Abstract
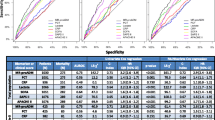
Early diagnosis of sepsis and its severity stratification at admission is critical to improve patient outcomes and to ensure the optimal use of health care resources. In order to assess the diagnostic potential of mid-regional pro-adrenomedullin (MR-proADM) in septic paediatric patients in comparison with procalcitonin (PCT), and to evaluate the usefulness of a single early determination of MR-proADM as a stratification and severity prediction tool, a prospective observational study was conducted. Seventy-three paediatric patients with a suspicion of sepsis were included. A single blood test was carried out at initial time to analyse infection biomarkers. PCT values were significantly higher in septic patients in comparison with non-septic patients (p = 0.03) with an AUC of 0.748 (p = 0.003). Levels of MR-proADM significantly increased in patients with severe sepsis (p = 0.048), with an AUC of 0.729 (p = 0.013). MR-proADM showed a positive correlation with pSOFA, PRISM III, and PELOD-2 severity scores. Levels of MR-proADM were significantly higher in patients who required vasoactive drugs (p = 0.02) or presented renal dysfunction (p = 0.004).
Conclusion: PCT appeared to be superior to MR-proADM in diagnosing sepsis. Determining MR-proADM plasma levels at the initial phase of sepsis could be a useful tool for sepsis stratification and morbidity prediction before organ failure occurs. The present results need to be assessed with larger sample size studies.
What is Known: •CRP and PCT are already included in clinical practice to assess sepsis and estimate disease severity, although their sensitivity and specificity are lower than desired. •ADM is a protein that has immune and vascular modulation actions, and its blood levels are increased in adult and paediatric sepsis. •ADM is a promising tool for early diagnosis and prognostic assessment in adult sepsis. | |
What is New: •PCT appeared to be superior to MR-proADM in diagnosing paediatric sepsis. •MR-proADM plasma levels could be a useful tool for paediatric sepsis stratification and morbidity prediction. |


Similar content being viewed by others
Abbreviations
- ACCM:
-
American College of Critical Care Medicine
- APACHE II:
-
Acute Physiology and Chronic Health disease Classification System II
- AUC:
-
Area under the curve
- CRP:
-
C-reactive protein.
- GNB:
-
Gram-negative bacilli
- GNC:
-
Gram-negative cocci
- GNCB:
-
Gram-negative cocci-bacilli
- GPC:
-
Gram-positive cocci
- ICU:
-
Intensive care unit
- IQR:
-
Interquartile ranges
- L:
-
Litre
- LH+:
-
Likelihood ratio
- LOS:
-
Length of hospitalization
- ml:
-
Millilitre
- MR-proADM:
-
Mid-regional pro-adrenomedullin
- MV:
-
Mechanical ventilation
- ng:
-
Nanogram
- nmol:
-
Nanomol
- NPV:
-
Negative predictive value
- PCT:
-
Procalcitonin
- PELOD-2:
-
Paediatric Logistic Organ Dysfunction Score-2
- PICU:
-
Paediatric Intensive Care Unit
- PPV:
-
Positive predictive value
- PRISM III:
-
Paediatric Risk of Mortality Score III
- pSOFA:
-
paediatric Sequential Organ Failure Assessment
- ROC:
-
Receiver operating characteristic
- SAPS II:
-
Simplified Acute Physiology Score
- Se:
-
Sensitivity
- SOFA:
-
Sequential Organ Failure Assessment
- SP:
-
Specificity
- TRACE:
-
Time-Resolved Amplified Cryptate Emission
References
Weiss SL, Fitzgerald JC, Pappachan J, Wheeler D, Jaramillo-Bustamante JC, Salloo A, Singhi SC, Erickson S, Roy JA, Bush JL, Nadkarni VM, Thomas NJ, Sepsis Prevalence, Outcomes, and Therapies (SPROUT) Study Investigators and Pediatric Acute Lung Injury and Sepsis Investigators (PALISI) Network (2015) Global epidemiology of pediatric severe sepsis: the sepsis prevalence, outcomes, and therapies study. Am J Respir Crit Care Med 191(10):1147–1157
Boeddha NP, Schlapbach LJ, Driessen GJ, Herberg JA, Rivero-Calle I, Cebey-López M, Klobassa DS, Philipsen R, de Groot R, Inwald DP, Nadel S, Paulus S, Pinnock E, Secka F, Anderson ST, Agbeko RS, Berger C, Fink CG, Carrol ED, Zenz W, Levin M, van der Flier M, Martinón-Torres F, Hazelzet JA, Emonts M, EUCLIDS consortium (2018) Mortality and morbidity in community-acquired sepsis in European pediatric intensive care units: a prospective cohort study from the European Childhood Life-threatening Infectious Disease Study (EUCLIDS). Crit Care 22(1):143
Sargentini V, Collepardo D, D Alessandro M, Petralito G, Ceccarelli G, Alessandri F et al (2017) Piciocchi A5, Angeloni A6, Venditti M3 BA. Role of biomarkers in adult sepsis and their application for a good laboratory practice: a pilot study. J Biol Regul Homeost Agents 31(4):1147–1154
Christ-Crain M, Morgenthaler NG, Struck J, Harbarth S, Bergmann A, Müller B (2005) Mid-regional pro-adrenomedullin as a prognostic marker in sepsis: an observational study. Crit Care 9(6):R816–R824
Hirata Y, Mitaka C, Sato K, Nagura T, Tsunoda Y, Amaha K, Marumo F (1996) Increased circulating adrenomedullin, a novel vasodilatory peptide, in sepsis. J Clin Endocrinol Metab 81(4):1449–1453
Zudaire E, Portal-Núñez S, Cuttitta F (2006) The central role of adrenomedullin in host defense. J Leukoc Biol 80:237–244
Kitamura K, Kangawa K, Kawamoto M, Ichiki Y, Nakamura S, Matsuo H, Eto T (1993) Adrenomedullin: a novel hypotensive peptide isolated from human pheochromocytoma. Biochem Biophys Res Commun 192(2):553–560
Struck J, Tao C, Morgenthaler NG, Bergmann A (2004) Identification of an adrenomedullin precursor fragment in plasma of sepsis patients. Peptides. 25(8):1369–1372
Benito J, Luaces-Cubells C, Mintegi S, Astobiza E, Martinez-Indart L, Valls-Lafont A, García-García JJ (2013) Lack of value of midregional pro-adrenomedullin and C-terminal pro-endothelin-1 for prediction of severe bacterial infections in infants with fever without a source. Eur J Pediatr 172(11):1441–1449
Oncel MY, Dilmen U, Erdeve O, Ozdemir R, Calisici E, Yurttutan S, Canpolat FE, Oguz SS, Uras N (2012) Proadrenomedullin as a prognostic marker in neonatal sepsis. Pediatr Res 72(5):507–512
Angeletti S, Battistoni F, Fioravanti M, Bernardini S, Dicuonzo G (2013) Procalcitonin and mid-regional pro-adrenomedullin test combination in sepsis diagnosis. Clin Chem Lab Med 51(5):1059–1067
Suberviola B, Castellanos-Ortega A, Ruiz Ruiz A, Lopez-Hoyos M, Santibañez M (2013) Hospital mortality prognostication in sepsis using the new biomarkers suPAR and proADM in a single determination on ICU admission. Intensive Care Med 39(11):1945–1952
Matics TJ, Sanchez-Pinto LN (2017) Adaptation and validation of a pediatric sequential organ failure assessment score and evaluation of the Sepsis-3 definitions in critically ill children. JAMA Pediatr 171(10):e172352
Lacroix J, Cotting J (2005) Pediatric Acute Lung Injury and Sepsis Investigators (PALISI) Network. Severity of illness and organ dysfunction scoring in children. Pediatr Crit Care Med 6(3):s126–s134
Jordan I, Corniero P, Balaguer M, Ortiz J, Vila D, Velasco J, Cambra FJ, Esteban E (2014) Adrenomedullin is a useful biomarker for the prognosis of critically ill septic children. Biomark Med 8(9):1065–1072
Rey C, García-Hernández I, Concha A, Martínez-Camblor P, Botrán M, Medina A, Prieto B, López-Herce J (2013) Pro-adrenomedullin, pro-endothelin-1, procalcitonin, C-reactive protein and mortality risk in critically ill children: a prospective study. Crit Care 17(5):R240
Davis AL, Carcillo JA, Aneja RK, Deymann AJ, Lin JC, Nguyen TC, Okhuysen-Cawley RS, Relvas MS, Rozenfeld RA, Skippen PW, Stojadinovic BJ, Williams EA, Yeh TS, Balamuth F, Brierley J, de Caen AR, Cheifetz IM, Choong K, Conway E Jr, Cornell T, Doctor A, Dugas MA, Feldman JD, Fitzgerald JC, Flori HR, Fortenberry JD, Graciano AL, Greenwald BM, Hall MW, Han YY, Hernan LJ, Irazuzta JE, Iselin E, van der Jagt E, Jeffries HE, Kache S, Katyal C, Kissoon N, Kon AA, Kutko MC, MacLaren G, Maul T, Mehta R, Odetola F, Parbuoni K, Paul R, Peters MJ, Ranjit S, Reuter-Rice KE, Schnitzler EJ, Scott HF, Torres A Jr, Weingarten-Arams J, Weiss SL, Zimmerman JJ, Zuckerberg AL (2017) American College of Critical Care Medicine clinical practice parameters for hemodynamic support of pediatric and neonatal septic shock. Crit Care Med 45(6):1061–1093
Goldstein B, Giroir B, Randolph A (2005) International consensus conference on pediatric sepsis. International pediatric sepsis consensus conference: definitions for sepsis and organ dysfunction in pediatrics. Pediatr Crit Care Med 6(1):2–8
Angeletti S, Spoto S, Fogolari M, Cortigiani M, Fioravanti M, De Florio L et al (2015) Diagnostic and prognostic role of procalcitonin (PCT) and MR-pro-Adrenomedullin (MR-proADM) in bacterial infections. APMIS. 123(9):740–748
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the study:Anna Solé-Ribalta contributed on conceptualization and design, methodology, investigation, data curation and formal analysis; Sara Bobillo-Pérez contributed on investigation, data curation and formal analysisAnna Valls contributed on methodology; Monica Girona-Alarcón contributed on conceptualization and design and investigation; Cristian Launes contributed on methodology and supervision; Francisco José Cambra contributed on investigation and supervision;Iolanda Jordán contributed on conceptualization and design, methodology, formal analysis and supervision;Elisabeth Esteban contributed on investigation formal analysis and supervision.
All authors also participated in the writing and/or revision of the manuscript: Anna Solé-Ribalta, Sara Bobillo-Pérez, Anna Valls, Monica Girona-Alarcon participated in drafting the initial manuscript; Anna Solé-Ribalta, Cristian Launes, Francisco José Cambra, Iolanda Jordan and Elisabeth Esteban participated in review and editing the manuscript.
All authors gave the final approval of the version to be published and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Communicated by Nicole Ritz
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 13 kb)
Rights and permissions
About this article
Cite this article
Solé-Ribalta, A., Bobillo-Pérez, S., Valls, A. et al. Diagnostic and prognostic value of procalcitonin and mid-regional pro-adrenomedullin in septic paediatric patients. Eur J Pediatr 179, 1089–1096 (2020). https://doi.org/10.1007/s00431-020-03587-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-020-03587-7