Abstract
Background
Minimally invasive pancreaticoduodenectomy (MIPD) is being performed with increasing frequency for pancreatic cancer, but the most oncologically efficacious surgical platform, whether robotic or laparoscopic, is yet to be determined. Currently, there are no national studies comparing the oncological outcomes between robotic (RPD) and laparoscopic (LPD) pancreaticoduodenectomy.
Methods
This was a retrospective study using the National Cancer Database between 2010 and 2013. We compared the perioperative, pathological, and mid-term oncological outcomes between RPD and LPD.
Results
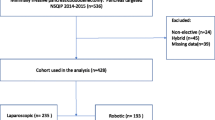
There were 1623 MIPD cases, of which 90% were LPD and 10% were RPD. Most LPD (63%) and RPD (51%) cases were performed at institutions with a volume of ≤ 5 MIPDs per year. There were no differences in patient- and tumor-related factors between the groups. The majority of treated tumors were adenocarcinoma (90.1% for RPD and 89.1% for LPD). RPDs were more likely to be performed at academic centers (89.1%) compared to LPDs (68.1%, P < 0.001) and at higher-volume centers (median MIPD/year of 4.7 for RPD vs 3.6 for LPD, P < 0.001). There was no difference in the median number of examined lymph nodes, margin status, median length of stay, 90-day mortality, or 30-day readmission between groups. There was no difference in median overall survival for pancreatic adenocarcinoma between LPD (20.7 months) and RPD (22.7 months; log-rank P = 0.445). The 1- and 3-year overall survival rates were 74 and 31% for LPD and 71 and 33% for RPD.
Conclusion
In this national cohort of patients, LPD and RPD were associated with equivalent perioperative, pathological, and mid-term oncological outcomes.


Similar content being viewed by others
References
Song KB, Kim SC, Hwang DW, Lee JH, Lee DJ, Lee JW, Park K-M, Lee Y-J (2015) Matched case-control analysis comparing laparoscopic and open pylorus-preserving pancreaticoduodenectomy in patients with periampullary tumors. Ann Surg 262:146–155
Tran TB, Dua MM, Worhunsky DJ, Poultsides GA, Norton JA, Visser BC (2016) The first decade of laparoscopic pancreaticoduodenectomy in the United States: costs and outcomes using the Nationwide Inpatient Sample. Surg Endosc 30:1778–1783
Adam MA, Choudhury K, Dinan MA, Reed SD, Scheri RP, Blazer DG, Roman S (2015) Minimally invasive versus open pancreaticoduodenectomy for cancer. Ann Surg 262:372–377
Croome KP, Farnell MB, Que FG, Reid-Lombardo KM, Truty MJ, Nagorney DM, Kendrick M (2014) Total laparoscopic pancreaticoduodenectomy for pancreatic ductal adenocarcinoma. Ann Surg 260:633–640
Sharpe SM, Talamonti MS, Wang CE, Prinz RA, Roggin KK, Bentrem DJ, Winchester DJ, Marsh RD, Stocker SJ, Baker MS (2015) Early national experience with laparoscopic pancreaticoduodenectomy for ductal adenocarcinoma: a comparison of laparoscopic pancreaticoduodenectomy and open pancreaticoduodenectomy from the National Cancer Data Base. J Am Coll Surg 221:175–184
Baker EH, Ross SW, Seshadri R, Swan RZ, Iannitti DA, Vrochides D, Martinie JB (2016) Robotic pancreaticoduodenectomy: comparison of complications and cost to the open approach. Int J Med Robot 12:554–560
Stauffer JA, Coppola A, Villacreses D, Mody K, Johnson E, Li Z, Asbun HJ (2016) Laparoscopic versus open pancreaticoduodenectomy for pancreatic adenocarcinoma: long-term results at a single institution. Surg Endosc 31:2233–2241
Zureikat AH, Postlewait LM, Liu Y, Gillespie TW, Weber SM, Abbott DE, Ahmad SA, Maithel SK, Hogg ME, Zenati M, Cho CS, Salem A, Xia B, Steve J, Nguyen TK, Keshava HB, Chalikonda S, Walsh RM, Talamonti MS, Stocker SJ, Bentrem DJ, Lumpkin S, Kim HJ, Zeh HJ 3rd, Kooby DA (2016) A multi-institutional comparison of perioperative outcomes of robotic and open pancreaticoduodenectomy. Ann Surg 264:640–649
Tee MC, Croome KP, Shubert CR, Farnell MB, Truty MJ, Que FG, Reid-Lombardo KM, Smoot RL, Nagorney DM, Kendrick ML (2015) Laparoscopic pancreatoduodenectomy does not completely mitigate increased perioperative risks in elderly patients. HPB (Oxford) 17:909–918
McMillan MT, Zureikat AH, Hogg ME, Kowalsky SJ, Zeh HJ, Sprys MH, Vollmer CM Jr (2016) A propensity score–matched analysis of robotic vs open pancreatoduodenectomy on incidence of pancreatic fistula. JAMA Surg 152:327–335
Asbun HJ, Stauffer JA (2012) Laparoscopic vs open pancreaticoduodenectomy: overall outcomes and severity of complications using the Accordion Severity Grading System. J Am Coll Surg 215:810–819
Nassour I, Wang SC, Christie A, Augustine MM, Porembka MR, Yopp AC, Choti MA, Mansour JC, Xie XJ, Polanco PM, Minter RM (2017) Minimally invasive versus open pancreaticoduodenectomy: a propensity-matched study from a national cohort of patients. Ann Surg. https://doi.org/10.1097/SLA.0000000000002259
Nassour I, Wang SC, Porembka MR, Yopp AC, Choti MA, Augustine MM, Polanco PM, Mansour JC, Minter RM (2017) Robotic versus laparoscopic pancreaticoduodenectomy: a NSQIP analysis. J Gastrointest Surg 21:1784–1792
Liu R, Zhang T, Zhao Z-M, Tan XL, Zhao GD, Zhang X, Xu Y (2016) The surgical outcomes of robot-assisted laparoscopic pancreaticoduodenectomy versus laparoscopic pancreaticoduodenectomy for periampullary neoplasms: a comparative study of a single center. Surg Endosc 31:2380–2386
Park EJ, Cho MS, Baek SJ, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2015) Long-term oncologic outcomes of robotic low anterior resection for rectal cancer. Ann Surg 261:129–137
Tsung A, Geller DA, Sukato DC, Sabbaghian S, Tohme S, Steel J, Marsh W, Reddy SK, Bartlett DL (2014) Robotic versus laparoscopic hepatectomy: a matched comparison. Ann Surg 259:549–555
Xie W, Cao D, Yang J, Shen K, Zhao L (2016) Robot-assisted surgery versus conventional laparoscopic surgery for endometrial cancer: a systematic review and meta-analysis. J Cancer Res Clin Oncol 142:2173–2183
Nassour I, Polanco PM (2016) Minimally invasive liver surgery for hepatic colorectal metastases. Curr Colorectal Cancer Rep 12:103–112
Daouadi M, Zureikat AH, Zenati MS, Choudry H, Tsung A, Bartlett DL, Hughes SJ, Lee KK, Moser AJ, Zeh HJ (2013) Robot-assisted minimally invasive distal pancreatectomy is superior to the laparoscopic technique. Ann Surg 257:128–132
Park JM, Kim HI, Han SU, Yang HK, Kim YW, Lee HJ, An JY, Kim MC, Park S, Song KY, Oh SJ, Kong SH, Suh BJ, Yang DH, Ha TK, Hyung WJ, Ryu KW (2016) Who may benefit from robotic gastrectomy? A subgroup analysis of multicenter prospective comparative study data on robotic versus laparoscopic gastrectomy. Eur J Surg Oncol 42:1944–1949
American College of Surgeons (2016) National Cancer Database. https://www.facs.org/quality%20programs/cancer/ncdb. Accessed 4 Jul 2016
Allan C, Ilic D (2016) Laparoscopic versus robotic-assisted radical prostatectomy for the treatment of localised prostate cancer: a systematic review. Urol Int 96:373–378
Shiomi A, Kinugasa Y, Yamaguchi T, Kagawa H, Yamakawa Y (2016) Robot-assisted versus laparoscopic surgery for lower rectal cancer: the impact of visceral obesity on surgical outcomes. Int J Colorectal Dis 31:1701–1710
Salehi S, Åvall-Lundqvist E, Legerstam B, Carlson JW, Falconer H (2017) Robot-assisted laparoscopy versus laparotomy for infrarenal paraaortic lymphadenectomy in women with high-risk endometrial cancer: a randomised controlled trial. Eur J Cancer 79:81–89
Mason MC, Tran Cao HS, Awad SS, Farjah F, Chang GJ, Massarweh NN (2017) Hospital minimally invasive surgery utilization for gastrointestinal cancer. Ann Surg. https://doi.org/10.1097/SLA.0000000000002302
de Rooij T, van Hilst J, Boerma D, Bonsing BA, Daams F, van Dam RM, Dijkgraaf MG, van Eijck CH, Festen S, Gerhards MF, Koerkamp BG, van der Harst E, de Hingh IH, Kazemier G, Klaase J, de Kleine RH, van Laarhoven CJ, Lips DJ, Luyer MD, Molenaar IQ, Patijn GA, Roos D, Scheepers JJ, van der Schelling GP, Steenvoorde P, Vriens MR, Wijsman JH, Gouma DJ, Busch OR, Hilal MA, Besselink MG; Dutch Pancreatic Cancer Group (2016) Impact of a nationwide training program in minimally invasive distal pancreatectomy (LAELAPS). Ann Surg 264:754–762
Adam MA, Thomas S, Youngwirth L, Pappas T, Roman SA, Sosa JA (2017) Defining a hospital volume threshold for minimally invasive pancreaticoduodenectomy in the United States. JAMA Surg 152:336–337
Ahola R, Siiki A, Vasama K, Vornanen M, Sand J, Laukkarinen J (2017) Effect of centralization on long-term survival after resection of pancreatic ductal adenocarcinoma. Br J Surg 150:701–707
Acknowledgements
The authors would like to thank Dave Primm for his help in editing this manuscript and Helen Mayo from the UTSW Health Sciences Digital Library and Learning Center for assistance with literature searches.
Funding
Research reported in this publication was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health under award number UL1TR001105. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Ibrahim Nassour, Michael A. Choti, Matthew R. Porembka, Adam C. Yopp, Sam C.Wang, and Patricio M. Polanco have no other conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Nassour, I., Choti, M.A., Porembka, M.R. et al. Robotic-assisted versus laparoscopic pancreaticoduodenectomy: oncological outcomes. Surg Endosc 32, 2907–2913 (2018). https://doi.org/10.1007/s00464-017-6002-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-6002-2