Abstract
Purpose
Surgical resection still remains the mainstay of management of hepatocellular carcinoma (HCC). At present, Barcelona clinic liver cancer (BCLC) staging is the most widely used tool to guide treatment; however, criteria for offering surgery as curative treatment are restrictive. We aimed to evaluate short-term and long-term outcomes of HCC after resection, even for patients outside BCLC criteria for resection.
Methods
Data was collected from a prospective database from GI and HPB Department, Tata Memorial Hospital, Mumbai. Study period was from June 2010 to June 2015.
Results
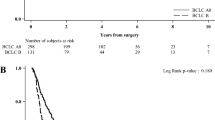
One hundred three patients of HCC were operated during this period, of which 100 underwent complete resection. Patients were staged according to the BCLC classification (BCLC stage A-25, B-64, C-11). Preoperative therapy was administered in 36 (36%) patients. At median follow-up of 21 months, overall 3-year survival for BCLC stages A, B, and C was 55.2, 62.7, and 37.5%, respectively.
Conclusion
In today’s era of liver transplantation, resection (especially for larger tumors) may still be the preferred treatment option, considering problems and difficulties in donor availability, cost, and long waiting list for liver transplant. With evolving modern surgical technique, long-term survival benefit can be achieved with acceptable safety in most BCLC stage B and selected BCLC stage C patients and those who either do not fit into the transplant criteria or cannot afford transplant. Carefully designed trials are required to further elucidate these results.


Similar content being viewed by others
References
Llovet JM, Fuster J, Bruix J (1999) Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology 30(6):1434–1440. https://doi.org/10.1002/hep.510300629
Llovet JM, Schwartz M, Mazzaferro V (2005) Resection and liver transplantation for hepatocellular carcinoma. Semin Liver Dis 25(02):181–200. https://doi.org/10.1055/s-2005-871198
Llovet JM, Brú C, Bruix J (1999) Prognosis of hepatocellular carcinoma: the BCLC staging classification. Semin Liver Dis 19(3):329–338. https://doi.org/10.1055/s-2007-1007122
European Association for the Study of the Liver (2012) European Organisation for Research and Treatment of Cancer: EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 56(4):908–943. https://doi.org/10.1016/j.jhep.2011.12.001
Ma C, Chi M, Su H, Cheng X, Chen L, Kan Y, Wei W, Huang X, Li Y, Li L, Lin K, Huang Y, Wu Y, Huang X, Huang A, Liu J (2012) Evaluation of the clinical features of HCC following hepatectomy for different stages of HCC. Hepato-Gastroenterology 59(119):2104–2111. https://doi.org/10.5754/hge12109
Bolondi L, Burroughs A, Dufour JF, Galle PR, Mazzaferro V, Piscaglia F, Raoul JL, Sangro B (2012) Heterogeneity of patients with intermediate (BCLC B) hepatocellular carcinoma: proposal for a subclassification to facilitate treatment decisions. Semin Liver Dis 32(4):348–359. https://doi.org/10.1055/s-0032-1329906
Makuuchi M, Thai BL, Takayasu K, Takayama T, Kosuge T, Gunvén P, Yamazaki S, Hasegawa H, Ozaki H (1990) Preoperative portal embolization to increase safety of major hepatectomy for hilar bile duct carcinoma: a preliminary report. Surgery 107(5):521–527
Graziadei IW, Sandmueller H, Waldenberger P, Koenigsrainer A, Nachbaur K, Jaschke W, Margreiter R, Vogel W (2003) Chemoembolization followed by liver transplantation for hepatocellular carcinoma impedes tumor progression while on the waiting list and leads to excellent outcome. Liver Transpl 9(6):557–563. https://doi.org/10.1053/jlts.2003.50106
Goel M, Gaikwad V, Dharia T, Kulkarni S, Shetty N, Shrikhande SV (2014) Preresection transarterial chemoembolization for hepatocellular carcinoma: an experience with 23 patients. Indian J Gastroenterol 33(5):432–439. https://doi.org/10.1007/s12664-014-0490-y
Majno PE, Adam R, Bismuth H, Castaing D, Ariche A, Krissat J, Perrin H, Azoulay D (1997) Influence of preoperative transarterial lipiodol chemoembolization on resection and transplantation for hepatocellular carcinoma in patients with cirrhosis. Ann Surg 226(6):688–703. https://doi.org/10.1097/00000658-199712000-00006
Yau T, Tang VY, Yao TJ, Fan ST, Lo CM, Poon RT (2014) Development of Hong Kong Liver Cancer staging system with treatment stratification for patients with hepatocellular carcinoma. Gastroenterology 146(7):1691–1700. https://doi.org/10.1053/j.gastro.2014.02.032
Frauenfelder T, Tutic M, Weder W, Gotti RP, Stahel RA, Seifert B, Opitz I (2011) Volumetry: an alternative to assess therapy response for malignant pleural mesothelioma? Eur Respir J 38(1):162–168. https://doi.org/10.1183/09031936.00146110
Shukla PJ, Pandey D, Rao PP, Shrikhande SV, Thakur MH, Arya S, Ramani S, Mehta S, Mohandas KM (2005) Impact of intra-operative ultrasonography in liver surgery. Indian J Gastroenterol 24(2):62–65
Simillis C, Li T, Vaughan J et al (2015) A Cochrane systematic review and network meta-analysis comparing treatment strategies aiming to decrease blood loss during liver resection. Int J Surg 23(Pt A):128–136
Ogata S, Belghiti J, Varma D, Sommacale D, Maeda A, Dondero F, Sauvanet A (2007) Two hundred liver hanging maneuvers for major hepatectomy: a single-center experience. Ann Surg 245(1):31–35. https://doi.org/10.1097/01.sla.0000224725.40979.0a
Liu CL, Fan ST, Lo CM, Tung-Ping Poon R, Wong J (2000) Anterior approach for major right hepatic resection for large hepatocellular carcinoma. Ann Surg 232(1):25–31. https://doi.org/10.1097/00000658-200007000-00004
Pamecha V, Gurusamy KS, Sharma D, Davidson BR (2009) Techniques for liver parenchymal transection: a meta-analysis of randomized controlled trials. HPB (Oxford) 11(4):275–281. https://doi.org/10.1111/j.1477-2574.2009.00057.x
Rahbari NN, Garden OJ, Padbury R, Brooke-Smith M, Crawford M, Adam R, Koch M, Makuuchi M, Dematteo RP, Christophi C, Banting S, Usatoff V, Nagino M, Maddern G, Hugh TJ, Vauthey JN, Greig P, Rees M, Yokoyama Y, Fan ST, Nimura Y, Figueras J, Capussotti L, Büchler MW, Weitz J (2011) Posthepatectomy liver failure: a definition and grading by the International Study Group of Liver Surgery (ISGLS). Surgery 149(5):713–724. https://doi.org/10.1016/j.surg.2010.10.001
Belghiti J, Hiramatsu K, Benoist S, Massault PP, Sauvanet A, Farges O (2000) Seven hundred forty-seven hepatectomies in the 1990s: an update to evaluate the actual risk of liver resection. J Am Coll Surg 191(1):38–46. https://doi.org/10.1016/S1072-7515(00)00261-1
Poon RT, Fan ST, Lo CM, Liu CL, Lam CM, Yuen WK, Yeung C, Wong J (2004) Improving perioperative outcome expands the role of hepatectomy in management of benign and malignant hepatobiliary diseases: analysis of 1222 consecutive patients from a prospective database. Ann Surg 240(4):698–708
Jarnagin WR, Gonen M, Fong Y, DeMatteo RP, Ben-Porat L, Little S, Corvera C, Weber S, Blumgart LH (2002) Improvement in perioperative outcome after hepatic resection: analysis of 1,803 consecutive cases over the past decade. Ann Surg 236(4):397–406. https://doi.org/10.1097/00000658-200210000-00001
Tsim NC, Frampton AE, Habib NA, Jiao LR (2010) Surgical treatment for liver cancer. World J Gastroenterol: WJG 16(8):927–933. https://doi.org/10.3748/wjg.v16.i8.927
Imamura H, Sano K, Sugawara Y, Kokudo N, Makuuchi M (2005) Assessment of hepatic reserve for indication of hepatic resection: decision tree incorporating indocyanine green test. J Hepato-Biliary-Pancreat Surg 12(1):16–22. https://doi.org/10.1007/s00534-004-0965-9
Okamoto E, Kyo A, Yamanaka N, Tanaka N, Kuwata K (1984) Prediction of the safe limits of hepatectomy by combined volumetric and functional measurements in patients with impaired hepatic function. Surgery 95(5):586–592
Turcotte JG, Lambert MJIII (1973) Variceal hemorrhage, hepatic cirrhosis, and portacaval shunts. Surgery 73(6):810–817
Poon RT, Fan ST (2005) Assessment of hepatic reserve for indication of hepatic resection: how I do it. J Hepato-Biliary-Pancreat Surg 12(1):31–37. https://doi.org/10.1007/s00534-004-0945-0
Cucchetti A, Ercolani G, Vivarelli M, Cescon M, Ravaioli M, Ramacciato G, Grazi GL, Pinna AD (2009) Is portal hypertension a contraindication tohepatic resection? Ann Surg 250(6):922–928. https://doi.org/10.1097/SLA.0b013e3181b977a5
Ishizawa T, Hasegawa K, Aoki T, Takahashi M, Inoue Y, Sano K, Imamura H, Sugawara Y, Kokudo N, Makuuchi M (2008) Neither multiple tumors nor portal hypertension are surgical contraindications for hepatocellular carcinoma. Gastroenterology 134(7):1908–1916. https://doi.org/10.1053/j.gastro.2008.02.091
Berzigotti A, Reig M, Abraldes JG, Bosch J, Bruix J (2015) Portal hypertension and the outcome of surgery for hepatocellular carcinoma in compensated cirrhosis: a systematic review and meta-analysis. Hepatology 61(2):526–536. https://doi.org/10.1002/hep.27431
Torzilli G, Belghiti J, Kokudo N, Takayama T, Capussotti L, Nuzzo G, Vauthey JN, Choti MA, de Santibanes E, Donadon M, Morenghi E, Makuuchi M (2013) A snapshot of the effective indications and results of surgery for hepatocellular carcinoma in tertiary referral centers: is it adherent to the EASL/AASLD recommendations? An observational study of the HCC East-West Study Group. Ann Surg 257(5):929–937. https://doi.org/10.1097/SLA.0b013e31828329b8
Zhong JH, Ke Y, Gong WF et al (2014) Hepatic resection associated with good survival for selected patients with intermediate and advanced-stage hepatocellular carcinoma. Ann Surg 260(2):329–340. https://doi.org/10.1097/SLA.0000000000000236
Ciria R, López-Cillero P, Gallardo AB, Cabrera J, Pleguezuelo M, Ayllón MD, Luque A, Zurera L, Espejo JJ, Rodríguez-Perálvarez M, Montero JL, de la Mata M, Briceño J (2015) Optimizing the management of patients with BCLC stage-B hepatocellular carcinoma: modern surgical resection as a feasible alternative to transarterial chemoemolization. Eur J Surg Oncol 41(9):1153–1161. https://doi.org/10.1016/j.ejso.2015.05.023
Wang JH, Changchien CS, TH H et al (2008) The efficacy of treatment schedules according to Barcelona clinic liver cancer staging for hepatocellular carcinoma: survival analysis of 3892 patients. Eur J Cancer 44(7):1000–1006. https://doi.org/10.1016/j.ejca.2008.02.018
Ho MC, Huang GT, Tsang YM, Lee PH, Chen DS, Sheu JC, Chen CH (2009) Liver resection improves the survival of patients with multiple hepatocellular carcinomas. Ann Surg Oncol 16(4):848–855. https://doi.org/10.1245/s10434-008-0282-7
Hsu CY, Hsia CY, Huang YH, Su CW, Lin HC, Pai JT, Loong CC, Chiou YY, Lee RC, Lee FY, Huo TI, Lee SD (2012) Comparison of surgical resection and transarterial chemoembolization for hepatocellular carcinoma beyond the Milan criteria: a propensity score analysis. Ann Surg Oncol 19(3):842–849. https://doi.org/10.1245/s10434-011-2060-1
Yokoo H, Kamiyama T, Kakisaka T, Orimo T, Wakayama K, Shimada S, Tsuruga Y, Kamachi H, Taketomi A (2015) Efficacy of sorafenib for extrahepatic recurrence of hepatocellular carcinoma after liver resection. Gan To Kagaku Ryoho 42(12):1497–1499
Marelli L, Stigliano R, Triantos C, Senzolo M, Cholongitas E, Davies N, Tibballs J, Meyer T, Patch DW, Burroughs AK (2007) Transarterial therapy for hepatocellular carcinoma: which technique is more effective? A systematic review of cohort and randomized studies. Cardiovasc Intervent Radiol 30(1):6–25. https://doi.org/10.1007/s00270-006-0062-3
Kaibori M, Tanigawa N, Matsui Y, Saito T, Uchida Y, Ishizaki M, Tanaka H, Kamiyama Y (2006) Influence of transcatheter arterial chemoembolization on the prognosis after hepatectomy for hepatocellular carcinoma in patients with severe liver dysfunction. Anticancer Res 26(5B):3685–3692
Ochiai T, Sonoyama T, Hironaka T, Yamagishi H (2003) Hepatectomy with chemoembolization for treatment of hepatocellular carcinoma. Hepato-Gastroenterology 50(51):750–755
CD L, Peng SY, Jiang XC et al (1999) Preoperative transcatheter arterial chemoembolization and prognosis of patients with hepatocellular carcinomas: retrospective analysis of 120 cases. World J Surg 23:293–300
Gerunda GE, Neri D, Merenda R, Barbazza F, Zangrandi F, Meduri F, Bisello M, Valmasoni M, Gangemi A, Faccioli AM (2000) Role of transarterial chemoembolization before liver resection for hepatocarcinoma. Liver Transpl 6(5):619–626. https://doi.org/10.1053/jlts.2000.8312
Jarnagin WR, Gonen M, Fong Y, DeMatteo RP, Ben-Porat L, Little S, Corvera C, Weber S, Blumgart LH (2002) Improvement in perioperative outcome after hepatic resection: analysis of 1,803 consecutive cases over the past decade. Ann Surg 236(4):397–406. https://doi.org/10.1097/00000658-200210000-00001
Acknowledgements
The authors would like to thank Department of Gastro-intestinal Surgery and Surgical Oncology, Department of Intervention Radiology, Tata Memorial Hospital, Mumbai, India.
Author information
Authors and Affiliations
Contributions
Authorship Manish S. Bhandare participated in study conception and design, acquisition of data, analysis and interpretation of data, and drafting of manuscript; Shraddha Patkar participated in study conception and design and acquisition of data; Nitin Shetty, Ashwin Polnaya, and Suyash Kulkarni participated in acquisition of data; Rohit R. Dusane participated in analysis of data; Shailesh V. Shrikhande participated in critical revision of manuscript; and Mahesh Goel participated in study conception and design, drafting of manuscript, and critical revision of manuscript.
Corresponding author
Ethics declarations
The data of the present study were collected in the course of common clinical practice, and accordingly, the signed informed consent was obtained from each patient for any surgical and clinical procedure. The study protocol was in accordance with the ethical standards of the institutional research committee and the 1964 Helsinki Declaration and its later amendments. Since this was a retrospective study, formal consent for this study is not required and no approval of the institutional research committee was needed.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Bhandare, M.S., Patkar, S., Shetty, N. et al. Liver resection for HCC outside the BCLC criteria. Langenbecks Arch Surg 403, 37–44 (2018). https://doi.org/10.1007/s00423-017-1640-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-017-1640-3