Abstract
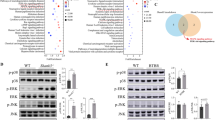
Restless legs syndrome (RLS) is characterized by an urge to move legs, usually accompanied by uncomfortable sensations. RLS symptoms generally happen at night and can be relieved by movements. Genetic studies have linked polymorphisms in BTBD9 to a higher risk of RLS. Knockout of BTBD9 homolog in mice (Btbd9) and fly results in RLS-like phenotypes. A dysfunctional dopaminergic system is associated with RLS. However, the function of BTBD9 in the dopaminergic system and RLS is not clear. Here, we made use of the simple Caenorhabditis elegans nervous system. Loss of hpo-9, the worm homolog of BTBD9, resulted in hyperactive egg-laying behavior. Analysis of genetic interactions between hpo-9 and genes for dopamine receptors (dop-1, dop-3) indicated that hpo-9 and dop-1 worked similarly. Reporter assays of dop-1 and dop-3 revealed that hpo-9 knockout led to a significant increase of DOP-3 expression. This appears to be evolutionarily conserved in mice with an increased D2 receptor (D2R) mRNA in the striatum of the Btbd9 knockout mice. Furthermore, the striatal D2R protein was significantly decreased and Dynamin I was increased. Overall, activities of DA neurons in the substantia nigra were not altered, but the peripheral D1R pathway was potentiated in the Btbd9 knockout mice. Finally, we generated and characterized the dopamine neuron-specific Btbd9 knockout mice and detected an active-phase sleepiness, suggesting that dopamine neuron-specific loss of Btbd9 is sufficient to disturb the sleep. Our results suggest that increased activities in the D1R pathway, decreased activities in the D2R pathway, or both may contribute to RLS.










Similar content being viewed by others
References
Abetz L, Allen R, Follet A, Washburn T, Earley C, Kirsch J, Knight H (2004) Evaluating the quality of life of patients with restless legs syndrome. Clin Ther 26:925–935
Akhisaroglu M, Kurtuncu M, Manev H, Uz T (2005) Diurnal rhythms in quinpirole-induced locomotor behaviors and striatal D2/D3 receptor levels in mice. Pharmacol Biochem Behav 80:371–377
Allen RP, Connor JR, Hyland K, Earley CJ (2009) Abnormally increased CSF 3-Ortho-methyldopa (3-OMD) in untreated restless legs syndrome (RLS) patients indicates more severe disease and possibly abnormally increased dopamine synthesis. Sleep Med 10:123–128
Bachmann CG, Rolke R, Scheidt U, Stadelmann C, Sommer M, Pavlakovic G, Happe S, Treede RD, Paulus W (2010) Thermal hypoaesthesia differentiates secondary restless legs syndrome associated with small fibre neuropathy from primary restless legs syndrome. Brain 133:762–770
Bara-Jimenez W, Aksu M, Graham B, Sato S, Hallett M (2000) Periodic limb movements in sleep: state-dependent excitability of the spinal flexor reflex. Neurology 54:1609–1616
Ben-Sreti MM, Gonzalez JP, Sewell RD (1983) Differential effects of SKF 38393 and LY 141865 on nociception and morphine analgesia. Life Sci 33(Suppl 1):665–668
Berretta N, Bernardi G, Mercuri NB (2010) Firing properties and functional connectivity of substantia nigra pars compacta neurones recorded with a multi-electrode array in vitro. J Physiol 588:1719–1735
Brewer KL, Baran CA, Whitfield BR, Jensen AM, Clemens S (2014) Dopamine D3 receptor dysfunction prevents anti-nociceptive effects of morphine in the spinal cord. Front Neural Circuits 8:62
Castaneda TR, de Prado BM, Prieto D, Mora F (2004) Circadian rhythms of dopamine, glutamate and GABA in the striatum and nucleus accumbens of the awake rat: modulation by light. J Pineal Res 36:177–185
Chase DL, Koelle MR (2004) Genetic analysis of RGS protein function in Caenorhabditis elegans. Methods Enzymol 389:305–320
Chase DL, Koelle MR (2007) Biogenic amine neurotransmitters in C. elegans. WormBook, Beijing, pp 1–15
Chase DL, Pepper JS, Koelle MR (2004) Mechanism of extrasynaptic dopamine signaling in Caenorhabditis elegans. Nat Neurosci 7:1096–1103
Clemens S, Hochman S (2004) Conversion of the modulatory actions of dopamine on spinal reflexes from depression to facilitation in D3 receptor knock-out mice. J Neurosci 24:11337–11345
Connor JR, Wang XS, Allen RP, Beard JL, Wiesinger JA, Felt BT, Earley CJ (2009) Altered dopaminergic profile in the putamen and substantia nigra in restless leg syndrome. Brain 132:2403–2412
Dang MT, Yokoi F, McNaught KS, Jengelley TA, Jackson T, Li J, Li Y (2005) Generation and characterization of Dyt1 DeltaGAG knock-in mouse as a model for early-onset dystonia. Exp Neurol 196:452–463
Dang MT, Yokoi F, Cheetham CC, Lu J, Vo V, Lovinger DM, Li Y (2012) An anticholinergic reverses motor control and corticostriatal LTD deficits in Dyt1 DeltaGAG knock-in mice. Behav Brain Res 226:465–472
DeAndrade MP, Yokoi F, van Groen T, Lingrel JB, Li Y (2011) Characterization of Atp1a3 mutant mice as a model of rapid-onset dystonia with parkinsonism. Behav Brain Res 216:659–665
DeAndrade MP, Johnson RL Jr, Unger EL, Zhang L, van Groen T, Gamble KL, Li Y (2012a) Motor restlessness, sleep disturbances, thermal sensory alterations and elevated serum iron levels in Btbd9 mutant mice. Hum Mol Genet 21:3984–3992
DeAndrade MP, Zhang L, Doroodchi A, Yokoi F, Cheetham CC, Chen HX, Roper SN, Sweatt JD, Li Y (2012b) Enhanced hippocampal long-term potentiation and fear memory in Btbd9 mutant mice. PLoS One 7:e35518
Earley CJ, Hyland K, Allen RP (2001) CSF dopamine, serotonin, and biopterin metabolites in patients with restless legs syndrome. Mov Disord 16:144–149
Earley CJ, Hyland K, Allen RP (2006) Circadian changes in CSF dopaminergic measures in restless legs syndrome. Sleep Med 7:263–268
Earley CJ, Kuwabara H, Wong DF, Gamaldo C, Salas R, Brasic J, Ravert HT, Dannals RF, Allen RP (2011) The dopamine transporter is decreased in the striatum of subjects with restless legs syndrome. Sleep 34:341–347
Earley CJ, Kuwabara H, Wong DF, Gamaldo C, Salas RE, Brasic JR, Ravert HT, Dannals RF, Allen RP (2013) Increased synaptic dopamine in the putamen in restless legs syndrome. Sleep 36:51–57
Erikson KM, Jones BC, Hess EJ, Zhang Q, Beard JL (2001) Iron deficiency decreases dopamine D1 and D2 receptors in rat brain. Pharmacol Biochem Behav 69:409–418
Esteves AM, de Mello MT, Lancellotti CL, Natal CL, Tufik S (2004) Occurrence of limb movement during sleep in rats with spinal cord injury. Brain Res 1017:32–38
Ezak MJ, Ferkey DM (2010) The C. elegans D2-like dopamine receptor DOP-3 decreases behavioral sensitivity to the olfactory stimulus 1-octanol. PLoS One 5:e9487
Ferre S, Quiroz C, Guitart X, Rea W, Seyedian A, Moreno E, Casado-Anguera V, Diaz-Rios M, Casado V, Clemens S, Allen RP, Earley CJ, Garcia-Borreguero D (2017) Pivotal role of adenosine neurotransmission in Restless legs syndrome. Front Neurosci 11:722
Ferri R, Proserpio P, Rundo F, Lanza A, Sambusida K, Redaelli T, De Carli F, Nobili L (2015) Neurophysiological correlates of sleep leg movements in acute spinal cord injury. Clin Neurophysiol 126:333–338
Freeman A, Pranski E, Miller RD, Radmard S, Bernhard D, Jinnah HA, Betarbet R, Rye DB, Sanyal S (2012) Sleep fragmentation and motor restlessness in a Drosophila model of Restless legs syndrome. Curr Biol CB 22:1142–1148
Gao X, Zhang Y, Wu G (2000) Effects of dopaminergic agents on carrageenan hyperalgesia in rats. Eur J Pharmacol 406:53–58
Garcia Borreguero D, Winkelmann J, Allen RP (2017) Introduction: towards a better understanding of the science of RLS/WED. Sleep Med 31:1–2
Garcia-Borreguero D, Silber MH, Winkelman JW, Hogl B, Bainbridge J, Buchfuhrer M, Hadjigeorgiou G, Inoue Y, Manconi M, Oertel W, Ondo W, Winkelmann J, Allen RP (2016) Guidelines for the first-line treatment of restless legs syndrome/Willis-Ekbom disease, prevention and treatment of dopaminergic augmentation: a combined task force of the IRLSSG, EURLSSG, and the RLS-foundation. Sleep Med 21:1–11
Gardner M, Rosell M, Myers EM (2013) Measuring the effects of bacteria on C. elegans behavior using an egg retention assay. J Vis Exp 80:e51203
Greenbaum D, Colangelo C, Williams K, Gerstein M (2003) Comparing protein abundance and mRNA expression levels on a genomic scale. Genome Biol 4:117
Hodgkin J, Barnes TM (1991) More is not better: brood size and population growth in a self-fertilizing nematode. Proc Biol Sci 246:19–24
Hore SK, Dumka VK, Kumar D, Tripathi HC, Tandan SK (1997) Central noradrenergic and dopaminergic modulation of brewer's yeast-induced inflammation and nociception in rats. Indian J Med Res 105:93–97
Iwata K, Ito K, Fukuzaki A, Inaki K, Haga T (1999) Dynamin and rab5 regulate GRK2-dependent internalization of dopamine D2 receptors. Eur J Biochem 263:596–602
Kamath RS, Martinez-Campos M, Zipperlen P, Fraser AG, Ahringer J (2001) Effectiveness of specific RNA-mediated interference through ingested double-stranded RNA in Caenorhabditis elegans. Genome Biol 2:Research0002
Kamath RS, Fraser AG, Dong Y, Poulin G, Durbin R, Gotta M, Kanapin A, Le Bot N, Moreno S, Sohrmann M, Welchman DP, Zipperlen P, Ahringer J (2003) Systematic functional analysis of the Caenorhabditis elegans genome using RNAi. Nature 421:231–237
Keeler BE, Baran CA, Brewer KL, Clemens S (2012) Increased excitability of spinal pain reflexes and altered frequency-dependent modulation in the dopamine D3-receptor knockout mouse. Exp Neurol 238:273–283
Keeler JF, Pretsell DO, Robbins TW (2014) Functional implications of dopamine D1 vs. D2 receptors: A 'prepare and select' model of the striatal direct vs. indirect pathways. Neuroscience 282:156–175
Khaldy H, Leon J, Escames G, Bikjdaouene L, Garcia JJ, Acuna-Castroviejo D (2002) Circadian rhythms of dopamine and dihydroxyphenyl acetic acid in the mouse striatum: effects of pinealectomy and of melatonin treatment. Neuroendocrinology 75:201–208
Kiritani T, Wickersham IR, Seung HS, Shepherd GM (2012) Hierarchical connectivity and connection-specific dynamics in the corticospinal-corticostriatal microcircuit in mouse motor cortex. J Neurosci 32:4992–5001
Klaus A, Alves da Silva J, Costa RM (2019) What, If, and when to move: basal ganglia circuits and self-paced action initiation. Annu Rev Neurosci 42:459–483
Koblinger K, Fuzesi T, Ejdrygiewicz J, Krajacic A, Bains JS, Whelan PJ (2014) Characterization of A11 neurons projecting to the spinal cord of mice. PLoS One 9:e109636
Koenig JA, Edwardson JM (1997) Endocytosis and recycling of G protein-coupled receptors. Trends Pharmacol Sci 18:276–287
Lyu S, DeAndrade MP, Mueller S, Oksche A, Walters AS, Li Y (2019a) Hyperactivity, dopaminergic abnormalities, iron deficiency and anemia in an in vivo opioid receptors knockout mouse: Implications for the restless legs syndrome. Behav Brain Res 374:112123
Lyu S, Xing H, DeAndrade MP, Liu Y, Perez PD, Yokoi F, Febo M, Walters AS, Li Y (2019b) The role of BTBD9 in striatum and restless legs syndrome. eNeuro 0277:19
Lyu S, Xing H, DeAndrade MP, Perez PD, Zhang K, Liu Y, Yokoi F, Febo M, Walters AS, Li Y (2019c) The role of BTBD9 in the cerebral cortex and the pathogenesis of restless legs syndrome. Exp Neurol 323:113111
Marconi S, Scaglione C, Pizza F, Rizzo G, Plazzi G, Vetrugno R, La Manna G, Campieri C, Stefoni S, Montagna P, Martinelli P (2012) Group I nonreciprocal inhibition in restless legs syndrome secondary to chronic renal failure. Parkinsonism Relat Disord 18:362–366
Meiser J, Weindl D, Hiller K (2013) Complexity of dopamine metabolism. Cell Commun Signal 11:34
Meneely S, Dinkins M-L, Kassai M, Lyu S, Liu Y, Lin C-T, Brewer K, Li Y, Clemens S (2018) Differential dopamine D1 and D3 receptor modulation and expression in the spinal cord of two mouse models of Restless legs syndrome. Front Behav Neurosci 12:199
Michaud M, Soucy JP, Chabli A, Lavigne G, Montplaisir J (2002) SPECT imaging of striatal pre- and postsynaptic dopaminergic status in restless legs syndrome with periodic leg movements in sleep. J Neurol 249:164–170
Ondo WG, He Y, Rajasekaran S, Le WD (2000) Clinical correlates of 6-hydroxydopamine injections into A11 dopaminergic neurons in rats: a possible model for restless legs syndrome. Mov Disord 15:154–158
Paladini CA, Robinson S, Morikawa H, Williams JT, Palmiter RD (2003) Dopamine controls the firing pattern of dopamine neurons via a network feedback mechanism. Proc Natl Acad Sci USA 100:2866–2871
Qu S, Le W, Zhang X, Xie W, Zhang A, Ondo WG (2007) Locomotion is increased in a11-lesioned mice with iron deprivation: a possible animal model for restless legs syndrome. J Neuropathol Exp Neurol 66:383–388
Ringstad N, Horvitz HR (2008) FMRFamide neuropeptides and acetylcholine synergistically inhibit egg-laying by C. elegans. Nat Neurosci 11:1168–1176
Rooney KF, Sewell RD (1989) Evaluation of selective actions of dopamine D-1 and D-2 receptor agonists and antagonists on opioid antinociception. Eur J Pharmacol 168:329–336
Schafer WR (2005) Egg-laying. In: WormBook (ed) The C. elegans Research Community. WormBook. http://www.wormbook.org.
Schafer WR, Kenyon CJ (1995) A calcium-channel homologue required for adaptation to dopamine and serotonin in Caenorhabditis elegans. Nature 375:73–78
Schormair B et al (2017) Identification of novel risk loci for restless legs syndrome in genome-wide association studies in individuals of European ancestry: a meta-analysis. Lancet Neurol 16:898–907
Spijker S (2011) Dissection of Rodent Brain Regions. Neuroproteomics 57:13–26
Stefansson H et al (2007) A genetic risk factor for periodic limb movements in sleep. N Engl J Med 357:639–647
Stogios PJ, Prive GG (2004) The BACK domain in BTB-kelch proteins. Trends Biochem Sci 29:634–637
Stogios PJ, Downs GS, Jauhal JJ, Nandra SK, Prive GG (2005) Sequence and structural analysis of BTB domain proteins. Genome Biol 6:R82
Thompson D, Martini L, Whistler JL (2010) Altered ratio of D1 and D2 dopamine receptors in mouse striatum is associated with behavioral sensitization to cocaine. PLoS One 5:e11038
Thompson ML, Chen P, Yan X, Kim H, Borom AR, Roberts NB, Caldwell KA, Caldwell GA (2014) TorsinA rescues ER-associated stress and locomotive defects in C. elegans models of ALS. Dis Model Mech 7:233–243
Tings T, Baier PC, Paulus W, Trenkwalder C (2003) Restless legs syndrome induced by impairment of sensory spinal pathways. J Neurol 250:499–500
Trenkwalder C, Paulus W, Walters AS (2005) The restless legs syndrome. Lancet Neurol 4:465–475
Trenkwalder C, Allen R, Hogl B, Clemens S, Patton S, Schormair B, Winkelmann J (2018) Comorbidities, treatment, and pathophysiology in restless legs syndrome. Lancet Neurol 17:994–1005
Trent C, Tsuing N, Horvitz HR (1983) Egg-laying defective mutants of the nematode Caenorhabditis elegans. Genetics 104:619–647
Verma A, Kulkarni SK (1993) Modulatory role of D-1 and D-2 dopamine receptor subtypes in nociception in mice. J Psychopharmacol 7:270–275
Waggoner LE, Zhou GT, Schafer RW, Schafer WR (1998) Control of alternative behavioral states by serotonin in Caenorhabditis elegans. Neuron 21:203–214
Wall NR, De La Parra M, Callaway EM, Kreitzer AC (2013) Differential innervation of direct- and indirect-pathway striatal projection neurons. Neuron 79:347–360
Weinshenker D, Garriga G, Thomas JH (1995) Genetic and pharmacological analysis of neurotransmitters controlling egg laying in C. elegans. J Neurosci 15:6975–6985
Winkelmann J et al (2007) Genome-wide association study of restless legs syndrome identifies common variants in three genomic regions. Nat Genet 39:1000–1006
Yokoi F, Dang MT, Liu J, Gandre JR, Kwon K, Yuen R, Li Y (2015) Decreased dopamine receptor 1 activity and impaired motor-skill transfer in Dyt1 DeltaGAG heterozygous knock-in mice. Behav Brain Res 279:202–210
Yokota T, Hirose K, Tanabe H, Tsukagoshi H (1991) Sleep-related periodic leg movements (nocturnal myoclonus) due to spinal cord lesion. J Neurol Sci 104:13–18
Zarrindast MR, Moghaddampour E (1989) Opposing influences of D-1 and D-2 dopamine receptors activation on morphine-induced antinociception. Arch Int Pharmacodyn Ther 300:37–50
Zhao H, Zhu W, Pan T, Xie W, Zhang A, Ondo WG, Le W (2007) Spinal cord dopamine receptor expression and function in mice with 6-OHDA lesion of the A11 nucleus and dietary iron deprivation. J Neurosci Res 85:1065–1076
Acknowledgements
We would like to thank Dr. Shohei Mitani for the hpo-9(tm3719) strain, Dr. Lin Zhang, Chad C. Cheetham, Sung Min Han, Jack Vibbert, Pauline Cottee, Jessica Winek, and Hieu Hoang for their technical assistance and stimulating discussions. This work was supported by a grant from Restless Legs Syndrome Foundation (2015 RLS Research Grants), and startup funds from the Departments of Neurology at UAB and UF, and the National Institutes of Health [Grants NS54246, NS57098, NS65273, NS72872, NS74423, and NS82244]. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest with the contents of this article (The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health).
Human and animal rights
This article does not contain any studies with human participants performed by any of the authors. All procedures performed in studies involving animals were in accordance with the ethical standards of East Carolina University and the University of Florida.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lyu, S., Doroodchi, A., Xing, H. et al. BTBD9 and dopaminergic dysfunction in the pathogenesis of restless legs syndrome. Brain Struct Funct 225, 1743–1760 (2020). https://doi.org/10.1007/s00429-020-02090-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00429-020-02090-x