Abstract
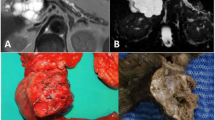
We report a case of serous cystadenoma of pancreas causing left-sided portal hypertension and gastric varices. A 68-year-old man was admitted for treatment of a pancreatic body tumor. Contrast-enhanced computed tomography (CT) showed a honeycombed cystic mass. A celiac angiogram showed a hypervascular tumor supplied mainly by a dilated splenic artery and dorsal pancreatic artery. In the venous phase, the patent splenic vein had a large hepatopetal collateral vein via the coronary gastric vein. Upper gastrointestinal endoscopy showed isolated varices of the gastric fundus. We made a preoperative diagnosis of a serous cystic tumor of the pancreas with left-sided portal hypertension and performed distal pancreatectomy with splenectomy. The resected tumor was 8 cm in diameter and had a typical honeycombed microcystic pattern with central stellate scarring. The spleen was not enlarged. Histopathological examination confirmed a diagnosis of serous cystadenoma without any sign of malignancy. Postoperative endoscopy showed disappearance of the gastric varices.
Similar content being viewed by others
References
Compagno J, Oertel JE. Microcystic adenomas of the pancreas (glycogen-rich cystadenomas). A clinicopathologic study of 34 cases. Am J Clin Pathol 1978;69:289–298.
George DH, Murphy F, Michalski R, Ulmer BG. Serous cystadenoma of the pancreas: a new entity? Am J Surg Pathol 1989;13: 61–66.
Kamei K, Funabiki T, Ochiai M, Amano H, Kasahara M, Sakamoto T. Multifocal pancreatic serous cystadenoma with atypical cells and focal perineural invasion. Int J Pancreatol 1992;10:161–172.
Yoshimi N, Sugie S, Tanaka T, Aijin W, Bunai Y, Tatematsu A, et al. A rare case of cystadenocarcinoma of the pancreas. Cancer 1992;69:2449–2453.
Abe H, Kubota K, Mori M, Miki K, Minagawa M, Noie T, et al. Serous cystadenoma of the pancreas with invasive growth: benign or malignant? Am J Gastroenterol 1998;93:1963–1966.
Widmaier U, Mattfeld T, Siech M, Berger HG. Serous cystadenocarcinoma of the pancreas. Int J Pancreatol 1996;20:135–138.
Ishikawa T, Nakao A, Nomato S, Hosono J, Harada A, Nonami T, et al. Immunohistochemical and molecular biological studies of serous cystadenoma of the pancreas. Pancreas 1998;16:40–44.
Eriguchi N, Aoyagi S, Nakayama T. Serous cystadenoma of the pancreas with liver metastasis. J Hepatobiliary Pancreat Surg 1998;5:467–470.
Ohta T, Nakakawa T, Itoh H, Fonseca L, Miyazaki I, Terada T. A case of serous cystadenoma of the pancreas with focal malignant changes. Int J Pancreatol 1993;14:283–289.
Formentini A, Birk D, Siech M. Serous cystadenocarcinoma of the pancreas and serous cystadenoma associated with ductal pancreatic adenocarcinoma. HPB Surg 2000;2:41–45.
Morohoshi T, Held G, Kloppel G. exocrine pancreatic tumours and their histological classification. A study based on 167 autopsy and 97 surgical cases. Histopathology 1983;7:645–661.
Maekawa T, Yabuki K, Satoh K, Tamasaki Y, Amano T, Sengoku H, et al. A case of pancreatic serous cystadenoma with obstructive jaundice. Dig Endosc 2000;12:55–60.
Horaguchi J, Fujita N, Kobayashi G, Noda Y, Kimura K, Ito K, et al. Serous cystadenoma of the pancreas associated with obstructive jaundice. J Gastroenterol 2003;38:501–506.
Watanabe H, Ohtsubo K, Yamaguchi Y, Mouri H, Motoo Y, Noto M, et al. Successful cystic fenestration for a macrocystic serous cystadenoma of the pancreas causing obstructive jaundice. Surg Today 2006;36:89–93.
Strobel O, Z’Graggen K, Schmitz-Winnenthal FH, Friess H, Kappeler A, Zimmermann A, et al. Risk of malignancy in serous cystic neoplasms of the pancreas. Digestion 2003;68:24–33.
Siech M, Tripp K, Schmidt-Rohlfing B, Mattfeldt T, Widmaier U, Gansauge F, et al. Cystic tumours of the pancreas: diagnostic accuracy, pathologic observations and surgical consequences. Langenbecks Arch Surg 1998;383:56–61.
Pyke CM, van Heerden JA, Colby TV, Sarr MG, Weaver AL. The spectrum of serous cystadenoma of the pancreas. Clinical, pathologic, and surgical aspects. Ann Surg 1992;215:132–139.
Fernandez-del Castillo C, Targarona J, Thayer SP, Rattner DW, Bruqqe WR, Warshaw AL. Incidental pancreatic cysts: clinicopathologic characteristics and comparison with symptomatic patients. Arch Surg 2003;138:427–434.
Le Borgne J, de Calan L, Partensky C. Cystadenomas and cystadenocarcinomas of the pancreas: a multiinstitutional retrospective study of 398 cases. French Surgical Association. Ann Surg 1999;230:152–161.
Tseng JF, Warshaw AL, Sahani DV, Lauwers GY, Rattner DW, Fernandez-del Castillo C. Serous cystadenoma of the pancreas. tumor growth rates and recommendations for treatment. Ann Surg 2005;242:413–421.
Belli L, Puttni M, Marni A. Extrahepatic portal obstruction: Clinical experience and surgical treatment in 105 patients. J Cardiovasc Surg 1980;21:439–448.
Moossa AR, Gadd MA. Isolated splenic vein thrombosis. World J Surg 1985;9:384–390.
Glynn MJ. Isolated splenic vein thrombosis. Arch Surg 1986;121: 723–725.
Madsen MS, Petersen TH, Sommer H. Segmental portal hypertension. Ann Surg 1986;204:72–77.
Sutton JP, Yarborough DY, Richards JT. Isolated splenic vein occlusion. Arch Surg 1970;100:623–626.
Okuyama M, Fujiwara Y, Hayakawa T, Shibata M, Watanabe T, Tominaga K, et al. Esophagogastric varices due to arterioportal shunt in a serous cystadenoma of the pancreas in von Hippel-Lindau disease. Dig Dis Sci 2003;48:1948–1954.
Iwasaki T, Nagata Y, Watahiki H, Yamamoto H, Ogawa H. A rare case of serous cystadenoma of the pancreas presenting with left-sided portal hypertension. Surg Today 1996;26:442–445.
Sarin SK, Lahoti D, Saxena SP, Murthy NS, Makwana UK. Prevalence, classification and natural history of gastric varices: A long-term follow-up study in 568 portal hypertension patients. Hepatology 1992;16:1343–1349.
Sakorafas GH, Sarr MG, Farley DR, Farnell MB. The significance of sinistral portal hypertension complicating chronic pancreatitis. Am J Surg 2000;179:129–133.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ito, K., Kudo, A., Nakamura, N. et al. Left-sided portal hypertension caused by serous cystadenoma of the pancreas: Report of a case. Surg Today 38, 184–187 (2008). https://doi.org/10.1007/s00595-007-3600-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-007-3600-y