Abstract
Background
The purpose of this study was to compare the degree of surgical smoke or vapor and lateral thermal damage caused by two different energy-based surgical devices (ESDs) used in colpotomy during total laparoscopic hysterectomy.
Methods
Patients undergoing laparoscopic hysterectomy were randomly assigned to an ultrasonic ESD group (n = 20) or monopolar ESD group (n = 20). Colpotomy was performed using the assigned ESD. The degree of surgical smoke or vapor obstructing the laparoscopic view was assessed by two independent reviewers using a 5-point Likert scale, in which a higher score indicates worse visibility. The degree of the lateral thermal damage was measured as the width from the point of instrument application to the margins of the unchanged nearby tissue using a light microscope.
Results
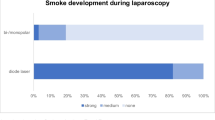
The baseline characteristics did not statistically differ between the two groups. The degree of surgical smoke or vapor obstructing vision was 1.2 ± 0.8 points in the ultrasonic group and 3.9 ± 0.7 points in the monopolar groups (p < 0.001). The lateral thermal damage was significantly increased in the monopolar group compared to in the ultrasound group (1500 µm [1200–2500 µm] vs. 950 µm [650–1725 µm], p = 0.037).
Conclusion
Ultrasonic ESD had better laparoscopic visibility and caused less lateral thermal damage during colpotomy compared to monopolar device.



Similar content being viewed by others
References
Kim FJ, Sehrt D, Pompeo A, Molina WR (2012) Comparison of surgical plume among laparoscopic ultrasonic dissectors using a real-time digital quantitative technology. Surg Endosc 26:3408–3412
Druzijanic N, Pogorelic Z, Perko Z, Mrklic I, Tomic S (2012) Comparison of lateral thermal damage of the human peritoneum using monopolar diathermy, Harmonic scalpel and LigaSure. Can J Surg 55:317–321
Broughton D, Welling AL, Monroe EH, Pirozzi K, Schulte JB, Clymer JW (2013) Tissue effects in vessel sealing and transection from an ultrasonic device with more intelligent control of energy delivery. Med Devices (Auckl) 6:151–154
Hefermehl LJ, Largo RA, Hermanns T, Poyet C, Sulser T, Eberli D (2014) Lateral temperature spread of monopolar, bipolar and ultrasonic instruments for robot-assisted laparoscopic surgery. BJU Int 114:245–252
Phillips CK, Hruby GW, Durak E, Lehman DS, Humphrey PA, Mansukhani MM, Landman J (2008) Tissue response to surgical energy devices. Urology 71:744–748
Song T, Lee Y, Kim ML, Yoon BS, Joo WD, Seong SJ, Kim IH (2013) Single-port access total laparoscopic hysterectomy for large uterus. Gynecol Obstet Invest 75:16–20
Vassiliou MC, Feldman LS, Andrew CG, Bergman S, Leffondre K, Stanbridge D, Fried GM (2005) A global assessment tool for evaluation of intraoperative laparoscopic skills. Am J Surg 190:107–113
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Weld KJ, Dryer S, Ames CD, Cho K, Hogan C, Lee M, Biswas P, Landman J (2007) Analysis of surgical smoke produced by various energy-based instruments and effect on laparoscopic visibility. J Endourol 21:347–351
Choi SH, Kwon TG, Chung SK, Kim TH (2014) Surgical smoke may be a biohazard to surgeons performing laparoscopic surgery. Surg Endosc 28:2374–2380
Tomita Y, Mihashi S, Nagata K, Ueda S, Fujiki M, Hirano M, Hirohata T (1981) Mutagenicity of smoke condensates induced by CO2-laser irradiation and electrocauterization. Mutat Res 89:145–149
Emam TA, Cuschieri A (2003) How safe is high-power ultrasonic dissection? Ann Surg 237:186–191
Humes DJ, Ahmed I, Lobo DN (2010) The pedicle effect and direct coupling: delayed thermal injuries to the bile duct after laparoscopic cholecystectomy. Arch Surg 145:96–98
Kadesky KM, Schopf B, Magee JF, Blair GK (1997) Proximity injury by the ultrasonically activated scalpel during dissection. J Pediatr Surg 32:878–879
Catena F, Di Saverio S, Ansaloni L, Coccolini F, Sartelli M, Vallicelli C, Cucchi M, Tarasconi A, Catena R, De’ Angelis G, Abongwa HK, Lazzareschi D, Pinna A (2014) The HAC trial (harmonic for acute cholecystitis): a randomized, double-blind, controlled trial comparing the use of harmonic scalpel to monopolar diathermy for laparoscopic cholecystectomy in cases of acute cholecystitis. World J Emerg Surg 9:53
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Chahien Choi, In-Gu Do, Taejong Song have no conflicts of interest or financial ties to disclose.
Additional information
Chahien Choi and In-Gu Do have contributed equally.
Rights and permissions
About this article
Cite this article
Choi, C., Do, IG. & Song, T. Ultrasonic versus monopolar energy-based surgical devices in terms of surgical smoke and lateral thermal damage (ULMOST): a randomized controlled trial. Surg Endosc 32, 4415–4421 (2018). https://doi.org/10.1007/s00464-018-6183-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6183-3