Abstract
Purpose
Despite advances in glaucoma treatment options, patient adherence and compliance remain very low. The EyePhone© App is a free non-commercial reminder application designed specifically for the needs of glaucoma patients. In this study, we evaluated its usefulness in improving adherence to medical treatment among glaucoma patients.
Methods
This is a prospective multicenter interventional study. Glaucoma patients were recruited from a tertiary center and a large community glaucoma service center. After a short explanation, the EyePhone© App was installed on their smartphone device, and the notifications for the current medical treatment were entered. After enrollment and at 1-month follow-up, subjects completed the Morisky Medication Adherence Scale (MMAS-8) and the Quality of Life and Glaucoma 17-item (GlauQOL-17) questionnaires for evaluation of adherence and QOL, respectively.
Results
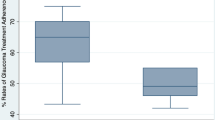
In the study, 133 patients (71 men and 62 women) aged 62±15.5 years and using 2.0±0.9 IOP-lowering drugs participated. The proportion of highly adherent subjects improved from 29.3% (39/133) at baseline to 42.1% (56/133) at follow-up (P < 0.001), and the proportion of poorly adherent subjects decreased from 29.3 (39/133) to 20.3% (27/133) at follow-up (P = 0.012). QOL also improved, as evidenced by a significant increase in the GlauQOL-17 score (P < 0.05). In a subgroup of patients for whom IOP measurements were available, IOP reduced by 0.92 mmHg (P = 0.069).
Conclusions
Significant improvements in glaucoma adherence and QOL were achieved among poorly adherent glaucoma patients after 1 month of using the EyePhone© App.





Similar content being viewed by others
Data availability
Upon request.
Code availability
The EyePhone® App is available for download without charge from the Google Play app store: https://play.google.com/store/apps/details?id=com.glaoucmaskaatleshno.drugreminder2
References
Quigley HA (1996) The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 80:389–393. https://doi.org/10.1136/bjo.80.5.389
Tham Y-C, Li X, Wong TY et al (2014) Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology 121:2081–2090. https://doi.org/10.1016/j.ophtha.2014.05.013
Blumberg D, Skaat A, Liebmann JM (2015) Emerging risk factors for glaucoma onset and progression. Prog Brain Res 221:81–101. https://doi.org/10.1016/bs.pbr.2015.04.007
Newman-Casey PA, Salman M, Lee PP, Gatwood JD (2020) Cost-utility analysis of glaucoma medication adherence. Ophthalmology 127:589–598. https://doi.org/10.1016/j.ophtha.2019.09.041
Schwartz GF, Quigley HA (2008) Adherence and persistence with glaucoma therapy. Surv Ophthalmol 53. https://doi.org/10.1016/j.survophthal.2008.08.002
Mansberger SL (2010) Are you compliant with addressing glaucoma adherence? Am J Ophthalmol 149:1–3. https://doi.org/10.1016/j.ajo.2009.08.011
Blaschke TF, Osterberg L, Vrijens B, Urquhart J (2012) Adherence to medications: Insights arising from studies on the unreliable link between prescribed and actual drug dosing histories. Annu Rev Pharmacol Toxicol 52:275–301
Olthoff CMGG, Schouten JSAGAG, Van De Borne BW, Webers CABB (2005) Noncompliance with ocular hypotensive treatment in patients with glaucoma or ocular hypertension: an evidence-based review. Ophthalmology 112:953–961.e7. https://doi.org/10.1016/j.ophtha.2004.12.035
Reardon G, Kotak S, Schwartz GF (2011) Objective assessment of compliance and persistence among patients treated for glaucoma and ocular hypertension: a systematic review. Patient Prefer Adherence 5:441–463. https://doi.org/10.2147/PPA.S23780
Leske MC, Heijl A, Hussein M et al (2003) Factors for glaucoma progression and the effect of treatment: the early manifest glaucoma trial. Arch Ophthalmol 121:48–56. https://doi.org/10.1001/archopht.121.1.48
Stewart WC, Chorak RP, Hunt HH, Sethuraman G (1993) Factors associated with visual loss in patients with advanced glaucomatous changes in the optic nerve head. Am J Ophthalmol 116:176–181. https://doi.org/10.1016/S0002-9394(14)71282-6
Rossi GCM, Pasinetti GM, Scudeller L et al (2011) Do adherence rates and glaucomatous visual field progression correlate? Eur J Ophthalmol 21:410–414. https://doi.org/10.5301/EJO.2010.6112
Sleath B, Blalock S, Covert D et al (2011) The relationship between glaucoma medication adherence, eye drop technique, and visual field defect severity. Ophthalmology 118:2398–2402. https://doi.org/10.1016/j.ophtha.2011.05.013
Paula JS, Furtado JM, Santos AS et al (2012) Risk factors for blindness in patients with open-angle glaucoma followed-up for at least 15 years. Arq Bras Oftalmol 75:243–246. https://doi.org/10.1590/S0004-27492012000400004
Newman-Casey PA, Niziol LM, Gillespie BW et al (2020) The association between medication adherence and visual field progression in the collaborative initial glaucoma treatment study. Ophthalmology 127:477–483. https://doi.org/10.1016/j.ophtha.2019.10.022
Newman-Casey PA, Robin AL, Blachley T et al (2015) The most common barriers to glaucoma medication adherence: a cross-sectional survey. Ophthalmology 122:1308–1316. https://doi.org/10.1016/j.ophtha.2015.03.026
Huang Z, Tan E, Lum E et al (2019) A smartphone app to improve medication adherence in patients with type 2 diabetes in Asia: feasibility randomized controlled trial. J Med Internet Res 21. https://doi.org/10.2196/14914
Santo K, Singleton A, Rogers K et al (2019) Medication reminder applications to improve adherence in coronary heart disease: a randomised clinical trial. Heart 105:323–329. https://doi.org/10.1136/heartjnl-2018-313479
Mehari T, Giorgis AT, Shibeshi W (2016) Level of adherence to ocular hypotensive agents and its determinant factors among glaucoma patients in Menelik II Referral Hospital, Ethiopia. BMC Ophthalmol 16. https://doi.org/10.1186/s12886-016-0316-z
Killeen OJ, Mackenzie C, Heisler M et al (2016) User-centered design of the eyeGuide: a tailored glaucoma behavior change program. J Glaucoma 25:815–821. https://doi.org/10.1097/IJG.0000000000000431
Lee TH, Sung MS, Heo H, Park SW (2018) Association between meibomian gland dysfunction and compliance of topical prostaglandin analogs in patients with normal tension glaucoma. PLoS One 13. https://doi.org/10.1371/journal.pone.0191398
Zanlonghi X, Arnould B, Bechetoille A et al (2003) Glaucoma and quality of life. J Fr Ophtalmol 26. https://doi.org/10.1097/icu.0000000000000455
Béchetoille A, Arnould B, Bron A et al (2008) Measurement of health-related quality of life with glaucoma: validation of the Glau-QoL © 36-item questionnaire. Acta Ophthalmol 86:71–80. https://doi.org/10.1111/j.1600-0420.2007.00999.x
Skaat A, Chetrit A, Belkin M et al (2012) Time trends in the incidence and causes of blindness in Israel. Am J Ophthalmol 153:214–221.e1. https://doi.org/10.1016/j.ajo.2011.08.035
Guerin MB, Flynn TH, Brady J, O’Brien CJ (2009) Worldwide geographical distribution of ophthalmology publications. Int Ophthalmol 29:511–516. https://doi.org/10.1007/s10792-008-9278-3
Patel SC, Spaeth GL (1995) Compliance in patients prescribed eyedrops for glaucoma. Ophthalmic Surg 26:233–236
Taylor SA, Galbraith SM, Mills RP (2002) Causes of non-compliance with drug regimens in glaucoma patients: a qualitative study. J Ocul Pharmacol Ther 18:401–409. https://doi.org/10.1089/10807680260362687
Waterman H, Evans JR, Gray TA et al (2013) Interventions for improving adherence to ocular hypotensive therapy. Cochrane Database Syst Rev 2013. https://doi.org/10.1002/14651858.CD006132.pub3
Waisbourd M, Dhami H, Zhou C et al (2016) The Wills eye glaucoma app: Interest of patients and their caregivers in a smartphone-based and tablet-based glaucoma application. J Glaucoma 25:e787–e791. https://doi.org/10.1097/IJG.0000000000000504
Pastor S, Harbin T (2013) Improving compliance with eye drop medications. Mo Med 110:52
Hermann MM, Papaconstantinou D, Muether PS et al (2011) Adherence with brimonidine in patients with glaucoma aware and not aware of electronic monitoring. Acta Ophthalmol 89. https://doi.org/10.1111/j.1755-3768.2010.02050.x
Hermann MM, Bron AM, Creuzot-Garcher CP, Diestelhorst M (2011) Measurement of adherence to brimonidine therapy for glaucoma using electronic monitoring. J Glaucoma 20:502–508. https://doi.org/10.1097/IJG.0b013e3181f3eb4a
Gray TA, Fenerty C, Harper R et al (2012) Individualised patient care as an adjunct to standard care for promoting adherence to ocular hypotensive therapy: an exploratory randomised controlled trial. Eye 26:407–417. https://doi.org/10.1038/eye.2011.269
Glanz K, Beck AD, Bundy L et al (2012) Impact of a health communication intervention to improve glaucoma treatment adherence: results of the interactive study to increase glaucoma adherence to treatment trial. Arch Ophthalmol 130:1252–1258. https://doi.org/10.1001/archophthalmol.2012.1607
Sakai H, Shinjyo S, Nakamura Y et al (2005) Comparison of latanoprost monotherapy and combined therapy of 0.5% timolol and 1% dorzolamide in chronic primary angle-closure glaucoma (CACG) in Japanese patients. J Ocul Pharmacol Ther 21:483–489. https://doi.org/10.1089/jop.2005.21.483
Laibovitz R, Boyle J, Snyder E et al (1996) Dorzolamide versus pilocarpine as adjunctive therapies to timolol: a comparison of patient preference and impact on daily life. Clin Ther 18:821–832. https://doi.org/10.1016/S0149-2918(96)80042-7
Schenker H, Maloney S, Liss C et al (1999) Patient preference, efficacy, and compliance with timolol maleate ophthalmic gel-forming solution versus timolol maleate ophthalmic solution in patients with ocular hypertension or open-angle glaucoma. Clin Ther 21:138–147. https://doi.org/10.1016/S0149-2918(00)88274-0
Sverrisson T, Gross R, Pearson J et al (1999) The dorzolamide/timolol combination versus timolol plus pilocarpine: patient preference and impact on daily life. J Glaucoma 8:315–324. https://doi.org/10.1097/00061198-199910000-00008
Barber BL, Strahlman ER, Laibovitz R et al (1997) Validation of a questionnaire for comparing the tolerability of ophthalmic medications. Ophthalmology 104:334–342. https://doi.org/10.1016/S0161-6420(97)30314-5
Svendsen MT, Andersen F, Andersen KH et al (2018) A smartphone application supporting patients with psoriasis improves adherence to topical treatment: a randomized controlled trial. Br J Dermatol 179:1062–1071. https://doi.org/10.1111/bjd.16667
Saeedi OJ, Luzuriaga C, Ellish N, Robin A (2015) Potential limitations of e-mail and text messaging in improving adherence in glaucoma and ocular hypertension. J Glaucoma 24:e95–e102. https://doi.org/10.1097/IJG.0000000000000150
Robin AL, Novack GD, Covert DW et al (2007) Adherence in glaucoma: objective measurements of once-daily and adjunctive medication use. Am J Ophthalmol 144. https://doi.org/10.1016/j.ajo.2007.06.012
Stone JL, Robin AL, Novack GD et al (2009) An objective evaluation of eyedrop instillation in patients with glaucoma. Arch Ophthalmol 127:732–736. https://doi.org/10.1001/archophthalmol.2009.96
Vrijens B, Urquhart J (2014) Methods for measuring, enhancing, and accounting for medication adherence in clinical trials. Clin Pharmacol Ther 95:617–626. https://doi.org/10.1038/clpt.2014.59
Covert D, Robin AL, Novack GD (2005) Systemic medications and glaucoma patients. Ophthalmology 112:1849.e1–1849.e2. https://doi.org/10.1016/j.ophtha.2005.07.016
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The study was approved by both the Sheba Medical Center and the “Clalit” healthcare services institutional review boards.
Consent to participate
All participants signed an informed consent form
Conflict of interest
Two of the authors (AL and AS) developed the EyePhone® App. The other authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Leshno, A., Gaton, D., Singer, R. et al. A novel EyePhone© App for improving adherence to glaucoma therapy. Graefes Arch Clin Exp Ophthalmol 259, 1253–1262 (2021). https://doi.org/10.1007/s00417-021-05091-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-021-05091-6