Abstract
Background
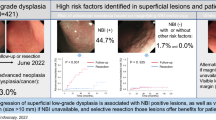
The optimal management of precursor lesions such as gastric low-grade dysplasia is crucial in order to improve gastric cancer-related mortality. However, there are no universally accepted management guidelines regarding which lesions should be resected or should be monitored by follow-up visits.
Patients and methods
We retrospectively analyzed data from 1006 gastric low-grade dysplasia lesions that had been resected via endoscopic submucosal dissection. We also evaluated the endoscopic risk factors associated with upstage diagnosis from low-grade dysplasia to high-grade dysplasia or gastric cancer.
Results
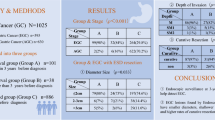
The mean age of our patients was 63.7 ± 9.1 years and 70.3% of our study population included men. The predominant location and gross type of lesions was the lower third of the stomach (78.6%) and the elevated type (57.8%), respectively. The rates of pathological concordance, upstage, and downstage diagnosis were 85.3, 12.1, and 2.6%, respectively. Multivariate analysis, after adjusting for age and sex, showed that a lesion size ≥ 10 mm (Odds ratio [OR] 2.231; p = 0.003), erythema (OR 7.315; p < 0.001), nodularity (OR 5.589; p < 0.001), depression (OR 3.024; p = 0.002), and erosion (OR 7.680; p < 0.001) were all factors significantly associated with upstage diagnosis. Furthermore, an increasing number of risk factors was associated with an increasing frequency of upstage diagnosis; if there were no risk factors, then there was no upstage diagnosis.
Conclusions
This study identified several risk factors that were significantly associated with the upstage diagnosis of gastric low-grade dysplasia: lesion size ≥ 10 mm and a variety of surface changes (erythema, nodularity, depression, and erosion). Our data indicate that if there is no evidence of these endoscopic risk factors, then regular follow-up may be considered, according to the patient’s combined comorbid conditions.



Similar content being viewed by others
References
Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM (2010) Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer 127:2893–2917
Li D, Bautista MC, Jiang SF, Daryani P, Brackett M, Armstrong MA, Hung YY, Postlethwaite D, Ladabaum U (2016) Risks and predictors of gastric adenocarcinoma in patients with gastric intestinal metaplasia and dysplasia: a population-based study. Am J Gastroenterol 111:1104–1113
Correa P (1992) Human gastric carcinogenesis: a multistep and multifactorial process—first American Cancer Society award lecture on cancer epidemiology and prevention. Cancer Res 52:6735–6740
Fox JG, Wang TC (2001) Helicobacter pylori—not a good bug after all! N Engl J Med 345:829–832
Dixon MF (2002) Gastrointestinal epithelial neoplasia: Vienna revisited. Gut 51:130–131
Choi CW, Kim HW, Shin DH, Kang DH, Hong YM, Park JH, Park SB, Cho M, Lee JH (2014) The risk factors for discrepancy after endoscopic submucosal dissection of gastric category 3 lesion (low grade dysplasia). Dig Dis Sci 59:421–427
Choi CW, Kim HW, Kang DH, Hong YM, Kim SJ, Park SB, Cho M, Kim DJ, Hong JB (2014) Clinical outcomes of second-look endoscopy after gastric endoscopic submucosal dissection: predictive factors with high risks of bleeding. Surg Endosc 28:2213–2220
(2003) The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, 2002. Gastrointest Endosc 58:S3-43
Japanese Gastric Cancer Association (2011) Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer 14:101–112
Cho SJ, Choi IJ, Kim CG, Lee JY, Kook MC, Park S, Ryu KW, Lee JH, Kim YW (2011) Risk of high-grade dysplasia or carcinoma in gastric biopsy-proven low-grade dysplasia: an analysis using the Vienna classification. Endoscopy 43:465–471
Kim MK, Jang JY, Kim JW, Shim JJ, Lee CK, Chang YW, Choe BK (2014) Is lesion size an independent indication for endoscopic resection of biopsy-proven low-grade gastric dysplasia? Dig Dis Sci 59:428–435
Jeon HK, Ryu HY, Cho MY, Kim HS, Kim JW, Park HJ, Kim MY, Baik SK, Kwon SO, Park SY, Won SH (2014) A randomized trial to determine the diagnostic accuracy of conventional vs. jumbo forceps biopsy of gastric epithelial neoplasias before endoscopic submucosal dissection; open-label study. Gastric Cancer 17:661–668
Graham DY, Schwartz JT, Cain GD, Gyorkey F (1982) Prospective evaluation of biopsy number in the diagnosis of esophageal and gastric carcinoma. Gastroenterology 82:228–231
Iishi H, Tatsuta M, Okuda S (1985) Endoscopic diagnosis of minute gastric cancer of less than 5 mm in diameter. Cancer 56:655–659
Yamada H, Ikegami M, Shimoda T, Takagi N, Maruyama M (2004) Long-term follow-up study of gastric adenoma/dysplasia. Endoscopy 36:390–396
Min BH, Kim KM, Kim ER, Park CK, Kim JJ, Lee H, Lee JH, Chang DK, Kim YH, Rhee PL, Rhee JC (2011) Endoscopic and histopathological characteristics suggesting the presence of gastric mucosal high grade neoplasia foci in cases initially diagnosed as gastric mucosal low grade neoplasia by forceps biopsy in Korea. J Gastroenterol 46:17–24
Choi JM, Kim SG, Yang HJ, Lim JH, Choi J, Im JP, Kim JS, Kim WH, Jung HC (2016) Clinical outcomes of no residual disease in the specimen after endoscopic resection for gastric neoplasms. Surg Endosc 30:610–618
Yang MJ, Shin SJ, Lee KS, Lee KM, Lim SG, Kang JK, Hwang JC, Kim SS, Lee D, Kim JS, Lee GH, Ryu HS, Yoo BM, Lee KJ, Kim YB, Kim JH (2015) Non-neoplastic pathology results after endoscopic submucosal dissection for gastric epithelial dysplasia or early gastric cancer. Endoscopy 47:598–604
Jeong DI, Kim HW, Choi CW, Kang DH, Park SB, Kim SJ, Nam HS (2017) Clinical features of negative pathologic results after gastric endoscopic submucosal dissection. Surg Endosc 31:1163–1171
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Cheol Woong Choi, Dae Hwan Kang, Hyung Wook Kim, Su Bum Park, Su Jin Kim, Hyeong Seok Nam, and Dae Gon Ryu have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Kang, D.H., Choi, C.W., Kim, H.W. et al. Predictors of upstage diagnosis after endoscopic resection of gastric low-grade dysplasia. Surg Endosc 32, 2732–2738 (2018). https://doi.org/10.1007/s00464-017-5971-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5971-5