Abstract
Aim
The aim of this study is to evaluate the clinical outcomes and cost-effectiveness of elective, robot-assisted choledochotomy and common bile duct exploration (RCD/CBDE) compared to open surgery for ERCP refractory choledocholithiasis.
Method
A prospective database of all RCD/CBDE has been maintained since our first procedure in April 2007 though April 2016. With ethics approval, this database was compared with all contemporaneous elective open procedures (OCD/CBDE) performed since March 2005. Emergency procedures were excluded from analysis. Cost analysis was calculated using a micro-costing approach. Outcomes were analyzed on the basis of intent-to-treat. A p value of 0.05 denoted statistical significance.
Results
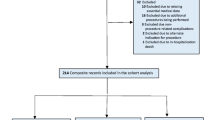
A total of 80 cases were performed since 2005 compromising 50 consecutive, unselected RCD/CBDE and 30 OCD/CBDE. Comparing RCD/CBDE to OCD/CBDE there were no significant differences between groups with respect to age (65 ± 20 vs. 67 ± 18 years, p = 0.09), gender (14/30 vs. 16/25 male/female, p = 0.52), ASA class or co-morbidities. The mean duration of surgery for RCD/CBDE trended longer compared to OCD/CBDE (205 ± 70 min vs. 174 ± 73 min, p = 0.08). However, there was significant reduction in postoperative complications with RCD/CBDE versus OCD/CBDE (22% vs. 56%, p = 0.002). Median hospital stay was also significantly reduced (6 vs 12 days, p = 0.01). The net overall hospital cost for RCD/CBDE was lower ($8449.88 CAD vs. $11671.2 CAD).
Conclusion
In this single-centre, cohort study, robotic-assisted CD/CBDE for ERCP refractory common bile duct stones provides the dominating strategy of improved patient outcomes with a reduction of overall cost.
Similar content being viewed by others
References
Hungness ES, Soper NJ (2006) Management of common bile duct stones. J Gastrointest Surg 10:612–619
McHenry L, Lehman G (2006) Difficult bile duct stones. Curr Treat Options Gastroenterol 9(2):123–132. doi:10.1007/s11938-006-0031-6
Scott D, Young W, Tesfay S, Frwley W et al (2001) Laparoscopic skills training. Am J Surg 182(2):42–137
Ozcan N, Kahriman G, Mavili E (2012) Percutaneous transhepatic removal of bile duct stones: results of 261 patients. Cardiovasc Interv Radiol 35(3):621–627
Alkhamesi NA, Davies WT, Pinto RF et al (2013) Robot-assisted common bile duct exploration as an option for complex choledocholithiasis. Surg Endosc 27(1):263–266
Jayaraman S, Davies W, Schlachta CM (2008) Robot-assisted minimally invasive common bile duct exploration: a Canadian first. Can J Surg 51:E93–E94
Cusheri A, Lezoche E, Morino M, Croce E et al (1999) E.A.E.S multicenter prospective randomized trial comparing two-stage vs single-stage management of patients with gallstone disease and ductal calculi. Surg Endosc 13:952–957
Thompson MH, Tranter SE (2002) All-comers policy for laparoscopic exploration of the common bile duct. Br J Surg 89:1608–1612
Hua J, Meng H, Yao L et al (2016) Five hundred consecutive laparoscopic common bile duct explorations: 5-year experience at a single institution. Surg Endosc. doi:10.1007/s00464-016-5388-6
Sweeney T, Rattner DW (2002) Robotically assisted minimally invasive biliary surgery in a porcine model. Surg Endosc 16:138–141
Cuschieri A (1995) Whither minimally access surgery: tribulations and expectations. Am J Surg 169:9–19
Park A, Lee G, Seagull FJ et al (2010) Patients benefit while surgeons suffer: An impending epidemic. J Am Coll Surg 210:306–313
Van Koughnett JA, Jayaraman S, Eagleson R et al (2009) Are there advantages to robotic-assisted surgery over laparoscopy from the surgeon’s perspective? J Robotic Surg 3:79–82
Lawson EH, Curet MJ, Sanchez BR et al (2007) Postural ergonomics during robotic and laparoscopic gastric bypass surgery: a pilot project. J Robotic Surg 1:61–67
Wilensky GR (2016) Robotic surgery: an example of when newer is not always better but clearly more expensive. Milbank Q 94:43–46. doi:10.1111/1468-0009.12178
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Ahmed Almamar, Nawar A. Alkhamesi, Ward T Davies and Christopher M. Schlachta have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Almamar, A., Alkhamesi, N.A., Davies, W.T. et al. Cost analysis of robot-assisted choledochotomy and common bile duct exploration as an option for complex choledocholithiasis. Surg Endosc 32, 1223–1227 (2018). https://doi.org/10.1007/s00464-017-5795-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5795-3