Abstract
Introduction
Robotic-assisted procedures were frequently found to have similar outcomes and indications to their laparoscopic counterparts, yet significant variation existed in the acceptance of robotic-assisted technology between surgical specialties and procedures. We performed a retrospective cohort study investigating factors associated with the adoption of robotic assistance across the United States from 2008 to 2013.
Methods
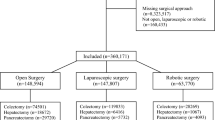
Using the Nationwide Inpatient Sample database, patient- and hospital-level variables were examined for differential distribution between robotic-assisted and conventional laparoscopic procedures. Multilevel logistic regression models were constructed to identify independent factors associated with robotic adoption. Furthermore, cases were stratified by procedure and specialty before being ranked according to proportion of robotic-assistance adoption. Correlation was examined between robotic-assistance adoption and relative outcome in comparison with conventional laparoscopic procedures.
Results
The national robotic case volume doubled over the five-year period while a gradual decline in laparoscopic case volume was observed, resulting in an increase in the proportion of procedures performed with robotic assistance from 6.8 to 17%. Patients receiving robotic procedures were more likely to be younger, males, white, privately insured, more affluent, and with less comorbidities. These differences have been decreasing over the study period. The three specialties with the highest proportion of robotic-assisted laparoscopic procedures were urology (34.1%), gynecology (11.0%), and endocrine surgery (9.4%). However, no significant association existed between the frequency of robotic-assistance usage and relative outcome statistics such as mortality, charge, or length of stay.
Conclusion
The variation in robotic-assistance adoption between specialties and procedures could not be attributable to clinical outcomes alone. Cultural readiness toward adopting new technology within specialty and target anatomic areas appear to be major determining factors influencing its adoption.

Similar content being viewed by others
References
Rogers EM (2003) Diffusion of innovations, 5th edn. Free Press, New York
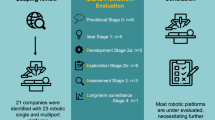
Barkun JS, Aronson JK, Feldman LS, Maddern GJ, Strasberg SM, Altman DG, Blazeby JM, Boutron IC, Campbell WB, Clavien PA, Cook JA, Ergina PL, Flum DR, Glasziou P, Marshall JC, McCulloch P, Nicholl J, Reeves BC, Seiler CM, Meakins JL, Ashby D, Black N, Bunker J, Burton M, Campbell M, Chalkidou K, Chalmers I, de Leval M, Deeks J, Grant A, Gray M, Greenhalgh R, Jenicek M, Kehoe S, Lilford R, Littlejohns P, Loke Y, Madhock R, McPherson K, Rothwell P, Summerskill B, Taggart D, Tekkis P, Thompson M, Treasure T, Trohler U, Vandenbroucke J (2009) Evaluation and stages of surgical innovations. Lancet 374:1089–1096
Binder J, Kramer W (2001) Robotically-assisted laparoscopic radical prostatectomy. BJU Int 87:408–410
Abbou CC, Hoznek A, Salomon L, Lobontiu A, Saint F, Cicco A, Antiphon P, Chopin D (2000) Remote laparoscopic radical prostatectomy carried out with a robot. Report of a case. Prog Urol 10:520–523
Elhage O, Challacombe B, Shortland A, Dasgupta P (2015) An assessment of the physical impact of complex surgical tasks on surgeon errors and discomfort: a comparison between robot-assisted, laparoscopic and open approaches. BJU Int 115:274–281
Hollingsworth JM, Krein SL, Dunn RL, Wolf JS Jr, Hollenbeck BK (2008) Understanding variation in the adoption of a new technology in surgery. Med Care 46:366–371
Parsons JK, Messer K, Palazzi K, Stroup SP, Chang D (2014) Diffusion of surgical innovations, patient safety, and minimally invasive radical prostatectomy. JAMA Surg 149:845–851
Mirheydar HS, Parsons JK (2012) Diffusion of robotics into clinical practice in the United States: process, patient safety, learning curves, and the public health. World J Urol 31:455–461
Casula R, Athanasiou T, Foale R (2004) Recent advances in minimal-access cardiac surgery using robotic-enhanced surgical systems. Expert Rev Cardiovasc Ther 2:589–600
Ismail M, Swierzy M, Ulrich M, Ruckert JC (2013) Application of the da Vinci robotic system in thoracic surgery. Chirurg 84:643–650
Herrell SD, Webster R, Simaan N (2014) Future robotic platforms in urologic surgery: recent developments. Curr Opin Urol 24:118–126
Jung M, Morel P, Buehler L, Buchs NC, Hagen ME (2015) Robotic general surgery: current practice, evidence, and perspective. Langenbecks Arch Surg 400:283–292
Mirnezami AH, Mirnezami R, Venkatasubramaniam AK, Chandrakumaran K, Cecil TD, Moran BJ (2010) Robotic colorectal surgery: hype or new hope?: A systematic review of robotics in colorectal surgery. Colorectal Dis 12:1084–1093
Choi JE, You JH, Kim DK, Rha KH, Lee SH (2010) Comparison of perioperative outcomes between robotic and laparoscopic partial nephrectomy: a systematic review and meta-analysis. Eur Urol 67:891–901
Robertson C, Close A, Fraser C, Gurung T, Jia X, Sharma P, Vale L, Ramsay C, Pickard R (2013) Relative effectiveness of robot-assisted and standard laparoscopic prostatectomy as alternatives to open radical prostatectomy for treatment of localised prostate cancer: a systematic review and mixed treatment comparison meta-analysis. BJU Int 112:798–812
Gaia G, Holloway RW, Santoro L, Ahmad S, Di Silverio E, Spinillo A (2010) Robotic-assisted hysterectomy for endometrial cancer compared with traditional laparoscopic and laparotomy approaches: a systematic review. Obstet Gynecol 116:1422–1431
Juo YY, Hyder O, Haider AH, Camp M, Lidor A, Ahuja N (2014) Is minimally invasive colon resection better than traditional approaches? First comprehensive national examination with propensity score matching. JAMA Surg 149:177–184
Nagendran J, Catrip J, Losenno KL, Adams C, Kiaii B, Chu MW (2017) Minimally invasive mitral repair surgery: why does controversy still persist? Expert Rev Cardiovasc Ther 15:15–24
Patel R, Szymaniak J, Radadia K, Faiena I, Lasser M (2015) Controversies in robotics: open versus robotic radical cystectomy. Clin Genitourin Cancer 13:421–427
Albright BB, Witte T, Tofte AN, Chou J, Black JD, Desai VB, Erekson EA (2016) Robotic versus laparoscopic hysterectomy for benign disease: a systematic review and meta-analysis of randomized trials. J Minim Invasive Gynecol 23:18–27
Cathelineau X, Sanchez-Salas R, Sivaraman A (2014) What is next in robotic urology? Curr Urol Rep 15:460
Gala RB, Margulies R, Steinberg A, Murphy M, Lukban J, Jeppson P, Aschkenazi S, Olivera C, South M, Lowenstein L, Schaffer J, Balk EM, Sung V (2014) Systematic review of robotic surgery in gynecology: robotic techniques compared with laparoscopy and laparotomy. J Minim Invasive Gynecol 21:353–361
Meshkinpour H, Hsu D, Farivar S (1988) Effect of gastric bubble as a weight reduction device: a controlled, crossover study. Gastroenterology 95:589–592
Ruffin JM, Grizzle JE, Hightower NC, McHardy G, Shull H, Kirsner JB (1969) A co-operative double-blind evaluation of gastric “freezing” in the treatment of duodenal ulcer. N Engl J Med 281:16–19
EC-IC Bypass Study Group (1985) Failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. Results of an international randomized trial. N Engl J Med 313:1191–1200
Kramer FM, Stunkard AJ, Spiegel TA, Deren JJ, Velchik MG, Wadden TA, Marshall KA (1989) Limited weight losses with a gastric balloon. Arch Intern Med 149:411–413
Warlow C (1991) MRC European Carotid Surgery Trial: interim results for symptomatic patients with severe (70–99%) or with mild (0–29%) carotid stenosis. Lancet 337:1235–1243
HCUP Nationwide Inpatient Sample (NIS) (2010) Healthcare Cost and Utilization Project (HCUP). Agency for healthcare research and quality. Rockville. http://www.hcup-us.ahrq.gov/nisoverview.jsp. Accessed 30 Jan 2013
Elixhauser A, Steiner C, Harris DR, Coffey RM (1998) Comorbidity measures for use with administrative data. Med Care 36:8–27
Romano PS, Roos LL, Jollis JG (1993) Adapting a clinical comorbidity index for use with ICD-9-CM administrative data: differing perspectives. J Clin Epidemiol 46: 1075–1079; discussion 1081–1090
Cuzick J (1985) A Wilcoxon-type test for trend. Stat Med 4:87–90
StataCorp (2005) Stata data management reference manual, Release 9. Stata Press, College Station
Karthikesalingam A, Holt PJ, Vidal-Diez A, Bahia SS, Patterson BO, Hinchliffe RJ, Thompson MM (2016) The impact of endovascular aneurysm repair on mortality for elective abdominal aortic aneurysm repair in England and the United States. J Vasc Surg 64:321.e322–327.e322
Chmielecki DK, Hagopian EJ, Kuo YH, Kuo YL, Davis JM (2012) Laparoscopic cholecystectomy is the preferred approach in cirrhosis: a nationwide, population-based study. HPB (Oxford) 14:848–853
Jaschinski T, Mosch C, Eikermann M, Neugebauer EA (2015) Laparoscopic versus open appendectomy in patients with suspected appendicitis: a systematic review of meta-analyses of randomised controlled trials. BMC Gastroenterol 15:48
Varda BK, Johnson EK, Clark C, Chung BI, Nelson CP, Chang SL (2014) National trends of perioperative outcomes and costs for open, laparoscopic and robotic pediatric pyeloplasty. J Urol 191:1090–1095
Moghadamyeghaneh Z, Phelan M, Smith BR, Stamos MJ (2015) Outcomes of open, laparoscopic, and robotic abdominoperineal resections in patients with rectal cancer. Dis Colon Rectum 58:1123–1129
Liu JJ, Leppert JT, Maxwell BG, Panousis P, Chung BI (2014) Trends and perioperative outcomes for laparoscopic and robotic nephrectomy using the National Surgical Quality Improvement Program (NSQIP) database. Urol Oncol 32:473–479
Yamasato K, Casey D, Kaneshiro B, Hiraoka M (2014) Effect of robotic surgery on hysterectomy trends: implications for resident education. J Minim Invasive Gynecol 21:399–405
Lee MG, Chiu CC, Wang CC, Chang CN, Lee SH, Lee M, Hsu TC, Lee CC (2017) Trends and outcomes of surgical treatment for colorectal cancer between 2004 and 2012—an analysis using national inpatient database. Sci Rep 7:2006
Moran PS, O’Neill M, Teljeur C, Flattery M, Murphy LA, Smyth G, Ryan M (2013) Robot-assisted radical prostatectomy compared with open and laparoscopic approaches: a systematic review and meta-analysis. Int J Urol 20:312–321
Maeso S, Reza M, Mayol JA, Blasco JA, Guerra M, Andradas E, Plana MN (2010) Efficacy of the Da Vinci surgical system in abdominal surgery compared with that of laparoscopy: a systematic review and meta-analysis. Ann Surg 252:254–262
Trinh BB, Hauch AT, Buell JF, Kandil E (2014) Robot-assisted versus standard laparoscopic colorectal surgery. JSLS. doi:10.4293/JSLS.2014.00154
Yu J, Wang Y, Li Y, Li X, Li C, Shen J (2014) The safety and effectiveness of Da Vinci surgical system compared with open surgery and laparoscopic surgery: a rapid assessment. J Evid Based Med 7:121–134
Wright JD, Ananth CV, Lewin SN, Burke WM, Lu YS, Neugut AI, Herzog TJ, Hershman DL (2013) Robotically assisted vs laparoscopic hysterectomy among women with benign gynecologic disease. JAMA 309:689–698
Blake EA, Sheeder J, Behbakht K, Guntupalli SR, Guy MS (2016) Factors impacting use of robotic surgery for treatment of endometrial cancer in the United States. Ann Surg Oncol 23:3744–3748
Gabriel E, Thirunavukarasu P, Al-Sukhni E, Attwood K, Nurkin SJ (2016) National disparities in minimally invasive surgery for rectal cancer. Surg Endosc 30:1060–1067
Kim SP, Boorjian SA, Shah ND, Weight CJ, Tilburt JC, Han LC, Thompson RH, Trinh QD, Sun M, Moriarty JP, Karnes RJ (2013) Disparities in access to hospitals with robotic surgery for patients with prostate cancer undergoing radical prostatectomy. J Urol 189:514–520
Monn MF, Bahler CD, Schneider EB, Sundaram CP (2013) Emerging trends in robotic pyeloplasty for the management of ureteropelvic junction obstruction in adults. J Urol 189:1352–1357
Falkenback D, Lehane CW, Lord RV (2015) Robot-assisted oesophageal and gastric surgery for benign disease: antireflux operations and Heller’s myotomy. ANZ J Surg 85:113–120
Tolboom RC, Broeders IA, Draaisma WA (2015) Robot-assisted laparoscopic hiatal hernia and antireflux surgery. J Surg Oncol 112:266–270
Benmessaoud C, Kharrazi H, MacDorman KF (2011) Facilitators and barriers to adopting robotic-assisted surgery: contextualizing the unified theory of acceptance and use of technology. PLoS ONE 6:e16395
Stafinski T, Topfer LA, Zakariasen K, Menon D (2010) The role of surgeons in identifying emerging technologies for health technology assessment. Can J Surg 53:86–92
Guru KA, Hussain A, Chandrasekhar R, Piacente P, Bienko M, Glasgow M, Underwood W, Wilding G, Mohler JL, Menon M, Peabody JO (2009) Current status of robot-assisted surgery in urology: a multi-national survey of 297 urologic surgeons. Can J Urol 16: 4736–4741; discussion 4741
Tseng TY, Cancel QV, Fesperman SF, Kuebler HR, Sun L, Robertson CN, Polascik TJ, Moul JW, Vieweg J, Albala DM, Dahm P (2007) The role of early adopter bias for new technologies in robot assisted laparoscopic prostatectomy. J Urol 177:1318–1323
Wright JD, Raglan GB, Schulkin J, Fialkow MF (2017) Attitudes and beliefs regarding the utility of robotically assisted gynecologic surgery among practicing gynecologists. J Healthc Qual 39(4):211–218. doi:10.1097/JHQ.0000000000000017
Cundy TP, Marcus HJ, Hughes-Hallett A, Najmaldin AS, Yang GZ, Darzi A (2017) International attitudes of early adopters to current and future robotic technologies in pediatric surgery. J Pediatr Surg 49:1522–1526
Wexner SD, Bergamaschi R, Lacy A, Udo J, Brolmann H, Kennedy RH, John H (2009) The current status of robotic pelvic surgery: results of a multinational interdisciplinary consensus conference. Surg Endosc 23:438–443
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Juo, Lin, Dutson, Ahmad, and Aditya have no conflicts of interest or financial ties to disclose.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Juo, YY., Mantha, A., Abiri, A. et al. Diffusion of robotic-assisted laparoscopic technology across specialties: a national study from 2008 to 2013. Surg Endosc 32, 1405–1413 (2018). https://doi.org/10.1007/s00464-017-5822-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5822-4