Abstract
Background
In THA, using a larger femoral head can increase the oscillation angle and jumping distance. However, there have been no reports which indicate precisely how increasing the jumping distance leads to an increase in the angle from impingement to dislocation (jumping angle). In this study, we clarified the jumping angle of various head diameters and its relationship with pelvic morphology.
Methods
Using a three-dimensional templating system, virtual THA and ROM simulations were performed in 82 patients. We investigated the distance between bony and prosthetic impingement points and the head centre and calculated the jumping angle for various head diameters. We measured various pelvic shapes and length to clarify the relationship between pelvic morphology and impingement distance.
Results
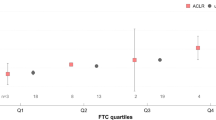
Jumping angles were 7.7° ± 3.2°, 12.1° ± 1.6°, 15.4° ± 2.5° and 10.0° ± 3.0° with flexion, internal rotation with 90° flexion (IR), extension and external rotation (ER), respectively, when we used a 22-mm head diameter. Bony jumping angle increased about 0.5°, 0.8°, 1.0° and 0.7° per 2-mm increase in head diameter with flexion, IR, extension and ER. On the other hand, prosthetic jumping angle remained almost stable at about 31°. Impingement distance was related to pelvic morphology in all directions. Bony jumping angles differed with ROM; the biggest was seen with extension, followed by IR, ER and flexion. On the other hand, bony jumping angle was less than prosthetic jumping angle in all cases.
Conclusion
Bony jumping angles differed with ROM; the biggest was seen with extension, followed by IR, ER and flexion. Prosthetic impingement angles were stable. In addition, the bony jumping angle was less than the prosthetic jumping angle in all cases.






Similar content being viewed by others
References
Alberton GM, High WA, Morrey BF (2002) Dislocation after revision total hip arthroplasty: an analysis of risk factors and treatment options. J Bone Joint Surg Am 84-A:1788–1792
Sariali E, Leonard P, Mamoudy P (2008) Dislocation after total hip arthroplasty using Hueter anterior approach. J Arthroplast 23:266–272. https://doi.org/10.1016/j.arth.2007.04.003
Bozic KJ, Kurtz SM, Lau E et al (2009) The epidemiology of revision total hip arthroplasty in the United States. J Bone Joint Surg Am 91:128–133. https://doi.org/10.2106/JBJS.H.00155
Dunbar MJ (2010) The proximal modular neck in THA: a bridge too far: affirms. Orthopedics 33:640. https://doi.org/10.3928/01477447-20100722-30
Duwelius PJ, Burkhart B, Carnahan C et al (2014) Modular versus nonmodular neck femoral implants in primary total hip arthroplasty: which is better? Clin Orthop Relat Res 472:1240–1245. https://doi.org/10.1007/s11999-013-3361-4
Malik A, Maheshwari A, Dorr LD (2007) Impingement with total hip replacement. J Bone Joint Surg Am 89:1832–1842. https://doi.org/10.2106/JBJS.F.01313
Widmer K-H (2007) Containment versus impingement: finding a compromise for cup placement in total hip arthroplasty. Int Orthop 31(Suppl 1):S29–S33. https://doi.org/10.1007/s00264-007-0429-3
Ohmori T, Kabata T, Kajino Y et al (2017) Differences in range of motion with the same combined anteversion after total hip arthroplasty. Int Orthop. https://doi.org/10.1007/s00264-017-3653-5
Shoji T, Yasunaga Y, Yamasaki T et al (2013) Bony impingement depends on the bone morphology of the hip after total hip arthroplasty. Int Orthop 37:1897–1903. https://doi.org/10.1007/s00264-013-1979-1
Shoji T, Yasunaga Y, Yamasaki T et al (2016) Anterior inferior iliac spine bone morphology in hip dysplasia and its effect on hip range of motion in total hip arthroplasty. J Arthroplast 31:2058–2063. https://doi.org/10.1016/j.arth.2016.02.018
Shoji T, Yamasaki T, Izumi S et al (2017) Factors affecting the potential for posterior bony impingement after total hip arthroplasty. Bone Joint J 99-B:1140–1146. https://doi.org/10.1302/0301-620x.99b9.bjj-2016-1078.r2
Ohmori T, Kabata T, Maeda T et al (2017) Increase in safe zone area of the acetabular cup using dual mobility cups in THA. Hip Int 27:361–367. https://doi.org/10.5301/hipint.5000466
Ohmori T, Kabata T, Maeda T et al (2017) Selection of a surgical approach for total hip arthroplasty according to the depth to the surgical site. Hip Int 27:273–280. https://doi.org/10.5301/hipint.5000463
Crowninshield RD, Maloney WJ, Wentz DH et al (2004) Biomechanics of large femoral heads: what they do and don’t do. Clin Orthop Relat Res 429:102–107. https://doi.org/10.1097/01.blo.0000150117.42360.f9
Ito H, Tanino H, Yamanaka Y et al (2013) Intermediate- to long-term results after hybrid total hip arthroplasty in patients with rheumatoid arthritis. J Arthroplast 28:309–314. https://doi.org/10.1016/j.arth.2012.06.002
Viceconti M, Ruggeri O, Toni A, Giunti A (1996) Design-related fretting wear in modular neck hip prosthesis. J Biomed Mater Res 30:181–186. https://doi.org/10.1002/(SICI)1097-4636(199602)30:2%3c181:AID-JBM7%3e3.0.CO;2-N
Tarasevicius S, Robertsson O, Kesteris U et al (2008) Effect of femoral head size on polyethylene wear and synovitis after total hip arthroplasty: a sonographic and radiographic study of 39 patients. Acta Orthop 79:489–493. https://doi.org/10.1080/17453670710015472
Lombardi AVJ, Berend KR, Morris MJ et al (2015) Large-diameter metal-on-metal total hip arthroplasty: dislocation infrequent but survivorship poor. Clin Orthop Relat Res 473:509–520. https://doi.org/10.1007/s11999-014-3976-0
Bolland BJRF, Culliford DJ, Langton DJ et al (2011) High failure rates with a large-diameter hybrid metal-on-metal total hip replacement: clinical, radiological and retrieval analysis. J Bone Joint Surg Br 93:608–615. https://doi.org/10.1302/0301-620X.93B5.26309
Simian E, Chatellard R, Druon J et al (2015) Dual mobility cup in revision total hip arthroplasty: dislocation rate and survival after 5 years. Orthop Traumatol Surg Res 101:577–581. https://doi.org/10.1016/j.otsr.2015.05.002
Puch J-M, Derhi G, Descamps L et al (2017) Dual-mobility cup in total hip arthroplasty in patients less than fifty five years and over ten years of follow-up: a prospective and comparative series. Int Orthop 41:475–480. https://doi.org/10.1007/s00264-016-3325-x
Cooper HJ, Della Valle CJ (2014) Large diameter femoral heads: is bigger always better? Bone Joint J 96-B:23–26. https://doi.org/10.1302/0301-620x.96b11.34342
Werner BC, Brown TE (2012) Instability after total hip arthroplasty. World J Orthop 3:122–130. https://doi.org/10.5312/wjo.v3.i8.122
Komiyama K, Fukushi J-I, Motomura G et al (2018) Does high hip centre affect dislocation after total hip arthroplasty for developmental dysplasia of the hip? Int Orthop. https://doi.org/10.1007/s00264-018-4154-x
Hummel MT, Malkani AL, Yakkanti MR, Baker DL (2009) Decreased dislocation after revision total hip arthroplasty using larger femoral head size and posterior capsular repair. J Arthroplast 24:73–76. https://doi.org/10.1016/j.arth.2009.04.026
Phillips CB, Barrett JA, Losina E et al (2003) Incidence rates of dislocation, pulmonary embolism, and deep infection during the first six months after elective total hip replacement. J Bone Joint Surg Am 85-A:20–26
Tsikandylakis G, Karrholm J, Hailer NP et al (2018) No increase in survival for 36-mm versus 32-mm femoral heads in metal-on-polyethylene THA: a registry study. Clin Orthop Relat Res. https://doi.org/10.1097/corr.0000000000000508
Prietzel T, Hammer N, Schleifenbaum S et al (2014) The impact of capsular repair on the dislocation rate after primary total hip arthroplasty: a retrospective analysis of 1972 cases. Z Orthop Unfall 152:130–143. https://doi.org/10.1055/s-0034-1368209
Bottner F, Pellicci PM (2006) Review: posterior soft tissue repair in primary total hip arthroplasty. HSS J 2:7–11. https://doi.org/10.1007/s11420-005-0134-y
Kumar V, Sharma S, James J et al (2014) Total hip replacement through a posterior approach using a 22 mm diameter femoral head: the role of the transverse acetabular ligament and capsular repair in reducing the rate of dislocation. Bone Joint J 96-B:1202–1206. https://doi.org/10.1302/0301-620x.96b9.31831
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest as related to the study.
Rights and permissions
About this article
Cite this article
Ohmori, T., Kabata, T., Kajino, Y. et al. Effect of changing femoral head diameter on bony and prosthetic jumping angles. Eur J Orthop Surg Traumatol 29, 625–632 (2019). https://doi.org/10.1007/s00590-018-2325-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-018-2325-5