Abstract
Purposes
The postoperative analgesic effect of tizanidine has not yet been evaluated sufficiently. The role of bilateral superficial cervical plexus block (BSCPB) for postoperative analgesia after thyroidectomy remains questionable. We aimed to evaluate the analgesic effect of combined use of BSCPB and a single-dose oral tizanidine in patients undergoing elective thyroid surgery.
Methods
Sixty patients undergoing thyroidectomy were randomized into 3 groups. The control group (Group C, n = 20) received BSCPB with 0.9% saline plus oral placebo. The superficial cervical group (Group SC, n = 20) received BSCPB with 0.25% bupivacaine plus oral placebo. The superficial cervical and tizanidine group (Group SC + T, n = 20) received BSCPB with 0.25% bupivacaine plus tizanidine 6 mg capsule. Surgical site pain scores, opioid consumption, rescue analgesia, posterior neck pain, headache, and opioid-related side effects were assessed for the first 24 h.
Results
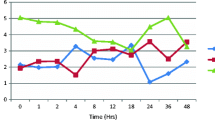
Compared with Group C, rest and swallowing pain scores in Group SC and Group SC + T were statistically lower at all postoperative time points (p < 0.05). Fentanyl consumption was lower in Group SC and Group SC + T than in Group C at time periods 0–4 and 4–8 h (p < 0.05). Fentanyl consumption was lower in Group SC + T than in Group SC at 0–4 h (p = 0.006). Total fentanyl consumption was higher in Group C than in the other groups (p < 0.001). Postoperative cervical pain and occipital headache were significantly lower in Group SC + T than in the other groups (p < 0.05).
Conclusions
Ultrasound-guided BSCPB with or without preemptive oral tizanidine was effective at reducing postoperative pain and opioid consumption in patients undergoing total thyroidectomy. Addition of preemptive oral tizanidine to BSCPB reduced the early postoperative opioid consumption, posterior neck pain, and occipital headache.
Clinical trials registry
The study was registered with a clinical trials registry (ClinicalTrials.gov. identifier NCT02725359).

Similar content being viewed by others
References
Yucel A, Yazici A, Muderris T, Gul F. Comparison of lornoxicam and low-dose tramadol for management of post-thyroidectomy pain. Agri. 2016;28(4):183–9.
Long K, Ruiz J, Kee S, Kowalski A, Goravanchi F, Cerny J, French K, Hernandez M, Perrier N, Rebello E. Effect of adjunctive dexmedetomidine on postoperative intravenous opioid administration in patients undergoing thyroidectomy in an ambulatory setting. J Clin Anesth. 2016;35:361–4.
Bindu M, Kumar AA, Kesavan M, Suresh V. Effect of preoperative pregabalin on postoperative pain relief in thyroidectomy patients: a prospective observational study. Anesth Essays Res. 2015;9(2):161–6.
Miu M, Royer C, Gaillat C, Schaup B, Menegaux F, Langeron O, Riou B, Aubrun F. Lack of analgesic effect induced by ropivacaine wound infiltration in thyroid surgery: a randomized, double-blind, placebo-controlled trial. Anesth Analg. 2016;122(2):559–64.
Gurkan Y, Tas Z, Toker K, Solak M. Ultrasound guided bilateral cervical plexus block reduces postoperative opioid consumption following thyroid surgery. J Clin Monit Comput. 2015;29(5):579–84.
Motamed C, Merle JC, Yakhou L, Combes X, Dumerat M, Vodinh J, Kouyoumoudjian C, Duvaldestin P. Intraoperative i.v. morphine reduces pain scores and length of stay in the post anaesthetic care unit after thyroidectomy. Br J Anaesth. 2004;93(2):306–7.
Ahiskalioglu EO, Ahiskalioglu A, Aydin P, Yayik AM, Temiz A. Effects of single-dose preemptive intravenous ibuprofen on postoperative opioid consumption and acute pain after laparoscopic cholecystectomy. Medicine (Baltimore). 2017;96(8):e6200.
Tabari M, Alipour M, Esalati H. Evaluation of oral tizanidine effects on [intraoperative] hemodynamic responses during direct laryngoscopy under general anesthesia. Iran Red Crescent Med J. 2013;15(7):541–6.
Takenaka M, Iida H, Kasamatsu M, Katoh H, Tashiro T, Dohi S. Tizanidine for preanesthetic medication. Masui. 1996;45(8):971–5.
Wajima Z, Yoshikawa T, Ogura A, Imanaga K, Shiga T, Inoue T, Ogawa R. Oral tizanidine, an alpha2-adrenoceptor agonist, reduces the minimum alveolar concentration of sevoflurane in human adults. Anesth Analg. 2002;95(2):393–6.
Yazicioglu D, Caparlar C, Akkaya T, Mercan U, Kulacoglu H. Tizanidine for the management of acute postoperative pain after inguinal hernia repair: a placebo-controlled double-blind trial. Eur J Anaesthesiol. 2016;33(3):215–22.
Talakoub R, Abbasi S, Maghami E, Zavareh SM. The effect of oral tizanidine on postoperative pain relief after elective laparoscopic cholecystectomy. Adv Biomed Res. 2016;5:19.
Bharti N, Dontukurthy S, Bala I, Singh G. Postoperative analgesic effect of intravenous (i.v.) clonidine compared with clonidine administration in wound infiltration for open cholecystectomy. Br J Anaesth. 2013;111(4):656–61.
Blaudszun G, Lysakowski C, Elia N, Tramer MR. Effect of perioperative systemic alpha2 agonists on postoperative morphine consumption and pain intensity: systematic review and meta-analysis of randomized controlled trials. Anesthesiology. 2012;116(6):1312–22.
Techanivate A, Dusitkasem S, Anuwattanavit C. Dexmedetomidine compare with fentanyl for postoperative analgesia in outpatient gynecologic laparoscopy: a randomized controlled trial. J Med Assoc Thail. 2012;95(3):383–90.
Smith C, Birnbaum G, Carter JL, Greenstein J, Lublin FD. Tizanidine treatment of spasticity caused by multiple sclerosis: results of a double-blind, placebo-controlled trial. US Tizanidine Study Group. Neurology. 1994;44(11 Suppl 9):S34–42 (discussion S-3).
Malanga GA, Gwynn MW, Smith R, Miller D. Tizanidine is effective in the treatment of myofascial pain syndrome. Pain Physician. 2002;5(4):422–32.
Semenchuk MR, Sherman S. Effectiveness of tizanidine in neuropathic pain: an open-label study. J Pain. 2000;1(4):285–92.
Saper JR, Lake AE III, Cantrell DT, Winner PK, White JR. Chronic daily headache prophylaxis with tizanidine: a double-blind, placebo-controlled, multicenter outcome study. Headache. 2002;42(6):470–82.
Park C, Choi JB, Lee YS, Chang HS, Shin CS, Kim S, Han DW. The effect of intra-operative transcutaneous electrical nerve stimulation on posterior neck pain following thyroidectomy. Anaesthesia. 2015;70(4):434–9.
Han DW, Koo BN, Chung WY, Park CS, Kim SY, Palmer PP, Kim KJ. Preoperative greater occipital nerve block in total thyroidectomy patients can reduce postoperative occipital headache and posterior neck pain. Thyroid. 2006;16(6):599–603.
Ayhan H, Tastan S, Iyigun E, Ozturk E, Yildiz R, Gorgulu S. The effectiveness of neck stretching exercises following total thyroidectomy on reducing neck pain and disability: a randomized controlled trial. Worldviews Evid Based Nurs. 2016;13(3):224–31.
Fernandez-de-Las-Penas C, Alonso-Blanco C, Cuadrado ML, Pareja JA. Myofascial trigger points in the suboccipital muscles in episodic tension-type headache. Man Ther. 2006;11(3):225–30.
Andrieu G, Amrouni H, Robin E, Carnaille B, Wattier JM, Pattou F, Vallet B, Lebuffe G. Analgesic efficacy of bilateral superficial cervical plexus block administered before thyroid surgery under general anaesthesia. Br J Anaesth. 2007;99(4):561–6.
Dieudonne N, Gomola A, Bonnichon P, Ozier YM. Prevention of postoperative pain after thyroid surgery: a double-blind randomized study of bilateral superficial cervical plexus blocks. Anesth Analg. 2001;92(6):1538–42.
Shih ML, Duh QY, Hsieh CB, Liu YC, Lu CH, Wong CS, Yu JC, Yeh CC. Bilateral superficial cervical plexus block combined with general anesthesia administered in thyroid operations. World J Surg. 2010;34(10):2338–43.
Eti Z, Irmak P, Gulluoglu BM, Manukyan MN, Gogus FY. Does bilateral superficial cervical plexus block decrease analgesic requirement after thyroid surgery? Anesth Analg. 2006;102(4):1174–6.
Steffen T, Warschkow R, Brandle M, Tarantino I, Clerici T. Randomized controlled trial of bilateral superficial cervical plexus block versus placebo in thyroid surgery. Br J Surg. 2010;97(7):1000–6.
Pandit JJ, Bree S, Dillon P, Elcock D, McLaren ID, Crider B. A comparison of superficial versus combined (superficial and deep) cervical plexus block for carotid endarterectomy: a prospective, randomized study. Anesth Analg. 2000;91(4):781–6.
Pandit JJ, Satya-Krishna R, Gration P. Superficial or deep cervical plexus block for carotid endarterectomy: a systematic review of complications. Br J Anaesth. 2007;99(2):159–69.
Stoneham MD, Doyle AR, Knighton JD, Dorje P, Stanley JC. Prospective, randomized comparison of deep or superficial cervical plexus block for carotid endarterectomy surgery. Anesthesiology. 1998;89(4):907–12.
Wagstaff AJ, Bryson HM. Tizanidine. A review of its pharmacology, clinical efficacy and tolerability in the management of spasticity associated with cerebral and spinal disorders. Drugs. 1997;53(3):435–52.
Funding
None declared.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
About this article
Cite this article
Ahiskalioglu, A., Yayik, A.M., Oral Ahiskalioglu, E. et al. Ultrasound-guided bilateral superficial cervical block and preemptive single-dose oral tizanidine for post-thyroidectomy pain: a randomized-controlled double-blind study. J Anesth 32, 219–226 (2018). https://doi.org/10.1007/s00540-018-2468-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-018-2468-x