Abstract
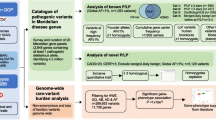
Congenital anomalies of the kidney and urinary tract (CAKUT) are the most common cause of chronic kidney disease (~ 45%) that manifests before 30 years of age. The genetic locus containing COL4A1 (13q33–34) has been implicated in vesicoureteral reflux (VUR), but mutations in COL4A1 have not been reported in CAKUT. We hypothesized that COL4A1 mutations cause CAKUT in humans. We performed whole exome sequencing (WES) in 550 families with CAKUT. As negative control cohorts we used WES sequencing data from patients with nephronophthisis (NPHP) with no genetic cause identified (n = 257) and with nephrotic syndrome (NS) due to monogenic causes (n = 100). We identified a not previously reported heterozygous missense variant in COL4A1 in three siblings with isolated VUR. When examining 549 families with CAKUT, we identified nine additional different heterozygous missense mutations in COL4A1 in 11 individuals from 11 unrelated families with CAKUT, while no COL4A1 mutations were identified in a control cohort with NPHP and only one in the cohort with NS. Most individuals (12/14) had isolated CAKUT with no extrarenal features. The predominant phenotype was VUR (9/14). There were no clinical features of the COL4A1-related disorders (e.g., HANAC syndrome, porencephaly, tortuosity of retinal arteries). Whereas COL4A1-related disorders are typically caused by glycine substitutions in the collagenous domain (84.4% of variants), only one variant in our cohort is a glycine substitution within the collagenous domain (1/10). We identified heterozygous COL4A1 mutations as a potential novel autosomal dominant cause of CAKUT that is allelic to the established COL4A1-related disorders and predominantly caused by non-glycine substitutions.


Similar content being viewed by others
References
Alamowitch S et al (2009) Cerebrovascular disease related to COL4A1 mutations in HANAC syndrome. Neurology 73:1873–1882. https://doi.org/10.1212/wnl.0b013e3181c3fd12
Baker NL et al (2007) Molecular consequences of dominant Bethlem myopathy collagen VI mutations. Ann Neurol 62:390–405. https://doi.org/10.1002/ana.21213
Braun DA et al (2016) Mutations in nuclear pore genes NUP93, NUP205 and XPO5 cause steroid-resistant nephrotic syndrome. Nat Genet 48:457–465. https://doi.org/10.1038/ng.3512
Chaki M et al (2011) Genotype-phenotype correlation in 440 patients with NPHP-related ciliopathies. Kidney Int 80:1239–1245. https://doi.org/10.1038/ki.2011.284
Chapman CJ, Bailey RR, Janus ED, Abbott GD, Lynn KL (1985) Vesicoureteric reflux: segregation analysis. Am J Med Genet 20:577–584. https://doi.org/10.1002/ajmg.1320200403
Chesnaye N et al (2014) Demographics of paediatric renal replacement therapy in Europe: a report of the ESPN/ERA-EDTA registry. Pediatr Nephrol 29:2403–2410. https://doi.org/10.1007/s00467-014-2884-6
Connaughton DM, Hildebrandt F (2019) Personalized medicine in chronic kidney disease by detection of monogenic mutations. Nephrol Dial Transplant. https://doi.org/10.1093/ndt/gfz028
Faguer S, Chassaing N, Bandin F, Prouheze C, Chauveau D, Decramer S (2012) Should SIX2 be routinely tested in patients with isolated congenital abnormalities of kidneys and/or urinary tract (CAKUT)? Eur J Med Genet 55:688–689. https://doi.org/10.1016/j.ejmg.2012.06.003
Gee HY et al (2014) Whole-exome resequencing distinguishes cystic kidney diseases from phenocopies in renal ciliopathies. Kidney Int 85:880–887. https://doi.org/10.1038/ki.2013.450
Kaylor J, Alfaro M, Ishwar A, Sailey C, Sawyer J, Zarate YA (2014) Molecular and cytogenetic evaluation of a patient with ring chromosome 13 and discordant results. Cytogenet Genome Res 144:104–108. https://doi.org/10.1159/000368649
Kim HY, Nelson CM (2012) Extracellular matrix and cytoskeletal dynamics during branching morphogenesis. Organogenesis 8:56–64. https://doi.org/10.4161/org.19813
Kuo DS, Labelle-Dumais C, Gould DB (2012) COL4A1 and COL4A2 mutations and disease: insights into pathogenic mechanisms and potential therapeutic targets. Hum Mol Genet 21:R97–110. https://doi.org/10.1093/hmg/dds346
Lek M et al (2016) Analysis of protein-coding genetic variation in 60,706 humans. Nature 536:285–291. https://doi.org/10.1038/nature19057
Lovric S, Ashraf S, Tan W, Hildebrandt F (2016) Genetic testing in steroid-resistant nephrotic syndrome: when and how? Nephrol Dial Transpl 31:1802–1813. https://doi.org/10.1093/ndt/gfv355
Lu W et al (2007) Disruption of ROBO2 is associated with urinary tract anomalies and confers risk of vesicoureteral reflux. Am J Hum Genet 80:616–632. https://doi.org/10.1086/512735
Luo J, Balkin N, Stewart JF, Sarwark JF, Charrow J, Nye JS (2000) Neural tube defects and the 13q deletion syndrome: evidence for a critical region in 13q33–34. Am J Med Genet 91:227–230
Meuwissen ME et al (2015) The expanding phenotype of COL4A1 and COL4A2 mutations: clinical data on 13 newly identified families and a review of the literature. Genet Med 17:843–853. https://doi.org/10.1038/gim.2014.210
Mimaki M et al (2015) Holoprosencephaly with cerebellar vermis hypoplasia in 13q deletion syndrome: critical region for cerebellar dysgenesis within 13q32.2q34. Brain Dev 37:714–718. https://doi.org/10.1016/j.braindev.2014.10.009
Noe HN, Wyatt RJ, Peeden JN Jr, Rivas ML (1992) The transmission of vesicoureteral reflux from parent to child. J Urol 148:1869–1871
Otto EA et al (2008) Mutation analysis in nephronophthisis using a combined approach of homozygosity mapping, CEL I endonuclease cleavage, and direct sequencing. Hum Mutat 29:418–426. https://doi.org/10.1002/humu.20669
Petritsa NA, Lukyanenko NS, Kens KA, Tretyak BI (2017) Effect of undifferentiated connective tissue dysplasia on the development of vesicoureteral reflux in infants. J Educ Health Sport 7:186–197. https://doi.org/10.5281/zenodo.1101092
Pietila I et al (2016) Wnt5a deficiency leads to anomalies in ureteric tree development, tubular epithelial cell organization and basement membrane integrity pointing to a role in kidney collecting duct patterning. PLoS One 11:e0147171. https://doi.org/10.1371/journal.pone.0147171
Plaisier E et al (2007) COL4A1 mutations and hereditary angiopathy, nephropathy, aneurysms, and muscle cramps. N Engl J Med 357:2687–2695. https://doi.org/10.1056/nejmoa071906
Plaisier E et al (2010) Novel COL4A1 mutations associated with HANAC syndrome: a role for the triple helical CB3[IV] domain. Am J Med Genet A 152A:2550–2555. https://doi.org/10.1002/ajmg.a.33659
Prockop DJ, Kivirikko KI (1995) Collagens: molecular biology, diseases, and potentials for therapy. Annu Rev Biochem 64:403–434. https://doi.org/10.1146/annurev.bi.64.070195.002155
Reis LM et al (2011) BMP4 loss-of-function mutations in developmental eye disorders including SHORT syndrome. Hum Genet 130:495–504. https://doi.org/10.1007/s00439-011-0968-y
Richards S et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17:405–424. https://doi.org/10.1038/gim.2015.30
Sadowski CE et al (2015) A single-gene cause in 29.5% of cases of steroid-resistant nephrotic syndrome. J Am Soc Nephrol 26:1279–1289. https://doi.org/10.1681/asn.2014050489
Shah MM, Sakurai H, Gallegos TF, Sweeney DE, Bush KT, Esko JD, Nigam SK (2011) Growth factor-dependent branching of the ureteric bud is modulated by selective 6-O sulfation of heparan sulfate. Dev Biol 356:19–27. https://doi.org/10.1016/j.ydbio.2011.05.004
Sievers F et al (2011) Fast, scalable generation of high-quality protein multiple sequence alignments using Clustal Omega. Mol Syst Biol 7:539. https://doi.org/10.1038/msb.2011.75
Soliman NA, Ali RI, Ghobrial EE, Habib EI, Ziada AM (2015) Pattern of clinical presentation of congenital anomalies of the kidney and urinary tract among infants and children. Nephrology (Carlton) 20:413–418. https://doi.org/10.1111/nep.12414
Suzuki S et al (2009) Mutations in BMP4 are associated with subepithelial, microform, and overt cleft lip. Am J Hum Genet 84:406–411. https://doi.org/10.1016/j.ajhg.2009.02.002
Turleau C, Seger J, de Grouchy J, Dore F, Job JC (1978) Del (13) (q33). Exclusion of esterase D (ESD) from 13q33 and q34. Ann Genet 21:189–192
van der Ven AT et al (2018a) Whole-exome sequencing identifies causative mutations in families with congenital anomalies of the kidney and urinary tract. J Am Soc Nephrol 29:2348–2361. https://doi.org/10.1681/ASN.2017121265
van der Ven AT, Vivante A, Hildebrandt F (2018b) Novel insights into the pathogenesis of monogenic congenital anomalies of the kidney and urinary tract. J Am Soc Nephrol 29:36–50. https://doi.org/10.1681/ASN.2017050561
Vats KR et al (2006) A locus for renal malformations including vesico-ureteric reflux on chromosome 13q33–34. J Am Soc Nephrol 17:1158–1167. https://doi.org/10.1681/asn.2005040404
Vivante A, Hildebrandt F (2016) Exploring the genetic basis of early-onset chronic kidney disease. Nat Rev Nephrol 12:133–146. https://doi.org/10.1038/nrneph.2015.205
Vivante A, Kohl S, Hwang DY, Dworschak GC, Hildebrandt F (2014) Single-gene causes of congenital anomalies of the kidney and urinary tract (CAKUT) in humans. Pediatr Nephrol 29:695–704. https://doi.org/10.1007/s00467-013-2684-4
Walczak-Sztulpa J et al (2008) Chromosome deletions in 13q33-34: report of four patients and review of the literature. Am J Med Genet A 146A:337–342. https://doi.org/10.1002/ajmg.a.32127
Walsh LE, Vance GH, Weaver DD (2001) Distal 13q deletion syndrome and the VACTERL association: case report, literature review, and possible implications. Am J Med Genet 98:137–144
Wang YP, Wang DJ, Niu ZB, Cui WT (2017) Chromosome 13q deletion syndrome involving 13q31qter: a case report. Mol Med Rep 15:3658–3664. https://doi.org/10.3892/mmr.2017.6425
Warejko JK et al (2018) Whole exome sequencing of patients with steroid-resistant nephrotic syndrome. Clin J Am Soc Nephrol 13:53–62. https://doi.org/10.2215/CJN.04120417
Weber S et al (2008) SIX2 and BMP4 mutations associate with anomalous kidney development. J Am Soc Nephrol 19:891–903. https://doi.org/10.1681/asn.2006111282
Acknowledgements
We would like to thank the families and study individuals for their contribution. Sequencing and data processing was performed by the Broad and Yale Centers for Mendelian Genomics funded by the National Human Genome Research Institute (UM1 HG008900 to DGM and HLR and U54 HG006504 to RPL). This research was supported by Grants from the National Institutes of Health to F.H. (R01-DK088767). A.M is supported by a Research Training in Pediatric Nephrology Grant (T32-DK007726) and the Harvard Stem Cell Institute Kidney Inter-lab Fellowship Award at Harvard Medical School (F-KP-0003-17-00). C.H.W.W. is supported by funding from the National Institutes of Health T32-GM007748 Grant. D.M.C. is funded by the Health Research Board, Ireland (HPF-206-674), the International Pediatric Research Foundation Early Investigators’ Exchange Program and the Amgen Irish Nephrology Society Specialist Registrar Research Bursary. N.M. is supported by funding from the National Institute of Health (T32-DK007726) Grant at Boston Children’s Hospital. T.M.K. is supported by a Post-Doctoral Fellowship award from the KRESCENT Program, a national kidney research training partnership of the Kidney Foundation of Canada, the Canadian Society of Nephrology, and the Canadian Institutes of Health Research. F.H. and S.S. are supported by the Begg Family Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kitzler, T.M., Schneider, R., Kohl, S. et al. COL4A1 mutations as a potential novel cause of autosomal dominant CAKUT in humans. Hum Genet 138, 1105–1115 (2019). https://doi.org/10.1007/s00439-019-02042-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00439-019-02042-4