Abstract
Purpose
To describe the characteristics of de novo uveitis in patients ≥ 60 years old.
Methods
Retrospective review of patients with uveitis followed in our tertiary center over a 14-year period. Patients aged 60–70 years and patients aged > 70 years were compared.
Results
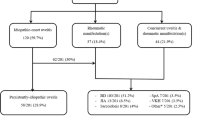
A total of 283/1044 (27.1%) patients with uveitis were ≥ 60 years of age. Idiopathic uveitis (36.1%) and sarcoidosis (31.5%) were the most frequent etiologies. Sarcoidosis was significantly more frequent (31.5% vs. 13.7%, p < 0.0001) after the age of 60 years. Intraocular lymphoma (5.0% vs. 1.1%) and herpes virus infection (5.0% vs. 0.9%) were also more common in this age group, unlike HLA B27-related uveitis and spondyloarthritis (4.6% vs. 14.9%). Pure ophthalmologic entities: birdshot retinochoroidopathy (2.8%) or Fuchs uveitis (0.4%), were rare in patients ≥ 60 years of age and Posner Scholssman, Pars planitis, White dots syndrome, Behçet’s disease, and Multiple Sclerosis were never reported. In patients > 70 years old, idiopathic uveitis (41.1% vs. 31.7%) and presumed sarcoidosis (56.5% vs. 25.6%) were more frequent than in the 60–70-year age group.
Conclusion
In our center, sarcoidosis is the leading cause of non-idiopathic uveitis in older patients. Idiopathic uveitis and other entities account for less than two-thirds of cases. Ophthalmologic entities are rare after 60 years of age. We also report for the first time the characteristics of uveitis after 70 years of age.
Similar content being viewed by others
References
Sève P, Cacoub P, Bodaghi B, Trad S, Sellam J, Bellocq D et al (2017) Uveitis: diagnostic work-up. A literature review and recommendations from an expert committee. Autoimmun Rev 16(12):1254–1264
Gritz DC, Wong IG (2004) Incidence and prevalence of uveitis in Northern California; the Northern California Epidemiology of Uveitis Study. Ophthalmology. 111(3):491–500 discussion 500
Rim TH, Kim SS, Ham D-I, Yu S-Y, Chung EJ, Lee SC et al (2018) Incidence and prevalence of uveitis in South Korea: a nationwide cohort study. Br J Ophthalmol 102(1):79–83
Grégoire M-A, Kodjikian L, Varron L, Grange J-D, Broussolle C, Seve P (2011) Characteristics of uveitis presenting for the first time in the elderly: analysis of 91 patients in a tertiary center. Ocul Immunol Inflamm 19(4):219–226
Chatzistefanou K, Markomichelakis NN, Christen W, Soheilian M, Foster CS (1998) Characteristics of uveitis presenting for the first time in the elderly. Ophthalmology. 105(2):347–352
Bouillet L, Sarrot Reynauld F, Gonzalvez B, Mouillon M, Romanet JP, Massot C (2000) Uveitis after the age of 60. Rev Med Interne 21(12):1131–1132
Kirsch O, Lautier-Frau M, Labetoulle M, Offret H, Frau E (2003) Characteristics of uveitis presenting de novo in the elderly. J Fr Ophtalmol 26(7):720–724
Barton K, Pavesio CE, Towler HM, Lightman S (1994) Uveitis presenting de novo in the elderly. Eye (Lond) 8 ( Pt 3:288–291
Favre C, Tran VT, Herbort CP (1994) Uveitis in the elderly. Klin Monatsbl Augenheilkd 204(5):319–322
Makley TA, Orlando RG (1982) Uveitis in older patients. Ann Ophthalmol 14(10):942–944
Bloch-Michel E, Nussenblatt RB (1987) International Uveitis Study Group recommendations for the evaluation of intraocular inflammatory disease. Am J Ophthalmol 103(2):234–235
de Parisot A, Kodjikian L, Errera M-H, Sedira N, Heron E, Pérard L et al (2017) Randomized controlled trial evaluating a standardized strategy for uveitis etiologic diagnosis (ULISSE). Am J Ophthalmol
Bodaghi B, Wechsler B, Du-Boutin LTH, Cassoux N, LeHoang P, Piette J-C (2003) Chronic severe uveitis: classification, search for etiology and therapeutic approach. Rev Med Interne 24(12):794–802
Gupta V, Gupta A, Rao NA (2007) Intraocular tuberculosis--an update. Surv Ophthalmol 52(6):561–587
Dougados M, van der Linden S, Juhlin R, Huitfeldt B, Amor B, Calin A et al (1991) The European Spondylarthropathy Study Group preliminary criteria for the classification of spondylarthropathy. Arthritis Rheum 34(10):1218–1227
Rudwaleit M, van der Heijde D, Landewé R, Listing J, Akkoc N, Brandt J et al (2009) The development of Assessment of SpondyloArthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis 68(6):777–783
Rudwaleit M, van der Heijde D, Landewé R, Akkoc N, Brandt J, Chou CT et al (2011) The Assessment of SpondyloArthritis International Society classification criteria for peripheral spondyloarthritis and for spondyloarthritis in general. Ann Rheum Dis 70(1):25–31
International Study Group for Behçet’s Disease (1990) Criteria for diagnosis of Behçet’s disease. Lancet. 335(8697):1078–1080
Read RW, Holland GN, Rao NA, Tabbara KF, Ohno S, Arellanes-Garcia L et al (2001) Revised diagnostic criteria for Vogt-Koyanagi-Harada disease: report of an international committee on nomenclature. Am J Ophthalmol 131(5):647–652
Levinson RD, Brezin A, Rothova A, Accorinti M, Holland GN (2006) Research criteria for the diagnosis of birdshot chorioretinopathy: results of an international consensus conference. Am J Ophthalmol 141(1):185–187
Polman CH, Reingold SC, Banwell B, Clanet M, Cohen JA, Filippi M et al (2011) Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 69(2):292–302
Abad S, Meyssonier V, Allali J, Gouya H, Giraudet AL, Monnet D et al (2004) Association of peripheral multifocal choroiditis with sarcoidosis: a study of thirty-seven patients. Arthritis Rheum 51(6):974–982
Seve P, Billotey C, Janier M, Grange J-D, Broussolle C, Kodjikian L (2009) Fluorodeoxyglucose positron emission tomography for the diagnosis of sarcoidosis in patients with unexplained chronic uveitis. Ocul Immunol Inflamm 17(3):179–184
Acharya NR, Browne EN, Rao N, Mochizuki M, International Ocular Sarcoidosis Working Group. (2018) Distinguishing features of ocular sarcoidosis in an international cohort of uveitis patients. Ophthalmology.;125(1):119–126
Fisson S, Ouakrim H, Touitou V, Baudet S, Ben Abdelwahed R, Donnou S et al (2013) Cytokine profile in human eyes: contribution of a new cytokine combination for differential diagnosis between intraocular lymphoma or uveitis. PLoS One [Internet] 8(2)
Chung Y-M, Lin Y-C, Liu Y-T, Chang S-C, Liu H-N, Hsu W-H (2007) Uveitis with biopsy-proven sarcoidosis in Chinese—a study of 60 patients in a uveitis clinic over a period of 20 years. J Chin Med Assoc 70(11):492–496
Rothova A, Alberts C, Glasius E, Kijlstra A, Buitenhuis HJ, Breebaart AC (1989) Risk factors for ocular sarcoidosis. Doc Ophthalmol 72(3–4):287–296
James DG, Anderson R, Langley D, Ainslie D (1964) Ocular sarcoidosis. Br J Ophthalmol 48:461–470
Tsen C-L, Chen S-C, Chen Y-S, Sheu S-J (2017) Uveitis as an initial manifestation of acquired immunodeficiency syndrome. Int J STD AIDS:956462417694569
Sudharshan S, Kaleemunnisha S, Banu AA, Shrikrishna S, George AE, Babu BR et al (2013) Ocular lesions in 1,000 consecutive HIV-positive patients in India: a long-term study. J Ophthalmic Inflamm Infect 3(1):2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
P. Grumet declares that he has no conflict of interest.
S. Kerever declares that he has no conflict of interest.
T. Gilbert declares that he has no conflict of interest.
L. Kodjikian has received speaker honorarium from ABBVIE, ALLERGAN, BAYER, NOVARTIS, ROCHE, and THEA.
M. Gerfaud-Valentin has received a speaker honorarium from SOBI.
A. De Parisot declares that she has no conflict of interest.
Y. Jamilloux has received a speaker honorarium from SOBI.
P. Sève has received speaker honorarium from ABBVIE, AKCEA THERAPEUTICS, GSK, NOVARTIS, SOBI, and ROCHE; he is a member of committee PEPITE (NOVARTIS).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Ethical approval
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Grumet, P., Kerever, S., Gilbert, T. et al. Clinical and etiologic characteristics of de novo uveitis in patients aged 60 years and above: experience of a French tertiary center. Graefes Arch Clin Exp Ophthalmol 257, 1971–1979 (2019). https://doi.org/10.1007/s00417-019-04411-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04411-1