Abstract
Purpose
Heart rate variability (HRV) may be influenced by several factors, such as environment (hypoxia, hyperoxia, hypercapnia) or physiological demand (exercise). In this retrospective study, we tested the hypothesis that inter-beat (RR) intervals in healthy subjects exercising under various environmental stresses exhibit oscillations at the same frequency than ventilatory oscillations.
Methods
Spectra from RR intervals and ventilation (\(\dot{V}\)E) were collected from 37 healthy young male subjects who participated in 5 previous studies focused on ventilatory oscillations (or periodic breathing) during exercise in hypoxia, hyperoxia and hypercapnia. Bland and Altman test and multivariate regressions were then performed to compare respective frequencies and changes in peak powers of the two signals.
Results
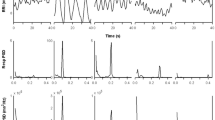
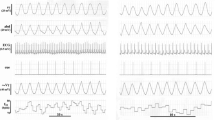
Fast Fourier analysis of RR and \(\dot{V}\)E signals showed that RR was oscillating at the same frequency than periodic breathing, i.e., ~ 0.09 Hz (11 s). During exercise, in these various conditions, the difference between minimum and maximum HRV peak power was positively correlated to the same change in ventilation peak power (P < 0.05). Low-frequency (LF) peak power was correlated to tidal volume (P < 0.01) and breathing frequency (P < 0.001).
Conclusions
This study suggests that low-frequency ventilatory oscillations in hypoxia are a major contributor to the LF band power of heart rate variability.
Clinical Trial Reg. no.
NCT02201875.




Similar content being viewed by others
Abbreviations
- ACZ:
-
Acetazolamide
- ANOVA:
-
Analysis of variance
- CHF:
-
Chronic heart failure
- FFT:
-
Fast Fourier transform
- HF:
-
High frequency
- HR:
-
Heart rate
- HRV:
-
Heart rate variability
- LF:
-
Low frequency
- LOA:
-
Limits of agreement
- MAP:
-
Maximal aerobic power
- PB:
-
Periodic breathing
- RR:
-
Interbeat interval
- SD:
-
Standard deviation
- Ti:
-
Inspiratory time
- Ttot:
-
Total respiratory cycle time
- \(\dot{V}E\) :
-
Ventilation
- VLF:
-
Very low frequency
- VT:
-
Tidal volume
References
Ainslie PN, Lucas SJE, Burgess KR (2013) Breathing and sleep at high altitude. Respir Physiol Neurobiol 188:233–256. https://doi.org/10.1016/j.resp.2013.05.020
Akselrod S, Gordon D, Ubel FA et al (1981) Power spectrum analysis of heart rate fluctuation: a quantitative probe of beat-to-beat cardiovascular control. Science 213:220–222
Aysin B, Aysin E (2006) Effect of respiration in heart rate variability (HRV) analysis. In: 2006 international conference of the IEEE Engineering in Medicine and Biology Society. IEEE, New York, NY, pp 1776–1779
Beda A, Simpson DM, Carvalho NC, Carvalho ARS (2014) Low-frequency heart rate variability is related to the breath-to-breath variability in the respiratory pattern. Psychophysiology 51:197–205. https://doi.org/10.1111/psyp.12163
Berntson GG, Cacioppo JT, Quigley KS (1993) Respiratory sinus arrhythmia: autonomic origins, physiological mechanisms, and psychophysiological implications. Psychophysiology 30:183–196
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Brack T, Randerath W, Bloch KE (2012) Cheyne–Stokes respiration in patients with heart failure: prevalence, causes, consequences and treatments. Respiration 83:165–176. https://doi.org/10.1159/000331457
Brown SJ, Howden R (2008) The effects of a respiratory acidosis on human heart rate variability. Adv Exp Med Biol 605:361–365. https://doi.org/10.1007/978-0-387-73693-8_63
Brown SJ, Barnes MJ, Mündel T (2014) Effects of hypoxia and hypercapnia on human HRV and respiratory sinus arrhythmia. Acta Physiol Hung 101:263–272. https://doi.org/10.1556/APhysiol.101.2014.3.1
American College of Sports Medicine, Riebe D, Ehrman JK, et al (eds) (2018) ACSM’s guidelines for exercise testing and prescription, Tenth edition. Wolters Kluwer, Philadelphia
Corrà U, Giordano A, Bosimini E et al (2002) Oscillatory ventilation during exercise in patients with chronic heart failure: clinical correlates and prognostic implications. Chest 121:1572–1580
De Burgh Daly M (2011) Interactions between respiration and circulation. In: Terjung R (ed) Comprehensive physiology. Wiley, Hoboken, NJ. https://doi.org/10.1002/cphy.cp030216
Daoud M, Ravier P, Buttelli O (2018) Use of cardiorespiratory coherence to separate spectral bands of the heart rate variability. Biomed Signal Process Control 46:260–267. https://doi.org/10.1016/j.bspc.2018.08.003
Duffin J (2011) Measuring the respiratory chemoreflexes in humans. Respir Physiol Neurobiol 177:71–79. https://doi.org/10.1016/j.resp.2011.04.009
Electrophysiology Task Force of the European Society of Cardiology the North American Society of Pacing (1996) Heart rate variability. Circulation 93:1043–1065. https://doi.org/10.1161/01.CIR.93.5.1043
Estévez M, Machado C, Leisman G et al (2015) Spectral analysis of heart rate variability. Int J Disability Hum Dev 15:5–17. https://doi.org/10.1515/ijdhd-2014-0025
Florea VG, Cohn JN (2014) The autonomic nervous system and heart failure. Circ Res 114:1815–1826. https://doi.org/10.1161/CIRCRESAHA.114.302589
Garde A, Giraldo BF, Jané R, Sörnmo L (2009) Time-varying respiratory pattern characterization in chronic heart failure patients and healthy subjects. Conf Proc IEEE Eng Med Biol Soc 2009:4007–4010. https://doi.org/10.1109/IEMBS.2009.5333501
Garde A, Giraldo BF, Jane R et al (2012) Periodic breathing during ascent to extreme altitude quantified by spectral analysis of the respiratory volume signal. Conf Proc IEEE Eng Med Biol Soc 2012:707–710. https://doi.org/10.1109/EMBC.2012.6346029
Gauda EB, Martin RJ (2012) Control of breathing. In: Avery's diseases of the newborn, 9th edn. Elsevier Inc., pp 584–597. https://doi.org/10.1016/B978-1-4377-0134-0.10043-5
Guzzetti S, Magatelli R, Borroni E, Mezzetti S (2001) Heart rate variability in chronic heart failure. Auton Neurosci 90:102–105. https://doi.org/10.1016/S1566-0702(01)00274-0
Hermand E, Lhuissier FJ, Larribaut J, et al. (2015a) Ventilatory oscillations at exercise: effects of hyperoxia, hypercapnia, and acetazolamide. Physiol Rep 3: doi: 10.14814/phy2.12446.
Hermand E, Pichon A, Lhuissier FJ, Richalet J-P (2015b) Periodic breathing in healthy humans at exercise in hypoxia. J Appl Physiol 118:115–123. https://doi.org/10.1152/japplphysiol.00832.2014
Hermand E, Lhuissier FJ, Voituron N, Richalet J-P (2016) Ventilatory oscillations at exercise in hypoxia: a mathematical model. J Theor Biol 411:92–101. https://doi.org/10.1016/j.jtbi.2016.10.002
Hermand E, Lhuissier FJ, Richalet J-P (2017) Effect of dead space on breathing stability at exercise in hypoxia. Respir Physiol Neurobiol 246:26–32. https://doi.org/10.1016/j.resp.2017.07.008
Hernandez AB, Patil SP (2016) Pathophysiology of central sleep apneas. Sleep Breath 20:467–482. https://doi.org/10.1007/s11325-015-1290-z
Hung P-H, Lin F-C, Tsai H-C et al (2019) The usefulness of prophylactic use of acetazolamide in subjects with acute mountain sickness. J Chin Med Assoc 82:126–132. https://doi.org/10.1097/JCMA.0000000000000014
Insalaco G, Salvaggio A, Pomidori L et al (2016) Heart rate variability during sleep at high altitude: effect of periodic breathing. Sleep Breath 20:197–204. https://doi.org/10.1007/s11325-015-1205-z
Latshang TD, Turk AJ, Hess T et al (2013) Acclimatization improves submaximal exercise economy at 5533 m. Scand J Med Sci Sports 23:458–467. https://doi.org/10.1111/j.1600-0838.2011.01403.x
Leung RS, Bradley TD (2001) Sleep apnea and cardiovascular disease. Am J Respir Crit Care Med 164:2147–2165. https://doi.org/10.1164/ajrccm.164.12.2107045
Leung RST, Floras JS, Lorenzi-Filho G et al (2003) Influence of Cheyne–Stokes respiration on cardiovascular oscillations in heart failure. Am J Respir Crit Care Med 167:1534–1539. https://doi.org/10.1164/rccm.200208-793OC
Liu XX, Lu LL, Zhong CF et al (2001) Analysis of heart rate variability during acute exposure to hypoxia. Space Med Med Eng (Beijing) 14:328–331
McCraty R, Shaffer F (2015) Heart rate variability: new perspectives on physiological mechanisms, assessment of self-regulatory capacity, and health risk. Glob Adv Health Med 4:46–61. https://doi.org/10.7453/gahmj.2014.073
Oliveira ALMB, Rohan P de A, Gonçalves TR, Soares PP da S (2017) Effects of hypoxia on heart rate variability in healthy individuals: a systematic review. International Journal of Cardiovascular Sciences. doi: 10.5935/2359-4802.20170035.
Olson TP, Johnson BD (2014) Quantifying oscillatory ventilation during exercise in patients with heart failure. Respir Physiol Neurobiol 190:25–32. https://doi.org/10.1016/j.resp.2013.09.008
Pinna GD, Maestri R, Di Cesare A et al (1995) Very low frequency oscillations of heart period: relationship to respiratory activity and blood pressure in heart failure patients. IEEE Comput Soc Press, pp 553–556
Pinna GD, Maestri R, Rovere MT, Mortara A (1996) An oscillation of the respiratory control system accounts for most of the heart period variability of chronic heart failure patients. Clin Sci 91(Suppl):89–91
Pomeranz B, Macaulay RJ, Caudill MA et al (1985) Assessment of autonomic function in humans by heart rate spectral analysis. Am J Physiol Heart Circ Physiol 248:H151–H153. https://doi.org/10.1152/ajpheart.1985.248.1.H151
Ponikowski P, Chua TP, Piepoli M et al (1998) Ventilatory response to exercise correlates with impaired heart rate variability in patients with chronic congestive heart failure. Am J Cardiol 82:338–344. https://doi.org/10.1016/S0002-9149(98)00303-8
Povea C, Schmitt L, Brugniaux J et al (2005) Effects of intermittent hypoxia on heart rate variability during rest and exercise. High Alt Med Biol 6:215–225. https://doi.org/10.1089/ham.2005.6.215
Pöyhönen M, Syväoja S, Hartikainen J et al (2004) The effect of carbon dioxide, respiratory rate and tidal volume on human heart rate variability. Acta Anaesthesiol Scand 48:93–101. https://doi.org/10.1111/j.1399-6576.2004.00272.x
Richalet J-P, Rivera M, Bouchet P et al (2005) Acetazolamide: a treatment for chronic mountain sickness. Am J Respir Crit Care Med 172:1427–1433. https://doi.org/10.1164/rccm.200505-807OC
Sarmiento S, García-Manso JM, Martín-González JM et al (2013) Heart rate variability during high-intensity exercise. J Syst Sci Complex 26:104–116. https://doi.org/10.1007/s11424-013-2287-y
Saul JP, Arai Y, Berger RD et al (1988) Assessment of autonomic regulation in chronic congestive heart failure by heart rate spectral analysis. Am J Cardiol 61:1292–1299
Siebenmann C, Ryrsø CK, Oberholzer L et al (2018) Hypoxia-induced vagal withdrawal is independent of the hypoxic ventilatory response in men. J Appl Physiol 126:124–131. https://doi.org/10.1152/japplphysiol.00701.2018
Tarvainen MP, Niskanen J-P, Lipponen JA et al (2014) Kubios HRV—heart rate variability analysis software. Comput Methods Programs Biomed 113:210–220. https://doi.org/10.1016/j.cmpb.2013.07.024
Tulppo MP, Mäkikallio TH, Takala TE et al (1996) Quantitative beat-to-beat analysis of heart rate dynamics during exercise. Am J Physiol 271:H244–252
Xu X-Q, Jing Z-C (2009) High-altitude pulmonary hypertension. Eur Respir Rev 18:13–17. https://doi.org/10.1183/09059180.00011104
Zhang D, She J, Zhang Z, Yu M (2014) Effects of acute hypoxia on heart rate variability, sample entropy and cardiorespiratory phase synchronization. BioMed Eng OnLine 13:73. https://doi.org/10.1186/1475-925X-13-73
Author information
Authors and Affiliations
Contributions
EH, AP and JPR conceived and designed research. EH, JPR and FL conducted experiments. EH analyzed data. EH wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Additional information
Communicated by Keith Phillip George.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hermand, E., Pichon, A., Lhuissier, F.J. et al. Low-frequency ventilatory oscillations in hypoxia are a major contributor to the low-frequency component of heart rate variability. Eur J Appl Physiol 119, 1769–1777 (2019). https://doi.org/10.1007/s00421-019-04166-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-019-04166-x