Abstract
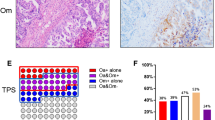
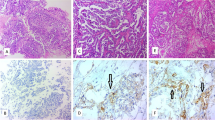
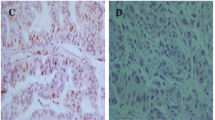
Endometrial carcinoma programmed death-ligand 1 (PD-L1) expression in tumor cells (TCs) and tumor-associated inflammatory cells (ICs) have recently been reported in several studies which vary in terms of their cohort size, design, and methodology. We aimed to assess PD-L1 staining in endometrial carcinomas and correlate this with clinical and pathological factors and PTEN, ARID1A, p53, and MMR protein expression. PD-L1 immunohistochemistry was performed on whole tissue sections of all tumor blocks of 59 consecutive unselected endometrial carcinomas between November 2018 and September 2019. TC and IC PD-L1 positivity with a 1% cut-off value was observed in 10.2% and 67.8% of cases, respectively, and with a 5% cut-off value in 3.4% and 42.4% of cases, respectively. TC PD-L1 positivity with both 1% and 5% cut-off values was significantly related to ARID1A loss (p = 0.001 and p = 0.046, respectively). IC PD-L1 positivity with 1% and 5% cut-off values and combined score were significantly associated with MMR protein deficiency (p = 0.041, p = 0.031, and p = 0.028, respectively). Advanced stage tumors exhibited more frequent PD-L1 expression in ICs (p = 0.039). MELF-type myometrial invasion pattern was more common in tumors with ARID1A loss (p = 0.047). We observed higher rates of IC PD-L1 positivity in endometrial carcinomas than documented in prior studies; this may be related to our usage of “recent” paraffin blocks and whole tissue sections of all tumor blocks. There was a much higher PD-L1 expression in the ICs compared to TCs in our cases. We confirm a previously documented association between MMR deficiency and PD-L1 expression and show a novel association between ARID1A loss and PD-L1 expression in endometrial carcinomas. ARID1A loss represents a potential biomarker of immune checkpoint inhibitor response in endometrial carcinoma.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Morice P, Leary A, Creutzberg C, Abu-Rustum N, Darai E (2016) Endometrial cancer. Lancet 387(10023):1094–1108. https://doi.org/10.1016/S0140-6736(15)00130-0
Fashoyin-Aje L, Donoghue M, Chen H, He K, Veeraraghavan J, Goldberg KB, Keegan P, McKee AE, Pazdur R (2019) FDA approval summary: pembrolizumab for recurrent locally advanced or metastatic gastric or gastroesophageal junction adenocarcinoma expressing PD-L1. Oncologist 24(1):103–109. https://doi.org/10.1634/theoncologist.2018-0221
Gubens MA, Sequist LV, Stevenson JP, Powell SF, Villaruz LC, Gadgeel SM, Langer CJ, Patnaik A, Borghaei H, Jalal SI, Fiore J, Saraf S, Raftopoulos H, Gandhi L (2019) Pembrolizumab in combination with ipilimumab as second-line or later therapy for advanced non–small-cell lung cancer: KEYNOTE-021 cohorts D and H. Lung Cancer 130:59–66. https://doi.org/10.1016/j.lungcan.2018.12.015
National Institutes of Health (2016) Study of pembrolizumab (MK-3475) versus placebo after complete resection of high-risk stage III melanoma (MK-3475-054/KEYNOTE-054)
Eggink FA, Van Gool IC, Leary A, Pollock PM, Crosbie EJ, Mileshkin L et al (2017) Immunological profiling of molecularly classified high-risk endometrial cancers identifies POLE-mutant and microsatellite unstable carcinomas as candidates for checkpoint inhibition. Oncoimmunology 6(2):e1264565. https://doi.org/10.1080/2162402X.2016.1264565
Bregar A, Deshpande A, Grange C, Zi T, Stall J, Hirsch H, Reeves J, Sathyanarayanan S, Growdon WB, Rueda BR (2017) Characterization of immune regulatory molecules B7-H4 and PD-L1 in low and high grade endometrial tumors. Gynecol Oncol 145(3):446–452. https://doi.org/10.1016/j.ygyno.2017.03.006
Yamashita H, Nakayama K, Ishikawa M, Nakamura K, Ishibashi T, Sanuki K et al (2018) Microsatellite instability is a biomarker for immune checkpoint inhibitors in endometrial cancer. Oncotarget 9(5):5652. https://doi.org/10.18632/oncotarget.23790
Li Z, Joehlin-Price AS, Rhoades J, Ayoola-Adeola M, Miller K, Parwani AV, Backes FJ, Felix AS, Suarez AA (2018) Programmed death ligand 1 expression among 700 consecutive endometrial cancers: strong association with mismatch repair protein deficiency. Int J Gynecol Cancer 28(1):59–68. https://doi.org/10.1097/IGC.0000000000001120
Kim J, Kim S, Lee HS, Yang W, Cho H, Chay DB, Cho SJ, Hong S, Kim JH (2018) Prognostic implication of programmed cell death 1 protein and its ligand expressions in endometrial cancer. Gynecol Oncol 149(2):381–387. https://doi.org/10.1016/j.ygyno.2018.02.013
Asaka S, Yen TT, Wang TL, Shih IM, Gaillard S (2019) T cell-inflamed phenotype and increased Foxp3 expression in infiltrating T-cells of mismatch-repair deficient endometrial cancers. Mod Pathol 32(4):576–584. https://doi.org/10.1038/s41379-018-0172-x
Kucukgoz Gulec U, Bagir EK, Paydas S, Guzel AB, Gumurdulu D, Vardar MA (2019) Programmed death-1 (PD-1) and programmed death-ligand 1 (PD-L1) expressions in type 2 endometrial cancer. Arch Gynecol Obstet 300(2):377–382. https://doi.org/10.1007/s00404-019-05180-2
Talhouk A, McConechy M, Leung S, Li-Chang H, Kwon J, Melnyk N et al (2015) A clinically applicable molecular-based classification for endometrial cancers. Br J Cancer 113(2):299–310. https://doi.org/10.1038/bjc.2015.190
Pasanen A, Ahvenainen T, Pellinen T, Vahteristo P, Loukovaara M, Bützow R (2020) PD-L1 expression in endometrial carcinoma cells and intratumoral immune cells: differences across histologic and TCGA-based molecular subgroups. Am J Surg Pathol 44(2):174–181. https://doi.org/10.1097/PAS.0000000000001395
Inaguma S, Wang Z, Lasota J, Sarlomo-Rikala M, McCue PA, Ikeda H et al (2016) Comprehensive immunohistochemical study of programmed cell death ligand 1 (PD-L1). Analysis in 5536 cases revealed consistent expression in trophoblastic tumors. Am J Surg Pathol 40(8):1133. https://doi.org/10.1097/PAS.0000000000000653
Quick CM, May T, Horowitz NS, Nucci MR (2012) Low-grade, low-stage endometrioid endometrial adenocarcinoma: a clinicopathologic analysis of 324 cases focusing on frequency and pattern of myoinvasion. Int J Gynecol Pathol 31(4):337–343. https://doi.org/10.1097/PGP.0b013e31823ff422
Mills AM, Liou S, Ford JM, Berek JS, Pai RK, Longacre TA (2014) Lynch syndrome screening should be considered for all patients with newly diagnosed endometrial cancer. Am J Surg Pathol 38(11):1501–1509. https://doi.org/10.1097/PAS.0000000000000321
Wiegand KC, Shah SP, Al-Agha OM, Zhao Y, Tse K, Zeng T et al (2010) ARID1A mutations in endometriosis-associated ovarian carcinomas. N Engl J Med 363(16):1532–1543. https://doi.org/10.1056/NEJMoa1008433
Lu F-I, Gilks CB, Mulligan A-M, Ryan P, Allo G, Sy K, Shaw PA, Pollett A, Clarke BA (2012) Prevalence of loss of expression of DNA mismatch repair proteins in primary epithelial ovarian tumors. Int J Gynecol Pathol 31(6):524–531
Alkushi A, Köbel M, Kalloger SE, Gilks CB (2010) High-grade endometrial carcinoma: serous and grade 3 endometrioid carcinomas have different immunophenotypes and outcomes. Int J Gynecol Pathol 29(4):343–350. https://doi.org/10.1097/PGP.0b013e31824fe2aa
Köbel M, Ronnett BM, Singh N, Soslow RA, Gilks CB, McCluggage WG (2019) Interpretation of P53 immunohistochemistry in endometrial carcinomas: toward increased reproducibility. Int J Gynecol Pathol 38(1 Suppl 1):123–131. https://doi.org/10.1097/PGP.0000000000000488
Lotan TL, Gurel B, Sutcliffe S, Esopi D, Liu W, Xu J, Hicks JL, Park BH, Humphreys E, Partin AW, Han M, Netto GJ, Isaacs WB, de Marzo AM (2011) PTEN protein loss by immunostaining: analytic validation and prognostic indicator for a high risk surgical cohort of prostate cancer patients. Clin Cancer Res 17(20):6563–6573. https://doi.org/10.1158/1078-0432.CCR-11-1244
Lotan TL, Wei W, Ludkovski O, Morais CL, Guedes LB, Jamaspishvili T, Lopez K, Hawley ST, Feng Z, Fazli L, Hurtado-Coll A, McKenney JK, Simko J, Carroll PR, Gleave M, Lin DW, Nelson PS, Thompson IM, True LD, Brooks JD, Lance R, Troyer D, Squire JA (2016) Analytic validation of a clinical-grade PTEN immunohistochemistry assay in prostate cancer by comparison with PTEN FISH. Mod Pathol 29(8):904–914. https://doi.org/10.1038/modpathol.2016.88
Kulangara K, Zhang N, Corigliano E, Guerrero L, Waldroup S, Jaiswal D, MS MJ, Shah S, Hanks D, Wang J, Lunceford J, Savage MJ, Juco J, Emancipator K (2018) Clinical utility of the combined positive score for programmed death ligand-1 expression and the approval of pembrolizumab for treatment of gastric cancer. Arch Pathol Lab Med 143(3):330–337. https://doi.org/10.5858/arpa.2018-0043-OA
Howitt BE, Shukla SA, Sholl LM, Ritterhouse LL, Watkins JC, Rodig S, Stover E, Strickland KC, D’Andrea AD, Wu CJ, Matulonis UA, Konstantinopoulos PA (2015) Association of polymerase e–mutated and microsatellite-instable endometrial cancers with neoantigen load, number of tumor-infiltrating lymphocytes, and expression of PD-1 and PD-L1. JAMA Oncol 1(9):1319–1323. https://doi.org/10.1001/jamaoncol.2015.2151
Sloan EA, Ring KL, Willis BC, Modesitt SC, Mills AM (2017) PD-L1 expression in mismatch repair-deficient endometrial carcinomas, including Lynch syndrome-associated and MLH1 promoter hypermethylated tumors. Am J Surg Pathol 41(3):326–333. https://doi.org/10.1097/PAS.0000000000000783
Rimm DL, Han G, Taube JM, Yi ES, Bridge JA, Flieder DB, Homer R, West WW, Wu H, Roden AC, Fujimoto J, Yu H, Anders R, Kowalewski A, Rivard C, Rehman J, Batenchuk C, Burns V, Hirsch FR, Wistuba II (2017) A prospective, multi-institutional, pathologist-based assessment of 4 immunohistochemistry assays for PD-L1 expression in non-small cell lung cancer. JAMA Oncol 3(8):1051–1058. https://doi.org/10.1001/jamaoncol.2017.0013
Scheel AH, Dietel M, Heukamp LC, Jöhrens K, Kirchner T, Reu S, Rüschoff J, Schildhaus HU, Schirmacher P, Tiemann M, Warth A, Weichert W, Fischer RN, Wolf J, Buettner R (2016) Harmonized PD-L1 immunohistochemistry for pulmonary squamous-cell and adenocarcinomas. Mod Pathol 29(10):1165–1172. https://doi.org/10.1038/modpathol.2016.117
Adam J, Rouquette I, Damotte D, Badoual C, Danel C, Damiola F, Penault-Llorca F, Lantuejoul S (2017) PL04a. 04: multicentric French harmonization study for PD-L1 IHC testing in NSCLC. J Thorac Oncol 12(1):S11–S12. https://doi.org/10.1016/j.jtho.2016.11.013
Le DT, Uram JN, Wang H, Bartlett BR, Kemberling H, Eyring AD et al (2015) PD-1 blockade in tumors with mismatch-repair deficiency. N Engl J Med 372(26):2509–2520. https://doi.org/10.1056/NEJMoa1500596
Lyford-Pike S, Peng S, Young GD, Taube JM, Westra WH, Akpeng B, Bruno TC, Richmon JD, Wang H, Bishop JA, Chen L, Drake CG, Topalian SL, Pardoll DM, Pai SI (2013) Evidence for a role of the PD-1:PD-L1 pathway in immune resistance of HPV-associated head and neck squamous cell carcinoma. Cancer Res 73(6):1733–1741. https://doi.org/10.1158/0008-5472.CAN-12-2384
Ma C, Patel K, Singhi AD, Ren B, Zhu B, Shaikh F, Sun W (2016) Programmed death-ligand 1 expression is common in gastric cancer associated with Epstein–Barr virus or microsatellite instability. Am J Surg Pathol 40(11):1496–1506. https://doi.org/10.1097/PAS.0000000000000698
Koh J, Go H, Keam B, Kim MY, Nam SJ, Kim TM, Lee SH, Min HS, Kim YT, Kim DW, Jeon YK, Chung DH (2015) Clinicopathologic analysis of programmed cell death-1 and programmed cell death-ligand 1 and 2 expressions in pulmonary adenocarcinoma: comparison with histology and driver oncogenic alteration status. Mod Pathol 28(9):1154–1166. https://doi.org/10.1038/modpathol.2015.63
Barreta A, Sarian LO, Ferracini AC, Costa LBE, Mazzola PG, de Angelo AL et al (2019) Immunohistochemistry expression of targeted therapies biomarkers in ovarian clear cell and endometrioid carcinomas (type I) and endometriosis. Hum Pathol 85:72–81. https://doi.org/10.1016/j.humpath.2018.10.028
Crumley S, Kurnit K, Hudgens C, Fellman B, Tetzlaff MT, Broaddus R (2019) Identification of a subset of microsatellite-stable endometrial carcinoma with high PD-L1 and CD8+ lymphocytes. Mod Pathol 32(3):396–404. https://doi.org/10.1038/s41379-018-0148-x
Gargiulo P, Della Pepa C, Berardi S, Califano D, Scala S, Buonaguro L, Ciliberto G, Brauchli P, Pignata S (2016) Tumor genotype and immune microenvironment in POLE-ultramutated and MSI-hypermutated endometrial cancers: new candidates for checkpoint blockade immunotherapy? Cancer Treat Rev 48:61–68. https://doi.org/10.1016/j.ctrv.2016.06.008
Longoria TC, Eskander RN (2015) Immunotherapy in endometrial cancer-an evolving therapeutic paradigm. Gynecol Oncol Res Pract 2(1):11. https://doi.org/10.1186/s40661-015-0020-3
Herzog T, Arguello D, Reddy S, Gatalica Z (2015) PD-1 and PD-L1 expression in 1599 gynecological malignancies—implications for immunotherapy. Gynecol Oncol 137(1):204–205
Vanderstraeten A, Luyten C, Verbist G, Tuyaerts S, Amant F (2014) Immunotherapy. Mapping the immunosuppressive environment in uterine tumors: implications for immunotherapy. Cancer Immunol Immunother 63(6):545–557. https://doi.org/10.1007/s00262-014-1537-8
Stelloo E, Nout RA, Osse EM, Jürgenliemk-Schulz IJ, Jobsen JJ, Lutgens LC, van der Steen-Banasik EM, Nijman HW, Putter H, Bosse T, Creutzberg CL, Smit VTHBM (2016) Improved risk assessment by integrating molecular and clinicopathological factors in early-stage endometrial cancer—combined analysis of the PORTEC cohorts. Clin Cancer Res 22(16):4215–4224. https://doi.org/10.1158/1078-0432.CCR-15-2878
Kanopienė D, Smailytė G, Vidugirienė J, Bacher J (2014) Impact of microsatellite instability on survival of endometrial cancer patients. Medicina 50(4):216–221. https://doi.org/10.1016/j.medici.2014.09.002
Hacking S, Jin C, Komforti M, Liang S, Nasim M (2019) MMR deficient undifferentiated/dedifferentiated endometrial carcinomas showing significant programmed death ligand-1 expression (sp 142) with potential therapeutic implications. Pathol Res Pract 215(10):152552. https://doi.org/10.1016/j.prp.2019.152552
Chavez JA, Wei L, Suarez AA, Parwani AV, Li Z (2019) Clinicopathologic characteristics, tumor infiltrating lymphocytes and programed cell death ligand-1 expression in 162 endometrial carcinomas with deficient mismatch repair function. Int J Gynecol Cancer 29(1):113–118. https://doi.org/10.1136/ijgc-2018-000042
Thiem A, Hesbacher S, Kneitz H, di Primio T, Heppt MV, Hermanns HM et al (2019) IFN-gamma-induced PD-L1 expression in melanoma depends on p53 expression. J Exp Clin Cancer Res 38(1):1–15
Xu C, Hua H, Chen T, Zhang W, Song G, Zhang Z (2017) PD-L1 is correlated with p53 expression in patients with lung adenocarcinoma. Int J Clin Exp Pathol 10(11)
Tojyo I, Shintani Y, Nakanishi T, Okamoto K, Hiraishi Y, Fujita S, Enaka M, Sato F, Muragaki Y (2019) PD-L1 expression correlated with p53 expression in oral squamous cell carcinoma. Maxillofac Plast Reconstr Surg 41(1):56. https://doi.org/10.1186/s40902-019-0239-8
Peng W, Chen JQ, Liu C, Malu S, Creasy C, Tetzlaff MT, Xu C, McKenzie JA, Zhang C, Liang X, Williams LJ, Deng W, Chen G, Mbofung R, Lazar AJ, Torres-Cabala CA, Cooper ZA, Chen PL, Tieu TN, Spranger S, Yu X, Bernatchez C, Forget MA, Haymaker C, Amaria R, McQuade JL, Glitza IC, Cascone T, Li HS, Kwong LN, Heffernan TP, Hu J, Bassett RL, Bosenberg MW, Woodman SE, Overwijk WW, Lizee G, Roszik J, Gajewski TF, Wargo JA, Gershenwald JE, Radvanyi L, Davies MA, Hwu P (2016) Loss of PTEN promotes resistance to T cell–mediated immunotherapy. Cancer Discov 6(2):202–216. https://doi.org/10.1158/2159-8290.CD-15-0283
Kakavand H, Jackett LA, Menzies AM, Gide TN, Carlino MS, Saw RP et al (2017) Negative immune checkpoint regulation by VISTA: a mechanism of acquired resistance to anti-PD-1 therapy in metastatic melanoma patients. Mod Pathol 30(12):1666–1676. https://doi.org/10.1038/modpathol.2017.89
Sun H, Enomoto T, Fujita M, Wada H, Yoshino K, Ozaki K, Nakamura T, Murata Y (2001) Mutational analysis of the PTEN gene in endometrial carcinoma and hyperplasia. Am J Clin Pathol 115(1):32–38. https://doi.org/10.1309/7JX6-B9U9-3P0R-EQNY
Kanamori Y, Kigawa J, Itamochi H, Shimada M, Takahashi M, Kamazawa S, Sato S, Akeshima R, Terakawa N (2001) Correlation between loss of PTEN expression and Akt phosphorylation in endometrial carcinoma. Clin Cancer Res 7(4):892–895
Quddus MR, Ologun BA, Sung CJ, Steinhoff MM, Lawrence WD (2009) Utility of PTEN expression of endometrial “surface epithelial changes” and underlying atypical endometrial hyperplasia. Int J Gynecol Pathol 28(5):471–476. https://doi.org/10.1097/PGP.0b013e3181a06f96
Song M, Chen D, Lu B, Wang C, Zhang J, Huang L, Wang X, Timmons CL, Hu J, Liu B, Wu X, Wang L, Wang J, Liu H (2013) PTEN loss increases PD-L1 protein expression and affects the correlation between PD-L1 expression and clinical parameters in colorectal cancer. PLoS One 8(6):e65821. https://doi.org/10.1371/journal.pone.0065821
Parsa AT, Waldron JS, Panner A, Crane CA, Parney IF, Barry JJ, Cachola KE, Murray JC, Tihan T, Jensen MC, Mischel PS, Stokoe D, Pieper RO (2007) Loss of tumor suppressor PTEN function increases B7-H1 expression and immunoresistance in glioma. Nat Med 13(1):84–88. https://doi.org/10.1038/nm1517
Allo G, Bernardini MQ, Wu R-C, Shih I-M, Kalloger S, Pollett A, Gilks CB, Clarke BA (2014) ARID1A loss correlates with mismatch repair deficiency and intact p53 expression in high-grade endometrial carcinomas. Mod Pathol 27(2):255–261. https://doi.org/10.1038/modpathol.2013.144
Li L, Li M, Jiang Z, Wang X (2019) ARID1A mutations are associated with increased immune activity in gastrointestinal cancer. Cells 8(7):678. https://doi.org/10.3390/cells8070678
Cancer Genome Atlas Research Network, Kandoth C, Schultz N, Cherniack AD, Akbani R, Liu Y, Shen H et al (2013) Integrated genomic characterization of endometrial carcinoma. Nature 497(7447):67–73. https://doi.org/10.1038/nature12113
Herbst RS, Soria JC, Kowanetz M, Fine GD, Hamid O, Gordon MS, Sosman JA, McDermott DF, Powderly JD, Gettinger SN, Kohrt HEK, Horn L, Lawrence DP, Rost S, Leabman M, Xiao Y, Mokatrin A, Koeppen H, Hegde PS, Mellman I, Chen DS, Hodi FS (2014) Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature 515(7528):563–567. https://doi.org/10.1038/nature14011
Funding
This study was supported by Istanbul Medeniyet University Scientific Research Project fund.
Author information
Authors and Affiliations
Contributions
G.K.: Designed the research study, contributed essential reagents or tools, performed the research, reviewed and corrected the manuscript.
T.S., Z.C.O.: Analyzed the data, wrote the paper.
A.A.: Contributed essential reagents or tools, performed the research.
W.G.M.: Reviewed and corrected the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Kir, G., Soylemez, T., Olgun, Z.C. et al. Correlation of PD-L1 expression with immunohistochemically determined molecular profile in endometrial carcinomas. Virchows Arch 477, 845–856 (2020). https://doi.org/10.1007/s00428-020-02867-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-020-02867-9