Abstract
Study design
Prospective analysis of patients who underwent minimally invasive posterior instrumentation.
Objective
The purpose of this study was to evaluate the safety of minimally invasive pedicle screw placement in patients with unstable thoracic and lumbar spine fractures using the conventional fluoroscopy technique.
Summary of background data
Although wound infection, haematoma, and new neurological deficit due to screw malplacement remain a common source of morbidity, estimates of their rates of occurrence remain relatively limited.
Methods
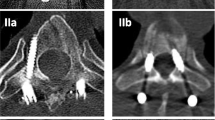
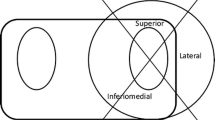
2052 percutaneous pedicle screws in 433 consecutive patients were evaluated. The accuracy of pedicle screw placement was based on evaluation of axial 3-mm slice computed tomography scans. Morbidity and mortality data were collected prospectively.
Results
A total of 2029 of 2052 screws (99%) had a good or excellent position. 5 screws (0.2%) showed a higher grade violation of the medial pedicle wall. Seven patients (1.8%) needed revision due to screw malposition (3 pat.), surgical site infection, postoperative haematoma, implant failure (2 pat.), and technical difficulties.
Conclusions
Minimally invasive transpedicular instrumentation is an accurate, reliable, and safe procedure to treat thoracic and lumbar spine fractures.








Similar content being viewed by others
References
Alpantaki K, Bano A, Pasku D, Mavrogenis AF, Papagelopoulos PJ, Sapkas GS, Korres DS, Katonis P (2010) Thoracolumbar burst fractures: a systematic review of management. Orthopedics 33(6):422–429
Oner FC, Wood KB, Smith JS, Shaffrey CI (2010) Therapeutic decision making in thoracolumbar spine trauma. Spine 35:S235–S244
Foley KT, Gupta SK, Justis JR, Sherman MC (2001) Percutaneous pedicle screw fixation of the lumbar spine. Neurosurg Focus 10:E10
Reinhold M, Knop C, Beisse R, Audige L, Kandziora F, Pizanis A, Pranzl R, Gercek E, Schultheiss M, Weckbach A, Bühren V, Blauth M (2010) Operative treatment of 733 patients with acute thoracolumbar spinal injuries: comprehensive results from the second, prospective, internet-based multicenter study of the Spine Study Group of the German Association of Trauma Surgery. Eur Spine J 19:1657–1676
Khare S, Sharma V (2013) Surgical outcome of posterior short segment trans-pedicle screw fixation for thoracolumbar fractures. J Orthop 10(4):162–167
Mobbs RJ, Sivabalan P, Li J (2011) Technique, challenges and indications for percutaneous pedicle screw fixation. J Clin Neurosci 18(6):741–749
Lee SH, Choi WG, Lim SR, Kang HY, Shin SW (2004) Minimally invasive anterior lumbar interbody fusion followed by percutaneous pedicle screw fixation for isthmic spondylolisthesis. Spine J 4:644–649
Rahman M, Summers LE, Richter B, Mimran RI, Jacob RP (2008) Comparison of techniques for decompressive lumbar laminectomy: the minimally invasive versus the “classic” open approach. Minim Invasive Neurosurg 51:100–105
Powers CJ, Isaacs RE (2006) Minimally invasive fusion and fixation techniques. Neurosurg Clin N Am 17:477–489
Dickerman RD, Reynolds AS, Tackett J, Winters K, Alvarado C (2008) Percutaneous pedicle screws significantly decrease muscle damage and operative time: surgical technique makes a difference. Eur Spine J 17:1398
Wild MH, Glees M, Plieschnegger C, Wenda K (2007) Five-year follow-up examination after purely minimally invasive posterior stabilization of thoracolumbar fractures: a comparison of minimally invasive percutaneously and conventionally open treated patients. Arch Orthop Trauma Surg 127(5):335–343
Merom L, Raz N, Hamud C, Weisz I, Hanani A (2009) Minimally invasive burst fracture fixation in the thoracolumbar region. Orthopedics 32(4):273–275
Heintel TM, Berglehner A, Meffert R (2013) Accuracy of percutaneous pedicle screws for thoracic and lumbar spine fractures: a prospective trial. Eur Spine J 22(3):495–502
Zdichavsky M, Blauth M, Knop C, Graessner M, Herrmann H, Krettek C, Bastian L (2004) Accuracy of pedicle screw placement in thoracic spine fractures. Part I: inter- and intra-observer reliability of the scoring system. Eur J Trauma 30:234–240
Vaccaro AR, Schroeder GD, Kepler CK, Cumhur Oner F, Vialle LR, Kandziora F, Koerner JD, Kurd MF, Reinhold M, Schnake KJ, Chapman J, Aarabi B, Fehlings MG, Dvorak MF (2016) The surgical algorithm for the AOSpine thoracolumbar spine injury classification system. Eur Spine J 25(4):1087–1094
Lund T, Laine T, Österman H, Yrjönen T, Schlenzka D (2012) Accuracy of computer assisted screw insertion. The evidence. J Bone Joint Surg Br 94-B(SUPP XXXI):32
Austin MS, Vaccaro AR, Brislin B, Nachwalter R, Hilibrand AS, Albert TJ (2002) Image-guided spine surgery; a cadaver study comparing conventional open laminoforaminotomy and two image-guided techniques for pedicle screw placement in posterolateral fusion and nonfusion models. Spine 27:2503–2508
Özkan N, Sandalcioglu IE, Petr O, Kurniawan A, Dammann P, Schlamann M, Sure U, Asgari S (2012) Minimally invasive transpedicular dorsal stabilization of the thoracolumbar and lumbar spine using the minimal access non-traumatic insertion system (MANTIS): preliminary clinical results in 52 patients. J Neurol Surg A Cent Eur Neurosurg 73(6):369–376
Hicks JM, Singla A, Shen FH, Arlet V (2010) Complications of pedicle screw fixation in scoliosis surgery: a systematic review. Spine 35(11):E465–E470
Fehlings MG, Brodke DS, Norvell DC, Dettori JR (2010) The evidence for intraoperative neurophysiological monitoring in spine surgery: does it make a difference? Spine 35(9 Suppl):S37–S46
Lall RR, Lall RR, Hauptman JS, Munoz C, Cybulski GR, Koski T, Ganju A, Fessler RG, Smith ZA (2012) Intraoperative neurophysiological monitoring in spine surgery: indications, efficacy, and role of the preoperative checklist. Neurosurg Focus 33(5):E10
Gavaret M, Jouve JL, Péréon Y, Accadbled F, André-Obadia N, Azabou E, Blondel B, Bollini G, Delécrin J, Farcy JP, Fournet-Fayard J, Garin C, Henry P, Manel V, Mutschler V, Perrin G, Sales de Gauzy J, French Society of Spine Surgery SFCR (2013) Intraoperative neurophysiologic monitoring in spine surgery. Developments and state of the art in France in 2011. Orthop Traumatol Surg Res 99(6 Suppl):S319–S327
Hamilton DK, Smith JS, Sansur CA, Glassman SD, Ames CP, Berven SH, Polly DW Jr, Perra JH, Knapp DR, Boachie-Adjei O, McCarthy RE, Shaffrey CI, Scoliosis Research Society Morbidity and Mortality Committee (2011) Rates of new neurological deficit associated with spine surgery based on 108,419 procedures: a report of the scoliosis research society morbidity and mortality committee. Spine 36(15):1218–1228
Abbey DM, Turner DM, Warson JS, Wirt TC, Scalley RD (1995) Treatment of postoperative wound infections following spinal fusion with instrumentation. J Spinal Disord 8:278–283
Hodges SD, Humphreys SC, Eck JC, Covington LA, Kurzynske NG (1998) Low postoperative infection rates with instrumented lumbar fusion. South Med J 91:1132–1136
Picada R, Winter RB, Lonstein JE, Denis F, Pinto MR, Smith MD, Perra JH (2000) Postoperative deep wound infection in adults after posterior lumbosacral spine fusion with instrumentation: incidence and management. J Spinal Disord 13:42–45
Tenney JH, Vlahov D, Salcman M, Ducker TB (1985) Wide variation in risk of wound infection following clean neurosurgery. Implications for perioperative antibiotic prophylaxis. J Neurosurg 62:243–247
Weinstein MA, McCabe JP, Cammisa FP Jr (2000) Postoperative spinal wound infection: a review of 2,391 consecutive index procedures. J Spinal Disord 13:422–426
Wimmer C, Gluch H, Franzreb M, Ogon M (1998) Predisposing factors for infection in spine surgery: a survey of 850 spinal procedures. J Spinal Disord 11:124–128
O’Toole JE, Eichholz KM, Fessler RG (2009) Surgical site infection rates after minimally invasive spinal surgery. J Neurosurg Spine 11(4):471–476
Ni WF, Huang YX, Chi YL, Xu HZ, Lin Y, Wang XY, Huang QS, Mao FM (2010) Percutaneous pedicle screw fixation for neurologic intact thoracolumbar burst fractures. J Spinal Disord Tech 23(8):530–537
Blondel B, Fuentes S, Pech-Gourg G, Adetchessi T, Tropiano P, Dufour H (2011) Percutaneous management of thoracolumbar burst fractures: evolution of techniques and strategy. Orthop Traumatol Surg Res 97(5):527–532
Bironneau A, Bouquet C, Millet-Barbe B, Leclercq N, Pries P, Gayet LE (2011) Percutaneous internal fixation combined with kyphoplasty for neurologically intact thoracolumbar fractures: a prospective cohort study of 24 patients with one year of follow-up. Orthop Traumatol Surg Res 97(4):389–395
Smith JS, Shaffrey CI, Sansur CA, Berven SH, Fu KM, Broadstone PA, Choma TJ, Goytan MJ, Noordeen HH, Knapp DR Jr, Hart RA, Donaldson WF 3rd, Polly DW Jr, Perra JH, Boachie-Adjei O, Scoliosis Research Society Morbidity and Mortality Committee (2011) Rates of infection after spine surgery based on 108,419 procedures: a report from the Scoliosis Research Society Morbidity and Mortality Committee. Spine 36(7):556–563
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the institutional review board in accordance with the ethical principles originating from the Declaration of Helsinki and in compliance with Good Clinical Practice.
Conflict of interest
None of the authors has any potential conflict of interest.
Informed consent
All patients gave their informed consent.
Rights and permissions
About this article
Cite this article
Heintel, T.M., Dannigkeit, S., Fenwick, A. et al. How safe is minimally invasive pedicle screw placement for treatment of thoracolumbar spine fractures?. Eur Spine J 26, 1515–1524 (2017). https://doi.org/10.1007/s00586-016-4908-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4908-3