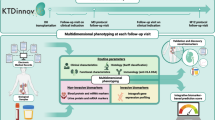
Abstract
Non-invasive technologies to monitor kidney allograft health utilizing high-throughput assays of blood and urine specimens are emerging out of the research realm and slowly becoming part of everyday clinical practice. HLA epitope analysis and eplet mismatch score determination promise a more refined approach to the pre-transplant recipient–donor HLA matching that may lead to reduced rejection risk. High-resolution HLA typing and multiplex single antigen bead assays are identifying potential new offending HLA antibody subtypes. There is increasing recognition of the deleterious role non-HLA antibodies play in post-transplant outcomes. Donor-derived cell-free DNA detected by next-generation sequencing is a promising biomarker for kidney transplant rejection. Multi-omics techniques are shedding light on discrete genomic, transcriptomic, proteomic, and metabolomic signatures that correlate with and predict allograft outcomes. Over the next decade, a comprehensive approach to optimize kidney matching and monitor transplant recipients for acute and chronic graft dysfunction will likely involve a combination of those emerging technologies summarized in this review.

Similar content being viewed by others
References
Dharnidharka VR, Fiorina P, Harmon WE (2014) Kidney transplantation in children. N Engl J Med 371:549–558
Paul LC (2001) Immunologic risk factors for chronic renal allograft dysfunction. Transplantation 71(11 Suppl):SS17–SS23
Ashoor IF, Dharnidharka VR (2019) Non-immunologic allograft loss in pediatric kidney transplant recipients. Pediatr Nephrol 34:211–222
Foster BJ (2015) Heightened graft failure risk during emerging adulthood and transition to adult care. Pediatr Nephrol 30:567–576
Chua A, Cramer C, Moudgil A, Martz K, Smith J, Blydt-Hansen T, Neu A, Dharnidharka VR, NAPRTCS investigators (2019) Kidney transplant practice patterns and outcome benchmarks over 30 years: the 2018 report of the NAPRTCS. Pediatr Transplant 23:e13597
Wiebe C, Pochinco D, Blydt-Hansen TD, Ho J, Birk PE, Karpinski M, Goldberg A, Storsley LJ, Gibson IW, Rush DN, Nickerson PW (2013) Class II HLA epitope matching – a strategy to minimize de novo donor-specific antibody development and improve outcomes. Am J Transplant 13:3114–3122
Sharma A, Taverniti A, Graf N, Teixeira-Pinto A, Lewis JR, Lim WH, Alexander SI, Durkan A, Craig JC, Wong G (2020) The association between human leukocyte antigen eplet mismatches, de novo donor-specific antibodies, and the risk of acute rejection in pediatric kidney transplant recipients. Pediatr Nephrol 35:1061–1068
Philogene MC, Amin A, Zhou S, Charnaya O, Vega R, Desai N, Neu AM, Pruette CS (2020) Eplet mismatch analysis and allograft outcome across racially diverse groups in a pediatric transplant cohort: a single-center analysis. Pediatr Nephrol 35:83–94
Kausman JY, Walker AM, Cantwell LS, Quinlan C, Sypek MP, Ierino FL (2016) Application of an epitope-based allocation system in pediatric kidney transplantation. Pediatr Transplant 20:931–938
Bryan CF, Chadha V, Warady BA (2016) Donor selection in pediatric kidney transplantation using DR and DQ eplet mismatching: a new histocompatibility paradigm. Pediatr Transplant 20:926–930
Bjerre A, Tangeraas T, Heidecke H, Dragun D, Dechend R, Staff AC (2016) Angiotensin II type 1 receptor antibodies in childhood kidney transplantation. Pediatr Transplant 20:627–632
Fichtner A, Süsal C, Schröder C, Höcker B, Rieger S, Waldherr R, Westhoff JH, Sander A, Dragun D, Tönshoff B (2018) Association of angiotensin II type 1 receptor antibodies with graft histology, function and survival in paediatric renal transplant recipients. Nephrol Dial Transplant 33:1065–1072
Hesemann LE, Subramanian V, Mohanakumar T, Dharnidharka VR (2015) De novo development of antibodies to kidney-associated self-antigens angiotensin II receptor type I, collagen IV, and fibronectin occurs at early time points after kidney transplantation in children. Pediatr Transplant 19:499–503
Pearl MH, Zhang Q, Palma Diaz MF, Grotts J, Rossetti M, Elashoff D, Gjertson DW, Weng P, Reed EF, Tsai Chambers E (2018) Angiotensin II type 1 receptor antibodies are associated with inflammatory cytokines and poor clinical outcomes in pediatric kidney transplantation. Kidney Int 93:260–269
Pearl MH, Reed EF (2019) Angiotensin II type I receptor antibodies in pediatric solid organ transplant. Hum Immunol 80:568–572
Puliyanda DP, Swinford R, Pizzo H, Garrison J, De Golovine AM, Jordan SC (2020) Donor-derived cell-free DNA (dd-cfDNA) for detection of allograft rejection in pediatric kidney transplants. Pediatr Transplant 2020:e13850
Roedder S, Sigdel T, Salomonis N, Hsieh S, Dai H, Bestard O, Metes D, Zeevi A, Gritsch A, Cheeseman J, Macedo C, Peddy R, Medeiros M, Vincenti F, Asher N, Salvatierra O, Shapiro R, Kirk A, Reed EF, Sarwal MM (2014) The kSORT assay to detect renal transplant patients at high risk for acute rejection: results of the multicenter AART study. PLoS Med 11:e1001759
ClinicalTrials.gov. VIRTUUS Children's Study. [cited 2020 November 21]; Available from: https://clinicaltrials.gov/ct2/show/NCT03719339
Mockler C, Sharma A, Gibson IW, Gao A, Wong A, Ho J, Blydt-Hansen TD (2018) The prognostic value of urinary chemokines at 6 months after pediatric kidney transplantation. Pediatr Transplant 22:e13205
Kanzelmeyer NK, Zürbig P, Mischak H, Metzger J, Fichtner A, Ruszai KH, Seemann T, Hansen M, Wygoda S, Krupka K, Tönshoff B, Melk A, Pape L (2019) Urinary proteomics to diagnose chronic active antibody-mediated rejection in pediatric kidney transplantation – a pilot study. Transpl Int 32:28–37
Blydt-Hansen TD, Sharma A, Gibson IW, Mandal R, Wishart DS (2014) Urinary metabolomics for noninvasive detection of borderline and acute T cell-mediated rejection in children after kidney transplantation. Am J Transplant 14:2339–2349
Blydt-Hansen TD, Sharma A, Gibson IW, Wishart DS, Mandal R, Ho J, Nickerson P, Rush D (2017) Urinary metabolomics for noninvasive detection of antibody-mediated rejection in children after kidney transplantation. Transplantation 101:2553–2561
Ahlenstiel-Grunow T, Pape L (2020) Virus-specific T cells in pediatric renal transplantation. Pediatr Nephrol. https://doi.org/10.1007/s00467-020-04522-6
Townamchai N, Safa K, Chandraker A (2013) Immunologic monitoring in kidney transplant recipients. Kidney Res Clin Pract 32:52–61. https://doi.org/10.1016/j.krcp.2013.04.002
Larkins NG, Wong G, Taverniti A, Lim WH (2019) Epitope matching in kidney transplantation: recent advances and current limitations. Curr Opin Organ Transplant 24:370–377
Sypek M, Kausman J, Holt S, Hughes P (2018) HLA epitope matching in kidney transplantation: an overview for the general nephrologist. Am J Kidney Dis 71:720–731
Senev A, Coemans M, Lerut E, Van Sandt V, Kerkhofs J, Daniëls L, Driessche MV, Compernolle V, Sprangers B, Van Loon E, Callemeyn J, Claas F, Tambur AR, Verbeke G, Kuypers D, Emonds MP, Naesens M (2020) Eplet mismatch load and De novo occurrence of donor-specific anti-HLA antibodies, rejection, and graft failure after kidney transplantation: an observational cohort study. J Am Soc Nephrol 31:2193–2204. https://doi.org/10.1681/ASN.2020010019
Dankers MK, Witvliet MD, Roelen DL, de Lange P, Korfage N, Persijn GG, Duquesnoy R, Doxiadis II, Claas FH (2004) The number of amino acid triplet differences between patient and donor is predictive for the antibody reactivity against mismatched human leukocyte antigens. Transplantation 77:1236–1239
Sapir-Pichhadze R, Tinckam K, Quach K, Logan AG, Laupacis A, John R, Beyene J, Kim SJ (2015) HLA-DR and -DQ eplet mismatches and transplant glomerulopathy: a nested case–control study. Am J Transplant 15:137–148
Wiebe C, Nevins TE, Robiner WN, Thomas W, Matas AJ, Nickerson PW (2015) The synergistic effect of class II HLA epitope-mismatch and nonadherence on acute rejection and graft survival. Am J Transplant 15:2197–2202
Tafulo S, Malheiro J, Santos S, Dias L, Almeida M, Martins LS, Pedroso S, Mendes C, Lobato L, Castro-Henriques A (2019) Degree of HLA class II eplet mismatch load improves prediction of antibody-mediated rejection in living donor kidney transplantation. Hum Immunol 80:966–975
Sapir-Pichhadze R, Zhang X, Ferradji A, Madbouly A, Tinckam KJ, Gebel HM, Blum D, Marrari M, Kim SJ, Fingerson S, Bashyal P, Cardinal H, Foster BJ (2020) Epitopes as characterized by antibody-verified eplet mismatches determine risk of kidney transplant loss. Kidney Int 97:778–785
Geneugelijk K, Spierings E (2018) Matching donor and recipient based on predicted indirectly recognizable human leucocyte antigen epitopes. Int J Immunogenet 45:41–53
Geneugelijk K, Spierings E (2020) PIRCHE-II: an algorithm to predict indirectly recognizable HLA epitopes in solid organ transplantation. Immunogenetics 72:119–129
National Kidney Registry. Kidney for Life Program. [cited 2020 November 21]; Available from: https://www.kidneyforlife.org/
Syed B, Augustine JJ (2020) The National Kidney Registry: time to buy in? Clin J Am Soc Nephrol 15:168–170
Tassone G, De Santis D, Vukovic I, Downing J, Martinez OP, D'Orsogna LJ (2020) Different eplet software programs give discordant and incorrect results: an analysis of HLAMatchmaker vs fusion Matchmaker Eplet calling software. HLA 96:52–63
Patel R, Terasaki PI (1969) Significance of the positive crossmatch test in kidney transplantation. N Engl J Med 280:735–739
Mulley WR, Kanellis J (2011) Understanding crossmatch testing in organ transplantation: a case-based guide for the general nephrologist. Nephrology (Carlton) 16:125–133
Carta P, Di Maria L, Caroti L, Buti E, Antognoli G, Minetti EE (2015) Anti-human leukocyte antigen DQ antibodies in renal transplantation: are we underestimating the most frequent donor specific alloantibodies? Transplant Rev (Orlando) 29:135–138
Cross AR, Lion J, Loiseau P, Charron D, Taupin JL, Glotz D, Mooney N (2016) Donor specific antibodies are not only directed against HLA-DR: minding your Ps and Qs. Hum Immunol 77:1092–1100
Ling M, Marfo K, Masiakos P, Aljanabi A, Lindower J, Glicklich D, de Boccardo G, Greenstein S, Chapochnick-Friedmann J, Kayler L, Kinkhabwala M, Akalin E (2012) Pretransplant anti-HLA-Cw and anti-HLA-DP antibodies in sensitized patients. Hum Immunol 73:879–883
Qiu J, Cai J, Terasaki PI, El-Awar N, Lee JH (2005) Detection of antibodies to HLA-DP in renal transplant recipients using single antigen beads. Transplantation 80:1511–1513
Hörmann M, Dieplinger G, Rebellato LM, Briley KP, Bolin P, Morgan C, Haisch CE, Everly MJ (2016) Incidence and impact of anti-HLA-DP antibodies in renal transplantation. Clin Transpl 30:1108–1114
Bachelet T, Martinez C, Del Bello A, Couzi L, Kejji S, Guidicelli G, Lepreux S, Visentin J, Congy-Jolivet N, Rostaing L, Taupin JL, Kamar N, Merville P (2016) Deleterious impact of donor-specific anti-HLA antibodies toward HLA-Cw and HLA-DP in kidney transplantation. Transplantation 100:159–166
Daniëls L, Claas FHJ, Kramer CSM, Senev A, Vanden Driessche M, Emonds MP, Van Laecke S, Hellemans R, Abramowicz D, Naesens M (2020) The role of HLA-DP mismatches and donor specific HLA-DP antibodies in kidney transplantation: a case series. Transpl Immunol. https://doi.org/10.1016/j.trim.2020.101287
Zhang Q, Reed EF (2016) The importance of non-HLA antibodies in transplantation. Nat Rev Nephrol 12:484–495
Dragun D, Müller DN, Bräsen JH, Fritsche L, Nieminen-Kelhä M, Dechend R, Kintscher U, Rudolph B, Hoebeke J, Eckert D, Mazak I, Plehm R, Schönemann C, Unger T, Budde K, Neumayer HH, Luft FC, Wallukat G (2005) Angiotensin II type 1-receptor activating antibodies in renal-allograft rejection. N Engl J Med 352:558–569
Zou Y, Stastny P, Süsal C, Döhler B, Opelz G (2007) Antibodies against MICA antigens and kidney-transplant rejection. N Engl J Med 357:1293–1300
Delville M, Lamarthée B, Pagie S, See SB, Rabant M, Burger C, Gatault P, Giral M, Thaunat O, Arzouk N, Hertig A, Hazzan M, Matignon M, Mariat C, Caillard S, Kamar N, Sayegh J, Westeel PF, Garrouste C, Ladrière M, Vuiblet V, Rivalan J, Merville P, Bertrand D, Le Moine A, Duong Van Huyen JP, Cesbron A, Cagnard N, Alibeu O, Satchell SC, Legendre C, Zorn E, Taupin JL, Charreau B, Anglicheau D (2019) Early acute microvascular kidney transplant rejection in the absence of anti-HLA antibodies is associated with preformed IgG antibodies against diverse glomerular endothelial cell antigens. J Am Soc Nephrol 30:692–709
Philogene MC, Zhou S, Lonze BE, Bagnasco S, Alasfar S, Montgomery RA, Kraus E, Jackson AM, Leffell MS, Zachary AA (2018) Pre-transplant screening for non-HLA antibodies: who should be tested? Hum Immunol 79:195–202
Deltombe C, Gillaizeau F, Anglicheau D, Morelon E, Trébern-Launay K, Le Borgne F, Rimbert M, Guérif P, Malard-Castagnet S, Foucher Y, Giral M (2017) Is pre-transplant sensitization against angiotensin II type 1 receptor still a risk factor of graft and patient outcome in kidney transplantation in the anti-HLA Luminex era? A retrospective study. Transpl Int 30:1150–1160
Pinelli DF, Friedewald JJ, Haarberg KMK, Radhakrishnan SL, Zitzner JR, Hanshew WE, Tambur AR (2017) Assessing the potential of angiotensin II type 1 receptor and donor specific anti-endothelial cell antibodies to predict long-term kidney graft outcome. Hum Immunol 78:421–427
Banasik M, Boratyńska M, Kościelska-Kasprzak K, Kamińska D, Bartoszek D, Zabińska M, Myszka M, Zmonarski S, Protasiewicz M, Nowakowska B, Hałoń A, Chudoba P, Klinger M (2014) The influence of non-HLA antibodies directed against angiotensin II type 1 receptor (AT1R) on early renal transplant outcomes. Transpl Int 27:1029–1038
Lefaucheur C, Viglietti D, Bouatou Y, Philippe A, Pievani D, Aubert O, Duong Van Huyen JP, Taupin JL, Glotz D, Legendre C, Loupy A, Halloran PF, Dragun D (2019) Non-HLA agonistic anti-angiotensin II type 1 receptor antibodies induce a distinctive phenotype of antibody-mediated rejection in kidney transplant recipients. Kidney Int 96:189–201
Cuevas E, Arreola-Guerra JM, Hernández-Méndez EA, Salcedo I, Castelán N, Uribe-Uribe NO, Vilatobá M, Contreras-Saldívar AG, Sánchez-Cedillo AI, Ramírez JB, de Rungs D, Granados J, Morales-Buenrostro LE, Alberú J (2016) Pretransplant angiotensin II type 1-receptor antibodies are a risk factor for earlier detection of de novo HLA donor-specific antibodies. Nephrol Dial Transplant 31:1738–1745
Carroll RP, Deayton S, Emery T, Munasinghe W, Tsiopelas E, Fleet A, Lake M, Humphreys I, Jalalonmuhali M, Coates P (2019) Proactive treatment of angiotensin receptor antibodies in kidney transplantation with plasma exchange and/or candesartan is safe and associated with excellent graft survival at 4 years: a single centre Australian experience. Hum Immunol 80:573–578
Hart A, Smith JM, Skeans MA, Gustafson SK, Wilk AR, Castro S, Foutz J, Wainright JL, Snyder JJ, Kasiske BL, Israni AK (2020) OPTN/SRTR 2018 annual data report: kidney. Am J Transplant 20(Suppl s1):20–130
Colvin RB, Smith RN (2005) Antibody-mediated organ-allograft rejection. Nat Rev Immunol 5:807–817
Bloom RD, Bromberg JS, Poggio ED, Bunnapradist S, Langone AJ, Sood P, Matas AJ, Mehta S, Mannon RB, Sharfuddin A, Fischbach B, Narayanan M, Jordan SC, Cohen D, Weir MR, Hiller D, Prasad P, Woodward RN, Grskovic M, Sninsky JJ, Yee JP, Brennan DC, Circulating Donor-Derived Cell-Free DNA in Blood for Diagnosing Active Rejection in Kidney Transplant Recipients (DART) Study Investigators (2017) Cell-free DNA and active rejection in kidney allografts. J Am Soc Nephrol 28:2221–2232
Erpicum P, Hanssen O, Weekers L, Lovinfosse P, Meunier P, Tshibanda L, Krzesinski JM, Hustinx R, Jouret F (2017) Non-invasive approaches in the diagnosis of acute rejection in kidney transplant recipients, part II: omics analyses of urine and blood samples. Clin Kidney J 10:106–115
Beck J, Bierau S, Balzer S, Andag R, Kanzow P, Schmitz J, Gaedcke J, Moerer O, Slotta JE, Walson P, Kollmar O, Oellerich M, Schütz E (2013) Digital droplet PCR for rapid quantification of donor DNA in the circulation of transplant recipients as a potential universal biomarker of graft injury. Clin Chem 59:1732–1741
Knight SR, Thorne A, Lo Faro ML (2019) Donor-specific cell-free DNA as a biomarker in solid organ transplantation. A systematic review. Transplantation 103:273–283
Suzuki N, Kamataki A, Yamaki J, Homma Y (2008) Characterization of circulating DNA in healthy human plasma. Clin Chim Acta 387:55–58
Jahr S, Hentze H, Englisch S, Hardt D, Fackelmayer FO, Hesch RD, Knippers R (2001) DNA fragments in the blood plasma of cancer patients: quantitations and evidence for their origin from apoptotic and necrotic cells. Cancer Res 61:1659–1665
Stroun M, Lyautey J, Lederrey C, Olson-Sand A, Anker P (2001) About the possible origin and mechanism of circulating DNA: apoptosis and active DNA release. Clin Chim Acta 313:139–142
Lui YY, Woo KS, Wang AY, Yeung CK, Li PK, Chau E, Ruygrok P, Lo YM (2003) Origin of plasma cell-free DNA after solid organ transplantation. Clin Chem 49:495–496
Jordan SC, Bunnapradist S, Bromberg JS, Langone AJ, Hiller D, Yee JP, Sninsky JJ, Woodward RN, Matas AJ (2018) Donor-derived cell-free DNA identifies antibody-mediated rejection in donor specific antibody positive kidney transplant recipients. Transplant Direct 4:e379
Stites E, Kumar D, Olaitan O, John Swanson S, Leca N, Weir M, Bromberg J, Melancon J, Agha I, Fattah H, Alhamad T, Qazi Y, Wiseman A, Gupta G (2020) High levels of dd-cfDNA identify patients with TCMR 1A and borderline allograft rejection at elevated risk of graft injury. Am J Transplant 20:2491–2498
Moreira VG, García BP, Baltar Martín JM, Suárez FO, Alvarez FV (2009) Cell-free DNA as a noninvasive acute rejection marker in renal transplantation. Clin Chem 55:1958–1966
Grskovic M, Hiller DJ, Eubank LA, Sninsky JJ, Christopherson C, Collins JP, Thompson K, Song M, Wang YS, Ross D, Nelles MJ, Yee JP, Wilber JC, Crespo-Leiro MG, Scott SL, Woodward RN (2016) Validation of a clinical-grade assay to measure donor-derived cell-free DNA in solid organ transplant recipients. J Mol Diagn 18:890–902
Altuğ Y, Liang N, Ram R, Ravi H, Ahmed E, Brevnov M, Swenerton RK, Zimmermann B, Malhotra M, Demko ZP, Billings PR, Ryan A (2019) Analytical validation of a single-nucleotide polymorphism-based donor-derived cell-free DNA assay for detecting rejection in kidney transplant patients. Transplantation 103:2657–2665
Li B, Hartono C, Ding R, Sharma VK, Ramaswamy R, Qian B, Serur D, Mouradian J, Schwartz JE, Suthanthiran M (2001) Noninvasive diagnosis of renal-allograft rejection by measurement of messenger RNA for perforin and granzyme B in urine. N Engl J Med 344:947–954
Suthanthiran M, Schwartz JE, Ding R, Abecassis M, Dadhania D, Samstein B, Knechtle SJ, Friedewald J, Becker YT, Sharma VK, Williams NM, Chang CS, Hoang C, Muthukumar T, August P, Keslar KS, Fairchild RL, Hricik DE, Heeger PS, Han L, Liu J, Riggs M, Ikle DN, Bridges ND, Shaked A, Clinical Trials in Organ Transplantation 04 (CTOT-04) Study Investigators (2013) Urinary-cell mRNA profile and acute cellular rejection in kidney allografts. N Engl J Med 369:20–31
Crespo E, Roedder S, Sigdel T, Hsieh SC, Luque S, Cruzado JM, Tran TQ, Grinyó JM, Sarwal MM, Bestard O (2017) Molecular and functional noninvasive immune monitoring in the ESCAPE study for prediction of subclinical renal allograft rejection. Transplantation 101:1400–1409
Van Loon E, Giral M, Anglicheau D, Lerut E, Dubois V, Rabeyrin M, Brouard S, Roedder S, Spigarelli MG, Rabant M, Bogaerts K, Naesens M, Thaunat O (2020) Diagnostic performance of kSORT, a blood-based mRNA assay for noninvasive detection of rejection after kidney transplantation: a retrospective multicenter cohort study. Am J Transplant. https://doi.org/10.1111/ajt.16179
Kaminski MM, Alcantar MA, Lape IT, Greensmith R, Huske AC, Valeri JA, Marty FM, Klämbt V, Azzi J, Akalin E, Riella LV, Collins JJ (2020) A CRISPR-based assay for the detection of opportunistic infections post-transplantation and for the monitoring of transplant rejection. Nat Biomed Eng 4:601–609
Dharnidharka VR, Malone A (2018) Biomarkers to detect rejection after kidney transplantation. Pediatr Nephrol 33:1113–1122
Ho J, Hirt-Minkowski P, Wilkins JA (2017) New developments in transplant proteomics. Curr Opin Nephrol Hypertens 26:229–234
Segerer S, Cui Y, Eitner F, Goodpaster T, Hudkins KL, Mack M, Cartron JP, Colin Y, Schlondorff D, Alpers CE (2001) Expression of chemokines and chemokine receptors during human renal transplant rejection. Am J Kidney Dis 37:518–531
Hirt-Minkowski P, Rush DN, Gao A, Hopfer H, Wiebe C, Nickerson PW, Schaub S, Ho J (2016) Six-month urinary CCL2 and CXCL10 levels predict long-term renal allograft outcome. Transplantation 100:1988–1996
Metzger J, Chatzikyrkou C, Broecker V, Schiffer E, Jaensch L, Iphoefer A, Mengel M, Mullen W, Mischak H, Haller H, Gwinner W (2011) Diagnosis of subclinical and clinical acute T-cell-mediated rejection in renal transplant patients by urinary proteome analysis. Proteomics Clin Appl 5:322–333
Suhre K, Schwartz JE, Sharma VK, Chen Q, Lee JR, Muthukumar T, Dadhania DM, Ding R, Ikle DN, Bridges ND, Williams NM, Kastenmüller G, Karoly ED, Mohney RP, Abecassis M, Friedewald J, Knechtle SJ, Becker YT, Samstein B, Shaked A, Gross SS, Suthanthiran M (2016) Urine metabolite profiles predictive of human kidney allograft status. J Am Soc Nephrol 27:626–636
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Answers:
1. C; 2. B; 3. C; 4. C; 5. B
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ehlayel, A., Simms, K.J.A. & Ashoor, I.F. Emerging monitoring technologies in kidney transplantation. Pediatr Nephrol 36, 3077–3087 (2021). https://doi.org/10.1007/s00467-021-04929-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-04929-9