of pneumocephalus after posterior fossa surgery in the semisitting position: a prospective randomized controlled trial. PLoS One 10(5):e0125710
Ihab Z (2012) Pneumocephalus after surgical evacuation of chronic subdural hematoma: is it a serious complication? Asian J Neurosurg 7(2):66–74. https://doi.org/10.4103/1793-5482.98647
Kryzanski JT et al (2008) Low complication rates of cranial and craniofacial approaches to midline anterior skull base lesions. Skull Base
Kuba H, Matsukado K, Inamura T, Morioka T, Sasaki M, Fukui M (2000) Pneumocephalus associated with aqueductal stenosis: three-dimensional computed tomographic demonstration of skull-base defects. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 16(1):1–3
Kumar R, Singh S (2005) Childhood choroid plexus papillomas: operative complications. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 21(2):138–143
Leslie K, Hui R, Kaye AH (2006) Venous air embolism and the sitting position: a case series. J Clin Neurosci Off J Neurosurg Soc Australas 13(4):419–422
Lunsford LD, Maroon JC, Sheptak PE, Albin MS (1979) Subdural tension pneumocephalus. Report of two cases. J Neurosurg 50(4):525–527
Maduri R, Daniel R-T, Diezi M, Cotting J, Messerer M (2016) Paraplegia after posterior fossa surgery in prone position: can we prevent it? Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg. https://doi.org/10.1007/s00381-016-3314-9
Menon G, Nair SN, Baldawa SS, Rao RB, Krishnakumar KP, Gopalakrishnan CV (2010) Choroid plexus tumors: an institutional series of 25 patients. Neurol India 58(3):429–435. https://doi.org/10.4103/0028-3886.66455
Nazzaro JM, Lyons KE, Honea RA, Mayo MS, Cook-Wiens G, Harsha A et al (2010) Head positioning and risk of pneumocephalus, air embolism, and hemorrhage during subthalamic deep brain stimulation surgery. Acta Neurochir 152:2047–2052
Paiva WS, de Andrade AF, Figueiredo EG, Amorim RL, Prudente M, Teixeira MJ (2014) Effects of hyperbaric oxygenation therapy on symptomatic pneumocephalus. Ther Clin Risk Manag 10:769–773
Porter JM, Pidgeon C, Cunningham AJ (1999) The sitting position in neurosurgery: a critical appraisal. Br J Anaesth 82(1):117–128
Reasoner DK, Todd MM, Scamman FL, Warner DS (1994) The incidence of pneumocephalus after supratentorial craniotomy. Observations on the disappearance of intracranial air. Anesthesiology 80(5):1008–1012
Samii M, Matthies C (1997) Management of 1000 vestibular schwannomas (acoustic neuromas): surgical management and results with an emphasis on complications and how to avoid them. Neurosurgery 40(1):11–21 discussion 21-23
Senior BA, Ebert CS, Bednarski KK, Bassim MK, Younes M, Sigounas D, Ewend MG (2008) Minimally invasive pituitary surgery. Laryngoscope 118(10):1842–1855. https://doi.org/10.1097/MLG.0b013e31817e2c43
Sharim J, Pezeshkian P, DeSalles A, Pouratian N (2015) Effect of cranial window diameter during deep brain stimulation surgery on volume of Pneumocephalus. Neuromodulation 18(7):574–578. https://doi.org/10.1111/ner.12328 discussion 578-9
Sloan T (2010) The incidence, volume, absorption, and timing of supratentorial pneumocephalus during posterior fossa neurosurgery conducted in the sitting position. J Neurosurg Anesthesiol 22(1):59–66
Solomiichuk VO, Lebed VO, Drizhdov KI (2013) Posttraumatic delayed subdural tension pneumocephalus. Surg Neurol Int 4:37
Suri A, Mahapatra AK, Singh VP (2000) Posterior fossa tension pneumocephalus. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 16(4):196–199
Toung T, Donham RT, Lehner A, Alano J, Campbell J (1983) Tension pneumocephalus after posterior fossa craniotomy: report of four additional cases and review of postoperative pneumocephalus. Neurosurgery 12(2):164–168
Toung TJ, McPherson RW, Ahn H, Donham RT, Alano J, Long D (1986) Pneumocephalus: effects of patient position on the incidence and location of aerocele after posterior fossa and upper cervical cord surgery. Anesth Analg 65(1):65–70
Xu F, Tang Z, Luo X, Kang H, Zhu W, Wang G, Xu K, Lian L, Zhu S (2014) Pneumocephalus following the minimally invasive hematoma aspiration and thrombolysis for ICH. Br J Neurosurg 28(6):776–781. https://doi.org/10.3109/02688697.2014.920486
Yates H, Hamill M, Borel CO, Toung TJ (1994) Incidence and perioperative management of tension pneumocephalus following craniofacial resection. J Neurosurg Anesthesiol 6(1):15–20
(1999) Literature review. J Clin Neurosci Off J Neurosurg Soc Australas 6(5):420–424
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None
The sponsor had no role in the design or conduct of this research.
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (name of institute/committee) and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Sachkova, A., Schemmerling, T., Goldberg, M. et al. Predictors of ventricular tension pneumocephalus after posterior fossa surgery in the sitting position. Acta Neurochir 160, 525–538 (2018). https://doi.org/10.1007/s00701-017-3444-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3444-1