Abstract
Background
Due to lacking evidence for confirming the efficacy of performing laparoscopic surgery for locally advanced gastric cancer (LAGC). Therefore, this study aimed to compare the static and dynamic failure patterns after laparoscopic gastrectomy (LG) and open gastrectomy (OG) in LAGC.
Methods
A total of 1792 LAGC patients who underwent radical resection between January 2010 and January 2017 were divided into the LG group (n = 1557) and the OG group (n = 235). Propensity score matching was performed to balance the two groups. Dynamic hazard rates of failure were calculated using the hazard function. Early and late failure were defined as failure occurring before and after 2 years since surgery, respectively.
Results
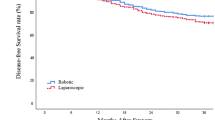
A total of 1175 patients with LAGC were included after matching (LG group, n = 940; OG, n = 235). The failure rate of the whole cohort was 43.2% (508/1175), accounting for 41.4% (389/940) and 50.6% (119/235) in the LG and OG groups, respectively. Although the two groups showed no significant differences in failure rate for any failure type, landmark analysis showed a lower early distant recurrence rate in the stage IIa–IIIb subgroup of the LG group (OG versus LG: 30.3% versus 21.1%, P = 0.004). The dynamic hazard rate peaked at 9.4 months (peak rate = 0.0186) before gradually declining. In stage IIa–IIIb patients, the hazard rate of the OG group remained significantly higher than that of the LG group within the first 2 years in terms of distant recurrence (peak rate: OG versus LG, 0.0091 versus 0.0055).
Conclusion
Given the differences in early failure between LG and OG, more intensive surveillance for distant recurrence within the first 2 years should be considered for patients with stage IIa–IIIb after OG.



Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author upon reasonable request.
References
Ferlay J, Soerjomataram I, Dikshit R et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386. https://doi.org/10.1002/ijc.29210
Kitano S, Iso Y, Moriyama M et al (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4(2):146–148
Kim W, Kim HH, Han SU et al (2016) Decreased morbidity of laparoscopic distal gastrectomy compared with open distal gastrectomy for stage I gastric cancer: short-term outcomes from a multicenter randomized controlled trial (KLASS-01). Ann Surg 263(1):28–35. https://doi.org/10.1097/SLA.0000000000001346
Katai H, Mizusawa J, Katayama H et al (2017) Short-term surgical outcomes from a phase III study of laparoscopy-assisted versus open distal gastrectomy with nodal dissection for clinical stage IA/IB gastric cancer: Japan Clinical Oncology Group Study JCOG0912. Gastric Cancer 20(4):699–708. https://doi.org/10.1007/s10120-016-0646-9
Katai H, Mizusawa J, Katayama H et al (2020) Survival outcomes after laparoscopy-assisted distal gastrectomy versus open distal gastrectomy with nodal dissection for clinical stage IA or IB gastric cancer (JCOG0912): a multicentre, non-inferiority, phase 3 randomised controlled trial. Lancet Gastroenterol Hepatol 5(2):142–151. https://doi.org/10.1016/S2468-1253(19)30332-2
Japanese gastric cancer treatment guidelines (2018) 5th edition. Gastric Cancer. https://doi.org/10.1007/s10120-020-01042-y
Azagra JS, Goergen M, De Simone P et al (1999) Minimally invasive surgery for gastric cancer. Surg Endosc 13(4):351–357. https://doi.org/10.1007/s004649900988
Ichiro U, Atsushi S, Junko F, Yoshiyuki K, Hideo M, Akitake H (1999) Laparoscopic total gastrectomy with distal pancreatosplenectomy and D2 lymphadenectomy for advanced gastric cancer. Gastric Cancer 2(4):230–234. https://doi.org/10.1007/s101200050069
Wang F-H, Shen L, Li J et al (2019) The Chinese Society of Clinical Oncology (CSCO): clinical guidelines for the diagnosis and treatment of gastric cancer. Cancer Commun (Lond) 39(1):10. https://doi.org/10.1186/s40880-019-0349-9
Hu Y, Huang C, Sun Y et al (2016) Morbidity and mortality of laparoscopic versus open D2 distal gastrectomy for advanced gastric cancer: a randomized controlled trial. J Clin Oncol 34(12):1350–1357. https://doi.org/10.1200/JCO.2015.63.7215
Lee H-J, Hyung WJ, Yang H-K et al (2019) Short-term outcomes of a multicenter randomized controlled trial comparing laparoscopic distal gastrectomy with D2 lymphadenectomy to open distal gastrectomy for locally advanced gastric cancer (KLASS-02-RCT). Ann Surg 270(6):983–991. https://doi.org/10.1097/SLA.0000000000003217
Inaki N, Etoh T, Ohyama T et al (2015) A multi-institutional, prospective, phase II feasibility study of laparoscopy-assisted distal gastrectomy with D2 lymph node dissection for locally advanced gastric cancer (JLSSG0901). World J Surg 39(11):2734–2741. https://doi.org/10.1007/s00268-015-3160-z
Yu J, Huang C, Sun Y et al (2019) Effect of laparoscopic vs open distal gastrectomy on 3-year disease-free survival in patients with locally advanced gastric cancer: the CLASS-01 randomized clinical trial. JAMA 321(20):1983–1992. https://doi.org/10.1001/jama.2019.5359
Hyung WJ, Yang H-K, Park Y-K et al (2020) Long-term outcomes of laparoscopic distal gastrectomy for locally advanced gastric cancer: the KLASS-02-RCT randomized clinical trial. J Clin Oncol. https://doi.org/10.1200/JCO.20.01210
Peacock O, Waters PS, Bressel M et al (2019) Prognostic factors and patterns of failure after surgery for T4 rectal cancer in the beyond total mesorectal excision era. Br J Surg 106(12):1685–1696. https://doi.org/10.1002/bjs.11242
Huber PM, Afzal N, Arya M et al (2020) Prostate specific antigen criteria to diagnose failure of cancer control following focal therapy of nonmetastatic prostate cancer using high intensity focused ultrasound. J Urol. https://doi.org/10.1097/JU.0000000000000747
Acharya S, Esthappan J, Badiyan S et al (2016) Medically inoperable endometrial cancer in patients with a high body mass index (BMI): patterns of failure after 3-D image-based high dose rate (HDR) brachytherapy. Radiother Oncol 118(1):167–172. https://doi.org/10.1016/j.radonc.2015.12.019
Al-Halabi H, Sayegh K, Digamurthy SR et al (2015) Pattern of failure analysis in metastatic EGFR-mutant lung cancer treated with tyrosine kinase inhibitors to identify candidates for consolidation stereotactic body radiation therapy. J Thorac Oncol 10(11):1601–1607. https://doi.org/10.1097/JTO.0000000000000648
Robinson CG, DeWees TA, El Naqa IM et al (2013) Patterns of failure after stereotactic body radiation therapy or lobar resection for clinical stage I non-small-cell lung cancer. J Thorac Oncol 8(2):192–201. https://doi.org/10.1097/JTO.0b013e31827ce361
Chen X, Yu X, Chen J et al (2013) Analysis in early stage triple-negative breast cancer treated with mastectomy without adjuvant radiotherapy: patterns of failure and prognostic factors. Cancer 119(13):2366–2374. https://doi.org/10.1002/cncr.28085
Rajasooriyar C, Van Dyk S, Bernshaw D et al (2011) Patterns of failure and treatment-related toxicity in advanced cervical cancer patients treated using extended field radiotherapy with curative intent. Int J Radiat Oncol Biol Phys 80(2):422–428. https://doi.org/10.1016/j.ijrobp.2010.02.026
Association JGC (2011) Japanese classification of gastric carcinoma: 3rd English Edition. Gastric Cancer 14:101
Gao Z, Jiang K, Ye Y, Wang S (2018) Interpretation on Chinese surgeons’ consensus opinion for the definition of gastric stump cancer (version 2018). Zhonghua Wei Chang Wai Ke Za Zhi 21:486–490
Japanese Gastric Cancer A (2017) Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer 20(1):1–19
Amin MB, Edge S, Greene F et al (2017) AJCC cancer staging manual, 8th edn. Springer International Publishing, New York
Lai Ji Fu, Sungsoo K, Kiyeol K et al (2009) Prediction of recurrence of early gastric cancer after curative resection. Ann Surg Oncol 16(7):1896–1902. https://doi.org/10.1245/s10434-009-0473-x
D’Angelica M, Gonen M, Brennan MF et al (2004) Patterns of initial recurrence in completely resected gastric adenocarcinoma. Ann Surg 240(5):808–816. https://doi.org/10.1097/01.sla.0000143245.28656.15
Seo N, Han K, Hyung WJ et al (2020) Stratification of postsurgical computed tomography surveillance based on the extragastric recurrence of early gastric cancer. Ann Surg 272:319–325
Lee JH, Chang KK, Yoon C, Tang LH, Strong VE, Yoon SS (2018) Lauren histologic type is the most important factor associated with pattern of recurrence following resection of gastric adenocarcinoma. Ann Surg 267(1):105–113. https://doi.org/10.1097/SLA.0000000000002040
Lee JH, Nam B-H, Ryu KW et al (2015) Comparison of outcomes after laparoscopy-assisted and open total gastrectomy for early gastric cancer. Br J Surg 102:1500–1505
Kennedy GD, Rajamanickam V, O’connor ES, et al (2011) Optimizing surgical care of colon cancer in the older adult population. Ann Surg 253:508–514
Hess KR, Levin VA (2014) Getting more out of survival data by using the hazard function. Clin Cancer Res 20(6):1404–1409. https://doi.org/10.1158/1078-0432.CCR-13-2125
DeQuardo JR (1999) Landmark analysis of corpus callosum shape in schizophrenia. Biol Psychiatry 46(12):1712–1714. https://doi.org/10.1016/s0006-3223(99)00196-1
Wang J-B, Zhong Q, Chen Q-Y et al (2019) Well-designed retrospective study versus small-sample prospective study in research based on laparoscopic and open radical distal gastrectomy for advanced gastric cancer. Surg Endosc. https://doi.org/10.1007/s00464-019-07237-4
Li Z, Shan F, Ying X et al (2019) Assessment of laparoscopic distal gastrectomy after neoadjuvant chemotherapy for locally advanced gastric cancer: a randomized clinical trial. JAMA Surg. https://doi.org/10.1001/jamasurg.2019.3473
National Comprehensive Cancer Networks (NCCN) (2019) NCCN practice guidelines for gastric cancer. http://www.nccn.org/professionals/physician_gls/f_guidelines.asp. Retrieved 20 Dec 2019
Youn HG, An JY, Choi MG et al (2010) Recurrence after curative resection of early gastric cancer. Ann Surg Oncol 17(2):448–454. https://doi.org/10.1245/s10434-009-0772-2
Fields RC, Strong VE, Gönen M et al (2011) Recurrence and survival after pathologic complete response to preoperative therapy followed by surgery for gastric or gastrooesophageal adenocarcinoma. Br J Cancer 104(12):1840–1847. https://doi.org/10.1038/bjc.2011.175
Lee J-H, Kim H-I, Kim MG et al (2016) Recurrence of gastric cancer in patients who are disease-free for more than 5 years after primary resection. Surgery 159(4):1090–1098. https://doi.org/10.1016/j.surg.2015.11.002
Jin LX, Moses LE, Squires MH et al (2015) Factors associated with recurrence and survival in lymph node-negative gastric adenocarcinoma: a 7-institution study of the US Gastric Cancer Collaborative. Ann Surg 262(6):999–1005. https://doi.org/10.1097/SLA.0000000000001084
Acknowledgements
We wish to thank all colleagues and nurses who provided care to the patients in this study.
Funding
This study was funded by Joint Funds for the innovation of science and technology, Fujian Province (Grant Numbers: 2017Y9011, 2017Y9004, 2018Y9041); the second batch of special support funds for Fujian Province innovation and entrepreneurship talents (2016B013); Construction Project of Fujian Province Minimally Invasive Medical Center (No. [2017]171), Natural Science Foundation of Fujian Province (2019J01155), Fujian provincial science and technology innovation joint fund project plan (2018Y9005), and Fujian provincial health technology project (2019-ZQN-37).
Author information
Authors and Affiliations
Contributions
Conception/Design: CMH, CH Z, PL, JL, and DW. Collection and/or assembly of data: JL, DW, BBX, ZX, HLZ, JWX, JBW, JXL, PL, CHZ, and CMH. Data analysis and interpretation: JL, DW, BBX, ZX, HLZ, PL, CHZ, and CMH. Manuscript writing: JL, DW, BBX, PL, CHZ, and CMH. All authors have read and approved the final manuscript.
Corresponding authors
Ethics declarations
Disclosures
Jun Lu, Dong Wu, Bin-bin Xu, Zhen Xue, Hua-Long Zheng, Jian-Wei Xie, Jia-Bin Wang, Jian-Xian Lin, Ping Li, Chao-Hui Zheng, and Chang-Ming Huang have no conflicts of interest or financial ties to disclose.
Informed consent
This article does not report individual participants’ data in any form.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lu, J., Wu, D., Xu, BB. et al. A matched cohort study of the failure pattern after laparoscopic and open gastrectomy for locally advanced gastric cancer: does the operative approach matter?. Surg Endosc 36, 689–700 (2022). https://doi.org/10.1007/s00464-021-08337-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08337-w