Abstract
Background
Despite the importance of defect size, there are no standardized recommendations on how to measure ventral hernias. Our aims were to determine (1) if any significant differences existed between various methods of measuring ventral hernias and (2) the effect of these methods of measurement on selection of mesh size.
Method
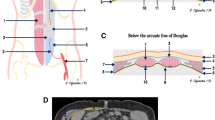
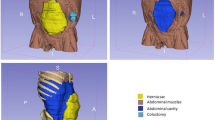
A prospective study of all patients enrolled in a randomized trial assessing laparoscopic ventral hernia repair at a single institution from 3/2015 to 7/2016 was eligible for inclusion. Abdominal wall hernia defect size was determined by multiplying defect length and width obtained separately using each of five methods: radiographic (CT), intraoperative with abdomen desufflated, intraoperative with abdomen insufflated to 15 mmHg (intra-abdominal aspect), intraoperative with abdomen insufflated to 15 mmHg (extra-abdominal aspect), and clinical. The primary outcome was intraclass correlation between the five different methods of measurement for each patient. Secondary outcome was changes in mesh selection assuming a 5 cm overlap in each direction.
Results
Fifty patients met inclusion criteria for assessment. The five different measurement methods had an intraclass correlation for each patient of 0.533 (95% CI 0.373–0.697) (weak correlation) for length; 0.737 (95% CI 0.613–0.844) (moderate correlation) for width; and 0.684 (95% CI 0.544–0.810) (moderate correlation) for area. Different types of measurements affected mesh selection in up to 56% of cases.
Conclusion
Among five common methods of measuring abdominal wall hernia defect, sizes are only weakly to moderately correlated. Further studies are needed to determine which method results in optimally sized abdominal wall prostheses and superior ventral hernia repair.


Similar content being viewed by others
References
Kurmann A, Visth E, Candinas D, Beldi G (2011) Long-term follow-up of open and laparoscopic repair of large incisional hernias. World J Surg 35:297–301
Le D, Deveney CW, Reaven NL, Funk SE, McGaughey KJ, Martindale RG (2013) Mesh choice in ventral hernia repair: so many choices, so little time. Am J Surg 205(5):602–607
Kapischke M, Schulz T, Schipper T, Tensfeldt J, Caliebe A (2008) Open versus laparoscopic incisional hernia repair: something different from a meta-analysis. Surg Endosc 22(10):2251–2260
Primary fascial closure with laparoscopic ventral hernia repair: a randomized controlled trial. ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT02363790?term=liang+hernia&rank=2. Accessed 11 Dec 2016
McHugh ML (2012) Interrater reliability: the kappa statistic. Biochem Med (Zagreb) 22(3):276–282
Muysoms FE, Miserez M, Berrevoet F, Campanelli G, Champault GG, Chelala E et al (2009) Classification of primary and incisional abdominal wall hernias. Hernia 13(4):407–414
LeBlanc K (2016) Proper mesh overlap is a key determinant in hernia recurrence following laparoscopic ventral and incisional hernia repair. Hernia 20(1):85–99
Carter SA, Hicks SC, Brahmbhatt R, Liang MK (2014) Recurrence and pseudorecurrence after laparoscopic ventral hernia repair: predictors and patient-focused outcomes. Am Surg 80(2):138–148
Guidelines for laparoscopic ventral hernia repair. SAGES [cited 18 Mar 2017]. Available from: https://www.sages.org/publications/guidelines/guidelines-for-laparoscopic-ventral-hernia-repair/. Accessed 18 Mar 2017
Moreno-Egea A, Carrasco L, Girela E, Martin JG, Aguayo JL, Canteras M (2002) Open vs laparoscopic repair of spigelian hernia: a prospective randomized trial. Arch Surg 137(11):1266–1268
Awaiz A, Rahman F, Hossain MB, Yunus RM, Khan S, Memon B et al (2015) Meta-analysis and systematic review of laparoscopic versus open mesh repair for elective incisional hernia. Hernia 19(3):449–463
Bernal E, Casado S, Grasa OG, Montiel JM, Gil I (2014) Computer vision distance measurement from endoscopic sequences: prospective evaluation in laparoscopic ventral hernia repair. Surg Endosc 28(12):3506–3512
Acknowledgements
None. The first (corresponding) author is willing to make the data, analytic methods, and study materials available to other researchers. This material can be obtained by communicating with Dr. Cherla at deepa.cherla@uth.tmc.edu (institutional email).
Funding information
This work was supported by the Center for Clinical and Translational Sciences, which is funded by National Institutes of Health Clinical and Translational Award UL1 TR000371 and KL2 TR000370 from the National Center for Advancing Translational Sciences. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center for Research Resources or the National Institutes of Health. The funding agencies were not involved in the study design, data collection, data analysis, manuscript preparation, or publication decisions. All authors had complete access to the study data that support the publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Cherla, Lew, Escamilla, Holihan, Gonzalez, Ko, Kao, Liang, and Mr. Cherla have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Cherla, D.V., Lew, D.F., Escamilla, R.J. et al. Differences of alternative methods of measuring abdominal wall hernia defect size: a prospective observational study. Surg Endosc 32, 1228–1233 (2018). https://doi.org/10.1007/s00464-017-5797-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5797-1