Abstract
Background
After initial pancreatic resection, local recurrence of pancreatic cancer (PC) or new primary PC can develop in the remnant. There are limited data available regarding this so-called remnant PC. The aim of this retrospective study was to clarify the clinical features and establish a treatment strategy for remnant PC.
Methods
A multicenter retrospective study with the Kyushu Study Group of Clinical Cancer was carried out. Clinical data from 50 patients who developed remnant PC were analyzed. RAS mutation analysis of the initial tumor and of remnant PC was performed in 17 cases.
Results
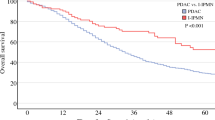
The initial pancreatic resections were performed for 37 invasive ductal carcinomas, and for 13 other tumors. Thirty-seven patients underwent a second pancreatectomy for remnant PC (resected group), while thirteen patients were not operated (unresected group). The median overall survival times were 42.2 months in the resected group and 12.3 months in the unresected group (HR 0.374; 95% CI 0.17–0.83). In RAS mutation analysis, 14 cases had at least 1 missense variant of KRAS, HRAS, or NRAS in the initial pancreatic tumor and/or remnant PC. The same missense variants between the initial tumor and remnant PC were discovered only in KRAS of one patient, and in HRAS of one patient. No case had completely consistent missense variants between the initial tumor and remnant PC.
Conclusions
This study found that repeated pancreatectomy for remnant PC can prolong patient survival, and RAS mutation analysis indicated that many remnant PCs are developed from metachronous multifocal origins.



Similar content being viewed by others
References
Miyata H, Gotoh M, Hirai I, et al. A pancreaticoduodenectomy risk model derived from 8575 cases from a national single-race population (Japanese) using a web-based data entry system: the 30-day and in-hospital mortality rates for pancreaticoduodenectomy. Ann Surg. 2014;259:773–80.
Uesaka K, Boku N, Fukutomi A, et al. Adjuvant chemotherapy of S-1 versus gemcitabine for resected pancreatic cancer: a phase 3, open-label, randomised, non-inferiority trial (JASPAC 01). Lancet. 2016;388:248–57.
Otsubo T, Kobayashi S, Sano K, et al. Safety-related outcomes of the Japanese Society of Hepato-Biliary-Pancreatic Surgery board certification system for expert surgeons. J Hepatobiliary Pancreat Sci. 2017;24:252–61.
Garcea G, Dennison AR, Pattenden CJ, et al. Survival following curative resection for pancreatic ductal adenocarcinoma. A systematic review of the literature. JOP. 2008;9:99–132.
Smeenk HG, Incrocci L, Kazemier G, et al. Adjuvant 5-FU-based chemoradiotherapy for patients undergoing R-1/R-2 resections for pancreatic cancer. Dig Surg. 2005;22:321–8.
Smeenk HG, Tran TC, Erdmann J, et al. Survival after surgical management of pancreatic adenocarcinoma: does curative and radical surgery truly exist? Langenbecks Arch Surg. 2005;390:94–103.
Kleeff J, Reiser C, Hinz U, et al. Surgery for recurrent pancreatic ductal adenocarcinoma. Ann Surg. 2007;245:566–72.
Hashimoto D, Chikamoto A, Masuda T, et al. Pancreatic cancer arising from the remnant pancreas: is it a local recurrence or new primary lesion? Pancreas. 2017;46:1083–90.
Hashimoto D, Chikamoto A, Ohmuraya M, et al. Pancreatic cancer in the remnant pancreas following primary pancreatic resection. Surg Today. 2014;44:1313–20.
Müller MW, Friess H, Kleeff J, et al. Is there still a role for total pancreatectomy? Ann Surg. 2007;246:966–74 (discussion#).
Thomas RM, Truty MJ, Nogueras-Gonzalez GM, et al. Selective reoperation for locally recurrent or metastatic pancreatic ductal adenocarcinoma following primary pancreatic resection. J Gastrointest Surg. 2012;16:1696–704.
Strobel O, Hartwig W, Hackert T, et al. Re-resection for isolated local recurrence of pancreatic cancer is feasible, safe, and associated with encouraging survival. Ann Surg Oncol. 2013;20:964–72.
Miyazaki M, Yoshitomi H, Shimizu H, et al. Repeat pancreatectomy for pancreatic ductal cancer recurrence in the remnant pancreas after initial pancreatectomy: is it worthwhile? Surgery. 2014;155:58–66.
Shima Y, Okabayashi T, Kozuki A, et al. Completion pancreatectomy for recurrent pancreatic cancer in the remnant pancreas: report of six cases and a review of the literature. Langenbecks Arch Surg. 2015;400:973–8.
Nakagawa M, Choi YY, An JY, et al. Staging for remnant gastric cancer: the metastatic lymph node ratio vs the UICC 7th edition system. Ann Surg Oncol. 2016;23:4322–31.
Qi X, Zhao Y, Li H, et al. Management of hepatocellular carcinoma: an overview of major findings from meta-analyses. Oncotarget. 2016;7:34703–51.
Renehan AG, Egger M, Saunders MP, et al. Impact on survival of intensive follow up after curative resection for colorectal cancer: systematic review and meta-analysis of randomised trials. BMJ. 2002;324:813.
Nakata M, Sawada S, Yamashita M, et al. Surgical treatments for multiple primary adenocarcinoma of the lung. Ann Thorac Surg. 2004;78:1194–9.
Miura F, Takada T, Amano H, et al. Repeated pancreatectomy after pancreatoduodenectomy. J Gastrointest Surg. 2007;11:179–86.
Ishida J, Toyama H, Matsumoto I, et al. Second primary pancreatic ductal carcinoma in the remnant pancreas after pancreatectomy for pancreatic ductal carcinoma: high cumulative incidence rates at 5 years after pancreatectomy. Pancreatology. 2016;16:615–20.
Lavu H, Nowcid LJ, Klinge MJ, et al. Reoperative completion pancreatectomy for suspected malignant disease of the pancreas. J Surg Res. 2011;170:89–95.
Hashimoto D, Arima K, Yokoyama N, et al. Heterogeneity of KRAS mutations in pancreatic ductal adenocarcinoma. Pancreas. 2016;45:1111–4.
Yamada S, Kobayashi A, Nakamori S, et al. Resection for recurrent pancreatic cancer in the remnant pancreas after pancreatectomy is clinically promising: results of a project study for pancreatic surgery by the Japanese Society of Hepato-Biliary-Pancreatic Surgery. Surgery. 2018;164:1049–56.
Bassi C, Marchegiani G, Dervenis C, et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery. 2017;161:584–91.
Cancer IUA: TNM Classification of Malignant Tumours. 7th ed. New York: Wiley-Blackwell; 2009.
Oettle H, Post S, Neuhaus P, et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA. 2007;297:267–77.
Oettle H, Neuhaus P, Hochhaus A, et al. Adjuvant chemotherapy with gemcitabine and long-term outcomes among patients with resected pancreatic cancer: the CONKO-001 randomized trial. JAMA. 2013;310:1473–81.
Ueno H, Kosuge T, Matsuyama Y, et al. A randomised phase III trial comparing gemcitabine with surgery-only in patients with resected pancreatic cancer: Japanese Study Group of Adjuvant Therapy for Pancreatic Cancer. Br J Cancer. 2009;101:908–15.
Yamaguchi K, Okusaka T, Shimizu K, et al. Clinical practice guidelines for pancreatic cancer 2016 from the Japan Pancreas Society: a synopsis. Pancreas. 2017;46:595–604.
Conroy T, Desseigne F, Ychou M, et al. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. N Engl J Med. 2011;364:1817–25.
Von Hoff DD, Ervin T, Arena FP, et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. N Engl J Med. 2013;369:1691–703.
Brune K, Abe T, Canto M, et al. Multifocal neoplastic precursor lesions associated with lobular atrophy of the pancreas in patients having a strong family history of pancreatic cancer. Am J Surg Pathol. 2006;30:1067–76.
Matsuda Y, Furukawa T, Yachida S, et al. The prevalence and Clinicopathological characteristics of high-grade pancreatic intraepithelial neoplasia: Autopsy Study evaluating the entire pancreatic parenchyma. Pancreas. 2017;46:658–64.
Tempero M, Malafa M, Al-Hawary M, et al. Pancreatic adenocarcinoma, version 2.2017, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 2017;15:1028–61.
Heinrich S, Pestalozzi B, Lesurtel M, et al. Adjuvant gemcitabine versus neoadjuvant gemcitabine/oxaliplatin plus adjuvant gemcitabine in resectable pancreatic cancer: a randomized multicenter phase III study (NEOPAC study). BMC Cancer. 2011;11:346.
Billings BJ, Christein JD, Harmsen WS, et al. Quality-of-life after total pancreatectomy: is it really that bad on long-term follow-up? J Gastrointest Surg. 2005;9:1059–66 (discussion#).
Acknowledgements
The authors thank the following institutions and investigators who participated in this study: Miyake K (Kumamoto University), Yonemura A (Kumamoto University), Yoshida M (Kumamoto University), Utsunomiya T (Oita Prefectural Hospital), Eguchi S (Nagasaki University Hospital), Kawanaka H (Beppu Medical Center), Kusumoto T (Kyusyu Medical Cnter), Okumura H (Kagoshima Koseiren Hospital). We also thank Sakamoto S and the staff at the Clinical Research Support Center Kyushu (CReS Kyushu) for their excellent data collection, management, and secretarial assistance. This work was supported by CReS Kyushu with no funding. We thank Maki S for grammatical editing of a draft of this manuscript.
Funding
No financial support or funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict to interest
Hashimoto D and all co-authors have no conflict to interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hashimoto, D., Arima, K., Nakagawa, S. et al. Pancreatic cancer arising from the remnant pancreas after pancreatectomy: a multicenter retrospective study by the Kyushu Study Group of Clinical Cancer. J Gastroenterol 54, 437–448 (2019). https://doi.org/10.1007/s00535-018-01535-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-018-01535-9