Abstract
Objective
To quantify muscle characteristics (volumes and fat infiltration) and identify their relationship to sagittal malalignment and compensatory mechanism recruitment.
Methods
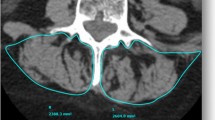
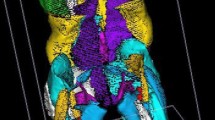
Female adult spinal deformity patients underwent T1-weighted MRI with a 2-point Dixon protocol from the proximal tibia up to the T12 vertebra. 3D reconstructions of 17 muscles, including extensors and flexors of spine, hip and knee, were obtained. Muscle volume standardized by bone volume and percentage of fat infiltration (Pfat) were calculated. Correlations and regressions were performed.
Results
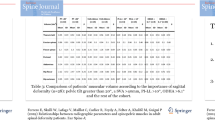
A total of 22 patients were included. Significant correlations were observed between sagittal alignment and muscle parameters. Fat infiltration of the hip and knee flexors and extensors correlated with larger C7-S1 SVA. Smaller spinal flexor/extensor volumes correlated with greater PI-LL mismatch (r = − 0.45 and − 0.51). Linear regression identified volume of biceps femoris as only predictor for PT (R2 = 0.34, p = 0.005) and Pfat of gluteus minimus as only predictor for SVA (R2 = 0.45, p = 0.001). Sagittally malaligned patients with larger PT (26.8° vs. 17.2°) had significantly smaller volume and larger Pfat of gluteus medius, gluteus minimus and biceps femoris, but similar values for gluteus maximus, the hip extensor.
Conclusion
This study is the first to quantify the relationship between degeneration of spino-femoral muscles and sagittal malalignment. This pathoanatomical study identifies the close relationship between gluteal, hamstring muscles and PT, SVA, which deepens our understanding of the underlying etiology that contributes to adult spinal deformity.

Similar content being viewed by others
References
Ferrero E, Vira S, Challier V et al. (2015) Analysis of an unexplored group of sagittal deformity patients: large sagittal malalignment but low pelvic tilt. In: ISASS. p Podium 499
Kang CH, Shin MJ, Kim SM et al (2007) MRI of paraspinal muscles in lumbar degenerative kyphosis patients and control patients with chronic low back pain. Clin Radiol 62:479–486. https://doi.org/10.1016/j.crad.2006.12.002
Helbostad JL, Sturnieks DL, Menant J et al (2010) Consequences of lower extremity and trunk muscle fatigue on balance and functional tasks in older people: a systematic literature review. BMC Geriatr 10:56. https://doi.org/10.1186/1471-2318-10-56
Hsu W-L, Chen C-Y, Tsauo J-Y, Yang R-S (2014) Balance control in elderly people with osteoporosis. J Formos Med Assoc 113:334–339. https://doi.org/10.1016/j.jfma.2014.02.006
Diebo BG, Lafage R, Ferrero E et al. (2015) Musculoskeletal compensatory mechanisms for spinal malalignment: an age-related study. In: American academy of orthopaedic surgeons (AAOS). Las Vegas, Nevada
Ferrero E, Liabaud B, Challier V et al (2015) Role of pelvic translation and lower-extremity compensation to maintain gravity line position in spinal deformity. J Neurosurg Spine. https://doi.org/10.3171/2015.5.SPINE14989
Schwab F, Ungar B, Blondel B et al (2012) Scoliosis research society—schwab adult spinal deformity classification. Spine 37:1077–1082
Champain S, Benchikh K, Nogier A et al (2006) Validation of new clinical quantitative analysis software applicable in spine orthopaedic studies. Eur Spine J 15:982–991. https://doi.org/10.1007/s00586-005-0927-1
Moal B, Raya JG, Jolivet E et al (2014) Validation of 3D spino-pelvic muscle reconstructions based on dedicated MRI sequences for fat-water quantification. Irbm 35:119–127. https://doi.org/10.1016/j.irbm.2013.12.011
Moal B (2015) Volume and fat infiltration of spino-pelvic musculature in adults with spinal deformity. World J Orthop 6:727. https://doi.org/10.5312/wjo.v6.i9.727
Diebo BG, Varghese JJ, Lafage R et al (2015) Sagittal alignment of the spine: what do you need to know? Clin Neurol Neurosurg 139:295–301. https://doi.org/10.1016/j.clineuro.2015.10.024
Schwab FJ, Diebo BG, Smith JS et al (2014) Fine-tuned surgical planning in adult spinal deformity: determining the lumbar lordosis necessary by accounting for both thoracic kyphosis and pelvic incidence. Spine J 14:S73. https://doi.org/10.1016/j.spinee.2014.08.189
Meakin JR, Fulford J, Seymour R et al (2013) The relationship between sagittal curvature and extensor muscle volume in the lumbar spine. J Anat 222:608–614. https://doi.org/10.1111/joa.12047
Patwardhan AG, Havey RM, Meade KP et al (1999) A follower load increases the load-carrying capacity of the lumbar spine in compression. Spine 24:1003–1009. https://doi.org/10.1097/00007632-199905150-00014
Meakin JR, Aspden RM (2012) Modeling the effect of variation in sagittal curvature on the force required to produce a follower load in the lumbar spine. J Mech Med Biol 12:1250013. https://doi.org/10.1142/S0219519412004466
Alvim FC, Peixoto JG, Vicente EJD et al (2010) Influences of the extensor portion of the gluteus maximus muscle on pelvic tilt before and after the performance of a fatigue protocol. Rev Bras Fisioter 14:206–213
Soderberg GL, Dostal WF (1978) Electromyographic study of three parts of the gluteus medius muscle during functional activities. Phys Ther 58:691–696
Gottschalk F, Kourosh S, Leveau B (1989) The functional anatomy of tensor fasciae latae and gluteus medius and minimus. J Anat 166:179–189. https://doi.org/10.1016/j.clinbiomech.2007.07.001
Beck M, Sledge JB, Gautier E et al (2000) The anatomy and function of the gluteus minimus muscle. J Bone Joint Surg Br 82:358–363. https://doi.org/10.1302/0301-620X.82B3.10356
Wolf SI, Mikut R, Kranzl A, Dreher T (2014) Which functional impairments are the main contributors to pelvic anterior tilt during gait in individuals with cerebral palsy? Gait Posture 39:359–364. https://doi.org/10.1016/j.gaitpost.2013.08.014
Ross JR, Nepple JJ, Philippon MJ et al (2014) Effect of changes in pelvic tilt on range of motion to impingement and radiographic parameters of acetabular morphologic characteristics. Am J Sports Med 42:2402–2409. https://doi.org/10.1177/0363546514541229
Ross JR, Tannenbaum EP, Nepple JJ et al (2015) Functional acetabular orientation varies between supine and standing radiographs: implications for treatment of femoroacetabular impingement. Clin Orthop Relat Res 473:1267–1273. https://doi.org/10.1007/s11999-014-4104-x
Shimizu M, Kobayashi T, Jimbo S et al. (2016) A cohort study of adult spinal deformity and its relation with hip-knee range of motion. In: AAOS. p Podium 500
Carregaro RL, Gil Coury HJC (2009) Does reduced hamstring flexibility affect trunk and pelvic movement strategies during manual handling? Int J Ind Ergon 39:115–120. https://doi.org/10.1016/j.ergon.2008.05.004
Esola MA, McClure PW, Fitzgerald GK, Siegler S (1996) Analysis of lumbar spine and hip motion during forward bending in subjects with and without a history of low back pain. Spine 21:71–78
Hosman AJ, de Kleuver M, Anderson PG et al (2003) Scheuermann kyphosis: the importance of tight hamstrings in the surgical correction. Spine 28:2252–2259. https://doi.org/10.1097/01.BRS.0000085097.63326.95
Acknowledgements
The manuscript submitted does not contain information about medical device(s)/drug(s). This work received funding from Youth Fund of Natural Science Foundation of Jiangsu Province (BK20180122). This work received funding from Key Project supported by Medical Science and Technology Development Foundation, Nanjing Department of Health (YKK18092).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bao, H., Moal, B., Vira, S. et al. Spino-femoral muscles affect sagittal alignment and compensatory recruitment: a new look into soft tissues in adult spinal deformity. Eur Spine J 29, 2998–3005 (2020). https://doi.org/10.1007/s00586-020-06488-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06488-3