Abstract
Aims
In this retrospective study, we sought to delineate the collateral circulation status of acute ischemic stroke patients by CT perfusion and evaluate 90-day modified Rankin Scale (mRS) scores of patients with good or poor collaterals and its correlation with admission fasting plasma glucose (FPG).
Methods
We enrolled acute ischemic stroke patients who presented to our hospital 4.5 h within an onset of the first episode between January 2009 and December 2015. Neurological assessment was performed using the 90-day mRS scores (0–2 for a favorable and 3–6 for an unfavorable neurologic outcome). Relative filling time delay (rFTD) was evaluated by CT perfusion scan. The primary outcomes were 90-day mRS scores stratified by good (rFTD ≤ 4 s) versus poor collateral circulation (rFTD > 4 s).
Results
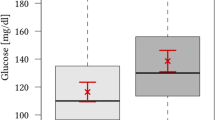
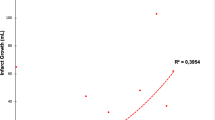
Totally 270 patients were included, and 139 (51.5%) patients achieved a favorable neurologic outcome. One hundred eighty-five (68.5%) patients had good collateral circulation. Significantly greater portions of patients with good collateral circulation (60.5%, 112/185) achieved a favorable neurologic outcome compared to those with poor collateral circulation (31.8%, 27/85) (P < 0.05). Patients with good collateral circulation achieving a favorable neurologic outcome had significantly lower baseline FPG (6.6 ± 1.96) than those with good collateral circulation achieving an unfavorable neurologic outcome (8.12 ± 4.02; P = 0.002). Spearman correlation analysis showed that rFTD significantly correlated with 90-day mRS scores (adjusted r = 0.258; P < 0.001) and admission FPG (r = 0.286; P < 0.001).
Conclusion
Higher admission FPG levels are associated with significantly higher rates of unfavorable neurologic outcome of acute ischemic stroke patients with good collateral circulation. FPG and rFTD may serve as useful predictors of short-term patient outcome and could be used for risk stratification in clinical decision making.





Similar content being viewed by others
References
Gao X et al (2012) Admission clinical characteristics and early clinical outcomes among acute ischemic stroke patients. J Biomed Res 26(3):152–158
Jeng JS et al (2008) Predictors of survival and functional outcome in acute stroke patients admitted to the stroke intensive care unit. J Neurol Sci 270(1–2):60–66
Kwak HS et al (2013) Predictors of functional outcome after emergency carotid artery stenting and intra-arterial thrombolysis for treatment of acute stroke associated with obstruction of the proximal internal carotid artery and tandem downstream occlusion. AJNR Am J Neuroradiol 34(4):841–846
Scott JF et al (1999) Prevalence of admission hyperglycaemia across clinical subtypes of acute stroke. Lancet 353(9150):376–377
Bruno A, Williams LS, Kent TA (2004) How important is hyperglycemia during acute brain infarction? Neurologist 10(4):195–200
Weir CJ et al (1997) Is hyperglycaemia an independent predictor of poor outcome after acute stroke? Results of a long-term follow up study. BMJ 314(7090):1303–1306
Williams LS et al (2002) Effects of admission hyperglycemia on mortality and costs in acute ischemic stroke. Neurology 59(1):67–71
Stead LG et al (2009) Hyperglycemia as an independent predictor of worse outcome in non-diabetic patients presenting with acute ischemic stroke. Neurocrit Care 10(2):181–186
Osei E et al (2017) Admission glucose and effect of intra-arterial treatment in patients with acute ischemic stroke. Stroke 48(5):1299–1305
Gray CS et al (2007) Glucose-potassium-insulin infusions in the management of post-stroke hyperglycaemia: the UK Glucose Insulin in Stroke Trial (GIST-UK). Lancet Neurol 6(5):397–406
Bruno A et al (2008) Treatment of hyperglycemia in ischemic stroke (THIS): a randomized pilot trial. Stroke 39(2):384–389
Winship IR (2015) Cerebral collaterals and collateral therapeutics for acute ischemic stroke. Microcirculation 22(3):228–236
Hatano S (1976) Experience from a multicentre stroke register: a preliminary report. Bull World Health Organ 54(5):541–553
Cox NH, Lorains JW (1986) The prognostic value of blood glucose and glycosylated haemoglobin estimation in patients with stroke. Postgrad Med J 62(723):7–10
Uyttenboogaart M et al (2005) Optimizing cutoff scores for the Barthel index and the modified Rankin scale for defining outcome in acute stroke trials. Stroke 36(9):1984–1987
Uyttenboogaart M et al (2007) Moderate hyperglycaemia is associated with favourable outcome in acute lacunar stroke. Brain 130(Pt 6):1626–1630
Cao W et al (2014) Relative filling time delay based on CT perfusion source imaging: a simple method to predict outcome in acute ischemic stroke. AJNR Am J Neuroradiol 35(9):1683–1687
Dankbaar JW et al (2017) Internal carotid artery stenosis and collateral recruitment in stroke patients. Clin Neuroradiol. https://doi.org/10.1007/s00062-017-0568-x
van Seeters T et al (2015) The prognostic value of CT angiography and CT perfusion in acute ischemic stroke. Cerebrovasc Dis 40(5–6):258–269
Capes SE et al (2001) Stress hyperglycemia and prognosis of stroke in nondiabetic and diabetic patients: a systematic overview. Stroke 32(10):2426–2432
Rosso C et al (2012) Intensive versus subcutaneous insulin in patients with hyperacute stroke: results from the randomized INSULINFARCT trial. Stroke 43(9):2343–2349
Kruyt ND et al (2010) Hyperglycemia in acute ischemic stroke: pathophysiology and clinical management. Nat Rev Neurol 6(3):145–155
Bruno A et al (2002) Admission glucose level and clinical outcomes in the NINDS rt-PA Stroke Trial. Neurology 59(5):669–674
Pulsinelli WA et al (1983) Increased damage after ischemic stroke in patients with hyperglycemia with or without established diabetes mellitus. Am J Med 74(4):540–544
Ahmed N et al (2010) Association of admission blood glucose and outcome in patients treated with intravenous thrombolysis: results from the Safe Implementation of Treatments in Stroke International Stroke Thrombolysis Register (SITS-ISTR). Arch Neurol 67(9):1123–1130
Kim JJ et al (2004) Regional angiographic grading system for collateral flow: correlation with cerebral infarction in patients with middle cerebral artery occlusion. Stroke 35(6):1340–1344
Prado R et al (1988) Hyperglycemia increases infarct size in collaterally perfused but not end-arterial vascular territories. J Cereb Blood Flow Metab 8(2):186–192
Mitchell EA et al (2012) Hyperglycaemia monitoring and management in stroke care: policy vs. practice. Diabet Med 29(9):1108–1114
Bravata DM et al (2003) Hyperglycaemia in patients with acute ischaemic stroke: how often do we screen for undiagnosed diabetes? QJM 96(7):491–497
Gray CS et al (2004) Prevalence and prediction of unrecognised diabetes mellitus and impaired glucose tolerance following acute stroke. Age Ageing 33(1):71–77
Masrur S et al (2015) Association of acute and chronic hyperglycemia with acute ischemic stroke outcomes post-thrombolysis: findings from get with the guidelines-stroke. J Am Heart Assoc 4(10):e002193
Ntaios G et al (2011) Persistent hyperglycemia at 24–48 h in acute hyperglycemic stroke patients is not associated with a worse functional outcome. Cerebrovasc Dis 32(6):561–566
Luitse MJ et al (2017) Chronic hyperglycemia is related to poor functional outcome after acute ischemic stroke. Int J Stroke 12(2):180–186
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and Animal Rights disclosure
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Melbourne Health Human Research Ethics Committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Patient consent was not required because of the retrospective nature of the study.
Additional information
Managed by Antonio Secchi.
Electronic supplementary material
Below is the link to the electronic supplementary material.
592_2018_1139_MOESM1_ESM.tif
Supplementary Figure 1 ROC curve of baseline FPG for 90-day mortality in diabetic patients with good collateral circulation. (TIFF 299 kb)
Rights and permissions
About this article
Cite this article
Wang, F., Jiang, B., Kanesan, L. et al. Higher admission fasting plasma glucose levels are associated with a poorer short-term neurologic outcome in acute ischemic stroke patients with good collateral circulation. Acta Diabetol 55, 703–714 (2018). https://doi.org/10.1007/s00592-018-1139-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-018-1139-6