Abstract
Aims
Our aim was to explore optimal treatment decisions for HbA1c control for type 2 diabetes mellitus patients and assess the impact on potential improvements in quality of life compared with current guidelines.
Methods
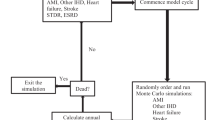
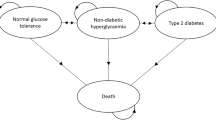
We analyzed a large dataset of HbA1c levels, diabetes-related key risk factors and medication dispensed to 70,069 patients with type 2 diabetes from polyclinics and a large public hospital in Singapore during January 1, 2008, to December 31, 2015. A Markov decision process (MDP) model was developed to determine the optimal treatment policy concerning medication management for glycemic control over a long-term treatment period. We assessed the model performance by comparing quality-adjusted life years (QALYs) gained by the model with those derived by a conventional Markov model informed by current clinical guidelines.
Results
Numerical results showed that optimal treatment strategies derived by the MDP model could increase the total expected QALYs by as much as 0.27 years for patients at higher risk such as old age, high HbA1c levels and smokers. In particular, the improvements in QALYs gained for patients with HbA1c levels of 9% (75 mmol/mol) and above were higher than those with lower HbA1c levels. However, the potential improvements appeared to be marginal for patients at lower risk compared with current guidelines.
Conclusions
Use of data-driven prescriptive analytics would help clinicians make evidence-based treatment decisions for HbA1c control for patients with type 2 diabetes, in particular for those at high risk.


Similar content being viewed by others
Availability of data and materials
The corresponding author has all the data and materials.
References
Chan JC, Malik V, Jia W, Kadowaki T, Yajnik CS, Yoon KH et al (2009) Diabetes in Asia: epidemiology, risk factors, and pathophysiology. JAMA 301:2129–2140
Ramachandran A, Snehalatha C, Shetty AS, Nanditha A (2012) Trends in prevalence of diabetes in Asian countries. World J Diabetes 3:110–117
International Diabetes Federation (2019) IDF diabetes atlas, 9th edn. International Diabetes Federation, Brussels, Belgium. https://diabetesatlas.org/en/resources/. Accessed 6 Jan 2020
Phan TP, Alkema L, Tai ES, Tan CHX, Yang Q, Lim W-Y et al (2014) Forecasting the burden of type 2 diabetes in Singapore using a demographic epidemiological model of Singapore. BMJ Open Diabetes Res Care 2:e000012
Ministry of Health, Singapore. News Highlights on 7th May, 2019. https://www.moh.gov.sg/news-highlights/details/percentage-of-spending-on-mental-health-diabetes-and-ageing-versus-total-healthcare-spending-in-2018-against-amount-budgeted-for-2019/. Accessed 6 Jan 2020
Gold M, Siegel J, Russell L, Weinstein M (1996) Cost-effectiveness in health and medicine. Oxford University Press, New York
Gold M, Stevenson D, Fryback D (2002) HALYs and QALYs and DALYs, OH MY: similarities and differences in summary measures of population health. Annu Rev Publ Health 23:115–134
Weinstein MC, Torrance G, McGuire A (2009) QALYs: the basics. Value Health 12:S5–S9
Ministry of Health (2018) Clinical practice guidelines: diabetes mellitus (summary booklet). Ministry of Health, Singapore. https://www.moh.gov.sg/hpp/doctors/guidelines/GuidelinesDetails/cpgmed_diabetes_mellitus; 2014. Accessed 15 Mar 2018
Roberts MS (1992) Markov process-based Monte Carlo simulation: a tool for modeling complex disease and its application to the timing of liver transplantation. In: Proceedings of the 24th conference on winter simulation 1992, Arlington, VA, pp 1034–1040
Puterman ML (2008) Markov decision processes: discrete stochastic dynamic programming. Wiley, Hoboken
Alagoz O, Hsu H, Schaefer AJ, Roberts MS (2010) Markov decision processes: a tool for sequential decision making under uncertainty. Med Decis Mak 30:474–483
Alagoz O, Maillart LM, Schaefer AJ, Roberts MS (2007) Choosing among living-donor and cadaveric livers. Manag Sci 53:1702–1715
Schechter SM, Bailey MD, Schaefer AJ, Roberts MS (2008) The optimal time to initiate HIV therapy under ordered health states. Oper Res 56:20–33
Mason JE, Denton BT, Shah ND, Smith SA (2014) Optimizing the simultaneous management of blood pressure and cholesterol for type 2 diabetes patients. Eur J Oper Res 233:727–738
Kurt M, Denton BT, Schaefer AJ, Shah ND, Smith SA (2011) The structure of optimal statin initiation policies for patients with type 2 diabetes. IIE Trans Healthc Syst Eng 1:49–65
Denton B, Kurt M, Shah N, Bryant S, Smith S (2009) Optimizing the start time of statin therapy for patients with diabetes. Med Decis Mak 29:351–367
American Diabetes Association (2013) Standards of medical care in diabetes. Diabetes Care 36:S11–S66
Zhang Y, McCoy RG, Mason JE, Smith SA, Shah ND, Denton BT (2014) Second-line agents for glycemic control for type 2 diabetes: are newer agents better? Diabetes Care 37:1338–1345
Arias E (2011) United States Life Tables, 2007. National Vital Statistics Reports, vol 59, no 9
Clarke PM, Gray AM, Briggs A, Farmer AJ, Fenn P, Stevens RJ et al (2004) A model to estimate the lifetime health outcomes of patients with type 2 diabetes: the United Kingdom Prospective Diabetes Study (UKPDS) Outcomes Model (UKPDS no. 68). Diabetologia 47:1747–1759
Expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (2001) Executive summary of the third report of the national cholesterol education program (NCEP) expert panel on detection evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 285:2486–2497
Hsu WC, Araneta MRG, Kanaya AM, Chiang JL, Fujimoto W (2015) BMI cut points to identify at-risk Asian Americans for type 2 diabetes screening. Diabetes Care 38:150–158
Fitch K, Iwasaki K, Pyenson B (2012) The cost and quality gap in diabetes care: an actuarial analysis. Milliman Client Report, commissioned by At&T Services, Inc
Acknowledgements
F. Meng acknowledges funding support by the National Medical Research Council, Singapore, Grant Number NMRC/HSRNIG/0008/2015. The authors thank Professor Melvyn Sim, the Department of Analytics & Operations of National University of Singapore, for providing his modeling expertise in decision science under uncertain environments. We thank the anonymous reviewers for their constructive suggestions and comments which helped to improve the presentation of the paper.
Funding
This work was supported by the National Medical Research Council, Singapore, Grant Number NMRC/HSRNIG/0008/2015.
Author information
Authors and Affiliations
Contributions
FM contributed to the definition of the problem, model development, data analysis, writing, reviewing and editing the paper. YS contributed to the definition of the problem, model development, reviewing and editing the paper. BHH contributed to the definition of the problem, constructive scientific and clinical advice, reviewing and editing the paper. MKSL contributed to the definition of the problem, model development, constructive scientific and clinical advice, reviewing and editing the paper. FM performed numerical experiments and is the principal investigator of this work. All authors take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Consent for publication
All the authors have approved the final manuscript and consented for publication.
Ethics standard statement
The data of this study were acquired in a retrospective study entitled “Evaluation of treatment strategies in prevention of stroke and coronary heart disease among type 2 diabetic patients using Markov decision process” and ethically approved by the Domain Specific Review Board (DSRB reference number—2015/00698) of National Healthcare Group, Singapore, which was determined by the DSRB to be an exempt category.
Informed consent
Informed consent from patients was not taken because this is a retrospective study and the data were de-identified.
Additional information
Managed By Antonio Secchi.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Meng, F., Sun, Y., Heng, B.H. et al. Analysis via Markov decision process to evaluate glycemic control strategies of a large retrospective cohort with type 2 diabetes: the ameliorate study. Acta Diabetol 57, 827–834 (2020). https://doi.org/10.1007/s00592-020-01492-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-020-01492-x